Standardizing patient education with technology establishes a culture of patient safety.
Takeaways:
- Technology—electronic health records, patient portals, telemedicine, and social media—is playing an increasingly important role in healthcare delivery
- Discharge education can have limited effectiveness when it’s offered only once and when other distracting activities are going on.
- A thoracic and cardiovascular surgery unit produced discharge videos that can be accessed by patients and families through their patient portals.
By Colleen Villamin, MSN, RN, OCN, CNL, and Kati Berg, BSN, RN, PCCN
Technology plays an increasingly important role in healthcare delivery, whether in the form of electronic health records, patient portals, telemedicine, or social media. Patient education across specialties is naturally influenced by a number of technological innovations including app-based learning, virtual and augmented reality, and web and social media–based educational platforms. Video-based education is particularly effective for preparing patients across diverse populations for discharge.
Thoracic surgery and discharge education


The interprofessional workgroup of thoracic surgery nurses, advanced practice providers, thoracic surgeons, clinical nurse leaders, and a dietitian identified an opportunity to develop population-specific video-based discharge education. Our goal was to streamline diverse interprofessional team content that had previously been offered at the bedside or in a classroom setting using printed materials and demonstrating care techniques. We wanted to improve patient satisfaction, enhance patients’ ability and confidence to care for themselves at home, and standardize education to ensure that each patient is getting the same information. Our team aimed to discover whether using video and internet technology to deliver discharge education can enhance patients’ ability to care for themselves at home and improve patient satisfaction.
Applying technology to enhance patient education
The improvement process began in April 2015 when the interprofessional workgroup from the thoracic surgery unit submitted an application for internal funding to develop the discharge education video. We estimated that 780 patients per year would access the videos. The administration provided over $18,000 to cover the costs of video recording, project management, and editing.
Nursing staff wrote the scripts for the lung resection and esophagectomy discharge videos in collaboration with thoracic surgeons and advanced practice nurses. The lung resection discharge video includes:
- education on incentive spirometry
- ambulation
- arm exercises
- weight restrictions
- incisioncare
- diet
- pain management
- infection prevention
- bowel management
- when to obtain further
The esophagectomy discharge video includes:
- education on incentive spirometry
- ambulation
- weight restrictions
- activities to avoid
- incision care
- enteral feeding
- pain management
- infection prevention
- aspiration prevention
- bowel management
- when to obtain further
After the scripts were edited and reviewed by the patient education office for literacy level and ease of understanding, video production began, which included working with actual patients and clinicians to ensure authenticity and accuracy. (See Lights, camera, action!)


Video access
Patients access the discharge videos on postoperative day one from the patient education video library available on the televisions in their rooms. Patients also can view the videos through their electronic health record, which they can access with a smart device application called MyChart during and after hospitalization. Patients can securely log in to their MyChart account from their computer, smartphone, or tablet and view the follow-up discharge appointments and review the lung resection or esophagectomy discharge videos on demand.
Nurses reinforce the videos with written materials, return demonstration, and the teach-back method, which has been shown to reduce readmission rates.
Project outcomes
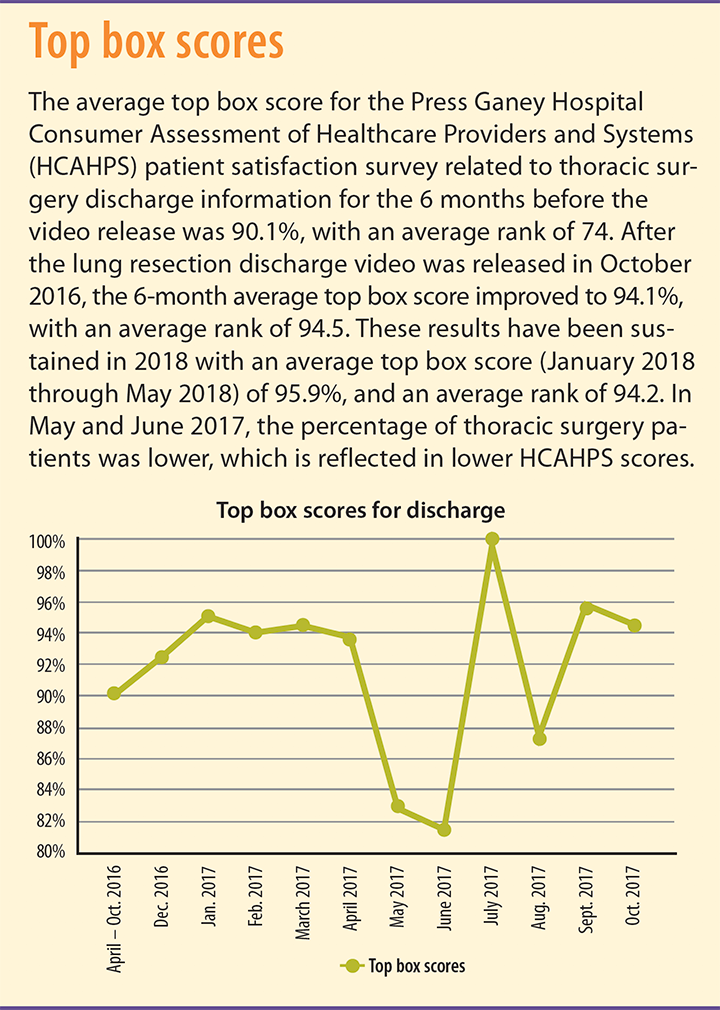
Outcome measures for this initiative were tracked using the Press Ganey Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) patient satisfaction survey. (See Top boxscores.) HCAHPS scores are reported in aggregate, so patient satisfaction on the unit includes many surgery types, not just esophagectomy and lung resection. Because of this, consistency of results varied according to the monthly percentage of thoracic surgery patients cared for on the unit versus other types of nonthoracic surgery patients. Patient satisfaction scores suggest a marked increase with higher volumes of thoracic surgery patients and a decrease with lower volumes. This may reflect more patients responding to the survey who aren’t eligible for the discharge videos. This outcome suggests the need for standardized discharge instructions for patients from other services, such as thoracic medical oncology and general internal medicine.

Pros and cons
Technology-driven patient education offers many advantages, including increasing accessibility to information when it’s convenient for the patient. Having control over access to health information can improve patient satisfaction, as demonstrated in this project, and decrease anxiety. In our organization, web-based educational videos have streamlined patient education, making the information and teaching consistent for each patient. And rather than receiving the education just one time while still in the hospital and confronting other distractions, patients can view the videos as needed to improve their comprehension of key points.
Technology-based education also can present challenges. Some patients have limited access to the technology necessary to view the videos, others might not understand how the technology works, and some might be uncomfortable or unwilling to use it. Another challenge is making the videos available in validated translations so they’re accessible to those for whom English isn’t a primary language. In our project, the videos were created in English for pilot purposes. Additional funding is necessary to produce the videos in other languages.
Translation to other settings
In a culture that focuses on patient safety and satisfaction, standardized discharge teaching reduces variation and ensures that patients receive accurate information to successfully care for themselves after discharge. Our initiative is translatable across patient populations and healthcare delivery settings.
If you’d like to implement a similar program at your organization, you’ll need to obtain funding to develop the educational content, work with interprofessional stakeholders (including patients), and assess individual patients to determine access to and comfort with technology platforms and devices.
Practice implications
Using video and internet technology to enhance discharge education has demonstrated improvements in patient satisfaction scores. Expanding use of this technology to other patient populations that our unit cares for may further increase patient safety and satisfaction. Future initiatives will explore the relationship between standardized discharge teaching with video and internet technology and readmission rates. Standardizing patient education content is essential for establishing a culture of high reliability and patient safety.
The authors work at University of Texas MD Anderson Cancer Center in Houston. Colleen Villamin is the associate director of telemetry/thoracic and cardiovascular surgery & central monitoring unit. Kati Berg is a clinical charge nurse
Selected References
Brown MM. Transitions of care. Chronic Illness Care: Principles and Practice. Daaleman TP, Helton MR, eds. New York: Springer; 2018:369-73.
Calvillo J, Román I, Roa LM. How technology is empowering patients? A literature review. Health Expect. 2015;18(5):643-52.
Centers for Medicare and Medicaid Services. HCAHPS: Patients’ Perspectives of Care Survey. December 21, 2017.
Chen HY, Wu TJ, Lin CC. Improving self‐perception and self‐efficacy in patients with spinal cord injury: The efficacy of DVD‐based instructions. J Clin Nurs. 2015;24(11-12):1666-75.
Mamlin BW, Tierney WM. The promise of information and communication technology in healthcare: Extracting value from the chaos. Am J Med Sci. 2016;351(1):59-68.
Saidinejad M, Zorc J. Mobile and web-based education: Delivering emergency department discharge and aftercare instructions. Pediatr Emerg Care. 2014;30(3):211-6.
Schooley B, San Nicolas-Rocca T, Burkhard R. Patient-provider communications in outpatient clinic settings: A clinic-based evaluation of mobile device and multimedia mediated communications for patient education. JMIR Mhealth UHealth. 2015;3(1):e2.
Win KT, Hassan NM, Bonney A, Iverson D. Benefits of online health education: Perception from consumers and health professionals. J Med Syst. 2015;39(3):27.
Wong TA, Lee C. Using technology, medical informatics in patient education. Optometry Times. 2017;9(6):8.
ant9-Tech Video-831



















