By Susan M. Priano, PhD, RN
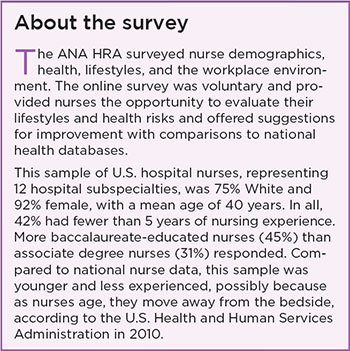
Nurses employed in U.S. hospitals are at risk for poor health outcomes due to unhealthy lifestyles and their work environment. Ranked by the public as the most trusted professionals and numbering 3.6 million nationwide, RNs have the power to effect behavior change as role models by practicing healthy lifestyles while improving their own health. Yet, a study of 2,730 hospital nurses from the American Nurses Association (ANA) Health Risk Appraisal (HRA), surveyed from October 2013 to December 2015, found serious deficits in diet, sleep, and physical activity that may jeopardize nurses’ health and negatively impact the healing strength of the profession. Here are some key findings from the survey related to health, lifestyle, and work environment.
Health


Lifestyles
Nurses’ lifestyles were often far from ideal in several areas, as these findings reflect:
- Diet. A mere 14% of the nurses were eating at least five servings of fruits and vegetables per day (2.5 cups).
- Physical activity. Just 45% of the respondents were engaged in aerobic activity of at least moderate intensity for 2.5 or more hours per week, while 47% performed muscle-strengthening activities twice a week.
- Sleep. Nearly half of the nurses (47%) slept fewer than 7 hours per day.
- Smoking. Most (94%) survey participants were not currently smoking cigarettes.
- Alcohol consumption. Over 90% of the nurses in the sample were within the recommended limit of 0 to 7 alcohol servings per week.
Lifestyle, by choice or consequence, exerts a great influence on one’s health. Nurses unable to adopt and maintain healthy lifestyle behaviors are at risk for chronic diseases and early mortality. On the other hand, nurses who make healthy lifestyle choices have positive effects in caring for patient populations. They’re more apt to discuss and recommend preventive behaviors such as smoking cessation, more physical activity, and eating a healthier diet to the people under their care.
Nurses who practice healthy lifestyles of daily physical activity, diet, and sleep habits may be better able to prevent workplace injury and avoid errors related to fatigue. Thus, improving the health and healthy lifestyles of nurses may improve patient care.
Nurses’ health risk factors may be attributed to hospital workplace conditions that counter their efforts to maintain a healthy lifestyle and contribute to poor self-rated health.
Work environment
ANA defines a healthy work environment as “one that is safe, empowering, and satisfying.” Yet, 63% of RNs in the United States are employed in hospitals, which are considered among the most hazardous workplaces in this country, according to reports from the U.S. Bureau of Labor Statistics and Occupational Safety and Health Administration. Hospital workers suffer work-related injuries at a rate of 6.8 for every 100 full-time employees, almost twice the rate in industry. Nurses, who constitute the largest segment of hospital employees, collectively, are the most vulnerable for multiple workplace safety hazards due to the hospital environment.

The HRA assessed eight areas of known work environment concerns: workplace climate, health and safety risks, safe patient handling and mobility, sharps, bullying/violence, fatigue, wellness, and absent/present. Highlights of the survey include the following:
- Climate. In total, 75%-80% of nurses had positive perceptions of their employer, and 84% felt they were treated with dignity and respect.
- Risks. Of 21 potential risks, workplace stress was felt by 80% of nurses, followed by 61% reporting musculoskeletal disability; 40%-48% were at risk for hospital-acquired infections of respiratory or blood borne pathogens.
- Sharps and safe patient handling. Programs were in 75%-90% of the facilities, but only 26%-35% of nurses were involved in the planning and selection of safety equipment, and only 47% of nurses routinely used lift assistance devices.
- Bullying/violence. Nurses often (56%) experienced verbal or physical abuse from patients, families, and peers, while 42% of nurses felt aggression from persons in a higher level of authority.
- Fatigue. Slightly more than half (52%) of nurses worked 12-hour shifts, 41% worked overtime (>40 hours/week), with 67% reporting unplanned overtime, and more than 50% felt obligated to work when ill. Many nurses (61%) were unable to complete their assignments unless they worked through their breaks.
- Wellness. Services such as weight loss and smoking cessation were accessible to 55% of nurses with 49% participation. Healthy foods were available for 57% of nurses but were more expensive than other food choices.
- Absent/present. Nurses (55%) reported to work when sick, and 67% felt present when at work.
Need for a healthy workforce

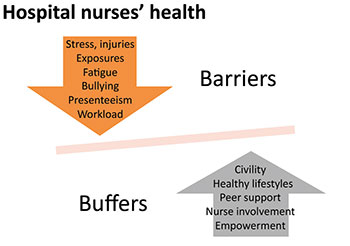
While nurses’ chief duty is to protect and promote health, hospital work exposes nurses to high levels of stress and physical and emotional injury. The ANA HRA has identified the barriers and buffers of a healthy nurse workforce and workplace. (See Hospital nurses’ health.)
A healthy nursing workforce functions as a team working together, supporting the health of their patients and each other. Healthy workplaces can minimize workplace stress, reduce injuries and medical errors, and improve patient outcomes. Alternative healthcare models offer solutions for flexible staffing, rest, and healthy food to benefit health for all. Collective efforts and visionary leadership are essential to achieving worker protections.
Susan M. Priano is a staff nurse for the city and county of San Francisco, department of public health.
ANA resources
- Healthy Nurse, Healthy Nation™. Connect with RNs and join nurses leading the way to better health.
- Healthy Work Environment. For ANA’s position statement, tools, and resources.
February 2018 Frontline FINAL




















1 Comment.
Dr. Priano,
Would you please point me to the reference for this study findings? I am not finding the report.