Navigating a new role during the pandemic
- Magnet program directors shoulder many roles and responsibilities, including finding the right initiatives, changes, and outcomes that will meet the elements of the Magnet standards.
- Positivity and motivation can help emphasize the desire for improvement, even in the face of challenges.
- Successful virtual site visits require organization, teamwork, and reliable technology and support.
The American Nurses Credentialing Center’s (ANCC) Magnet Recognition Program® serves as the highest recognition of nursing excellence. The designation puts nurses at the forefront of influencing improved patient outcomes and experience as well as ensuring a safe and healthy work environment. Magnet recognition represents nurses’ commitment to lifelong learning and bedside autonomy, which allows them to continue to advocate for patient care and safety.
Each organization working to achieve Magnet designation appoints a Magnet program director (MPD) to spearhead the journey and serve as the main contact with the Magnet Program Office throughout the process. My organization hired me as MPD for our sixth Magnet designation, which occurred during the COVID-19 pandemic. As a novice MPD, I faced challenges, but the journey proved rewarding for me, the organization, and the nursing staff. (See Novice MPD resources.)
Novice MPD resources
As a novice Magnet® program director (MPD), learning the Magnet standards and understanding the MPD role and responsibilities took time, effort, and dedication. Some of the resources I found most helpful include the following:
- Guidance from another experienced MPD within the organization
- American Nurses Credentialing Center (ANCC) In Pursuit of Excellence classes
- ANCC resources and learning communities (the Magnet® Application Manual updates and FAQs help clarify the standards and provide guidance)
- New Jersey Coalition of Magnet organizations, a group of experienced MPDs within the state. Other states may offer something similar
- Independent experts and consultants
- Magnet4Europe International mentoring (magnet4europe.eu)
For more information about ANCC Magnet educational programs, visit nursingworld.org/organizational-programs/magnet/program-tools/education.
MPD key roles
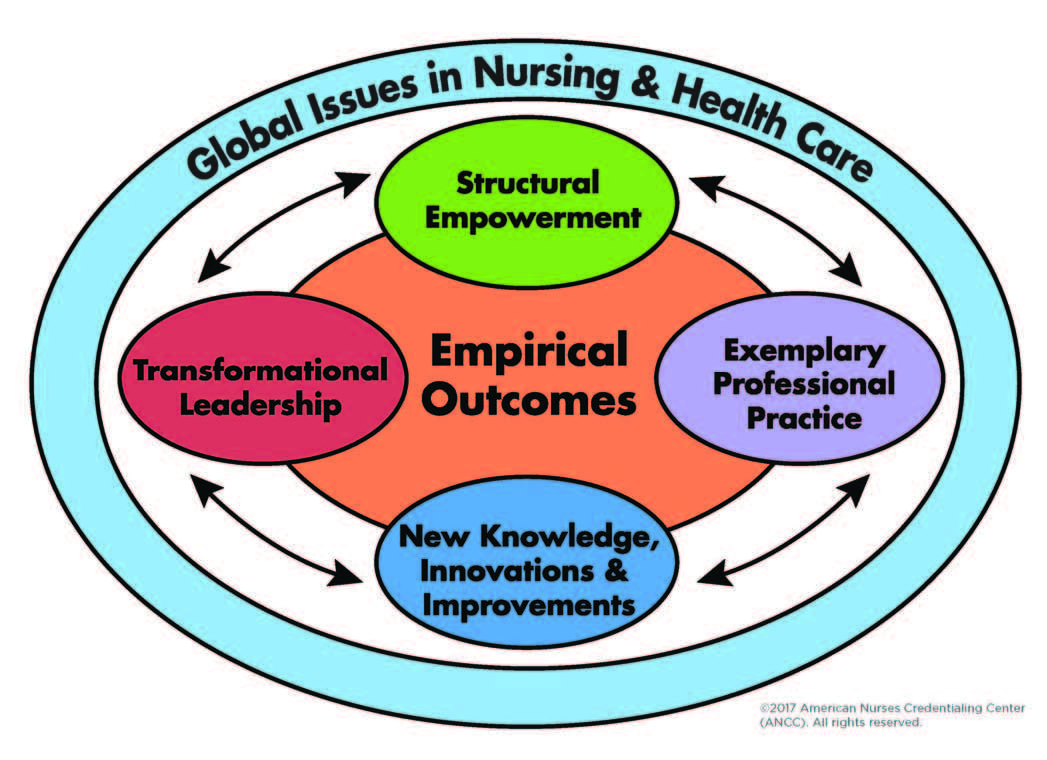
The MPD shoulders many roles and responsibilities, including finding the right initiatives, changes, and outcomes that will meet the elements of the Magnet standards: Transformational Leadership, Structural Empowerment, Exemplary Professional Practice, and New Knowledge, Innovations, and Improvements. MPDs must have a keen eye for how the organization’s processes and applications meet the standards and showcase nursing excellence. They help the nursing and interdisciplinary team understand the standard’s requirements (including Empirical Outcomes [EOs]) and facilitate brainstorming ideas from across the organization until they identify the strongest and most appropriate suggestion. MPDs also motivate and inspire the team throughout the journey.
Meeting the standards
The MPD creates an outline that identifies which projects and processes align with specific Magnet standards to ensure all elements are met. For example, one Magnet standard requires the demonstration of an improved outcome associated with an evidence-based change made by clinical nurses in alignment with the organization’s professional practice model (PPM). In this example, the standard requires two key elements: a clinical nurse spearheading the change and an improved patient outcome. We selected the implementation of the Bedside Mobility Assessment Tool, an evidence-based change led by clinical nurses. Our organization’s PPM aligns with this change, which emphasizes patient-centered care and improved outcomes (falls reduction). During implementation, I tracked each step of the process and identified those involved, highlighting the contributions of clinical nurses and monitoring the fall rate until we achieved the desired goal.
Magnet standards may require demonstration of EOs, which presents data results in graphs and tables, or non-empirical outcomes, which demonstrates standards using documents such as meeting minutes, attendee lists, presentation slides, and modules. MPDs measure EOs based on data (pre-intervention [baseline for improvement], intervention implementation, and post-intervention) that demonstrate the most compelling and sustained improvement. Some measures of EO success—such as nurse satisfaction, patient satisfaction, and nurse-sensitive indicators or quality outcomes—require comparing performance against national benchmarks. The comparison allows an organization to see beyond its four walls to identify opportunities for development and seek more efficient processes.
Inspiring the team
The Magnet journey can be frustrating, especially if desired or sustained results aren’t being achieved. The MPD’s positivity and motivation can help emphasize the desire for improvement, even in the face of challenges. Leading and inspiring the team to find alternative plans when one doesn’t work plays an important role in our continued journey to nursing excellence and in embedding the Magnet standards into an organization’s culture.
Navigating Magnet in a pandemic
During my time as MPD, we completed and submitted the Magnet document and then had our site visit during the pandemic. All the proven strategies for accomplishing these complex tasks required modification to ensure adherence to necessary safety guidelines, especially with regard to social distancing.
Completing and submitting the document
The sources of evidence planner and tracking tool that we created before the height of the pandemic proved very helpful. The tool identified possible stories and initiatives that meet the elements of the Magnet standard, which provided me with ample examples to pursue during the height of the pandemic as we focused on caring for the rising number of patients with COVID-19 and a high census. In addition, the planner and tracking tool helped me adapt to new guidelines and protocols and offered alternatives for processes and initiatives that proved unfeasible or unsustainable due to the pandemic.
The changes required in response to the pandemic created challenges and feelings of uncertainty and confusion among staff. However, they also highlighted nurses’ resilience, creativity, and innovation, which offered us new knowledge and opened the door for novel processes and initiatives for exploration. Adhering to social distancing guidelines led to an increase in technology use, including emails, phone calls, text messages, and virtual conferences to replace face-to-face meetings. Educational strategies—such as web-based learning games, animations, video recordings, and electronic newsletters—replaced the typical processes for disseminating information and providing education. These changes came suddenly with little time to adjust, but they led to creative solutions for encouraging participation and sustaining interest. In addition, because virtual platforms allowed us to offer several sessions on different days and times, more nurses could participate by joining from work or home and eliminated audience limitations due to space.
In the midst of these challenges, our organization migrated from a Microsoft to a Google workspace. Exploring the new Google Forms, I created an electronic documentation method for peer review and professional development planning, which eliminated the need for collecting hard copies. The digital format allowed us to send the documents via email, text messages, URLs, and QR codes. Novice and experienced nurses provided overall positive feedback on this new process. It shortened our turnaround time for completion and made tracking and collating results easy and seamless because of the ability to generate a spreadsheet from the submitted responses, which replaced the manual process.
Virtual site visit
We received Magnet Program Office notification that we qualified for a direct on-site visit, but we chose a virtual visit because of the high number of COVID-19 cases in our state and organization. Our hospital was the first in the health system to conduct a virtual visit, so few processes existed to provide guidance. The coordination, constant communication, and support of the Magnet lead appraiser proved beneficial.
Using computers on wheels (COWs) or an iPad for virtual meetings and unit tours helped us conduct meetings and interact with the Magnet appraisers during the visit. With almost 50 units scheduled for appraisal, we prioritized ensuring that nurses in each unit had the opportunity to interact with the appraisers. We developed an innovative plan to use two COWs with a camera and a microphone managed by two Magnet champion escorts per appraiser. One escort and COW started at the first unit on the agenda while the other escort and COW waited at the next unit. After handing off the appraiser to the second unit escort, the first escort and COW moved to the third unit to wait. The two escorts alternated this process (turning off microphones and cameras when moving from unit to unit) until the tour was complete. This helped us maximize the 15 to 30 minutes allotted for unit tours. The escorts and appraisers appreciated this approach, calling it seamless and efficient.
In developing this process, we paired units close to each other, chose escorts familiar with the different units, and selected easy-to-use technology. A pre-visit dry run helped us identify and address challenges with Wi-Fi connectivity, noise control, and computer power sources. Information technology and audiovisual support provided technical troubleshooting support.
For meetings, each appraiser had their own conference room and call-in number that they used throughout the visit. For meetings requiring all of the appraisers, we established a separate call-in number. This strategy, as well as setting up recurring virtual meeting invitations for the duration of the site visit (one for meetings attended by all appraisers and another for each appraiser) simplified the process of joining meetings and eliminated the need to log in and out each time.
The participation and involvement of our Magnet champions proved essential to the successful implementation of the virtual site visit. These designated staff nurses motivated and prepared their units and teams for the visit. They took ownership of communicating Magnet information and updates, tracking their unit’s performance, and creatively displaying their unit’s metrics, stories, and achievements. They also acted as cheerleaders to rally their teams for unit tours, welcome appraisers, and sustainin unit excitement and energy. In addition, they escorted the appraisers during unit tours and meetings and served as hosts and facilitators to represent our organization’s nurses and culture. (See 10 virtual site visit tips.)
10 virtual site visit tips
The following tips can help you plan a successful virtual site visit.
- Pair units. If possible, pair units near each other to save time when moving from one unit to the next.
- Maximize time. Especially for bigger organizations, consider having two nurse escorts with two computers on wheels or iPads rather than one. This will save time when moving between units.
- Test technology. Before the visit, check Wi-Fi connectivity in units and meeting rooms, as well as the computer’s camera, microphone, and battery/power source life. If possible, conduct a virtual visit dry run to identify issues to resolve.
- Plan the tour route. Map out the route of each appraiser with the nurse escorts. Ensure escorts are familiar with the area and can access their assigned units.
- Get support. Enlist information technology and audio-visual support for the dry run and site visit to help troubleshoot and resolve any technical glitches.
- Assign conference rooms. If possible, assign one conference room for each appraiser for the duration of the site visit. This will eliminate the need to log in and out for every meeting session.
- Simplify virtual meeting invitations. Set up recurring virtual invitations for the duration of the site visit, one for meetings attended by all appraisers and another for each appraiser. This will simplify the process of joining the meeting and eliminate the need to log in and out for every session.
- Plan ahead. Provide login information and the meeting ID number for each appraiser in the designated meeting rooms and have a computer on wheels or iPad available in case anyone loses connectivity or calls are dropped.
- Create an agenda. Provide the agenda or, if possible, create a separate list of meetings and unit tour schedules for each appraiser and provide them to designated escorts.
- Remind staff. Display signage to remind staff that the survey is ongoing and that activities in the units will continue. Interaction with appraisers will occur
in the hallways, so alert staff to keep noise to a minimum and avoid areas where the tour is being conducted.
Key to success
The MPD plays a huge role in spearheading the Magnet journey, but the key to our success was the people in our organization, from our team of nurses to every member of the interprofessional teams led by the chief hospital executive. The interprofessional team’s support, collaboration, and eagerness to speak about how they value nurses, their role, influence, contributions, and collaboration in improving outcomes and the work environment served as a morale booster and demonstrated teamwork and partnership. The nursing leaders—especially the chief nursing officer, network chief nurse executive, network Magnet designation director, nursing directors, and nurse managers—modeled and supported the Magnet culture and championed nursing excellence. And, most importantly, the nurses who live the Magnet standards and principles in their everyday practice, despite the challenges and changes of the pandemic, exemplify why we received Magnet designation.
Rocel Dela Rosa Besa is the Magnet Program Director at Hackensack Meridian Health–Jersey Shore University Medical Center in Neptune, New Jersey.
American Nurse Journal. 2023; 18(1). Doi: 10.51256/ANJ012356
References
American Nurses Credentialing Center. ANCC Magnet Recognition Program® nursingworld.org/organizational-programs/magnet
American Nurses Credentialing Center. 2019 Magnet Application Manual. Silver Spring, MD: ANA Enterprise; 2017.
Bottino B, Wood DA. Magnet program directors guide nursing team members through an extensive process. Nurse.com. August 10, 2015. nurse.com/blog/magnet-program-directors-guide-nursing-team-members-through-extensive-process
Lackey SAM, Lott TF, Whade J. Pivotal role of the Magnet® program director. Am Nurse J. 2021;16(10):46-9.
Tomaseski C. The inside scoop of a virtual site visit. Am Nurse J. 2020;15(9):70-3.
Key words: Magnet, program director, novice, pandemic, COVID-19




















3 Comments. Leave new
Such an inspiring article and proud and grateful for Rocel Besa’s influence on my growth and development as nurse. My relationship with Rocel as a colleague, mentor, Program manager but most of all a dear friend is valuable beyond measure and I’m blessed to know her.
As a new Magnet Program Manager, the responsibilities of the Magnet journey are overwhelming at times. Rocel has done a wonderful job of offering guidance from her personal experience for those new to our roles. This article has given me the inspiration and motivation I need to continue to strive to do my very best. I love the description offered of the Magnet Champions and leaderships roles as well. Rocel you offer wisdom and inspiration to all pursuing Magnet designation or redesign in their organizations, thank you for a wonderful article.
Jane & Jan, thank you so much! I am so glad that you find the article helpful and inspiring. I feel fortunate to be given the opportunity by American Nurse journal to share my experience and learning as a novice Magnet Program Director.