“Iam involved in decisions that affect my work.” Many hospitals are striving to achieve better scores on this important employee-engagement survey question, as well as to incorporate a robust shared leadership program to meet recommendations of the Magnet Recognition Program®.
At the University of Colorado Hospital (UCH) in Aurora, we had a unique opportunity to revise our shared leadership model to focus on providing more consistency and structure for existing unit-based councils (UBCs) and to kick-start UBC development in areas that lacked a council.
According to research by Nancy Ballard of the Center for Nursing Excellence of Wellstar Health System in Georgia, structural factors (including role identification, support processes, decision structure, scheduling, and education) are crucial to successfully communicate a vision by senior nurse leaders. Support from nurse managers is also important to changing practice patterns from authoritative to shared decision making.
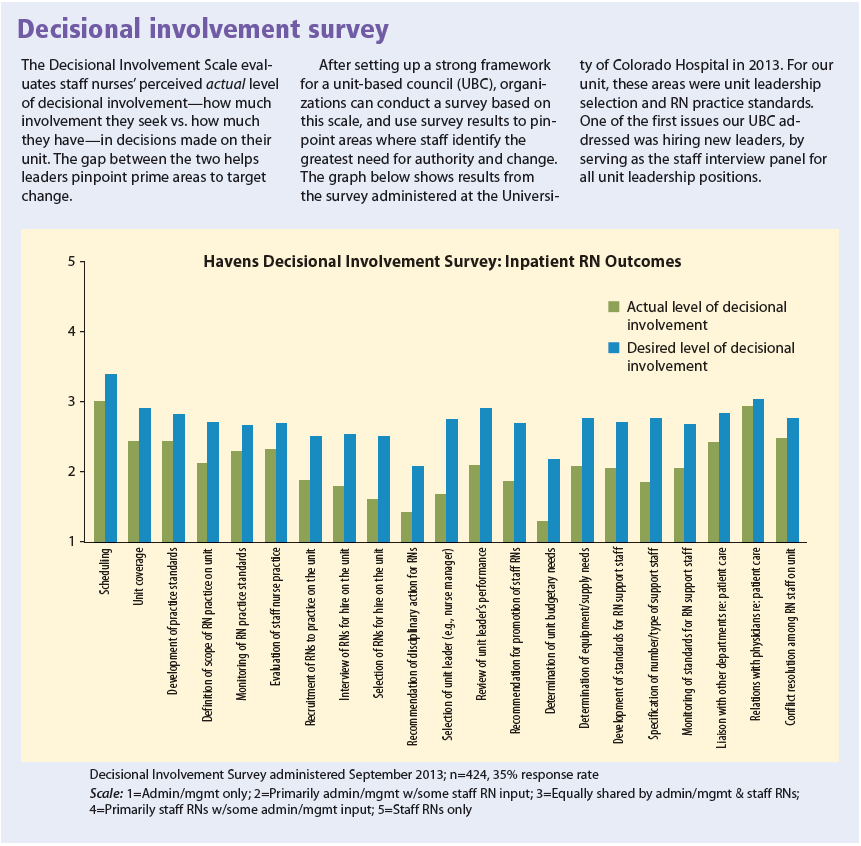
Active participation in decision making is also vital in optimizing UBCs. Havens and Vasey define decisional involvement as “the pattern of distribution of authority for decisions and activities that govern nursing practice policy and the practice environment.” To prepare for restructuring the shared leadership model at UCH, nursing leaders decided to use the Decisional Involvement Scale (developed by Havens) to develop a baseline measure of staff decision making before and after UBC implementation. In 2013, the hospital used the scale to collect baseline data from nurses and other care providers to determine satisfaction with their current decision-making level. This instrument lets users rate their actual level of decisionmaking in their work area and compare it to their desired level. Managers were surveyed on the same dimensions. (See Decisional involvement survey.)
You’ve been selected to serve on a nursing council: Now what?
Developing a mentor program to improve support and retention
Preliminary steps to creating or revising a shared decision model
Before addressing gaps revealed by the survey, UCH had to create a solid foundation and structure to promote UBC success. The council’s overall structure should encompass how the unit selects this leadership group, how the manager mentors the council on its new authority, and how council members can skillfully discuss issues in a way that promotes resolution.
Selecting UBC members
When forming or restructuring a UBC, leaders must create energy around the council’s purpose and educate staff on the return on investment. They need to establish a clear purpose for the council from the beginning. Staff can nominate themselves or their peers to represent them on the UBC; they may need to urge peers to apply for this role.
Staff also need to feel confident that UBC members will act in the unit’s best interest, because the unit’s work directly affects unit outcomes. So those nominated as council members should have a respected skill level and be perceived as capable leaders. In addition, to put as many stakeholders as necessary at the table, all care roles (such as nurses, therapists, techs, and other ancillary support staff) should be represented, including night-shift staff. For example, when addressing a medication shortage issue, we made sure to include the unit pharmacist in the discussion.
Mentoring by managers
Managers play a key role in developing a successful UBC by establishing the correct scope of decision making for each issue, providing the council with valuable information, removing potential decision-making barriers, and advocating for resolution on the unit and other affected departments. Manager engagement and training are crucial to supporting UBCs and guiding them without stifling their decision-making authority. Attending meetings helps the manager gain insight into the unit’s real-time temperament.
Submitting issues
Funneling frustrating unit issues through a decision-making committee made up of informal leaders sounds as if it would be easy. But in many cases, workarounds that staff incorporates into the workflow hide the true issues. Creating a positive culture around issue resolution is the first step in opening up opportunities for resolving problems by the UBC. For our UBC, we used the basic SBAR tool to create a familiar framework for staff to evaluate an issue and submit it to the committee for discussion.
- Situation: What is the issue, problem, or idea?
- Background: What is the clinical context, hospital policy, or standard of practice surrounding the issue?
- Assessment: What do you think the problem is? What is really happening?
- Recommendation: What would you do to correct or improve this?
Sharing power, control, and responsibilities
Unlike the traditional formal hierarchical power structure, the UBC allows frontline clinical nurses and other staff to share power, control, and responsibility in their work areas across the hospital system. Decentralized decision making is a core component of organizations with Magnet® designation.
Research supports UBCs’ contributions to increased staff engagement and frontline empowerment, creating a more satisfying environment for staff and patients. However, leaders must recognize and visibly support these councils to ensure that the components of a shared leadership model are successful and productive.
Kaycee Shiskowsky is nurse manager of the pulmonary unit at the University of Colorado Hospital in Aurora. Mary Krugman is an independent consultant in Denver, Colorado.
Selected references
Ballard N. Factors associated with success and breakdown of shared governance. J Nurs Adm. 2010;40(10):411-6.
Fray B. Evaluating shared governance: measuring functionality of unit practice councils at the point of care. Creat Nurs. 2011;17(2):87-95.
Havens DS, Vasey J. Measuring staff nurse decisional involvement: the Decisional Involvement Scale. J Nurs Adm. 2003;33(6):331-6.
Hess RG Jr. Slicing and dicing shared governance: in and around the numbers. Nurs Adm Q. 2011;35(3):235-41.
Wessel S. Impact of unit practice councils on culture and outcomes. Creat Nurs. 2012;18(4):187-92.




















3 Comments.
I am working on developing a unit based council here on our Medical Surgical Unit. Looking for any additional information at I can use to get staff energized and invested in this process. Looking for any information on this topic that your willing to share.
I am in the process of trying to start a unit based council for our unit. I’m interested in finding someone to come in and speak to our unit about how they implemented a council and the types of issues that have been successfully tackled. Please contact me if you would be willing to speak to our group. We are in the St Petersburg, FL area and eager to get this started. My email address is lindsay.predmore15@gmail.com.
Thank you in advance.
Lindsay Predmore
I am currently preparing my capstone and this article was very helpful to me. The topic that I am working on is shared governance.