To keep patients healthy, safe, and well, registered nurses (RNs) have to be healthy, safe, and well themselves. Yet RNs face health, safety, and wellness risks unique to their profession. This article outlines how RNs and employers can identify, mitigate, and reduce these risks. To provide context and evidence for risks, it also describes key findings from the American Nurses Association’s (ANA) HealthyNurse™ health risk appraisal (HRA).
Identifying risks
Workplace risks can be identified in various ways, including employee surveys, incident report reviews, literature reviews, hiring of occupational health professionals, workplace walk-throughs, and detailed observation of employees’ routine job tasks. The HRA is another useful tool. In collaboration with Pfizer, ANA developed an HRA to help RNs and nursing students identify their personal and occupational health, safety, and wellness risks. This online survey allows them to compare their results with established ideal standards and national averages (where available). After completing the survey, respondents can access a wellness portal with resources specific to their identified needs. Compliant with the Health Insurance Portability and Accountability Act, this HRA is free and available to all RNs and nursing students enrolled in a program leading to RN licensure.
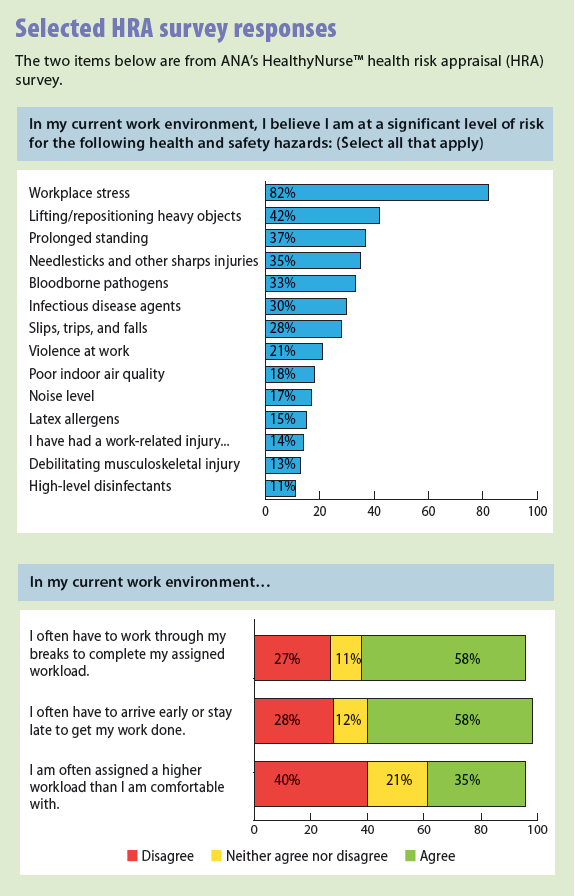
Findings from the HRA survey will help establish context for the actions that nurses and employers need to take. Preliminary findings provide a snapshot of the 3,765 RN and student nurse participants’ responses received between October 2013 and October 2014. Of the participants, 90% were RNs, 8% were student nurses, and 2% were retired or former RNs. Because the HRA survey remains open, results can’t be generalized to the broader nursing workforce yet. (See HRA’s full executive summary at http://www.nursingworld.org/MainMenuCategories/WorkplaceSafety/Healthy-Nurse/HRA-Executive-Summary/ANA-HRA-Executive-Summary.pdf and see Selected HRA survey responses.)
Occupational safety
Occupational safety risks for RNs include stress; fatigue; injuries caused by manual patient handling; needlestick injuries; incivility, bullying, and workplace violence; and toxic chemical exposures.
Stress
Respondents in ANA’s HRA survey identified stress as the top risk in the work environment; 82% believed they were at a significant risk level. In comparison, the average percentage of employees who feel stressed out is only 36%, as reported by the 2011 Stress in the Workplace Survey from the American Psychological Association.
To cope with stress effectively, RNs must practice self-care. Make the effort to recognize when you’re feeling increased stress, and identify and use effective stress-reducing techniques, such as meditation, prayer, mindfulness, exercise, deep breathing, and work breaks. Employers can provide counseling, individual coping strategies, employee assistance programs, wellness centers, and support groups. A quiet place, such as a restoration room where nurses can go to decompress, may help. Most important, employers must decrease workplace stressors by ensuring optimal staffing, reasonable workloads, appropriate work hours, supportive policies and procedures, and a carefully cultivated culture of safety and respect for employees.
Fatigue
HRA survey respondents reported sleeping an average of 8 hours during a 24-hour period. To ensure a culture of safety, employers and RNs must reduce RN fatigue and sleepiness. ANA recommends RNs work no more than 40 hours in professional nursing during a 7-day period and strive for 7 to 9 hours of sleep in a 24-hour period. Employers need to eliminate mandatory overtime as a staffing solution and give RNs opportunities to provide input into scheduling.
Injuries caused by manual patient handling
Manually lifting, transferring, and repositioning patients is hazardous and commonly results in painful, career-ending injuries. In ANA’s HRA survey, 42% of respondents identified manual lifting as a serious workplace concern and 53% reported experiencing musculoskeletal pain at work. Remember—there’s no safe way to lift a patient manually, regardless of your physical strength, fitness level, gender, or age.
Musculoskeletal injuries can be reduced drastically through comprehensive safe patient-handling and mobility (SPHM) programs involving SPHM technology (such as lifts and friction-
reducing devices). In 2013, ANA released Safe Patient Handling and Mobility Interprofessional National Standards, which outlines the key elements of an effective SPHM program.
Needlestick injuries
The Needlestick Safety and Prevention Act requires employers to review new technology, maintain sharps injury logs, and obtain input from frontline staff in evaluating and selecting safer devices. RNs and employers need to purchase and use safety devices, ensure that safe sharps disposal is available and used properly, and use best practices when handling sharps. Among HRA survey respondents, 94% reported they have access to sharps safety devices but only 31% said they’re involved in the selection process.
Incivility, bullying, and workplace violence
Approximately half of survey respondents said they’ve experienced verbal or nonverbal aggression from a peer. Aggression from patients and their family members also is a concern: 43% of respondents said they’ve been threatened by a patient or family member, and 24% said they’ve been physically assaulted. ANA’s Professional Issues Panel on Incivility, Bullying, and Workplace Violence has developed a position statement with detailed recommendations for RNs and employers. The document was released in August 2015.
Toxic chemical exposures
RNs may be exposed to toxic workplace chemicals, including hazardous drugs, pesticides, sterilants, disinfectants, and industrial cleaning solutions. For instance, 11% of HRA respondents reported they felt at significant risk from exposure to high-level disinfectants. Note all chemicals you have handled and have been exposed to. When using and disposing of these products, follow the product’s labeling, safety data sheets, instructions, government regulations, and established policies and procedures.
Employers should strictly observe the hierarchy of hazard control—elimination, safer substitute, engineering, administrative controls, and personal protective equipment. They must provide information about chemicals, and RNs should attend all education programs offered. For more information, visit www.osha.gov/SLTC/healthcarefacilities and http://www.cdc.gov/niosh/topics/healthcare, as well as the websites of the Centers for Disease Control and Prevention, Environmental Protection Agency, and Oncology Nursing Society.
Worksite wellness
Typically, full-time employees spend at least 8 hours at work or in a related activity during an average workday. Healthy workplaces that promote employee wellness may improve morale, increase employee health, and yield positive financial results. Employers are recognizing this: Nearly 70% of HRA survey respondents reported having access to worksite wellness and health promotion programs.
Diet and exercise
Fewer than 60% of respondents said they have access to healthy foods, such as fruits, vegetables, and whole grains, during work hours. Besides packing healthy food for meals and snacks, avoid sugar-sweetened beverages and join an employee wellness committee. To increase your physical activity during the workday, take the stairs and wear an electronic health tracker. Employers should offer nutritious, fresh, whole foods in cafeterias and vending machines, priced equitably and available to all shifts. Onsite weight-loss programs, gym discounts, and farmers’ markets are additional possibilities.
Tobacco cessation
RNs have a low rate of smoking. About 18% of U.S. adults use tobacco, whereas 94% of HRA survey respondents said they don’t smoke at all.
Don’t use tobacco in any form. Employers should enforce a strict tobacco-free policy in the workplace. The National Quitline Network, National Cancer Institute, and other organizations offer free quitlines. For more resources, visit ANA’s Tobacco Cessation website (www.nursingworld.org/TobaccoCessation).
Focus on self-care
More than 80% of HRA survey participants responded favorably about their workplace health and safety. But 66% of nurses reported they put their patients’ health, safety, and wellness before their own. As a nurse, you need to place greater emphasis on self-care and occupational health. Take ANA’s HRA survey and visit ANA’s wellness portal (http://www.nursingworld.org/MainMenuCategories/WorkplaceSafety/Healthy-Nurse) to understand personal risks and learn about solutions.
Holly Carpenter is a policy associate in Nursing Practice and Work Environment at ANA. Jaime Murphy Dawson is a senior policy advisor, Occupational Safety and Health, in Nursing Practice and Work Environment at ANA.
Selected references
American Nurses Association. Addressing Nurse Fatigue to Promote Safety and Health: Joint Responsibilities of Registered Nurses and Employers to Reduce Risks. 2014. http://www.nursingworld.org/MainMenuCategories/Policy-Advocacy/Positions-and-Resolutions/ANAPositionStatements/Position-Statements-Alphabetically/Addressing-Nurse-Fatigue-to-Promote-Safety-and-Health.html
American Nurses Association. Safe Patient Handling and Mobility: Interprofessional National Standards Across the Care Continuum. Silver Spring, MD: Author; 2013.
American Psychological Association and Harris Interactive. Stress in the workplace: Survey summary; 2011. www.apa.org/news/press/releases/phwa-survey-summary.pdf
Goetzel RZ, Henke RM, Tabrizi M, et al. Do workplace health promotion (wellness) programs work? J Occup Environ Med. 2014;56(9):927-34.
Jamal A, Agaku IT, O’Connor E, King BA, Kenemer JB, Neff L. Current cigarette smoking among adults—United States, 2005–2013. MMWR Morb Mortal Wkly Rep. 2014;63(47):
1108-12.
Virgin Pulse. 2015: The business of healthy employees: A survey of workplace health priorities. 2015. http://community.virginpulse.com/businessofhealthyemployees15
Click to read the next article: Understanding the charge nurse’s role in staffing




















1 Comment.
Great article! Used this in our journal club.