SCENARIO: When you meet your patient Tom for the first time, he reports fever, headaches, a rash on his stomach, and muscle aches. As you perform your assessment, he says, “I’m not sure what’s wrong with me. It just came on a few days ago. At least it didn’t interfere with my camping trip.”
Staying healthy through outdoor exercise and other activities includes certain risks, including Lyme disease. Exposed skin outdoors provides an opportunity for black-legged or deer ticks to attach and transmit the disease to humans. (See Lyme disease by the numbers.)
If not diagnosed and treated early, initial Lyme disease, which is caused by the bacterium Borrelia burgdorferi, can lead to chronic disease. Patients with chronic Lyme disease experience a substantial decline in health and quality of life, similar to patients with heart failure and type 2 diabetes, and they may require symptom management for many years. Currently, no Lyme disease vaccine is commercially available, making early recognition and treatment crucial to positive outcomes.
Prevention and tick removal
Preventing tick bites is the key to decreasing the occurrence of Lyme disease. (See Steps to prevention.) Nurses in endemic areas (the Northeast United States and upper Midwest) are in a prime position to offer education to patients, family, and friends. Topics to cover include preventing tick bites, inspecting for ticks, and safely removing ticks.
Locating ticks can be difficult; adult ticks are the size of a sesame seed, while nymph ticks that infect most humans are the size of a poppy seed. To transmit bacteria, the tick must be attached longer than 36 to 48 hours.
Instruct patients to remove ticks as soon as they’re found. Explain the importance of removing the head of the tick (which is typically embedded in the skin) and not just the body protrusion. (See Safe tick removal.) Patients who don’t want to remove a tick themselves should contact their healthcare provider.
Assessment and testing
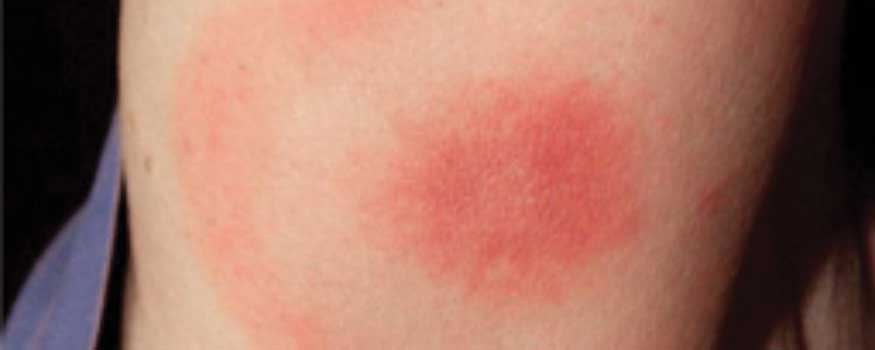
Lyme disease is categorized into three stages, with stage one being early and stage three being late and most severe. Symptoms of early Lyme disease include fever, chills, and the bull’s-eye rash. (See Lyme signs and symptoms.) However, some cases don’t present with obvious symptoms, so your interviewing and assessment skills are key to early detection and treatment.
Ask patients about recent activities (for example, camping or hiking), travel (for example, in the Northeast or upper Midwest regions of the United States), and exposure to or interaction with animals, including household pets that have been in wooded areas or open fields. Also, ask patients if they’ve experienced headaches, rashes, joint pain, or other recent onset symptoms. Be especially attentive to patients who present during the warm months because of increased risk of tick bites. Next, carefully inspect the patient’s skin for any possible ticks or a rash.
If signs and symptoms point to possible Lyme disease, the provider may recommend testing, which includes two steps. First, an enzyme immunoassay (EIA) or indirect immunofluorescence assay (IFA) is performed. If this test is negative, no further testing is required. However, if the test is positive or inconclusive, the next step is an immunoblot test, which detects immunoglobulin M and G classes of antibodies. Results are considered positive only if both the EIA/IFA and immunoblot are positive.
Treatment
Treatment of Lyme disease begins as soon as a diagnosis is made. Most patients recover rapidly and completely when treated with oral antibiotics, such as doxycycline or amoxicillin, in the early stages of the disease. If treatment begins in the later stages when neurological or cardiac symptoms are present, patients also may require I.V. medications, such as ceftriaxone or penicillin, to manage symptoms. About 28% of those infected with Lyme disease experience residual symptoms after treatment.
Tom’s rash, combined with his other symptoms, lead you to consider that he might have Lyme disease. Mention of the camping trip prompts you to ask where he went camping so you can determine if he was in a high-concentration area and how long he was there. You also ask if he noticed any insect bites. You then begin a thorough search of Tom’s skin, looking for a bull’s-eye’s mark, an infected area, or an embedded tick. You see a reddened area on Tom’s abdomen and detect swollen lymph glands. You share your findings with the provider and begin serological testing as ordered.
Education provider
As trusted members of the healthcare profession, nurses have the opportunity to provide education about the prevention of Lyme disease, the best way to remove ticks, and how to spot early symptoms. When assessing patients, engage them in conversation about the spread of the disease. If you’re a bedside or home health nurse, you’re in a unique position to share your knowledge with patients and their families. Increasing community awareness of Lyme disease is the first step to prevention.
Denise Stagg is a second-semester nursing coordinator at the University of Louisiana at Lafayette. Jessica McCarthy is an instructor at University of Louisiana at Lafayette, a nurse practitioner at Minute Med Walk-In Clinic in Lafayette, and a DNP student at the University of Alabama at Huntsville.
Selected references
Adams D, Fullerton K, Jajosky R, et al. Summary of notifiable infectious diseases and conditions–United States, 2013. MMWR Morb Mortal Wkly Rep. 2015;62(53):1-122.
Ali A, Vitulano L, Lee R, Weiss TR, Colson ER. Experiences of patients identifying with chronic Lyme disease in the healthcare system: A qualitative study. BMC Fam Pract. 2014;15:79.
Centers for Disease Control and Prevention. Lyme disease: Data and statistics. December 16, 2016.
Centers for Disease Control and Prevention. Lyme disease: How many people get Lyme disease. September 30, 2015.
Centers for Disease Control and Prevention. Lyme disease: Lyme disease rashes and lookalikes. September 4, 2015.
Centers for Disease Control and Prevention. Lyme disease: Transmission. March 4, 2015.
Centers for Disease Control and Prevention. Lyme disease: Treatment. December 7, 2016.
Centers for Disease Control and Prevention. Lyme disease: Two-step laboratory testing process. March 26, 2015.
Centers for Disease Control and Prevention. Lyme disease: Understanding the immunoblot test. March 4, 2015.
Dersch R, Sommer H, Rauer S, Meerpohl JJ. Prevalence and spectrum of residual symptoms in Lyme neuroborreliosis after pharmacological treatment: A systematic review. J Neurol. 2016;263(1):17-24.
Shen AK, Mead PS, Beard CB. The Lyme disease vaccine—a public health perspective. Clin Infect Dis. 2011;52(Suppl 3):s247-52.
World Health Organization. Vector-borne diseases: Lyme disease.



















3 Comments.
Eli Richardson, the author stated, “Patients with chronic Lyme disease experience a substantial decline in health and quality of life, similar to patients with heart failure and type 2 diabetes”. The quality of life is as poor as patients with heart failure and type 2 diabetes. Lyme disease is not similar to those diseases. Misdiagnosis of Lyme disease include: Multiple Sclerosis, Lupus, Fibromyalgia, Parkinson’s disease, Chronic Fatigue Syndrome and several other chronic diseases of unknown etiology.
How interesting that Lyme diseases mimic type 2 diabetes and even heart failure. I hear of a case of Lyme near our neighborhood not too long ago. We will reach out to a specialist to inspect our lawn for any insects that can harm my family’s health.
I appreciate this work amazing post for us I like it.