There are no doubt countless RNs who have stood out and inspired others during this challenging last year. For Nurses Month, we are highlighting the ways nurses make a difference through the stories of four RNs and the exceptional contributions they have made in terms of patient care, leadership, education, mentoring, advocacy, and community service.
Changing the narrative around mental health


Last summer, Melissa Earley, BSN, RN, QMHP-C, NHDP-BC, CCEMT-P, called up a long-time friend and colleague in healthcare, who had lost friends to
COVID-19, after she saw a Facebook post that suggested they might be contemplating suicide. She later learned that were it not for that phone call, in which her colleague, “busted out crying,” they likely would not be alive today.
Earley, a mental health professional and nurse consultant in Richmond, Virginia, is no stranger to the issue of suicide in the healthcare profession. Just before the pandemic, she joined the American Nurses Association (ANA) Nurse Suicide Prevention Review Committee (now the Strength Through Resiliency Committee). As a result of her contributions, she was invited to co-author the peer-reviewed article, “Nurse suicide prevention starts with crisis intervention” for the February 2021 issue of the American Nurse Journal. “Even [if only] one life gets saved because of that article, it’s worth it,” she said. With the reality of the pandemic, she realized nurses would be exposed to an unprecedented level of trauma and suggested the committee focus on providing resources to build resiliency. “I knew that nurses would need a soft place to land,” said Earley, a Virginia Nurses Association board member.
Based on both research and personal experience, Earley believes healthcare workers are especially affected by the stigma around mental health issues, which can prevent them from seeking help, especially if they’re having suicidal thoughts. “We’re [seen as] superheroes and [that] we’re invincible, but we’re not; we’re impacted just like anybody else,” said Earley, who has post-traumatic stress disorder stemming from cumulative exposure to trauma after nearly 30 years in emergency services and healthcare. She has seen things “you can’t unsee…. When you’re there in the middle of it, you’re running on almost instinct, and then when you have time to reflect, you start picking apart everything you did….it’s like the flood gates open.”
During the pandemic, Earley volunteered at a COVID-19 call center, mass vaccination clinics, and testing events, including at a congregate living care facility, where she contracted COVID-19. She continues to deal with residual symptoms.


Earley was shaped by her Great Aunt Katie, a volunteer medical assistant for the American Red Cross during WWI and WWII and later, the Presbyterian Missionary for Richmond, whom she often accompanied on care visits. “It impressed upon me that when a person is in need of help it’s our responsibility to answer that call.” When she was 5 years old, her great aunt hired her as a “dollar-a-day” nurse. “That’s where I caught the bug of wanting to be in healthcare and taking care of people.”
Empowering others is her superpower
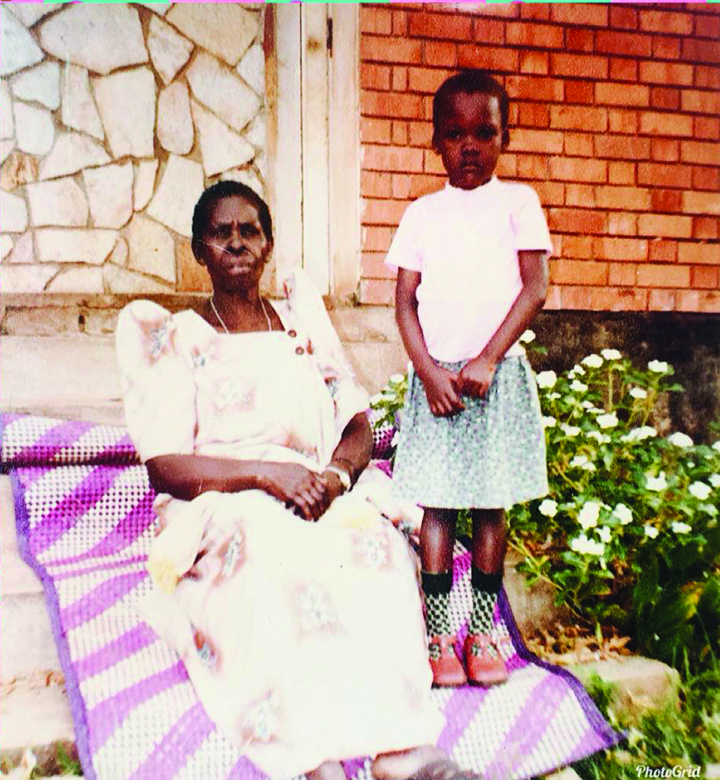
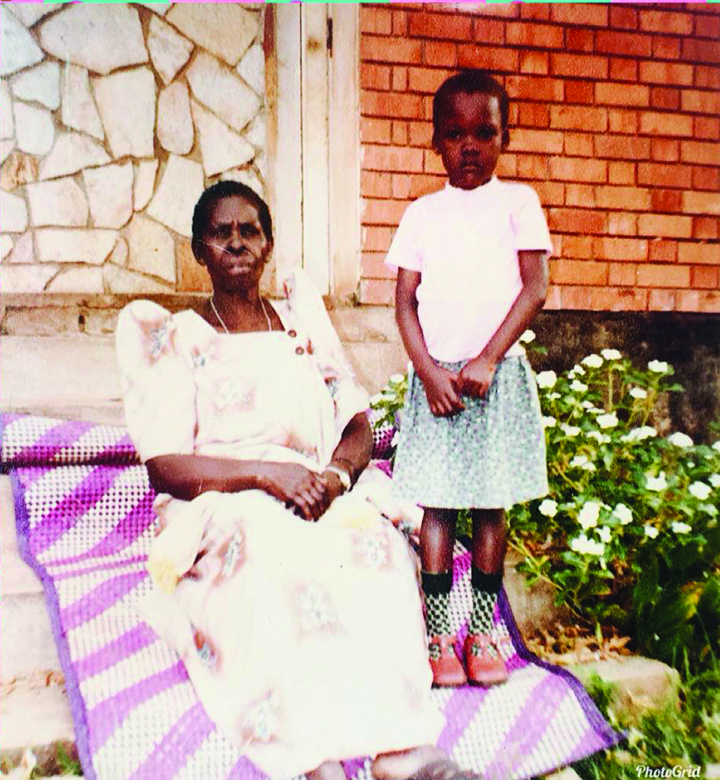
When she was a young girl, Schola Matovu, PhD, RN, MSN, gathered herbs so her grandmother, an informal nurse/midwife in a small Ugandan village where Matovu grew up, could provide remedies for different ailments, such as malaria. Her grandmother was Matovu’s primary caregiver—and her first mentor. “I knew that there was something special about what she did and I wanted to emulate her. So, to me, that was the beginning of my nursing career.”


While working on a medical-surgical oncology unit in Oakland, California, Matovu became acutely aware that people living in poverty, many of them racial minorities, frequently experienced poorer health outcomes. Matovu, a post-doctoral fellow at the Betty Irene Moore School of Nursing at UC Davis, is contributing to decreasing health inequities through her research, which promotes health and overall well-being of older family caregivers, particularly in Uganda where 660,000 children were orphaned as a result of the HIV/AIDS epidemic. The multiple stressors faced by these grandparent-caregivers, such as extreme financial burden and unresolved grief, intrigued her, leading her to explore the impact of caregiving on mental health. Matovu is helping in a practical way by developing a community-based pilot project in Uganda that will enable caregivers to generate income by raising farm animals.
Matovu and a colleague, Linda D. Gregory, PhD, MSN, RN, adjunct professor in the college of nursing at Samuel Merritt University in Oakland and an ANA\California member, co-founded the Nurse-to-Nurse Global Initiative (NTNGI) in 2013. NTNGI, which helps nurses navigate occupational barriers and advocate for themselves and their patients, plans to launch a leadership and professional development training program in Uganda next spring.
Matovu and Gregory also collaborated with the Center for Global Health at UCSF in San Francisco to start Global Nursing Forum to support nurses interested in global health opportunities. Matovu recently was appointed to the WomenLift Health Leadership Fellowship, which expands her professional network and raises the visibility of her work. “To be surrounded by brilliant global health women leaders is truly, truly a privilege,“ said Matovu, who recently accepted an assistant professor position at the University of Utah.


An alumna of the Minority Fellowship Program (MFP) at ANA, Matovu described the impact of that experience. “The dedicated mentorship and financial support provided me [with] the most valuable resources and a sense of community that I desperately needed in my nursing education.” She gives back by mentoring others and helping recruit minority nurses trained in mental health and substance use disorder for MFP nursing conferences.
“Being able to empower others to be the best that they can be is what nourishes me, what speaks to my soul,” Matovu said. “Being able to support others to achieve their superpower is my superpower.”
Planting seeds in students and nurses
As one of the world’s foremost experts in transcultural nursing and a nurse educator for more than 30 years, Priscilla L. Sagar, EdD, RN, ACNS-BC, CTN-A, FAAN, has encouraged students to find out what they love in nursing, to follow their dreams, and to pursue their full potential.
“I’m a firm believer in mentoring,” said Sagar, an ANA-New York member, who mentors nurses through ANA’s virtual mentoring program and has mentored nurses in the Philippines and Vietnam. “I believe in giving back. I believe I wouldn’t be where I am today without mentoring.” While studying for her doctoral degree, Sagar, who is professor emerita of nursing at Mount Saint Mary College (MSMC) in Newburgh, New York, went with her three mentors to Vietnam, where they trained nurse leaders to train other nurses. In 1999, she also participated in a presentation with her mentors at the International Council of Nurses (of which ANA is a member). “If I were not a part of that presentation, I wouldn’t be comfortable doing other presentations later in my life. That was like a start for me.”
Sagar pays back the support she received by mentoring faculty, nurse colleagues, and students in developing posters for conferences, podium presentations, and writing for publication. (MSMC faculty members and BSN students contributed to her second textbook on transcultural nursing, which is used worldwide.) She also conducts workshops for her alma mater, the Philippine Women’s University, and for the Philippine Nurses Association of New York (PNA-NY) Balik Turo program in which U.S.-based Filipino nurses go back to teach Filipino nurse colleagues current trends in nursing practice, education, administration, and research.
Last year, through the leadership development program of the Philippine Nurses Association of America, an organizational affiliate of ANA, Sagar’s proposal for a formal nurse mentoring program was awarded the most innovative capstone project. She hopes to implement this program at the Transcultural Nursing Society, where she is a Transcultural Scholar, and the PNA-NY.

“With my role modelling, I’ve been able to make a difference because I walk the talk,” she said, adding that she encourages and empowers her mentees to give back to the community and mentor others. Sagar’s own community involvement includes administering COVID-19 vaccines for the Medical Reserve Corps. She also encourages nurses to speak up and get involved in policy work. She co-wrote an op-ed urging the Centers for Disease Control and Prevention to redesign the Vaccine Administration Management System with end users in mind.
Speaking out and speaking the truth
Justin Gill, DNP, ARNP, RN, a Washington State Nurses Association member, is a health policy leader grounded by his day-to-day work in an urgent care clinic in Everett, Washington. Working with patients “helps me realize that this is what really matters,” he said.


Early in Gill’s career as a nurse practitioner (NP), he successfully developed an initial plan for a patient who had symptoms of colon cancer but neglected screening because she lacked health insurance. “It reinforced the fact that it didn’t matter if we have the best colonoscopy technology…if people can’t access it or have a fear of accessing it due to cost, then their health is actually jeopardized,” Gill said.
Both his clinical and advocacy work impact his third role—lecturer at the University of Washington Bothell School of Nursing, where he highlights how health policy directly affects bedside care. “If patients don’t have insurance, or if nurses don’t have access to PPE [personal protective equipment], that all comes from some policy level, and finding a way for them to find their voice helps amplify my overall goal, which is to get nurses more involved in legislative and clinical advocacy,” he said.
On an advocacy level, Gill worked on a campaign that led to the introduction of legislation in Washington requiring that insurance companies reimburse NPs who own their practice at the same rate as physicians. As chair of the legislative/health policy council of the Washington State Nurses Association, he worked to strengthen safe staffing legislation. He
also has served as a trustee on the ANA Political
Action Committee Board.
As a health policy leader and a clinician, Gill educates patients who have been misinformed about COVID-19 and vaccines and participated in the COVID Vaccine Education and Equity Project, which aims to build confidence in authorized vaccines. (covidvaccineproject.org).
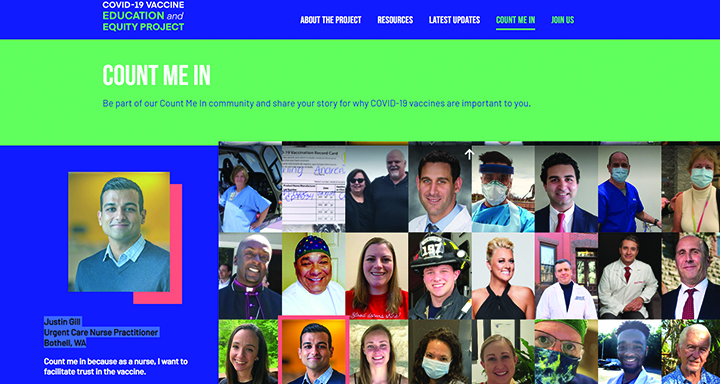

Gill tells his patients, “You’ve come here to trust me with your care, and I’m going to give you the best care available, which means telling you the truth and not telling you necessarily what it is that you want to hear.” Gill also spoke recently to CBS News, NBC News, and MSNBC about the safety of the COVID-19 vaccine.
Seeing a positive change in a patient’s health is one of Gill’s most rewarding experiences. “My ability to have an impact on that person’s life is just as important as my ability to impact a law that passes at the congressional level or the state level, or my ability to advocate for legislation that would help that patient in the long run.”
Katherine O’Brien is a freelance writer focused on health, nursing, and aging.
Resources
ANA Enterprise Nurse Suicide Prevention and Resilience web pages
(nursingworld.org/practice-policy/nurse-suicide-prevention/)
ANA Regulatory and Legislative Advocacy
(RNAction.org)

















