After undergoing radiation, Suzanne Rossi, 63, receives standard chemotherapy to treat metastatic non-small-cell lung cancer (NSCLC). When the cancer continues to progress, her oncologist switches her to erlotinib (Tarceva), a biologically targeted cancer drug. Although the drug halts further cancer spread, it triggers a severe acne-like facial rash. The doctor tells Suzanne this adverse effect indicates a good response so he’d like to keep her on the same dosage. In clinical trials, patients who developed the rash lived longer than those who didn’t.
Suzanne faces a dilemma experienced by many patients receiving a certain type of targeted biotherapy. Drugs used in such therapy affect specific receptors commonly found on cancer cells. Typically, these drugs cause fewer adverse effects than standard chemotherapy and don’t severely compromise blood counts. However, erlotinib and other agents that inhibit epidermal growth factor receptors (EGFRs) can cause an irritating skin reaction, which can be challenging to manage. In some cases, the reaction is so physically and psychologically debilitating that the patient considers discontinuing the drug despite its life-extending benefit.
Many clinicians are tempted to withhold or discontinue an EGFR inhibitor when the skin reaction appears or when they can’t control it. Yet, because the reaction correlates with a positive response, continuing the drug gives the patient the best chance to benefit from it. This article describes the current approach to managing such skin reactions.
Understanding EGF, targeted biotherapy, and skin reactions
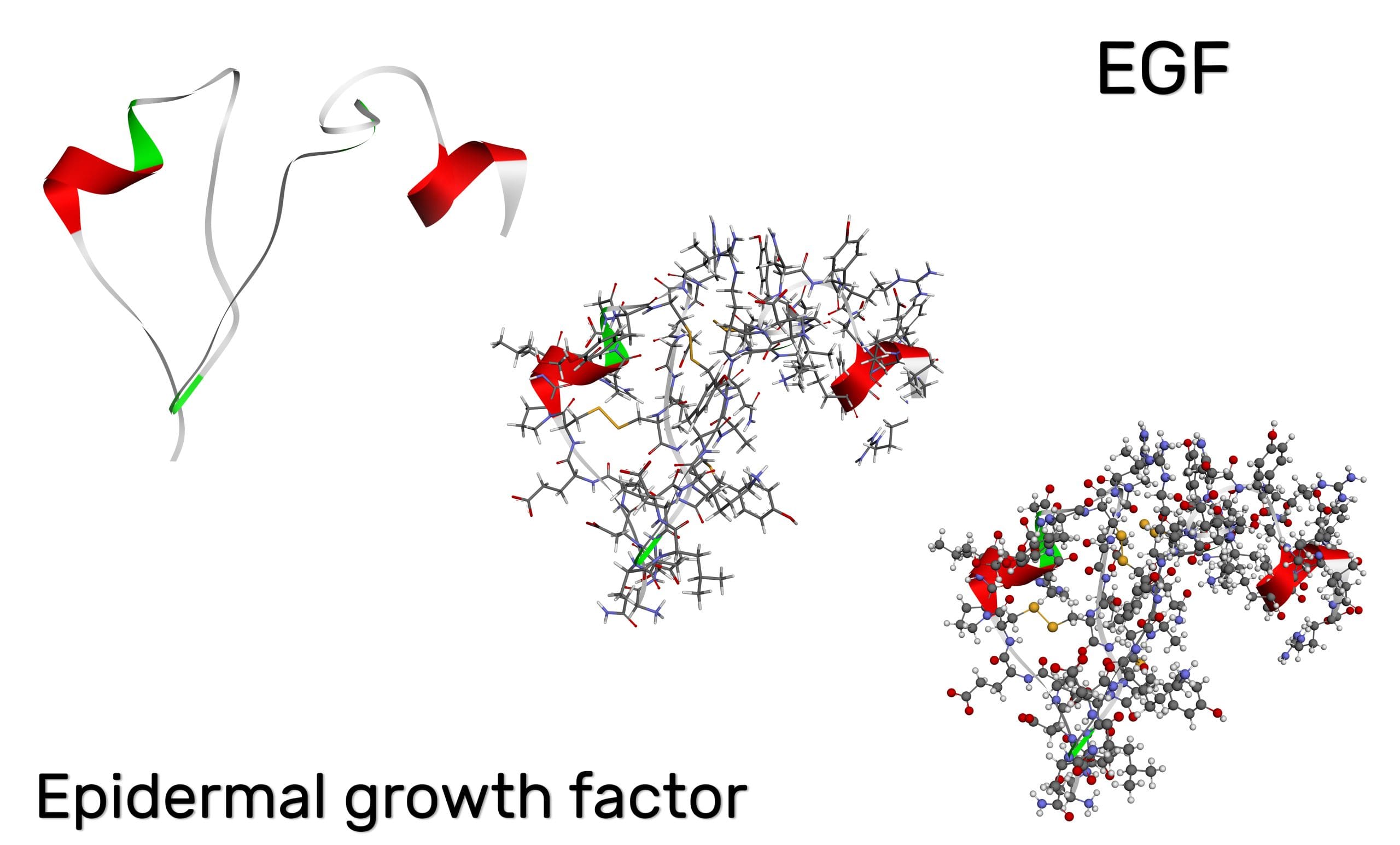
A protein, epidermal growth factor (EGF) promotes cell growth and multiplication. Cancer cells and many other cells have EGF receptors (EGFRs) on their surface. EGFR inhibitors, such as erlotinib, attach to EGFRs; researchers suspect they stop tumor growth by blocking the binding of EGF and tyrosine kinase.
Although the exact cause of the skin reaction linked to EGFR inhibitors isn’t completely understood, it may stem from an immune response to EGFR inhibition in skin tissue. The rash occurs in roughly 80% of patients receiving erlotinib, but is moderate to severe in only about 15% of cases.
Approved EGFR inhibitors for NSCLC treatment include erlotinib and gefitinib (Iressa). These drugs bind to EGFR, blocking activity at the tyrosine kinase domain inside the cell. (In contrast, EGFR inhibitors that are monoclonal antibodies, such as cetuximab, block EGFR on the cell surface, inhibiting EGF binding.)
Assessment
Typically, the skin reaction to EGFR inhibitors is a dry, erythematous, and sometimes papulopustular eruption. Most commonly, it arises on the face and neck, but it can also appear on the trunk, scalp, and extremities. The patient may complain of burning and itching, as well as anxiety caused by body image changes. Usually, the rash emerges 5 to 10 days after drug therapy starts and may last for the entire course of treatment. In my practice, I typically see it peak at week 2, last for 3 to 4 months, and then fade, leaving patches of dry skin.
Grading the reaction
To grade the skin reaction, some clinicians use the National Cancer Institute’s Common Terminology Criteria for Adverse Events (CTCAE), which provides a grading (severity) scale. However, CTCAE is mostly a descriptor and doesn’t correlate well with treatment recommendations. Designed for patients on study drugs, it rates the reaction more in terms of body surface area than intensity and subjective symptoms.
As an alternative, a grading scale based on a “best practices” model was developed in 2006 by a national team of oncologists, dermatologists, nurses, and pharmacists who are lung cancer experts. This simple model uses a grading system that includes mild, moderate, and severe categories.
Interventions
Experts recommend an anticipatory or proactive approach to preventing or managing skin reactions to EGFR inhibitors. The new grading system described above includes treatment recommendations for each severity grade, using a stepped approach. (See Treatment algorithm in the PDF offered in the download now file.)
Patient teaching
Instruct a patient who has just been prescribed an EGFR inhibitor to start using a thick, alcohol-free emollient cream twice daily, as well as a sunscreen of SPF 15 or higher (preferably one containing zinc oxide or titanium dioxide). Advise the patient to avoid sun exposure, bathe with lukewarm (not hot) water, and use a mild, fragrance-free soap. If the patient is receiving erlotinib, stress the importance of taking it on an empty stomach, because food increases its bioavailability and could lead to increased toxicity.
Not just for oncology nurses
You don’t have to be an oncology nurse to encounter patients with skin reactions to EGFR inhibitors. If you work in a dermatology clinic or a primary care setting, you may care for patients who develop the reaction while receiving one of these drugs. By knowing how to assess and intervene appropriately, you’ll increase patient comfort while helping the patient continue to receive the potentially life-sustaining drug.
Beth Eaby is a Thoracic Oncology Nurse Practitioner at the Abramson Cancer Center at the University of Pennsylvania in Philadelphia.
Selected references
Fox L. Pathology and management of dermatologic toxicities associated with anti-EGFR therapy. Oncology (Williston Park). 2006;20:26-34.
Lynch T, Kim E, Eaby B, Garey J, West D, Lacouture M. Epidermal growth factor receptor (EGFR) inhibitor–associated rash: an evolving paradigm in clinical management. Oncologist. 2007;12(5):610-621. http://theoncologist.alphamedpress.org/cgi/content/full/12/5/610. Accessed October 17, 2007.