A simple smartphone app helps reduce stress.
Providing bedside care is stressful, and finding ways to reduce that stress can be difficult in a sometimes chaotic and unpredictable environment. Research shows that meditation can be a helpful stress reducer in many settings, including hospitals and other healthcare organizations.
Our small, 204-bed community hospital has created a holistic approach to providing care for patients and staff. This approach has steadily grown over the past 2 or 3 years, demonstrated by the inclusion of several stress-reducing programs, including a shared governance structure with a policy-guided holistic care council, aromatherapy, pet therapy, attention to work-life balance, and massage chairs in each nursing break room.
We targeted brief, informal meditation using a smart phone application as another possible strategy in this effort and implemented a pilot study.
Before we began


Healthcare leaders play a critical role in creating a work environment that fosters staff well-being and quality patient care. The literature also suggests that leaders need to pay attention to three domains:
- emotional management strategies
- cognitive action strategies
- social support strategies.
During our background research, we also found a 2013 meta-analysis that compared seven studies of nurses using meditation as a stress-relief intervention. The studies included daily meditation, classes over many weeks, or multiple sessions via computer. They differed in terms of participants, variables, and method, but the general finding was that meditation could be a positive intervention. None of the studies used brief meditation or a smartphone application.
Over the past 30 years, significant work has been done related to meditation and specifically mindfulness-based stress reduction (MBSR). Jon Kabat-Zinn, PhD, author, teacher, researcher, and founder of the Center for Mindfulness in Medicine, Health Care, and Society at the University of Massachusetts Medical School is a leader in this field. His work on the value of meditation for self-care and healthy lifestyles has laid the foundation for research and growth in stress reduction related to mindfulness meditation. However, little is reported on the value of brief silent meditation specifically for healthcare providers.
What we did
For our pilot study, we chose the One-Moment Meditation (OMM) free smartphone application, which includes an optional guided 30-second warm-up, a timed 1-minute silent meditation to focus on breathing and clearing the mind, and an optional 30-second cooldown. It’s an informal way to meditate that can easily be incorporated into a daily routine without requiring a special place and time, and it can be done throughout the day as needed.
Assisted by the hospital’s Clinical Education and Research Committee, we solicited volunteers for our study. Fifty caregivers responded, including nurses, physical therapists, cardiopulmonary technicians, and team members from guest, pharmacy, and nutritional services. We met with each one and helped him or her download the free OMM app.
We developed three premeditation and postmeditation statements based on values noted in the literature:
- My thoughts are clear and organized.
- I have energy to care for my patients.
- I am feeling positive about my day.
These statements were chosen to provide an opportunity for the participants to think about how stress relief can influence and regulate their emotional state. They were asked to assess their perception of the usefulness of the meditation using a five-point Likert scale, before and after using OMM for 10 working shifts. The participants kept a log tracking their meditation and evaluation. They decided where they would meditate; some chose their car before coming into the hospital, others chose the hospital chapel, the break room, or an office area. We encouraged participants to use narratives to describe their meditation, but they weren’t required.
What we found
Forty-six of the 50 logs were returned. Six of those weren’t used because of limited information, with two participants stating “This just isn’t for me.” We used data from 38 logs. The participants included 28 RNs and 10 we defined as “others” (clinicians other than RNs). Demographics included age and years of professional experience. Little demographic difference existed between the two groups. (See Who participated?)
Who Participated?
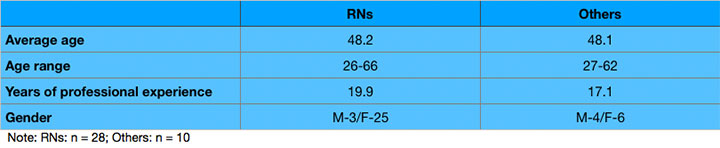  |
We evaluated the total combined scores (both RNs and “others”) and broke them out separately. (See How they scored.) Only one participant gave a low self-assessment in two of the three statements, resulting in a lower total difference for just this participant, who was in the first 3 months of employment. The participant noted that on the first day without a preceptor, both totals for statement 1 and statement 3 were lower after meditation, which resulted in a lower overall average for both statements.
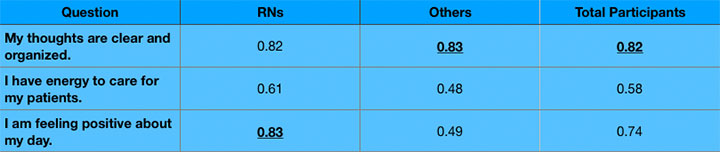
How they scored
| The following tables review the Likert scale self-scored assessment (1 = strongly disagree; 5 = strongly agree) using the three statements: (1) My thoughts are clear and organized, (2) I have energy to care for my patients, and (3) I am feeling positive about my day. The results are broken out in combined numbers (both RNs and “others”), RNs only, and “others” only. |
Combined mean total self-scored assessment—Usefulness of meditation (n = 38)
|
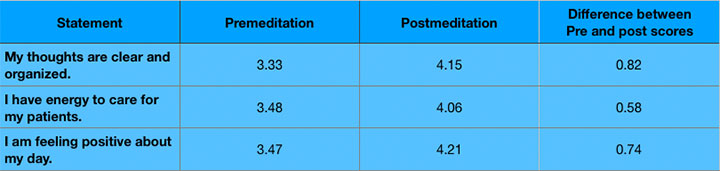
Mean RN self-scored assessment—Usefulness of meditation (n = 28)
|
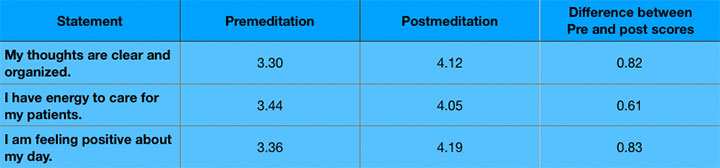
Mean “others” self-scored assessment—Usefulness of |
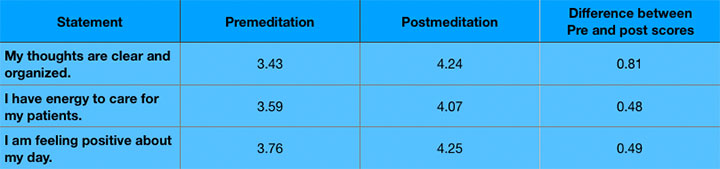
The two groups differed in their premeditation and postmeditation scores. (See How they differed.) Both the total participant group and the “other” group showed the greatest difference in statement 1 (My thoughts are clear and organized.). For the nurse-only group, statement 3 (I am feeling positive about my day.) showed the greatest difference at 0.83, with statement 3 (My thoughts are clear and organized.) was a close second at 0.82.
How they differed
| The two participant groups differed in their premeditation and postmeditation self-scored assessments, as illustrated in the table. (Bold number show the highest differences for each group.) |
  |
Thirty-three of the participants noted the value of brief meditation on multiple days after day 5. Over time, participants grew to appreciate the meditation. Two participants stated, “Not sure this helped me,” but all others noted the positive effects. Some participants wanted more meditation time, saying such things as, “It would be better if it guided you through the process.” and “I needed more than 1 minute.”
When the premeditation and postmeditation scores were compared, there was a significant difference noted in the score sets. The responses to all three questions were found to be more positive after the meditation.
We used a grounded theory approach to review the narratives, and four themes emerged:
- Positive impact of a brief meditation—Many comments reflected participant benefit from meditation.
“This minute clears the minutia from our minds.”
“I find myself retraining my brain to focus [only] on [the] present and I’ve seen the beauty around me.”
“I am attempting to have more intention.”
“My heart rate slowed and I feel more calm.” - RNs report feeling stressed—Forty percent of the RNs commented on actual/anticipated stress of the day.
“Expecting a tough day on a Monday.”
“I need to get away from my coworkers…I need to block out my coworkers.”
“The stress of the day got the best of me in the afternoon.” - Personal life issues matter—As several respondents indicated, the state of our mind is a factor in our approach to work, whether community, family, or health related:
“Personal issues going on today, this [meditation] helped me to calm and refocus.”
“So upset today about the mass shooting in California.”
“I have a sore throat.” - Meditated more frequently—As the study progressed, participants used meditation more often at home and work.
“I meditated twice today.”
“I plan to keep doing it [meditating].”
“Had a fantastic day and starting to meditate more frequently.”
How we translated the results
Reducing the negative implications of prolonged stress creates a safer work environment, reduces risk of burnout and staff turnover, and increases emotional, physical, and overall satisfaction for both staff and patients.
Jean Watson’s Theory of Human Caring supports healthcare workers taking care of themselves using the mind, body, and spirit as part of an interactive healing process for compassionate care and leadership. The attention to mindful practices can intensify the positive impact of communication, decision-making, and teamwork.
The most positive outcomes of this study were the systemic implications for educators and nurse administrators, including acknowledging the extreme and persistent nature of stress on nurses and other healthcare professionals; promoting organizational environments that emphasize a holistic approach to health and stress management; and transforming stress into therapeutic techniques that can be practiced by all team members.
What’s next?
Further objective review may help expand this research. For example, we could evaluate participant performance, absenteeism, and error rate. Or we could look for evidence of physical change, such as cortisol levels. This was a small study; we would like to expand it across multiple hospitals to collect data to validate the outcomes.
Helping nurses thrive
We want nurses and other healthcare professionals to thrive, not just survive, in the stressful, ever-changing corporate landscape of healthcare. Mindfulness, which uses motivators such as self-awareness, body stretching, and meditation to stimulate discovery, can help healthcare workers focus on the here and now rather than expending valuable energy on the future or past. They can use meditation to ground themselves, nurture inner thoughts and emotions, and maintain self-control, helping them properly manage personal and occupational stress.
Donna Linette is the nurse manager for behavioral health services at Broward Health Imperial Point in Fort Lauderdale, Florida, and adjunct faculty at Florida Atlantic University in Fort Lauderdale. Jamethan Bryant is a clinical educator in ICU/PCU/IVR at Broward Health Imperial Point.
Selected references
Ball J, Pike G, Griffiths P, Rafferty AM, Murrells T. RN4CAST Nurse Survey in England. June 2012. National Nursing Research Unit. kcl.ac.uk/nursing/research/nnru/publications/Reports/RN4Cast-Nurse-survey-report-27-6-12-FINAL.pdf
Burke M. Managing work-related stress in the district nursing workplace. Br J Community Nurs. 2013;18(11):535-8.
Dunlop J. Meditation, stress relief, and well-Being. Radiol Technol. 2015;85(5):535-55.
Farquharson B, Bell C, Johnston D, et al. Nursing stress and patient care: Real-time investigation of the effect of nursing tasks and demands on psychological stress, physiological stress, and job performance: Study protocol. J Adv Nurs. 2013;69(10):2327-35.
Kabat-Zinn J. Mindfulness meditation: What it is, what it isn’t, and its role in health care and medicine. In: Haruki Y, Ishii Y, Suzuki, M, eds. Comparative and Psychological Study on Meditation. Delft, Netherlands: Eburon; 2007: 161-170.
Lim MH, Chow YL, Poon E. Evaluation of meditation programmes used by nurses to reduce stress: A literature review. Singapore Nurs J. 2013;40(3):11-20.
McIntosh B, Sheppy B. Effects of stress on nursing integrity. Nurs Stand. 2013;27(25):35-9.
One Moment Meditation. onemomentmeditation.com
Walinga J, Rowe W. Transforming stress in complex work environments: Exploring the capabilities of middle managers in the public sector. Int J Workplace Health Manag. 2013;6(1):66-88.
Watson J. Theory of Human Caring. Watson Caring Science Institute.




















1 Comment.
I am writing in response to the article entitled Managing Stress in Health Care with Meditation: Got a Minute? Written by Linette and Bryant in the October 2017, volume twelve, number ten. This article discussed the impact a brief meditation could have on stress in the workplace for the bedside nurse. I was extremely impressed and inspired after reading this article. I have a great appreciation for holistic care and enjoyed reading an article about its application to nursing. Nurses deal with many stressors during a workday and having strategies to manage that stress is imperative. The purpose of my letter is to offer additional research I have found regarding another holistic approach to stress that is realistic for nurses and also to share my plans to apply this on my own unit.
One aspect of this article I greatly appreciated was how feasible a brief meditation is for a busy nurse. I was moved by the results as almost all nurses who participated felt it assisted in improving their stress and wanted to continue the practice of meditation. It led me to reflect on some of the practices on my unit. I work on a medical surgical floor and we have taken many holistic approaches to care in regard to our nurses and also the patients. One recent addition to our unit practices is diffusing essential oils in each foyer. Essential oils have endless benefits but one main use is for the reduction of stress. This practice, like the brief meditation, is very practical for a bedside nurse; it involves very little prep time and has been proven to reduce stress. An article published in Asian Pacific Journal of Tropical Biomedicine entitled Essential Oils Used in Aromatherapy: A Systemic Review, discusses many essential oils and their benefits. It lists some common oils used for stress which include lavender, chamomile, ylang ylang, eucalyptus, orange, and many more. All have been found to be very beneficial for stress, are natural, and have little to no negative side effects.
Your article inspired me to discuss the findings of Linette and Bryant’s study to my own unit in hopes that it could be something our nurses utilize for stress management in the workplace. I would like to thank you for posting this as it brings more awareness to the non-pharmalogical options to stress for nurses. The stress nurses deal with in the workplace is real and very underappreciated. There are many other complementary options available and I hope to see more of this topic posted in the future.
Sincerely,
Vanessa Tatum, RN