MPD preparation is the first step in the journey.
Editor’s note: This is an early release of an article that will appear in the October 2021 issue of American Nurse Journal.
Takeaways:
- Magnet® program recognition that validates nursing excellence and superior patient outcomes is a critical focus for all hospitals.
- Many Magnet program director (MPD) orientation programs rely on checklists that provide only cursory onboarding of this important role.
- Migrating toward competency-based orientation and onboarding cultivates an autonomous, self-paced learning environment.
American Nurses Credentialing Center (ANCC) Magnet® designation recognizes healthcare organizations for patient care and nursing excellence as well as innovative nursing practice. Organizations on the Magnet journey need a dedicated Magnet program director (MPD) to successfully lead them toward designation and ensure they maintain it. ANCC guidelines for the MPD position state that organizations must appoint a single source of communication and contact for the process. However, no specific published requirements for the role exist.
MPD onboarding and orientation can be challenging because it’s a single role within the organization and the previous MPD may no longer be present to ensure a smooth transition. Organizations frequently promote staff who exhibit strong leadership skills, but may lack knowledge of the Magnet components and standards. To ensure MPD and Magnet submission success, organizations should develop a detailed orientation program.
MPD role
As of March 2021, 552 Magnet facilities represent approximately 9% of U.S. hospitals. However, many more hospitals may be actively pursuing Magnet designation and have a formal MPD responsible for overseeing the program.
Serving as an MPD can be overwhelming, especially if no one else in the organization has experience in the role. Some states and regions have consortiums for networking, some healthcare systems have former and current MPDs who support and mentor one another, and the Magnet website includes guidance resources, including a new MPD checklist. Recently, robust discussion on private Magnet listservs have focused on the need to create and share a formal MPD orientation competency for successful onboarding.
Developing a new MPD competency model
MPD orientation at our 12-hospital healthcare system in the mid-Atlantic used a standard checklist of tasks, information, and data sources. It included reviewing the current Magnet manual and website, data collection tools, clinical benchmark and nursing and patient satisfaction vendors, nurse-sensitive clinical indicators, document preparation, professional practice domains (care delivery models, professional practice model, shared governance structures), nursing research activities, and site visit logistics. The checklist had been updated over the past decade to meet changing Magnet requirements.
To align with the Magnet model components within transition to practice, we saw an opportunity to advance MPD orientation from a checklist focus to a competency-based outcome assessment.
Literature review
We started with a literature review (using the key words “Magnet program director,” “competency,” and “orientation”) to guide our development of a new MPD orientation and competency tool. Little literature on the MPD role and innovative competency-based orientation models exits. Martin and Holskey, however, note that MPD succession planning has an impact on data collection, shared governance, mentoring, operations, document preparation, and site visit coordination. Lavin’s description of the role includes the ideal structure for reporting to the chief nursing officer and its importance in cultural development and as an organizational change catalyst. A 2015 survey by Winslow and colleagues noted that one-third of MPDs in Virginia indicated they received no formal orientation. Most were self-taught.
Collaboration
MPDs and education leaders within the health system, representing nine Magnet-designated organizations, collaborated to transform the checklist into a competency validation tool. We based the new tool design on the Martin and LaVigne Nurse Development Resources® Benchmark, a standardized, evidence-based tool for assessing and documenting a transitioning nurse’s readiness to practice.
The new MPD competency tool uses a design that promotes progression toward independence and incorporates concepts from current nursing competency theorists. It also includes the fundamental Magnet components (transformational leadership, structural empowerment, exemplary professional practice, new knowledge, innovations and improvement, and empirical outcomes) and familiarity with the Magnet manual and Magnet website resources. In addition, we integrated several competencies from the American Organization for Nursing Leadership (AONL), including communication, knowledge, leadership, professionalism, and business skills.
The tool defines each benchmark through an overarching competency outcome statement that’s supported by purpose-driven objectives and defined by actions and activities for achieving independence. It also includes suggested verification methods. (See Benchmark overview.)
Benchmark overview
The Magnet® program director competency tool sets the following benchmarks:
• Demonstrate an overall understanding of Magnet and its impact within the organization.
• Demonstrate transformational leadership qualities by instilling vision and guiding nurses to embrace change for improved outcomes.
• Facilitate and promote shared governance structures to endorse a culture of structural empowerment.
• Model and influence professional nursing practice development to promote exemplary professional practice.
• Advocate for integration of nursing research and evidence-based practice to promote outcome improvements and new knowledge innovation.
• Navigate (access, review, retrieve) and analyze data from locations and repositories necessary to support empirical outcomes.
Validating competency
This migration toward competency-based onboarding cultivates an autonomous, self-paced learning environment that preserves the subject-matter expert dynamic required for MPD success. To address the lone position of most MPDs, the competency tool was designed with independent accountability in mind. The MPD validates their own competencies for each Magnet domain using standard orientation processes, benchmarks, and myriad other strategies (See Competency validation.)
Competency validation
The Magnet® program director competency tool uses a variety of methods to assess competency and validate completion of orientation benchmarks. Here are some of them:
• case studies
• direct observations
• evidence of daily work
• exemplars
• group discussions and demonstrations
• mock events/surveys
• monitoring and reviewing reports or documentation
• peer review
• performance reviews
• presentations
• return demonstrations
• self-assessment
• simulation
• teach-back
• tests/quizzes/exams
• verbal feedback.
The MPD’s supervisor monitors the completion of the overall process and periodically evaluates the MPD until they can function independently. (See Magnet® Program Director competency tool: Empirical outcomes.)
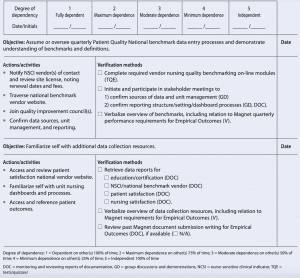
Magnet® program director competency tool: Empirical outcomes
This sample of a competency tool is for empirical outcomes. The competency outcome statement is: The Magnet Program Director navigates (accesses, reviews, retrieves) and analyzes data from locations and repositories necessary to support empirical outcomes for Magnet designation.

New model success
The new tool was successfully validated by five seasoned MPDs who led multiple Magnet designation outcomes for their organizations. It’s been used to onboard several new MPD colleagues with clear focus on the leadership competencies required to successfully lead the Magnet process and the professional practice, data outcomes, and Magnet document creation.
MPDs in settings without prior Magnet experience may need to navigate their own onboarding and champion access to resources, experiences, asynchronous education, and mentorship outside of their organization.
This tool is ideal for MPDs who have a year or more before designation or redesignation. However, many MPDs are appointed less than a year before documentation submission or after submission and before the on-site visit. In those situations, using this tool may not be feasible.
Looking ahead
The MPD competency tool closes an identified gap and serves as one component of helping organizations achieve Magnet success. We’ll continue to evaluate the tool for usefulness and make modifications as the MPD role is revised and refined to meet Magnet expectations.
MPDs at our health system are finalizing plans for a formal mentorship program to complement the competency tool and help increase MPD confidence and motivation as well as support retention. Currently, mentorship is informal, but we’ve identified a need to match each new MPD with a fellow MPD, taking into account both nurses’ schedules and timelines for designation or redesignation. Our health system is large enough to provide internal mentorship, but a smaller or single hospital MPD could pursue mentorship from an MPD in another organization. In our experience, MPDs across the nation are happy to share their time and talents with others.
Magnet excellence is a journey of innovation, creativity, and best practices. Seasoned MPDs attest to the positive difference the Magnet experience has had on their own lives as well as those of their fellow nurses and patients. Setting up MPDs for success is step one of that journey.
Susan A. Winslow is the system director of professional practice and clinical education at Sentara Healthcare, Chesapeake, Virginia. Teresa E. Bilyeu is the director of patient care services/Magnet program director at Sentara Leigh Hospital in Norfolk, Virginia. Lesley A. Cook is director of nursing excellence/Magnet program director at Sentara RMH Medical Center in Harrisonburg, Virginia. Jolene J. Dorrell is system manager of education at Sentara Healthcare in Chesapeake, Virginia. Kelly A. Via is manager of professional practice/Magnet program director at Sentara Martha Jefferson Hospital in Charlottesville, Virginia. Kelly F. Winslow is manager of professional practice/Magnet program director at Sentara Princess Anne Hospital in Virginia Beach, Virginia.
References
American Nurses Credentialing Center. 2019 Magnet® Application Manual. Silver Spring, MD: ANA Enterprise; 2017.
American Nurses Credentialing Center. Find a Magnet® organization. March 19, 2021.
American Nurses Credentialing Center. New MPD checklist.
American Organization for Nursing Leadership. AONL nurse leader competencies.
Lavin PM. Boots on the ground: The role of the Magnet® project director. Nurs Manage. 2013;44(2):50-2. doi:10.1097/01.NUMA.0000426140.60785.0d
Martin B, LaVigne R. Benchmarks: An evidence-based approach to creating high performing nurses. J Health Sci. 2016;4:26-34. doi:10.17265/2328-7136/2016.01.004
Martin JA, Holskey MP. Succession planning for Magnet® Program Director. Am Nurse Today. 2013;8(9):36-9.
Winslow S, Brown K, Cook L, et al. Lessons learned by Magnet® Program Directors. Am Nurse Today. 2016;11(1):38-41.
Winslow S, Zimmerman D, Cook L, Goodloe L. Trending models of Magnet® Project Director resource allocation in Virginia. Virginia Nurses Today. 2015;23(3):14-6.
Wright D. The Ultimate Guide to Competency Assessment in Healthcare. 3rd ed. Bloomington, MN: Creative Health Care Management, Inc.; 2005.



















