Arriving back in Ethiopia for the third time after having left only four months earlier, I had many questions. Had the Ethiopian nurses managed to retain the knowledge and continue the hygiene project I had started? Had my work been sustainable?
Ethiopia is one of the poorest countries in the world. There are fewer than one physician and two hospital beds per 10,000 persons, the infant mortality rate is 67 per 1,000 live births, and the number one cause of death for all ages is infectious disease. With a literacy rate of only 42.7%, educational needs are great.
When volunteering in Ethiopia for the first time, I met nuns who had taught an entire village to wash their hands before eating. Although the nuns did not track statistics, they noted an apparent decrease in diarrhea and other enteral diseases. They demonstrated that the best way to make a difference in health and standard of living was to engage in health education and to teach self-care while working and living in the community.
Based on my experience with the nuns, I realized that one individual alone can make a difference, and I decided to return to Ethiopia.
What can one person do?
I returned to Ethiopia as a volunteer at a medical facility located in a town west of Addis Ababa with a population of about 121,000. The medical compound consists of 14 inpatient wards and an outpatient department (OPD), which includes a wound clinic, pharmacy, and laboratory.
I spent the first 2 days observing work performance, facilities, and equipment available. I then developed an intervention plan. My goal and driving motto was “teaching the teachers.” I planned to work with the health staff, make suggestions, and teach new ideas while striving to ensure sustainability. I obtained permission from the facility’s manager and involved the staff throughout the process.
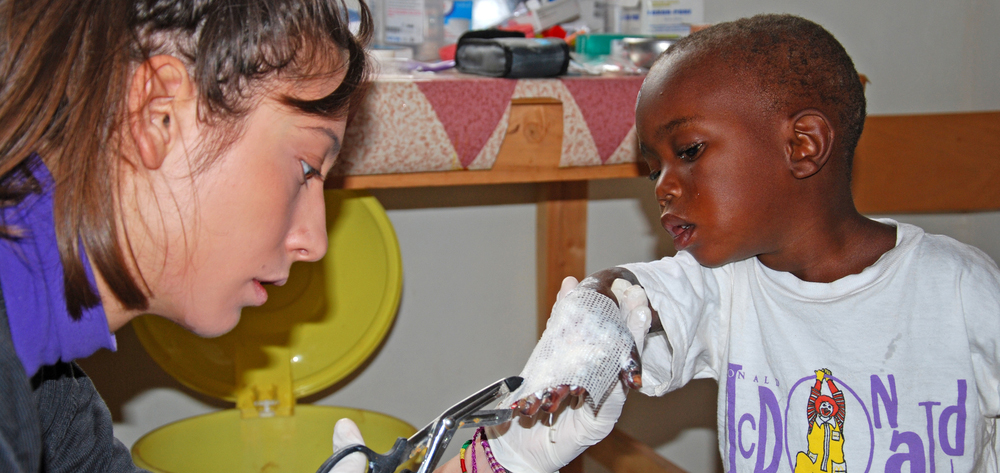
To make a real change in 3 weeks, I limited my efforts to two main projects. The first project was directed towards care of wounds, primarily animal bites, surgical wounds, burns, cancer wounds, and parasitic infections. Nurses washed and redressed all the wounds, but healing was often complicated by infections that prevented tissue repair, leading to pain and accumulation of pus in the wound.
The other nurses and I collaborated to improve patients’ knowledge of wound treatment and strengthen their confidence in self-care. We taught patients to remove the gauze, wash the wounds with soap and water, and leave them open to air until evaluation.
The second project was developed in reaction to the observation that women frequently stopped breastfeeding from one breast and subsequently developed mastitis. Many women lacked sufficient education in breastfeeding as well as female hygiene, resulting in urinary tract infections and pelvic inflammatory disease. After developing a lesson plan with the staff, I supervised two female nurses who taught the women in the compound. Experiencing teaching a class increased the nurses’ self-confidence while improving women’s health education.
During the 3 weeks I worked in the compound, I observed significant changes. Patients we had taught started teaching new patients to wash their wounds properly. Nurses who dressed the wounds could see (and smell!) the difference in the wound hygiene, and they gained self-confidence in their teaching abilities. Nevertheless, I wondered if the projects would last after my departure. Would they be sustained?
Ensuring sustainability
Returning to the compound 4 months later, I saw patients washing their wounds after taking off their bandages. The nurses taught the new patients, and the patients taught each other the correct procedure, reinforcing the knowledge gained. Furthermore, the nurses were showing greater self-confidence and understanding of the importance of teaching. During the following weeks, the nurses and I worked together to improve the lesson plans we had made on my previous visit. We also developed teaching plans on vaccinations and tuberculosis treatment. Lessons were all taught by the local nurses. To reinforce information, we made posters of the major points of each lesson in Amharic, the national language of Ethiopia, and posted them in prominent places.
Changing one simple procedure regarding wound treatment in the OPD and witnessing the results was enough to build trust in the new method. Having the nurses teach increased faith in their expanded role. Once they saw the outcome, they understood the importance of health education and were encouraged to continue.
Lessons learned
Working within an unfamiliar cultural setting required an understanding and sensitivity to new cultural knowledge. This led to appropriate caution in suggesting and planning changes. To have a significant impact, it was essential to understand the nurses’ current decision making process and take a top-down approach. Consulting with the head of the facility and obtaining her consent was critical. This approach facilitated healthy, productive relationships with both the manager and the staff.
The nurses in the compound were the ones who would continue the work in their community and teach health care skills to increasing numbers of patients over time; therefore, involving them in every step of the process was crucial to the success and sustainability of the projects.
Focusing on two projects that would show results in a short period of time proved to be a significant decision. Teaching simple hygiene accelerated the healing process. Patients exercised autonomy and used new knowledge to make decisions themselves and thus gained self-confidence. Staff-members were first-hand witnesses to these changes and therefore understood and appreciated the improvements in their work.
Healthy relations with the staff and patients, working and making decisions together as a team, and the satisfaction of seeing the results were all key factors in the sustainability of the project.
Regardless of the places nurses work or volunteer, our knowledge, the structure of our work, and the important role we play in peoples’ lives can guide us to make real changes. Health is a universal right. As nurses we can help secure that right all over the world.
Selected references
Central Intelligence Agency. The World Factbook. 2013. https://www.cia.gov/library/publications/the-world-factbook/geos/et.html.
Central Statistical Agency of Ethiopia. Census Tabular Report, Oromiya- 1. 2007.
World Health Organization. Ethiopia Factsheets of Health Statistics 2010. www.afro.who.int/en/ethiopia/country-health-profile.html
Zohar H. Morris works in community health for Clalit, one of the four national healthcare plans in Israel. She would like to thank and Judith L. Reishtein, PhD, RN, CNE, for her assistance with writing the article.



















1 Comment.
Zohar,
Congratulations to you for taking nursing and nursing education to the Ethiopian people and their nurses. You have really made a difference you may see, but also may never be aware of the total impression you have left with this community.