Nurses share a common theme: Hope.
Be prepared, be strong, and don’t panic
Crystal Davis Campbell, BSN, RN
Staff nurse, medical ICU, Vidant Medical Center
Greenville, North Carolina



Crystal Davis Campbell took time from service on the frontlines to educate school officials.
Since the beginning of the COVID-19 pandemic, Crystal
Davis Campbell has lived by this motto: Be prepared, and don’t panic.
When her teenage son began having panic attacks and was afraid to go to school, she educated him about staying safe and sent him to school with a mask. Initially, his fears were calmed, but masks and social distancing weren’t yet mandatory, and nervous school authorities told him to remove his mask.
Campbell spoke to the district superintendent and shared the facts about COVID-19 with him, other school officials, and the district’s school nurses. “Initially, school authorities thought wearing a mask would cause a panic, but once they heard me and saw the data, they changed their minds,” she says. “They realized that wearing masks would help protect our children, comfort them, and prevent panic.”
Her proactive approach resulted in a district-wide COVID-19 education program and mandatory masks and social distancing. “As nurses, we have to be aware of our role in our families and in the community,” says Campbell, who is pursuing her degree as a family nurse practitioner. “We have to be strong and proactive in crisis situations such as COVID-19.”
Campbell draws on her strength and that of her coworkers at Vidant Medical Center where she’s been a medical ICU (MICU) staff nurse for 5 years. “We have a motto there too: #MICUstrong,” she says.
The Vidant health system has been dealing with a high census of patients with COVID-19 since the beginning of the pandemic. As of January 16, 2021, they had 206 patients.
Working through the pandemic has given Campbell a new outlook on the importance of a group of people who trust one another and work well together. “We haven’t fallen apart because of the pandemic,” she says. “The pandemic has brought about more teamwork, and we have become stronger because of it. From the cleaning staff, to the nurses, to the physicians, everyone has come together. Our team is a well-oiled machine.”
Campbell, who is the chair of Vidant Medical Center’s practice council, credits the organization’s leadership. “Leadership fights to ensure we have everything we need, so we’re prepared to go to battle with this pandemic,” she says.
However, the battle isn’t without its casualties. “When we get sad, upset, or broken, when one of us is limping, we all pull together and lift each other up,” Campbell says. “We’re limping toward that finish line together.”
Campbell believes the intensified teamwork developed during the pandemic will impact the future of nursing in a positive way. A heightened awareness of self-protection and self-care also will be a boon to nurses and their patients. “Nurses are exceedingly giving, but this experience has taught us that we have to remember to protect and care for ourselves,” Campbell says.
In response to the stressful demands of the pandemic, Vidant Medical Center created a staff sanctuary where nurses and staff can take a break, enjoy music and coffee, and rejuvenate. The sanctuary has been a godsend for busy staff. “In the future, we’ll be able to nurse harder and nurse further because we’ve learned how to protect and renew ourselves, which makes us stronger,” Campbell says.
Nursing at a small hospital with big COVID-19 challenges
Marie Sheppy, RN
ICU charge nurse, San Mateo Medical Center
San Mateo, California


Marie Sheppy has worked at San Mateo Medical Center for 31 years. It’s a small public health, safety-net hospital with a seven-bed ICU. Early in 2020, as word spread about the upcoming COVID-19 pandemic, Sheppy considered retirement.
“It seemed a good time to retire, but I was concerned about what would happen to my coworkers if I left, so I stayed,” she says. “We all look out for each other, and I understand their fears and needs because I’ve worked beside them for so long.”
As part of the leadership team, Sheppy attended a command center, which included all the hospital departments. The team spent hours pre-planning to enhance the organization’s pandemic emergency response. “We didn’t know much about the disease yet, and we were frightened,” she says. “It felt like a scene in a war movie. We were all gathered with laptops, white boards, and people on speaker phones to plan our pandemic strategy—and that was just the beginning.”
The response strategy evolved almost continuously to address the rising demands on the staff and hospital resources. By August 2020, the U.S. Department of Health and Human Services had identified San Mateo Medical Center as one of the hospitals experiencing a disproportionate intensity of COVID-19 admissions.


Policies and procedures have changed weekly, daily, and even hourly in some cases to keep up with patient and staff needs. Implementing rapidly evolving policies effectively requires a hospital-wide effort.
“My team has worked hard to keep pace and adapt, but we are tired, and it hasn’t gotten any easier,” Sheppy says. “My ICU family has kept me going, and everyone works together from the top down to ensure staff and patients are safe. I’ve been impressed by management’s ability to provide us with equipment and supplies, keep us updated on Centers for Disease Control and Prevention recommendations, and offer counseling when the staff needs it. Seeing the managers work so hard has been an inspiration to staff.”
Another critical aspect of care is to provide education to patients’ families about the seriousness of COVID-19. Despite education, working with families who aren’t allowed to visit loved ones has been a challenge. “It’s been very difficult for some families to understand the restrictions unless they’re healthcare workers themselves,” Sheppy says.
Sheppy believes the pandemic has shown how essential nurses are to the healthcare system and that we’ll care for our patients, no matter the situation. “I think nurses are more resilient now and are adapting and moving forward, knowing there is hope. I hope that this experience will inspire future nurses to see the difference they can make.”
Sheppy has faced difficulties within her own family due to the pandemic. Last year, her youngest son’s hockey playoffs and high school graduation were cancelled. He had a makeshift graduation in August, but none of the family who live in Canada could attend. He also had to start his freshman year at the University of California, Berkeley, online and missed out on the dorm experience.
A day after the hockey playoffs were cancelled, Sheppy had to move her middle son out of his dorm at the University of California, Los Angeles. A week later, her oldest son, a Peace Corps member, was evacuated from Kyrgyzstan. He’s safely home now but is struggling to find a job.
“Everything changed so quickly,” Sheppy says. “We’ve felt cheated and isolated at times, but I also feel blessed. My kids are home and safe and healthy, and this experience has made both my family and my work family stronger.”
The upside of a challenging time
Shannen Kane, BSN, RN, CEN, SANE
Clinical nurse IV, emergency department, University of North Carolina (UNC) at Chapel Hill Medical Center
President, Heart of Carolina Chapter of the Emergency Nurses Association


Shannen Kane, who’s been an ED nurse for 2-1/2 years, sees the positives coming out of this challenging time. “The most positive experience of the pandemic has been watching the teamwork we value so much in the ED amplify in our department and throughout the entire hospital,” she says. “We all have a shared understanding that this is a very difficult time and of what we’re all going through. We know we’re there for each other, and we’re all trying to make work a bit easier across all of the units.”
UNC Medical Center ED is a Level I trauma center with 94 treatment spaces. The heightened demands on this busy trauma center during the pandemic have tested the nurses’ abilities to turn on a dime. Kane has been heartened to see the staff adopt and run with sudden process changes quickly and flawlessly. “In the ED, we’re used to change and not knowing what’s coming through our doors, but isolating patients with COVID-19 and triaging in a tent outside was new for us,” she says. “The experience has brought us together.”
Kane believes that this shared experience will lead to even stronger teamwork and better support of each other, both in the ED and across the hospital. “This kind of bonding and teamwork is going to stay with us, leave a lasting impact on nursing and how healthcare works, and shape our nursing careers forever.”
The relentless stress of working in the ED during the pandemic can take a toll on nurses. “As ED nurses, we’ve had to get creative to develop hobbies and activities that distract us from the demands and stress of the pandemic,” Kane says. “We’re constantly talking and thinking about COVID-19 at work, and it can be hard to disconnect from it at home.”

To disengage from the pandemic, Kane has reconnected with the interests and hobbies she loves, including hiking and being outside. “This has been a huge positive for me,” she says. “Taking the dog out and exploring new trails has given us so much joy and a sense of peace and normalcy.”
Kane is grateful for the extra time she’s had with family at home. “Our time together is precious, and I don’t take it for granted. I appreciate being home and the time spent with family.”
She also values the technology that has allowed her to stay connected with friends and family she hasn’t seen for weeks or months. This was especially significant during the holidays, and she fondly remembers a family video call on Christmas. “Because of technology, we might even be talking to each other more than we did before the pandemic,” Kane says.
Kane believes that COVID-19 solidifies the high level of trust the public has in nurses already. She’s seen an outpouring of support and many expressions of gratitude from the community, including food donations, handwritten thank-you notes, and shout-outs on social media.
“Knowing the community truly trusts and supports us is priceless,” Kane says.
At one point, the ED nurses felt like they were getting so much recognition that they wanted to ensure the nurses on the COVID-19 unit were acknowledged as well. They recruited a local restaurant to donate food to one of the units, and the ED nurses and staff sent them a poster with supportive and encouraging messages.
“Because of the pandemic, the community has a better understanding of what nursing is, what we do, and our values,” Kane says. “We’re now fielding a lot of questions about the vaccine, and I’m seeing how people truly value nurses’ opinions and perspectives. I think this will continue long after the pandemic.”
A role in research and new treatments
Christin Vaskas, BS, RN, CCRN
Nurse clinician, surgical ICU, New York University (NYU) Langone Health
New York City, New York
Guest lecturer, NYU Rory Meyers College of Nursing


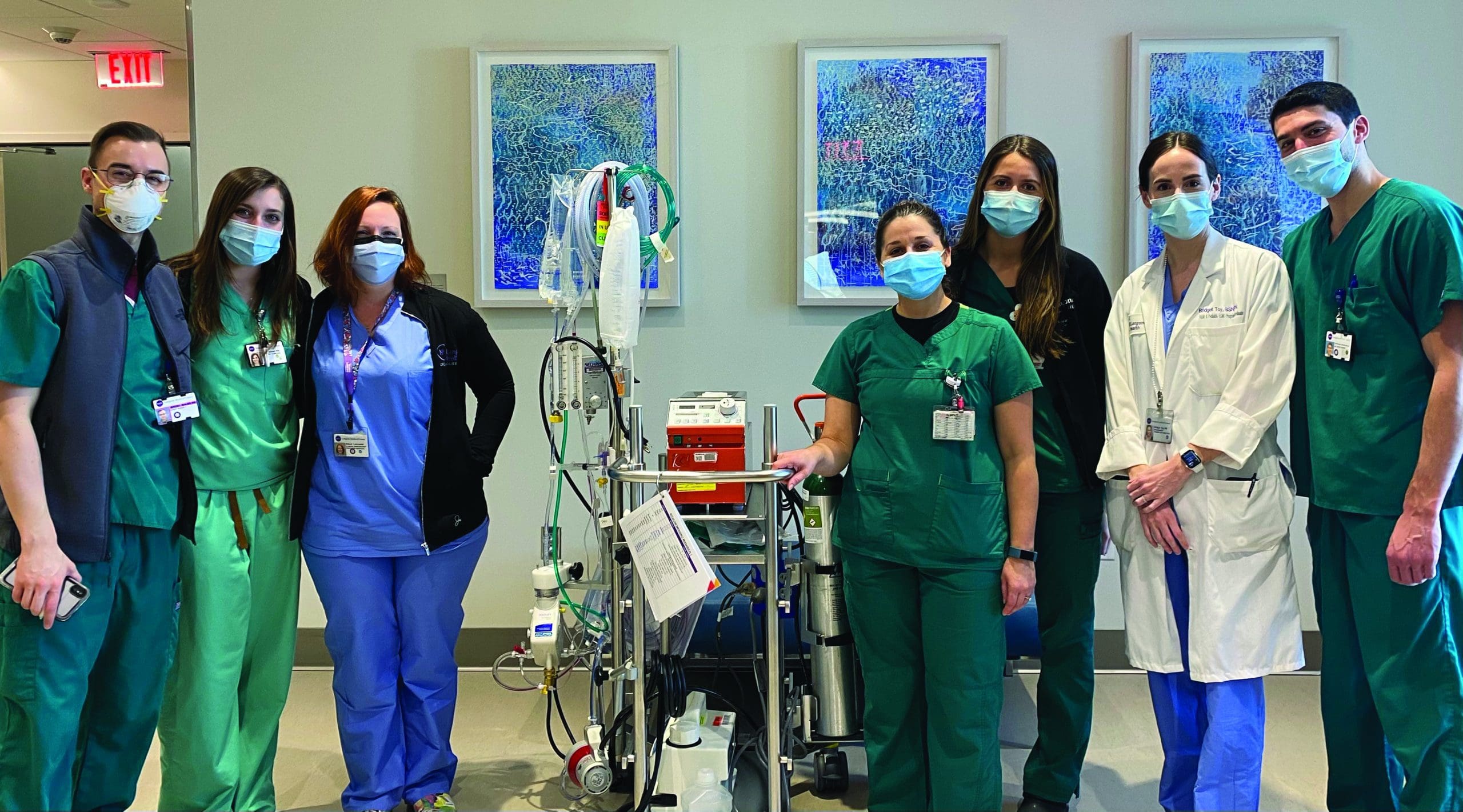
Christin Vaskas is proud to have been one of the nurses who cared for critically ill patients enrolled in the study by Kon and colleagues on extracorporeal membrane oxygenation (ECMO) support in severe cases of COVID-19. The participating patients, who required intubation and ventilation, received ECMO, which pumps blood outside the body to a heart–lung machine that removes carbon dioxide and returns oxygen-filled blood. The study found that 96% of the patients survived over a 44-day period.
Vaskas was excited about her role in the study because ventilated COVID-19 patients usually have a mortality rate as high as 88.1%, according to a study by King and colleagues.
“Caring for these patients and seeing them go home energizes me to go back to work every day and do more for patients,” Vaskas says.
ECMO is a complex treatment for nurses to manage and has serious risks, including stroke and bleeding complications. The study patients required long periods of top-notch nursing care to prevent and manage complications. “Many of these patients were on ECMO for longer than we’d seen before, as long as 4 months,” says Vaskas, whose background includes cardiothoracic ICU.


One of her patients woke up in August after 4 months on ECMO and believed it was still spring. The last thing he remembered was leaving for work one morning in April before he passed out.
Supporting these patients’ recovery, mentally and psychologically, remains a critical aspect of their nursing care. “When patients wake up after weeks or months and don’t remember anything, it sits heavy on my heart. So much of their life is gone,” Vaskas says. “Helping patients adjust and fill in the long gap in their lives showed us how important what nurses do is.”
Throughout the pandemic, Vaskas also has seen an increase in camaraderie among nurses and other providers from all levels of healthcare. “Everyone has been in this together and gotten to know each other on a deeper level. We work together in an equitable way, and everyone’s input is valued,” she says. “The more we build personal relationships, the better we are as a team.”
Outside work, Vaskas has faced the challenge of living in the biggest U.S. city and an early epicenter of the pandemic. “It’s been difficult living in New York City because we don’t have many outdoor options,” she says. “The trade-off we normally make is easy: We live in tiny apartments, but we live in this amazing city with so much to do. But those options have been cut drastically or have disappeared. COVID-19 has taught us how to appreciate a simpler life with our families and to be grateful for that time together.”
Vaskas says one good thing that’s come out of the pandemic is a heightened recognition of the skills of nurses. She hopes that in the future nurses will continue working to their maximum capabilities with the maximum respect from colleagues and the public. “We’re in the patient rooms and are the eyes and the hands for the rest of the team,” she says. “We’ve truly shown the world what we’re capable of.”
Confronting fears and seizing victories
Debra Packard, RN
Multidiscipline nurse, biocontainment unit and step-down
isolation ward, Halifax Health Medical Center of Daytona
Daytona, Florida




Debra Packard will never forget her first day of work on the COVID-19 biocontainment unit at Halifax Health Medical Center of Daytona. “I was so scared that I put on my respirator too tight and it created indentions and pressure points on my face,” says Packard, who’s also a preceptor for new nurses. “We were all scared because we didn’t know what we were facing at the beginning.”
Packard has been a nurse for 16 years and has a diverse nursing background, including ICU, medical psychiatric care, and pediatrics. Her skills led her to the role of preceptor and multidiscipline nurse. As such, she works where she’s needed within the hospital, in particular, the COVID-19 biocontainment and step-down isolation units.
After that first day, Packard’s fears quickly took a back seat to helping the sickest patients and their families deal with the harsh realities of the disease. The most moving experience she had was when a family chose to take an end-of-life patient off bilevel positive airway pressure (BiPAP) and put him on a nasal cannula. “He was healthy and playing golf in July, got COVID-19, and could never kick it,” she says.
As soon as the BiPAP was discontinued, he began to die. Packard remained in the biocontainment room when his wife told him she loved him and said good-by via a video call. “Normally, we give families privacy to be together in these situations,” she says. “It was heart-wrenching to see a wife have to say good-by to her husband over video.”
When the numbers of COVID-19 patients needing hospitalization dropped over the summer, the isolation step-down unit closed. The patients from both units occupied the biocontamination unit. One patient who was transferred from the step-down unit had the opportunity to see his sister, who had been on a ventilator, before she passed away. Then his condition deteriorated, and he was intubated. His prognosis was grim because he had type I diabetes, but he recovered and was eventually discharged. “We were bursting with joy and so excited for that one victory,” Packard says. “It was wonderful to see that we were doing something good.”
Packard and other nurses she works with face many smaller challenges that make giving care more complex. “Even going to the bathroom or taking a meal break is a challenge because you have to go to a special room and disrobe completely from the personal protective equipment (PPE) and then put it all back on,” she says. “Wearing PPE for 12 hours is difficult. It’s hot, and we’re often sweating.”
Packard also has had to cope with fear and anxiety in her personal life. “In the beginning of the pandemic, people were afraid of me because I was working in the COVID-19 unit, and my husband and son were terrified for me because so little was known about the disease,” she says.
Packard also was concerned for the safety of her family. She and her husband, who has diabetes, decided he would move into a different bedroom as a precaution. She also decided not to visit her grandson, who has asthma, and missed many family events. “Their safety was my priority,” she says. “It’s been hard and has hurt the family, but it has gotten better as understanding of how to stay safe has evolved. Now we’re not as afraid as we were, and I’ve been able to safely visit my daughter and grandkids. In the end, the experience has made us closer.”
Catherine Spader is a freelance writer based in Littleton, Colorado.
Sources
King CS, Sahjwani D, Brown AW, et al. Outcomes of mechanically ventilated patients with COVID-19 associated respiratory failure. PLOS ONE. 2020;15(11):e0242651. doi:10.1371/journal.pone.0242651
Kon ZN, Smith DE, Chang SH, et al. Extracorporeal membrane oxygenation support in severe COVID-19. Ann Thorac Surg. 2021;111(2):537-43.doi:10.1016/j.athoracsur.2020.07.002


















2 Comments.
Thank God we can write about it. At a point when the heat was on, I thought we are all probably going to die. You read messages about the end times .
I can identify with writers. The heat, noise from the vents created was a lot.
I must say thank you to ANA for provision of safe place after work. The hotels helped a lot. I washed off and double bagged my close to take directly to the laundry .
I add that every profession is a call to duty. I love nursing and even though I’m a full time school nurse, I stay at bedside because I want to keep my skills. It came in handy because when covid came, my job left .
I was asked to go to New York for a contract which I almost did but lost a very dear friend to same covid. It was devastating. I couldn’t leave my children.
Most interestingly my family was afraid for me but I was really enthusiastic. All I asked for was PPE. I tell my contract person with my agency it is being in the military. At least that’s how I feel. Save lives.
And yes nurses matter. Most respected profession.
Being a nurse educator I feel proud. This unprecedented Covid-19 pandemic situation made the whole world understood how important the nurses are in providing care to the people, how great their contribution is to manage this situation. The Nightingale Oath which the nursing students take during their course have an impact on their mind to serve the people in need whatever the situation is, the students said. I hope this pandemic situation will uplift the nurses dignity to all the nations as they observed their role, dedication and commitment to serve the people.