Innovation and coordination are keys for success.
As authorized COVID-19 vaccines are being distributed across the nation, RNs are leading rollout administration, coordination, and education efforts. The strategy for getting “shots in arms” varies by state with the aim to vaccinate all Americans as quickly and safely as possible to turn the tide on the course of the pandemic.
In Kentucky, Ruth Carrico, PhD, DNP, APRN, CIC, professor at the University of Louisville School of Medicine, her colleagues, and volunteers are administering about 2,000 COVID-19 vaccines per day at LouVax, a mass vaccination drive-through clinic in Louisville’s Broadbent Arena.
Drive-through vaccine clinics were considered “off the wall” when the university held one providing influenza vaccination in 1994. “Many thought no one would want to get a vaccine in their car or at the grocery store, but the drive-through events proved otherwise,” said Carrico, a Kentucky Nurses Association member.
This early experience meant that when H1N1 hit in 2009, the university was ready. They gave 20,000 vaccines in 18 hours via a drive-through clinic set up at a football stadium on campus. This event also demonstrated the important role student nurses could play in community response efforts. Through LouVax, nursing students, who have had difficulty identifying clinical rotations during the pandemic, are able to participate in all aspects of mass vaccination, including vaccine handling, administration, and patient education.




Dawn Balcom (R) at a mass vaccination center in Louisville, Kentucky.
Broadbent Arena, a large indoor facility known for sporting and other big-audience events, provides easy access and ventilation systems able to support a large-scale indoor vaccination process. Providing vaccinations to individuals in automobiles allows for those seeking immunization to remain isolated. “We must ensure the safety of not only the vaccine recipients, but also our volunteers, and the vaccines themselves,” Carrico said.
Carrico has shared Kentucky’s vaccination plan with other states through the National Association of City and County Health Officials and has made LouVax materials available in a shareable folder for access and use. (bit.ly/3sGYtk0) “Collaborating with your state nurses association, your health department, and nursing schools really expands the reach,” said Carrico, who also serves as director of the University of Louisville’s Center for Education and Training in Infection Prevention.
On another front, in West Virginia, community-based clinics have been instrumental in getting COVID-19 vaccines distributed efficiently and safely throughout the states’ rural geography. The state’s Joint Interagency Task Force (JIATF) for COVID-19 Vaccines asked each of its 55 counties to develop a local leadership planning team. “Each week, every county gets an allocation of shared doses,” said Deborah Koester, PhD, DNP, MSN, RN, an assistant professor and director of the division of community health at the Joan C. Edwards School of Medicine at Marshall University in Huntington, who serves as deputy on the JIATF. It’s then up to the county’s local team to get those doses administered at their community vaccination clinics. They’ve been able to administer 100% of those vaccines every week.
“The people on local planning teams know their communities the best, and their communities trust them,” Koester said. She believes that West Virginia’s success is due to its unique structure and strategy, trusting community health departments to get the vaccines to the people in their counties and very rural geographies.
Communication and coordination
In her role on the task force, Koester performs at a systems level with liaisons for other key stakeholders such as community health centers, hospitals, schools, pharmacies, and emergency management. Onsite she coordinates with the National Guard, the Department of Homeland Security, West Virginia Health and Human Services, West Virginia Board of Pharmacy, West Virginia Hospital Association, and West Virginia Primary Care Association.


“We’re working in tandem and everything is aligned,” Koester said of the large team at Yeager Air National Guard Base in Charleston, which meets for strategic planning and operations every day at 10 am and 2 pm.
Koester supported coordination of West Virginia’s response across the state with its 48 local health departments. She prepared by working with local health department testing, contact tracing, case investigation, public education, and local businesses, until the state got the vaccines in December 2020.
Meanwhile, Carrico and her colleagues, including Dawn Balcom, DNP, FNP-C, a Kentucky Nurses Association member, arrive at Broadbent Arena at 6 am 5 to 6 days a week to set up the operation. They spend the day training and supporting volunteers, troubleshooting, and working alongside public health partners. Balcom, who’s a travel and vaccine specialist at the University of Louisville’s Vaccine and International Travel Clinic, developed several communication processes, including a sign system to help easily communicate needs across the huge arena. The signs, attached to dowel rods, have pictures indicating what the volunteer needs, whether it’s assistance with a vaccination, help with the computer system, questions regarding vaccines or vaccination procedures, or mechanical assistance with one of the cars in line.
Reaching everyone who needs a vaccine presents a challenge. Carrico’s team is working with local public health to identify other ways to make the systems for vaccination at LouVax available to those who may not be able to drive themselves. Public health partners are working on other approaches that focus on areas in the community experiencing poverty, those with language and cultural differences, and groups traditionally vaccine hesitant.
At the end of the day, the team works with public health leadership to make any leftover doses of vaccine available to the volunteer workforce. Carrico and Balcom then go home and answer questions via email and phone and hold conference calls with other communities seeking to replicate the Louisville process. Then the cycle starts all over again the next day.
“It’s not a sprint, it’s a journey,” Carrico said.
Building vaccine confidence
Reliable information from trusted sources is critical to combat vaccine misinformation and to increase COVID-19 vaccination confidence among healthcare professionals and the public.
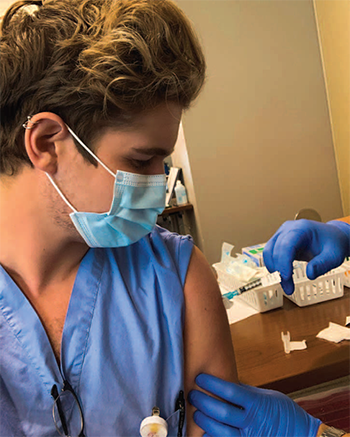

Luke Velickoff, BSN, RN, a cardiovascular ICU nurse at a tertiary hospital, began working at a free clinic in Clarksburg, West Virginia, in October of 2020. “I wanted to have a broader impact on the community,” he said, and felt he could do that in primary education and prevention. He and his clinic colleagues provide vaccine education and dispel myths about vaccination.
“Nurses are highly trusted in our community,” said Velickoff, a West Virginia Nurses Association member. “People see us and know us, so it’s important to make ourselves available (for education and outreach), especially when we have COVID-19 patient experience.”
In January, Velickoff joined a vaccine work group made up of healthcare professionals and community leaders from agencies that are part of the JIATF, including the West Virginia Department of Health and Human Resources (DHHR), and the West Virginia Center for Rural Health Development, to disseminate consistent, factual, and scientific resources regarding COVID-19 and the vaccines.
As part of this effort, he made a video chronicling his experience getting the COVID-19 vaccine, describing his mild side effects, and explaining some of the science behind the vaccine. The video has gotten almost 10,000 views through his own social media and the DHHR rollout, according to Velickoff.
Ahnnya Slaughter, MSN, RN-C, CNS-BC, systems redesign and improvement manager at the VA Long Beach Healthcare System in Long Beach, California, was concerned about vaccine hesitancy in the Black community. She collaborated with her facility’s public relations department to put together an information session as part of a weekly interactive wellness broadcast hosted by a large African American church in Los Angeles. Experts, church leaders, and congregants discussed concerns about the vaccine.
Slaughter, an ANA\California member, reported that the session was well received, with strong engagement. The same church later coordinated with the state of California to set up a vaccination site.
Nationally, the American Nurses Association (ANA) has joined other organizations to build vaccine confidence through educational campaigns. ANA has participated with the American Hospital Association and the American Medical Association in communications to encourage healthcare workers to be vaccinated and in public service announcements asking the public to “do their part” by getting vaccinated, handwashing, wearing a mask, and physical distancing.
The Ad Council and the COVID Collaborative, of which ANA is a part, launched the COVID-19 Vaccine Education Initiative, which includes a video series designed to address healthcare professionals’ questions about COVID-19 vaccination, featuring ANA President Ernest Grant, PhD, RN, FAAN, and ANA board members. A second component seeks to inform the public about the vaccines (getvaccineanswers.org). Grant is also featured as part of the “Count Me In” campaign and WSNA member Justin Gill and PSNA President Tarik Kahn are on the Count Me In Photo wall on the site: covidvaccineproject.org/countmein.
In addition, the COVID Vaccine Facts for Nurses site was developed by 19 nursing organizations, including ANA and the American Nurses Foundation, and is sponsored by Johnson & Johnson, and ANA regularly updates the vaccination pages on its COVID-19 Resources site at nursingworld.org/coronavirus.
Leading and educating
“At our local level, public health nurses have had the opportunity to become community leaders,” Koester said. “They are the voices in vaccine education, whether it’s at community health centers, at hospitals, on social media, in interviews they’re doing, or in public education announcements.” Koester holds calls for West Virginia nurses and administrators every day at 4 pm. Facilitating those calls is another way for nurses to lead, she said.
Velickoff believes it’s important for nurses to enhance their visibility in leadership roles during the pandemic. “My effort has been in education, in making sure the vaccine is available to people, and ensuring that people are comfortable receiving the vaccine,” Velickoff said.
A glimmer of hope
The availability of COVID-19 vaccines is helping some nurses see a light in what’s been a very dark time.
“Nurses are, to say the least, very tired, and I’m hearing a sense of hope—hope that we can finally start getting a handle on this pandemic that has caused such devastation,” Velickoff said.
“I do it with joy,” said Carrico, of the long hours and hard work at LouVax. “At the end of the day, we want to feel like our work makes a difference in our communities—both serving and leading.” Balcom agrees. “I’m so proud to have had the opportunity to be a part of this,” she said.
Even the most hopeful nurse leaders know there’s a long road ahead. “Every day, our director asks us ‘Have you done everything you can to save a life today?’” Koester said. “And every day we say no. Because there are still people dying.”
Nurses have provided valuable leadership during the public health crisis, and Koester believes that it’s lifting up nursing as a whole. “There’s a huge opportunity from a nursing perspective to connect across states and learn from each other, identifying best practices and innovations,” she said. In the future, she hopes that nurses can make time to work together to keep these innovations moving forward.
— Elizabeth Moore is a writer at ANA.














1 Comment.
Good article. They should really be the first one and other health care front liners since they are the one who has close contact with the patients of Covid-19.