Collaborate and advocate to meet patient needs and implement policy change.
Takeaways:
- Older adults have increased vulnerability to the effects of climate change because of greater exposure to the impact of climate change as well greater susceptibility due to aging-associated changes.
- Nurses have an opportunity to help older citizens prepare for the impact of climate change in their practice and through advocacy efforts in their communities and beyond.
- The impact of climate change on older adults can be addressed with mitigation efforts designed to reduce the underlying causes of climate change and adaptive strategies consisting of secondary preventive efforts designed to reduce the impact on health.


IN 2015, an estimated 8.5% of the world’s population was 65 years and older; that number is expected to double by 2050 and total 1.6 billion people. The World Health Assembly has named 2020-2030 as the decade of healthy aging, and the World Health Organization is developing a framework for helping people live long and happy lives by focusing on individuals’ functional abilities and their physical and social environments.
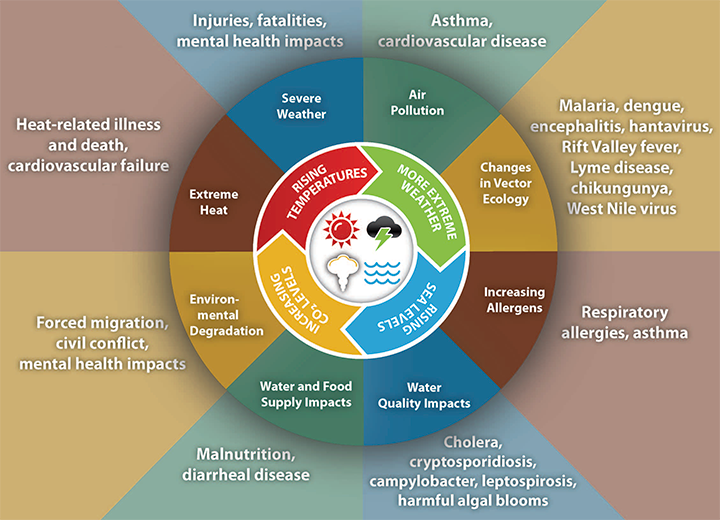
The aging in population is occurring as the effects of climate change are increasing. (See Impact of climate change on human health.) For example, heat waves have included death tolls in the thousands (Europe, 2003, 71,310; Russia, 2010, 55,736; Europe, 2006, 3,418; India, 1998, 2,541 and 2015, 1,826+) that disproportionately affected older adults. Nurses must understand the connection between global environmental changes and older adults’ health. Current environmental trends require vigilance and specific strategies to protect the health of this vulnerable population.
Impact of climate change on human healthEnvironmental risks to health include weather (temperature extremes, storms, floods, wildfires, tornadoes, cyclones), exacerbated vector-borne disease, compromised agriculture (poor soil and food quality, plant diseases), compromised water quality, and decreased habitability of population centers because of sea-level rise, air pollution, violence, and conflict. Populations vulnerable to climate change include anyone living within or near areas:
Source: Centers for Disease Control and Prevention. Climate effects on health. 2014. cdc.gov/climateandhealth/effects |
Aging and climate change
Healthcare systems aren’t prepared to address the coming impact of climate change and the needs of older citizens, who are at risk of high rates of chronic disease, limited access to healthcare and medication during a crisis, respiratory distress during temperature increases, poor diet and nutrition, reduced access to water, and higher poverty rates in some settings. In addition, during a climate crisis, older adults (even those with limited access to food and water distribution centers) may give their meager supplies to family members.
A 2018 study by Kishore and colleagues of Hurricane Maria’s aftermath in Puerto Rico indicated that there were 4,645 more deaths than would ordinarily have been expected during that time period and that this number was most likely underestimated. The median age of those who left and didn’t return or were missing was 25 years, compared to 50 years for those who died or stayed; one-third of deaths were related to delayed or interrupted healthcare. Disruption to healthcare services included inaccessible medications (14.4%), loss of electrically powered respiratory services (9.5%), closed healthcare facilities (8.6%), absent physicians (6.1%), and inability to reach 911 services (8.8%).
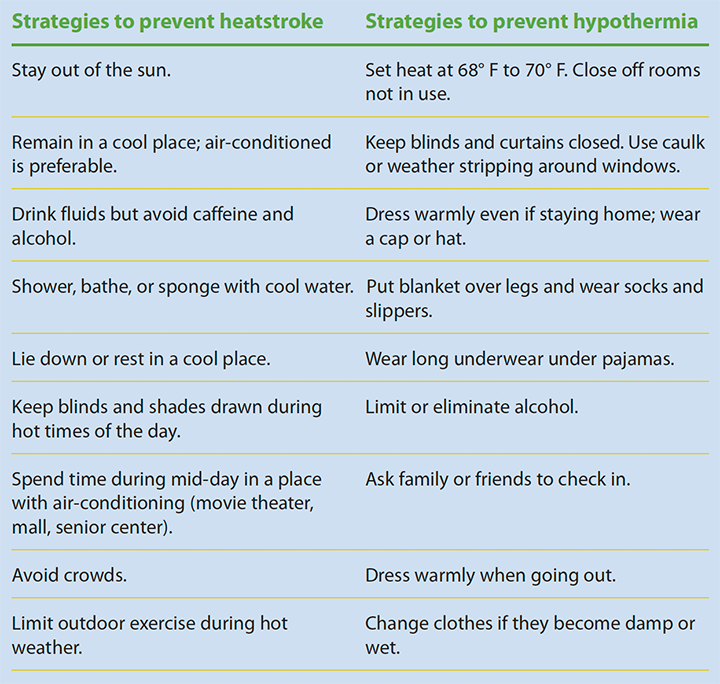
Common physiologic changes associated with aging make older adults particularly vulnerable to the effects of global climate change. These changes include reduced ability to regulate body temperature, changes in sweating, reduced sense of thirst and awareness of dehydration, decreased cardiac reserve, decreased respiratory muscle strength and vital capacity, decreased immune response, reduced mobility, and cognitive changes. The potential for a range of climate effects on older adults is broad and complex and includes temperature extremes, vector-borne illnesses, storms, financial loss, extended allergy seasons, pollution, and disasters. For example, extreme heat may result in heatstroke and extreme cold may lead to hypothermia.
Older adults’ vulnerabilities to climate change are exacerbated by poverty, polypharmacy (or extended lack of access to medication), and limited social networks.
Social impact of climate change
Older adults also face social risks associated with aging, including isolation, lack of family or social support, and poverty. Women living alone are most at risk. Older adults may be left behind in war zones and face the risk for violence and injuries. Social inequalities are exacerbated in the presence of environmental stressors. Various environmental, behavioral, lifestyle, and socioeconomic effects interact.
Mitigation and adaptive strategies
Addressing older citizens’ needs requires an approach that includes mitigation and adaptation.
Mitigation strategies focus on reducing the underlying causes of global challenges to health by reducing human contributions to the greenhouse effect. Because the healthcare sector also contributes to greenhouse emissions, efforts should be extended to decreasing healthcare facilities’ carbon footprint, decreasing the amount of travel needed to obtain healthcare services or medication, reducing medical waste, and expanding green space in cities where more heat is generated. Several groups provide tools and guidance in advocating for mitigation strategies. Health Care Without Harm (noharm.org) has a global focus, and HelpAge (helpage.org) focuses on strategies to ensure that older people’s rights are addressed.
Adaptive strategies focus on secondary prevention to reduce the impact of global climate change on health. They address built environment, community services, protective policies, and education for older citizens and their caregivers. Older adults may have limited ability to adapt to global climate changes, so they may need additional services to assist with implementing adaptive strategies. (See Adaptive strategies for secondary prevention efforts.)


Nursing actions
Nurses have a long history of focusing on the environment when implementing health-promotion strategies. You can play an integral role at several levels: in your own family, through direct patient care, and in your communities and beyond to prevent health marginalization and deterioration in vulnerable older citizens.
Assess and recommend
Much of the data and publicity about the risks of climate change and the elderly are focused on mortality, but weather extremes have an impact on older adults’ day-to-day lives. You can help older adults prepare for and manage mobility restrictions and social isolation that may occur. Think about the specific effects that older adults are likely to experience in your own community (winter storms, heat waves, hurricanes, tornadoes, flooding, air pollution, wildfires) and consider how they might restrict normal daily activities. Start with a needs assessment of vulnerable adults within your own family and use the results to develop recommendations for those in your practice. Focus on individual capacity; relationships with family, friends, and the community; and the community’s infrastructure.
Encourage older adults to conduct a self-assessment with one of the many available online toolkits. (See Resources for older adults.) Completing an assessment can contribute to raising risk awareness for older adults who don’t consider themselves to be susceptible to the effects of climate change. Some of the most vulnerable older adults may not have access to or the ability to use internet resources, so download these toolkits and review key features of preparedness with them.
Advocate and volunteer
Be an advocate within your healthcare organization and community for policy changes that include implementing climate change mitigation and adaptation strategies. Take measures to ensure that older patients are well-informed about climate risks to health, and work with your organization’s leadership to include pertinent questions on health histories, post visible signage about climate change health risks, and share written literature. (See Adaptive strategies for extreme temperatures.)
Serve as a champion to address needed changes in the built environment, planning for community services, and advocating for the implementation of policies that protect workers, including older adults. And serve as an early-warning system by alerting public health officials when you see unusual changes in patterns of illness that might be attributed to climate (for example, increased respiratory illnesses in the summer months). From a broader policy perspective, you’re ideally positioned to examine the social service infrastructure available in your community. For example, does community have a heat wave response plan? Learn about the parameters for its activation, the media communication plan, daily checks for at-risk older adults, transportation to climate-controlled community centers, and the preparation of emergency and urgent care center staff.
Volunteer with local social service or government agencies to serve as a responder during a disaster. At a more macro level, you can participate in efforts to address policy implications of global climate change (for example, advocating for a national smoke health warning system and emergency services for at-risk older adults). You also can work to implement policies to lift restrictions on prescription refills in the face of an impending emergency or participate in developing a plan to address extreme heat or cold events. Identifying the potential stumbling blocks that older adults may face in an emergency will facilitate preparedness and enhance safety.
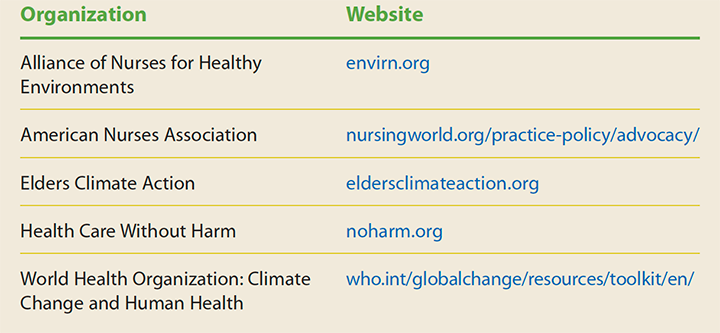
Partner with older adults and others by joining advocacy groups to adopt climate mitigation strategies in your community. Advocacy groups can include diverse stakeholders such as nurses’ organizations (e.g., state nurses associations, special interest groups), healthcare professional groups, elder advocacy groups, single-issue groups, and local and national environmental organizations. (See Advocacy resources.)
Deliberate effort, meaningful change
According to the 2015 Lancet Commission report on Health and Climate Change, responding to climate change could be the “greatest global health opportunity of the 21st century.” That response, when caring for older adults, requires a concerted collaborative effort that begins with addressing individual patients’ needs. Advocate for thoughtful planning and implementation of mitigation and adaptive strategies to meet the needs of this vulnerable population. And engage in deliberate efforts to institute meaningful policy changes to ensure a sustained response.
Margarete L. Zalon is professor of nursing and director of the online MS in health informatics program at the University of Scranton in Scranton, Pennsylvania.
Clarke PJ, Yan T, Keusch F, Gallagher NA. The impact of weather on mobility and participation in older U.S. adults. Am J Pub Health. 2015;105(7):1489-94.
Conlon KC, Rajkovich NB, White-Newsome JL, Larsen L, O’Neill MS. Preventing cold-related morbidity and mortality in a changing climate. Maturitas.2011;69(3):197-202.
Filiberto D, Wethington E, Pillemer K, Wells NM, Wysocki M, Parise JT. Older people and climate change: Vulnerability and health effects. Generations. 2010;33(4):19-25.
Haq G, Gutman G. Climate gerontology: Meeting the challenge of population ageing and climate change. Z Gerontol Geriatr. 2014;47(6):461-7.
He W, Goodkind D, Kowal P. An Aging World: 2015—International Population Reports. United States Census Bureau.2016. census.gov/content/dam/Census/library/publications/2016/demo/p95-16-1.pdf
Kishore N, Marqués D, Mahmud A, et al. Mortality in Puerto Rico after Hurricane Maria. N Engl J Med. 2018;379(2):162-70.
Kretschmer M,Coumou D, Agel L, Barlow M, Tziperman E, Cohen J. More-persistent weak stratospheric polar vortex states linked to cold extremes. Bull Am Meteorol Soc. 2018. journals.ametsoc.org/doi/10.1175/BAMS-D-16-0259.1
Masters J. Earth’s 5th deadliest heat wave in recorded history kills 1,826 in India. Weather Underground.com blog. May 29, 2015. maps.wunderground.com/blog/JeffMasters/earths-5th-deadliest-heat-wave-in-recorded-history-kills-1826-in-ind
Patz JA, Grabow ML, Limaye VS. When it rains, it pours: Future climate extremes and health. Ann Glob Health. 2014;80(4):332-44.
Stotz A, Rapp K, Oksa J, et al. Effect of a brief heat exposure on blood pressure and physical performance of older women living in the community—A pilot-study. Int J Environ Res Public Health. 2014;11(12):12623-31.
Watts N, Adger WN, Agnolucci P, et al. Health and climate change: Policy responses to protect public health. Lancet.2015; 386(10006):1861-1914.
Watts N, Adger WN, Ayeb-Karlsson S, et al. The Lancet countdown: Tracking progress on health and climate change. Lancet. 2017;389(10074):1151-64.
World Health Organization. 10 Priorities Towards a Decade of Healthy Ageing. 2017. who.int/ageing/WHO-ALC-10-priorities.pdf