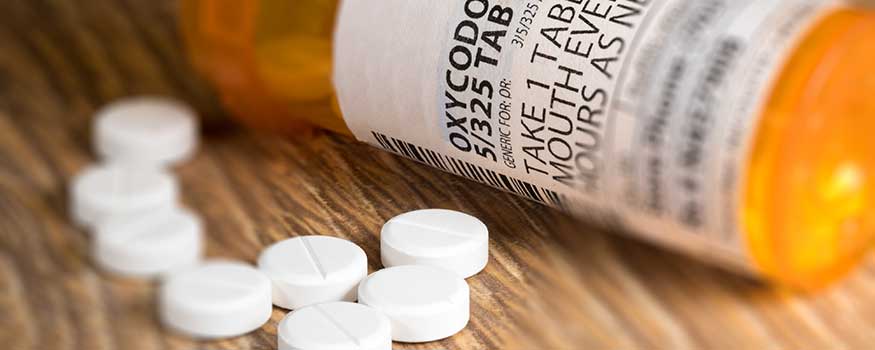
When Tom Smith* finds his mother Mary, age 59, extremely sleepy and difficult to awaken, he calls 911. The emergency medical technician (EMT) notes a prescription bottle labeled oxycodone IR (immediate release) 30 mg. While she’s in the ambulance, Mrs. Smith experiences respiratory distress and the EMT administers 0.4 mg naloxone** I.V., which results in improved breathing and alertness.
After Mrs. Smith arrives at the hospital, her emergency department (ED) nurse Susan notes her vital signs: blood pressure 130/84 mm Hg, heart rate 110 beats/minute, respiratory rate even and unlabored at 16 breaths/minute, oxygen saturation 94% on room air, and temperature 98.8° F (37.1° C). During the assessment, Mrs. Smith is alert, restless, and complaining of left shoulder pain.
History and assessment hints
To learn more about Mrs. Smith’s situation, Susan asks the standard drug screening question, “How many times in the past year have you used an illegal drug or used a prescription medication for nonmedical reasons, for instance because of the experience or feeling it caused?” Mrs. Smith says she doesn’t use any drugs, but that she takes a prescribed pain medication. When asked about alcohol use, Mrs. Smith reports that she does not drink any alcohol because of her medications.
Mrs. Smith’s son provides additional history about a shoulder fracture and surgery 4 months ago. He tells Susan that Mrs. Smith takes oxycodone for pain and has unsuccessfully attempted to decrease the medication.
In further conversation, Mrs. Smith tells Susan, “I might have taken some extra pills this morning and dozed off.” When Susan asks why she took extra medication, Mrs. Smith says she overexerted herself the day before and was in more pain than usual. Susan asks Mrs. Smith if she’s done that before and Mrs. Smith says, “Never.”
Education and follow-up
Susan is aware that the recent opioid epidemic reflects a combination of the use of illegal opioids such as heroin and a dramatic increase in prescription opioids to treat chronic noncancer pain. Before Mrs. Smith and her son leave the ED, Susan instructs them in the five essential steps for preventing overdose deaths: 1) call for help; 2) check for signs of overdose such as sleepiness, inability to awaken, blue or purple fingernails or lips, and breathing difficulty; 3) provide rescue breaths as needed; 4) administer naloxone; and 5) monitor response. Susan teaches Mrs. Smith’s son rescue breathing and reviews the Substance Abuse and Mental Health Services Administration Opioid Overdose Prevention Toolkit, available from the Substance Abuse and Mental Health Services Administration.
Susan recommends that Mrs. Smith follow up with her prescribing physician for assessment. In the meantime, Susan suggests other pain-management techniques such as heat and ice, electrical stimulation, or nonopioid medications.
Outcome
The administration of naloxone effectively reverses Mrs. Smith’s unintended opiate overdose. Intravenous naloxone has a rapid onset of action, but it also can be given intramuscularly, subcutaneously, or as a nasal spray. It’s available as an auto-injector for emergency use in the home or other nonmedical settings. Diluting I.V. naloxone with normal saline ensures more accurate dosing.
Mrs. Smith’s vital signs stabilize after the naloxone. However, naloxone has only a 30-minute half-life in some patients, so it may have to be readministered. Susan monitors Mrs. Smith for several hours to ensure that the opioids are completely metabolized and don’t pose any additional risk.
Deborah S. Finnell is a professor and Christine L. Savage is adjunct professor, both at Johns Hopkins School of Nursing in Baltimore, Maryland.
*Names in clinical scenarios are fictitious. **United States federal agencies such as the Substance Abuse and Mental Health Services, Office of National Drug Control, and the Food and Drug Administration have endorsed the use of naloxone to prevent opioid-related deaths.
Selected References
American Nurses Association. The opioid epidemic: Addressing the growing drug overdose problem. ANA IssueBrief.
Centers for Disease Control and Prevention. Injury prevention & control: Opioid overdose. Understanding the epidemic. Updated December 16, 2016.
Harm Reduction Coalition. After care. Overdose response.
Harm Reduction Coalition. Recognizing opioid overdose.
Substance Abuse and Mental Health Services Administration. SAMHSA opioid overdose prevention toolkit. Revised 2016.