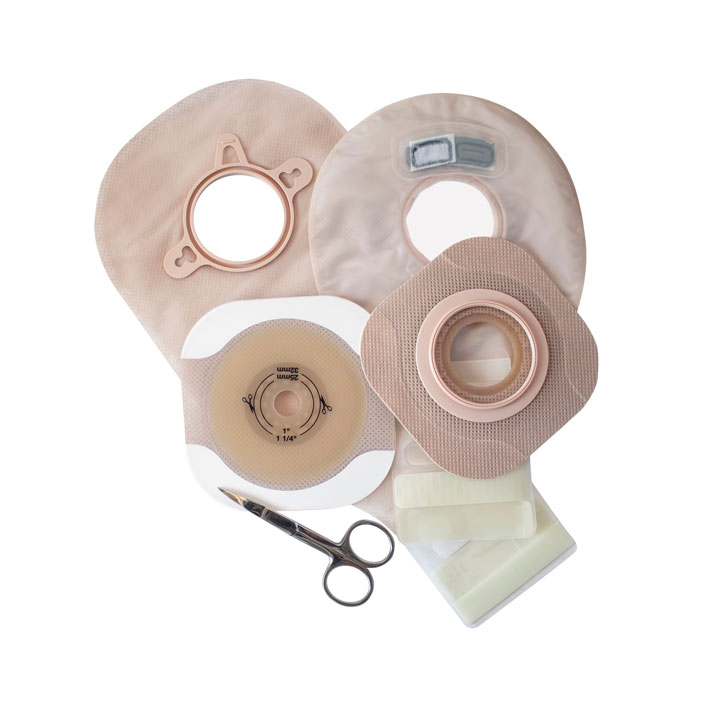
Overview of ostomy care and management
Takeaways:
- Ostomies save lives and improve patients’ quality of life, but stigma about odor and interference in daily life still exist.
- Focus patient education on proper ostomy care, including pouch changing, recognizing signs of an unhealthy stoma, and troubleshooting leaks and odor.
- Consulting with certified ostomy specialists can help ensure proper inpatient care and patient education.
Several myths about ostomies exist, including that they’re malodorous or messy, they interfere with daily activities and hobbies, and they limit quality of life. However, for most patients, ostomies improve quality of life, and for some they’re life savers. Education (beginning in the pre-operative period through discharge into the community and beyond) can address myths, reduce stigma, and provide support to all patients as they learn how to care for and manage their ostomy.
Ostomy defined
An ostomy is a surgical procedure that creates a stoma (opening in the abdomen) to reroute the usual path of urine or stool as it exits the body. After most ostomies, the patient wears a pouch over the stoma to collect waste. Some people may receive a continent diversion, which eliminates the need for a pouch.
Ostomies, which are named based on their location, may be performed to address issues related to various conditions, such as cancer, bowel diseases (including Crohn’s disease and diverticulitis), obstructions, birth defects, incontinence, and spinal cord injury. They can be temporary or permanent. Three of the most common types are colostomy, ileostomy, and urostomy (or ileal conduit). (See Ostomy types.)
Ostomy types
The following three types of ostomy are the most common:
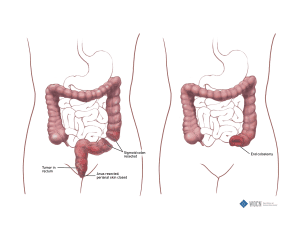
Colostomy
• Location: left lower quadrant, right lower quadrant (if transverse)
• Output: thick or pasty

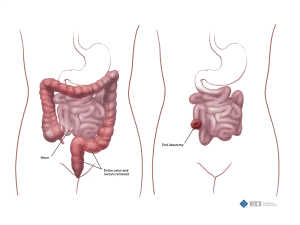
Ileostomy
• Location: right lower quadrant
• Output: thin or loose

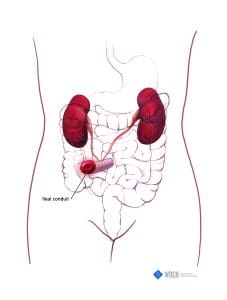
Ileal conduit (urostomy)
• Location: right lower quadrant
• Output: urine

Images courtesy of the Wound, Ostomy and Continence Nurses Society.
Colostomies can be ascending, transverse, descending, or sigmoid. The type of colostomy depends on why it’s needed. Most transverse colostomies are located in the right upper abdominal quadrant, whereas sigmoid or descending colostomies are located in the left lower quadrant. The patient’s anatomy and intraoperative findings guide stoma location, which may be atypical in some situations. Output (consistency, frequency, odor) also is related to the type of ostomy and location. Colostomies typically have a more formed or pasty output and odor may be a concern, but it can be addressed with odor-elimination drops.
Ileostomies generally are located in the right lower quadrant (depending on anatomy and intraoperative findings). They’re created by bringing the end of the small intestine (ileum) out through the abdomen during stoma creation. Ileostomy output may be thinner compared to that of a colostomy, which can result in dehydration, especially in the postoperative period.
As its name implies, an ileal conduit uses the ileum as a path to divert urine. This relatively simple surgery has a low rate of complications. Urologists typically create ileal conduits, whereas general or colorectal surgeons create colostomies or ileostomies.
Other types of ostomies are beyond the scope of this article. A thorough patient history, exam, and review of surgical notes can help you determine the type of ostomy present and any modifications you may need to make in terms of patient care or education.
Pre-operative considerations
Pre-operative ostomy education and marking by a certified ostomy nurse (formerly known as an enterostomal therapist or nurse) or trained surgeon or provider ensure optimal location and prepare the patient for stoma care. If an emergency requires an ostomy procedure, this preparation may not be possible.
In 2014, the American Society of Colon and Rectal Surgeons and the Wound, Ostomy, and Continence Nurses Society collaborated on a stoma site–marking position statement. This strongly endorsed and widely shared document reinforces the importance of pre-operative education and ostomy site marking by a trained clinician to reduce complications. It details stoma site selection and the procedure for pre-operative marking.
Some people grow up with an ostomy while others require the surgery as adults. Each situation is unique and requires an individualized nursing care plan and education based on specific patient needs.
Ostomy and pouch care
Ostomy pouches (appliances), which come in various shapes and sizes, are placed over the stoma to collect rerouted waste. Certified ostomy nurses help to determine the most appropriate pouching system based on patient need, body shape, lifestyle, and ostomy type. Pouches typically are changed twice weekly and as needed for leakage. (See Changing an ostomy pouch.)
Changing an ostomy pouch
Less is more with ostomy care. To eliminate extra steps and reduce the chance of errors, use only the needed supplies (avoid unnecessary accessory products).
- Wash hands with soap and water and prepare supplies (disposal area for old pouch, cleaning supplies, cut new pouch out if it’s not pre-cut). Cut the skin barrier (the area of the pouch that adheres to the abdomen) one-eighth of an inch larger than the stoma to avoid trauma and to protect the peristomal skin from complications such as moisture-associated skin damage caused by a leaky pouch.
- Remove and dispose of the old pouch.
- Clean peristomal skin with non-lotion soap and water. Soaps with lotions or perfumes may interfere with the pouch seal or cause peristomal skin irritation. Rinse and dry well.
- Apply protective barrier powder or skin barrier film, based on pouch type and peristomal skin condition, if directed by the certified ostomy nurse. Place skin barrier paste (or ring) directly on the peristomal skin or on the cut edge of the new pouch, whichever works best for the individual patient’s pouching technique.
- Apply the new pouch to clean, dry skin. Hold a warm hand over the new pouch for a few minutes to create a good seal. To allow the seal to set, avoid any immediate bending, lifting, and exercise.
Remind patients that they can decide who knows whether they have an ostomy. Many resources and tools exist for increasing patients’ quality of life and to conceal the pouch when desired (for example, during intimacy, sports, and swimming).
Pouches should be emptied when they’re one-third to half full. They also can be “burped” when they contain air or gas. Two-piece pouches can be partially disconnected from the skin barrier at the top to release air. For one-piece pouches, the closure device (clamp or Velcro) should be removed to release air from the bottom. Some pouches have filters, which a provider may recommend based on a patient’s needs. Most filters are made from charcoal and provide added protection against odor while allowing a slow release of gas from the pouch. Getting the filter wet may deactivate it. Many pouches come with small stickers to place over the filter to protect it during bathing.
Before discharge, ensure the patient understands the appearance of a healthy stoma (beefy red, moist, and with the presence of output from the stoma itself) vs. one that may require further assessment (dusky, dark red, or dry). Lack of or a significant decrease in output also requires provider evaluation. All patients with an ostomy should be able to change and empty the pouch independently. (See Healthy stoma.)
Healthy stoma
A healthy stoma is red, moist, and shows signs of output. The photograph below shows a viable budded stoma.
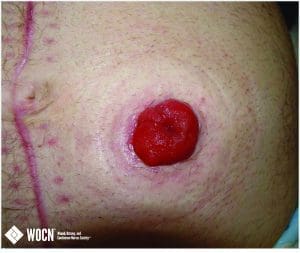

Image courtesy of the Wound, Ostomy and Continence Nurses Society.
Independence before discharge can reduce repeat emergency department (ED) visits and promote a better quality of life. Engage the patient’s support system based on the long-term capabilities of the patient or specific concerns in the immediate post-operative period. Also ensure patients have supplies ordered at discharge, resources in place, and access to a home healthcare nurse and certified ostomy nurse for support when returning to the community. The United Ostomy Associations of America (UOAA) provides resources and support groups, some of which meet virtually.
Troubleshooting leaks and odor
Early clues that a pouch may be getting ready to leak include itching or burning of peristomal skin, odor, or lifting of the skin barrier edges. Leaks can’t be taped or patched; the entire pouch should be changed to avoid peristomal skin irritation or inadvertent removal of the pouch. Common causes of pouch leaks include cutting the pouch too big or too small, skin folds or stoma within a skin fold, and weight gain or loss (stoma size could change).
The back of the skin barrier can provide insight into the cause and location of a leak. Examine the pattern on the back of the skin barrier when it’s removed. Do you see signs of wear and tear? Are some areas of the hydrocolloid wafer losing more integrity than others? Does the patient have a skin barrier ring (especially for stomas that may produce caustic effluent, such as high-output ileostomies)? Do you see signs of early barrier wear (thinning, completely worn away)?
Leaks can result in moisture-associated skin damage, which can be treated by cleansing with non-moisturizing soap and water then rinsing and drying. Protective barrier powder applied to the skin can help absorb moisture and enhance healing. (Patients should use only powders or skin barrier films recommended by an ostomy nurse.) Avoid alcohol-based products, which may result in pain and further skin damage. For severely denuded skin, dispense powder onto gauze and then apply to the skin. Expelling the powder from the container directly onto the skin may cause pain or a burning sensation. Soft convexity of the back of the ostomy skin barrier can aid conformity to body contours, minimize pressure, and improve the seal in a skin fold. (See Skin damage.)
Skin damage
The image below shows denuded peristomal skin caused by moisture-associated skin damage (reddened, open area above
the stoma) as a result of a pouch being cut too large.
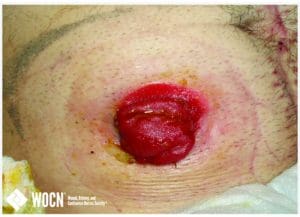

Image courtesy of the Wound, Ostomy and Continence Nurses Society.
Ostomy belts provide added support to prevent leaks. Hernia belts, which can be custom-made for patients with a parastomal hernia (a postoperative complication), also aid leak prevention.
Odor
Odor can impact quality of life for patients with ostomies, especially when traveling or in public. Defecation or flatulence via the anus frequently results in odor. However, ostomies may have unpredictable elimination patterns also accompanied by odor. Odor-reducing drops can be dispensed directly into ostomy pouches. Room sprays and deodorizers may be helpful when a patient is out or has an unexpected leak.
Diet
Dehydration is common in patients with a new ostomy who are learning new body patterns and fluid/electrolyte balance. It’s also a common complication after ileostomy surgeries. Monitor intake and output closely, and ensure patients understand high-output ileostomy management and fluid replacement.
To reduce the risk of intestinal obstruction, advise patients to avoid fresh fruits and vegetables in the immediate postoperative period. These foods should be cooked and chewed well. Individualize food pattern assessments, keeping in mind that what causes gas or increased output for one person, may not for another.
Interprofessional approach and support
An interprofessional approach can enhance positive outcomes. A certified ostomy specialist, surgeon, or primary care provider; dietitian or nutritionist; physical or occupational therapist (depending on the patient’s needs); diabetes educator (as appropriate); and access to an ostomy support group or individual are all important pieces of the puzzle for postoperative success. UOAA provides strong support and education for new and established patients with ostomies. The Ostomy & Continent Diversion Patient Bill of Rights guides patients in advocating for their own care and to improve outcomes. Community support groups and ostomy nurses can help reinforce education, establish routines and independence, and aid in access to supplies.
Complete the circle
Certified ostomy nurses play a significant role in providing education, advancing clinical knowledge, and promoting patient quality of life. Include community resources and follow-up in each care plan to promote positive outcomes and decrease readmissions and ED visits. Taking an interprofessional approach enhances ostomy management and accessing available resources within the community ensures education and support come full circle.
Holly M. Hovan is an advanced practice Certified Wound Ostomy and Continence Nurse at the VA Northeast Ohio Healthcare System in Cleveland, Ohio. She’s a member of the Wound, Ostomy and Continence Nursing Certification Board of Directors.
References
Netsch DS. Anatomy and physiology of the gastrointestinal tract. In: Carmel JE, Colwell JC, Goldberg MT, eds. Wound, Ostomy, and Continence Nurses Society Core Curriculum: Ostomy Management. 2nd edition. Philadelphia, PA: Wolters Kluwer; 2022; 13-28.
Packiam VT, Patel SG, Werntz RP, Steinberg GD. Urinary diversions. In: Carmel JE, Colwell JC, Goldberg MT, eds. Wound, Ostomy, and Continence Nurses Society Core Curriculum: Ostomy Management. 2nd edition. Philadelphia, PA: Wolters Kluwer; 2022; 117-30.
United Ostomy Associations of America. Ostomy & Continent Diversion Patient Bill of Rights. 2007.
Wound, Ostomy, and Continence Nurses Society. WOCN Society, AUA and ASCRS Position Statement on Preoperative Stoma Site Marking for Patients Undergoing Ostomy Surgery. 2007.
Key words: Ostomy, colostomy, ileostomy, ileal conduit, stoma, ostomy pouch, ostomy care