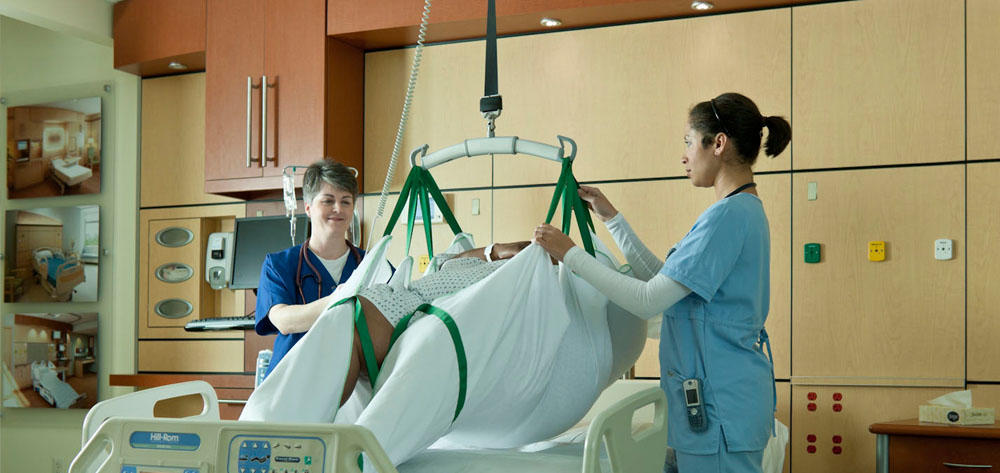
To avoid injuring their patients and themselves, healthcare providers must get in the habit of using safe patient handling and mobility (SPHM) technology. In this supplement, national experts share their perspectives and best practices on topics ranging from dealing with bariatric patients, managing slings, and assessing a patient’s mobility to transforming the culture, building the business case for an SPHM, and developing a successful SPHM program.
Download a PDF of the entire supplement here.
Providing care for bariatric patients is a concern for healthcare facilities and staff everywhere. Delayed patient mobilization due to fear of injury and lack of proper policy, knowledge, or equipment for handling these patients can lead to poor outcomes—and may pose legal and ethical concerns. Specialized equipment, beds, patient lifts, and surgical instruments must be made available to help nurses and other healthcare professionals care for and support best practices for bariatric patients. (See Bariatrics by the numbers.)
Mobility matters
When patients can’t mobilize independently, they rely on nursing and physical therapy staff to prevent immobility complications—pressure ulcers, contractures, deep vein thrombosis, muscle wasting, and pneumonia. Increased patient size is a significant barrier to early mobility, as are lack of proper equipment to lift and move the patient.
Yet providing early mobilization for dependent patients is challenging, and when they’re large, it may seem overwhelming. The bariatric patient may be at even greater risk for immobility and deconditioning during hospitalization because nurses may fear they’ll injure themselves while providing patient care. Manual patient mobilization increases the risk of musculoskeletal injury to caregivers. One study found that although bariatric patients accounted for less than 10% of the patient census in acute-care facilities, patient-handling injuries involving them accounted for 29.8% of staff-reported injuries. Safe patient handling and lifting requires skill and specialized products that support early mobility, lifting, and ambulation.
Bariatric patients may fear falling and may be embarrassed that it takes four or five people to lift, move, or support them during toileting or out-of-bed activities. They may have moderate to severe mobility limitations due to body type, decreased range of motion at the hip and knee, generalized adiposity, and location and size of the pannus (a dense layer of fatty tissue over the lower abdominal area).
Promoting a culture of safety
As a nurse, you can lead the way to creating and maintaining a culture of safety by supporting and modeling safe patient-handling practices on your unit. A focused approach to managing bariatric patients’ mobility needs requires thoughtful planning and knowledge of the technology designed to support care for these patients throughout their entire stay. Lifting and mobility practices can be standardized successfully if nurses have a voice in developing a safe patient-handling and mobility (SPHM) program and in selecting SPHM technology.
Assessing the level of assistance needed
Changing practice begins with evaluating the types of lifting and moving tasks required. Bariatric patients may need assistance with common activities, such as toileting, bathing, skin care, eating, sitting upright, and ambulating. To eliminate variations in care practices, caregivers should be clear on how to assess a patient’s mobility status. Barriers to moving independently—not the patient’s weight—should be the main criteria for determining the need for lift equipment.
Standard categories of dependency levels include:
- dependent—the patient relies on the nurse or caregiver for all lifting and moving activities
- minimally to moderately dependent—the patient relies on the nurse or caregiver for more than 50% of lifting and moving activities
- independent—the patient can perform lifting and moving activities without assistance from the nurse or other caregiver.
Other assessment considerations include:
- weight-bearing capability (full, partial, or none)
- whether the patient has bilateral upper-extremity strength
- patient’s level of cooperation and comprehension
- medications, such as vasopressors and paralytics
- conditions that may affect choice of transfer technique, such as stomas, fractures, severe edema, or joint replacements.
For more information on assessment, read “Implementing a mobility assessment tool for nurses” in this supplement.
Patient-handling algorithms
In 2003, the Veterans Administration created algorithms to provide guidance on how to safely perform high-risk activities related to patient handling and movement. Each algorithm specifies the suggested number of caregivers as well as selection and use of appropriate lift equipment. To download these algorithms, visit www.tampavaref.org/safe-patient-handling.htm.
Organizational guidelines
Manual lifting of any patient isn’t safe. The National Institute of Occupational Safety and Health (part of the Occupational Safety and Health Administration), recommends 35 lb (15 kg) as the safe patient-lifting limit for healthcare workers. The American Nurses Association (ANA) supports a policy of no manual lifting, as discussed in its 2013 book, Safe Patient Handling and Mobility: Interprofessional National Standards.
A 2010 white paper from The Facility Guidelines Institute, titled Patient handling and mobility assessment (FGI-PHAMA), provides recommendations for the right amount of equipment in the right location based on the specific needs of patients on each type of unit. (The ANA publication mentioned above cites this document as supporting evidence on selecting and using lift equipment.) For example, we know many patients in intensive care units (ICUs) are dependent and must rely on nurses to boost, turn, and reposition them frequently throughout the day. FGI-PHAMA recommends 100% ceiling lift coverage in ICUs to ensure patient mobilization activities can be done without delay or injury to nurses. For medical-surgical units, FGI-PHAMA recommends 50% ceiling lift coverage, because generally half the patients on these units depend on the nurse to lift, manage, move, and support their ambulation activities throughout some portion of their stay.
Challenging environments
Advances currently are under way to promote safe patient handling in other challenging hospital areas, such as the operating room (OR), emergency department, outpatient areas, and ancillary units. Preplanning for patient flow and transfer activity to and from these units is essential. The care team must communicate, coordinate, and cooperate during patient transport, lateral transfers, and repositioning. With technology available to prevent injury to both caregivers and patients, no department should put staff at risk for injury during transfer activities. (For a case study on bariatric equipment use in the OR, see Case study: Bariatric surgery using the proper SPHM technology.)
Bariatric patients present multiple concerns for healthcare workers. We encourage all nurses to speak up about safety and to support a SPHM workplace environment.
Selected references
American Nurses Association. Safe Patient Handling and Mobility: Interprofessional National Standards. Silver Spring, MD: Author; 2013.
American Society for Metabolic and Bariatric Surgery. Estimate of bariatric surgery numbers. 2014. http://asmbs.org/2014/03/estimate-of-bariatric-surgery-numbers. Accessed June 24, 2014.
American Society of Bariatric Surgeons. Medical options for treating obesity fact sheet. Updated May 2014. Accessed June 24, 2014.
The Facility Guidelines Institute. 2010 Health Guidelines Revision Committee Specialty Subcommittee on Patient Movement. Patient handling and movement assessments: A white paper. April 2010. https://www.dli.mn.gov/wsc/PDF/FGI_PHAMAwhitepaper_042710.pdf. Accessed June 24, 2014.
Gallagher S. Implementation Guide to the Safe Patient Handling and Mobility Interprofessional National Standards. Silver Spring, MD: American Nurses Association; 2013.
Gallagher S. The Challenges of Caring for the Obese Patient. Edgemont, PA: Matrix Medical Communications; 2005.
Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of childhood and adult obesity in the United States, 2011-2012. JAMA. 2014; 311(8):806-14.
Randall SB, Pories WJ, Pearson A, Drake DJ. Expanded Occupational Safety and Health Administration 300 log as metric for bariatric patient-handling staff injuries. Surg Obes Relat Dis. 2009;5(4);463-8.
Schallom L, Metheny NA, Stewart J, et al. Effect of frequency of manual turning on pneumonia. Am J Crit Care. 2005;14(6):476-8.
U.S. Department of Veterans Affairs. Safe patient handling and movement. Reviewed/Updated April 30, 2014. www.visn8.va.gov/visn8/patientsafetycenter/safePtHandling/default.asp. Accessed June 24, 2014.
Dee Kumpar is the director for Safe Patient Handling Programs at Hill-Rom in Batesville, Indiana and a member of the workgroup for ANA’s Safe Patient Handling and Mobility: Interprofessional National Standards. She is on the board of directors of the Association of Safe Patient Handling Professionals.