Consider this scenario: Over the past 12 months, Pat, an RN, has participated in two Awareness conversations with a peer member of the Professionalism Committee, but reports about unsafe and disrespectful behavior continue, including: 1) She refused to assist a team member turn a patient safely. 2) She didn’t deal with a patient’s pain during the previous shift. 3) She wouldn’t talk with me about my patient’s status and the doctor’s orders.
The first three articles in this series introduced the Promoting Professionalism Pyramid for fostering professionalism, explored Cup of Coffee conversations for informally discussing behaviors that seem to undermine a culture of safety and respect, and described Awareness conversations for sharing what appears to be a pattern of concerns.
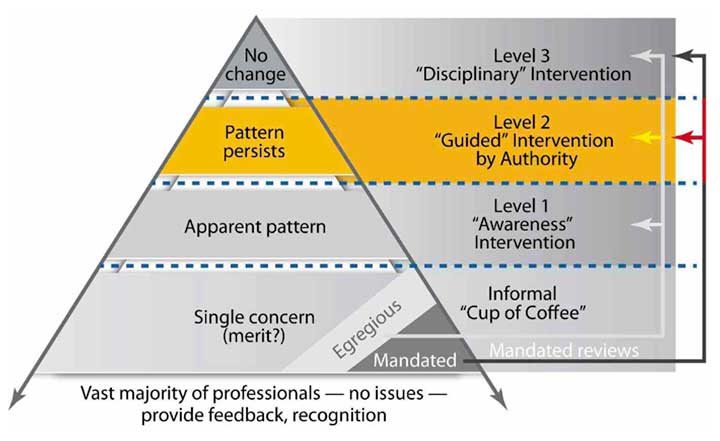

This final article focuses on the Guided intervention by an authority figure (those with authority over the employee’s continued relationship with the organization, such as a manager, supervisor, or other leader in the organization’s chain of command). We present a framework for a current or future leader to address a pattern that persists despite the professional’s opportunities to reflect and self-regulate after Cup of Coffee and Awareness conversations.
What is a Guided intervention?
About 2% to 5% of an organization’s professionals demonstrate a pattern of unprofessional conduct, and 75% to 80% of them respond to Awareness interventions. Generally, an individual is provided two chances to respond to Awareness conversations, based on policy and the rate at which meaningful data can accrue, unless perceived risk is imminent. Giving professionals the opportunity to reflect and self-regulate has integrity and is fair. At some point, however, organizations must support efforts to escalate interventions for the few individuals whose unprofessional behavior persists. This is when the authority figure moves from “pause and reflect” to an “accountability action plan” designed to facilitate improvement.
Who, what, where, when, why, and how


Who. The messenger is the receiver’s (clinician’s) manager, director, or designated authority figure in the reporting structure, not a peer as in previous intervention levels.
What. As the messenger, your goals for the Guided intervention are to alert the professional that a previously presented pattern has persisted (or single significant event has occurred) and to create a corrective action plan.
Where. Hold the meeting in your office to signal its importance.
When. Guided interventions should be scheduled as soon as there’s evidence that a pattern of unprofessional behavior has persisted, or soon after the report of an egregious or mandated event.
Why. Repeated demonstrations of disrespectful and unsafe behaviors may lead to preventable adverse outcomes, team member disengagement or burnout, staff turnover, and associated costs. Leaders demonstrate their commitment to both patients and coworkers when they address any subordinate’s persistent unsafe, unprofessional behaviors.
How. To prepare for the Guided intervention, review the pattern of behavior revealed in the data and reports and anticipate what resources might help the professional address performance issues. Next, review relevant governing documents, including human resources and professional conduct policies. These documents will guide you through the process and its performance- related outcome: either the professional improves or is escalated to the Pyramid’s Disciplinary tier.
Before the meeting, send a letter to the professional stating the need to meet, making clear that this is different from previous meetings. For example, the letter might say: You’ve previously been made aware of concerns about unsafe and disrespectful behavior…. As your manager, I am scheduling a meeting with you because those behaviors have continued…. We need to develop an accountability plan aimed at addressing the pattern.
Keep in mind the following strategies for success during your conversation:
• Focus on expectations and the behavior inconsistent with those expectations, not what prompted the behavior or performance.
• Concentrate on the stories and data you have in hand. Identifying themes or patterns of behavior may help formulate action plans.
• Know your message and stick to it (avoid tangents).
• Remind your colleague about previous discussions on this topic (have documentation to handle denials).
• Remember your hope to restore the clinician to a fully functioning professional performance, but also your commitment to safety and to your organization and its patients.
• Document the conversation.
For talking points and associated documentation, we suggest using the acronym EDICTS as a guide.
Follow-up and consequences
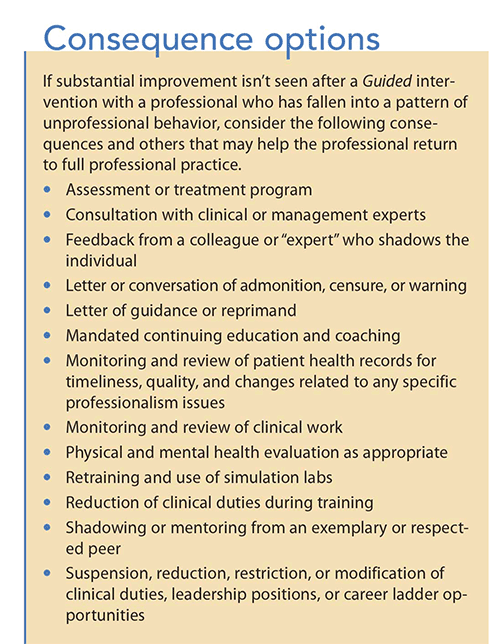

In rare cases, the professional will fail to complete the agreed-upon plan, or the pattern will continue. In some instances, an investigation will find the assertion of a serious allegation (mandated or egregious act) to be true. In these circumstances, organizational leaders must be prepared to advance to corrective or disciplinary action, which may lead to restrictions on the clinician’s duties or a required departure from the organization.
Professionalism: A two-way street
Promoting professionalism and professional accountability depends on every healthcare professional’s willingness and ability to share concerns and, if needed, accept feedback about perceptions of their own conduct. We hope this series helps you consider how best to do both and act accordingly.
All authors work at Vanderbilt University Medical Center in Nashville, Tennessee. Marilyn Dubree is the executive chief nursing officer in clinical enterprise administration; April Kapu is associate chief nursing officer of advanced practice; Michelle Terrell is the director of advanced practice at Monroe Carell Jr. Children’s Hospital; James W. Pichert is professor of medical education and administration at the Vanderbilt Center for Patient and Professional Advocacy; William O. Cooper is professor and vice chair in the department of pediatrics, professor in the departmentof health policy, and director of the Vanderbilt Center for Patient and Professional Advocacy; Gerald B. Hickson is senior vice president for quality, safety and risk prevention, clinical enterprise administration, center for quality, safety and risk prevention.
This is the final installment in a series of articles on promoting professionalism. You can read the first three articles here:
Promoting professionalism by sharing a cup of coffee
Nurses’ essential role in supporting professionalism
Promoting professionalism through awareness
Selected references
Dubree M, Kapu A, Terrell M, Pichert JW, Cooper WO, Hickson GB. Nurses’ essential role in supporting professionalism. Am Nurse Today. 2017;12(4):6-8.
Dubree M, Kapu A, Terrell M, Pichert JW, Cooper WO, Hickson GB. Promoting professionalism by sharing a cup of coffee. Am Nurse Today. 2017;12(5):18-19.
Dubree M, Kapu A, Terrell M, Pichert JW, Cooper WO, Hickson GB. Promoting professionalism through awareness. Am Nurse Today. 2017;12(6):6-8.
Hickson GB, Moore IN, Pichert JW, Benegas Jr M. Balancing systems and individual accountability in a safety culture. In: Berman S, ed. From Front Office to Front Line: Essential Issues for Health Care Leaders. 2nd ed. Oakbrook Terrace, IL: Joint Commission Resources; 2012; 1-36.
Reiter CE, Pichert JW, Hickson GB. Addressing behavior and performance issues that threaten quality and patient safety: What your attorneys want you to know. Prog Pediatr Cardio. 2012;33(1): 37-45.
Shapiro J, Whittemore A, Tsen LC. Instituting a culture of professionalism: The establishment of a center for professionalism and peer support. Jt Comm J Qual Patient Saf. 2014;40(4):168-77.



















