Early identification results in a positive outcome.
Takeaways:
- Abdominal pain, bloating and distension, vomiting, and obstipation are warning signs of small bowel obstruction.
- Small bowel obstructions are treatable if recognized early.
- Some bowel obstructions are life-threatening and require surgical intervention.
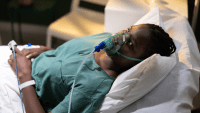
Anna Smith* is a 56-year-old woman who arrives in a wheelchair to the emergency department (ED). She’s doubled over with her arms across her abdomen. Her husband reports that she’s had severe, sudden-onset, mid-abdominal pain for the past 6 hours. Ms. Smith doesn’t drink alcohol or smoke, and her only chronic condition is hypothyroidism.
History and assessment hints
Ms. Smith is unable to respond to the triage nurse’s questions because of her pain. She’s diaphoretic, tachypneic, and afebrile. Her pain severity is 8/10, and her blood pressure is stable at 145/90 mmHg. Ms. Smith’s husband reports that she’s unable to keep anything down and has been vomiting dark green bile. The nurse learns that Ms. Smith had abdominal surgery for a hernia a few months ago and had been recovering well. On physical examination, Ms. Smith’s abdomen is distended and tender to palpation with hypoactive bowel sounds. She says she’s been constipated for the past few days and is unable to pass gas. The nurse notes that her mucous membranes are dry.
Taking action
The nurse recognizes that Ms. Smith has the classic symptoms of a bowel obstruction, including a positive history for recent abdominal surgery, and takes her to a room for a provider examination. The provider assesses Ms. Smith’s distended abdomen and performs a digital rectal exam to check for fecal impaction. Lab results are unremarkable for severe or systemic infection. After chest and abdominal radiographs rule out a complete obstruction, a computed tomography (CT) scan with oral contrast (Gastrografin) is ordered.
The scan reveals a small bowel obstruction without necrosis or perforation. Ms. Smith is given pain and nausea medication, as well as I.V. fluids for hydration, and a nasogastric (NG) tube is inserted. The ED nurse educates Ms. Smith and her husband about the purpose of the NG tube, which will help remove excess stomach fluid. She understands that she shouldn’t eat or drink with the tube in place.
Outcome
After 3 days in the hospital, Ms. Smith reports significant improvement in her pain. Her abdomen is no longer distended and she says that she can pass gas, a good sign for small bowel obstruction recovery. Ms. Smith continues I.V. fluids. After she has a bowel movement, the NG tube is removed. Her laboratory tests indicate that she’s adequately hydrated and she reports that her pain is 1/10, with only mild cramping.
Education and follow up
When Ms. Smith is feeling better and no longer receiving opioid pain medication, she asks the provider and nurse about her condition. The provider explains that the hernia surgery created adhesions around the bowel that caused the obstruction, which could recur. The nurse explains that the bowel could have been unhealthy or even dead, requiring immediate surgical intervention. The nurse also talks to Ms. Smith about the importance of staying hydrated with sips of clear liquids and eating a modified diet of small, bland meals to avoid recurrence of the obstruction.
*Name is fictitious.
Access references at myamericannurse.com/?p=73275.
Jessica Dzubak is director of nursing practice at the Ohio Nurses Association in Hilliard.
References
Baiu I, Hawn MT. Small bowel obstruction. JAMA. 2018;319(20):2146. doi:10.1001/jama.2018.5834
Catena F, Di Saverio S, Coccolini F, et al. Adhesive small bowel adhesions obstruction: Evolutions in diagnosis, management and prevention. World J Gastrointest Surg. 2016;8(3):222-31. doi:10.4240/wjgs.v8.i3.222
Hill AG, Sammour T. Gastrografin for adhesive small bowel obstruction. UpToDate. November 19, 2019. uptodate.com/contents/gastrografin-for-adhesive-small-bowel-obstruction
Long S, Emigh B, Wolf JS, Byrne C, Coopwood TB, Aydelotte J. This too shall pass: Standardized Gastrografin protocol for partial small bowel obstruction. Am J Surg. 2019;217(6):1016-8. doi:10.1016/j.amjsurg.2018.12.063
Medline Plus. Intestinal or bowel obstruction—discharge. September 2018. medlineplus.gov/ency/patientinstructions/000150.htm
National Institute of Diabetes and Digestive and Kidney Diseases. Abdominal adhesions. June 2019. niddk.nih.gov/health-information/digestive-diseases/abdominal-adhesions