To: Ethics Advisory Board
From: Student nurse
Subject: Social determinants of health
I’m a nursing student, and my instructor has been talking about social determinants of health and how nurses have an ethical obligation to improve the health of communities and populations. Can you help me understand why?
From: ANA Center for Ethics and Human Rights
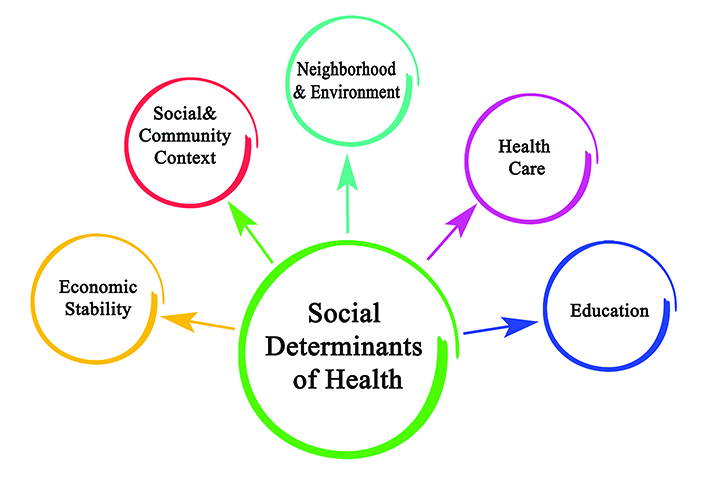
Social determinants of health encompass the conditions in which people live, learn, work, play, worship, and age. These conditions are pivotal in determining a person’s quality of life and health status. Research has found that where you live—your Zip Code—may be more important than your genetic code. The community where you live has a profound impact on whether you and the people in your neighborhood are healthy.
We know that health and long life require access to affordable, quality healthcare, but they also require access to healthy food, quality schools, affordable housing, and jobs that provide the resources necessary to prevent illness and live a meaningful life. If these basic necessities are lacking in a community, its health will suffer.
Many of the social determinants of health—poverty, homelessness, race, ethnicity, and lifestyle choices, such as smoking—can influence outcomes for patients with COVID-19. We know that low-income communities have higher mortality rates when compared with more affluent communities, smokers are more likely to have severe symptoms, and children who depend on free lunch programs suffer from hunger during school closures. These are just some examples.
Provision 8 in the Code of Ethics for Nurses with Interpretive Statements (nursingworld.org/coe-view-only) states that “health is a universal human right. This right includes access to healthcare, education, food security, immunizations, and basic sanitation. Nurses understand that the lived experiences of inequality, poverty, and social marginalization contribute to the deterioration of health.” Provision 8 also instructs nurses to address social determinants of health such as poverty, hunger, access to nutritionally sound food, and education. It’s critical for nurses to identify issues that impact the health of communities and their populations. Health equity is essential: People should be able to be healthy and thrive in every community—not just some. Confronting the social determinants of health may prevent or minimize the impact of illnesses or health conditions on populations.
Provision 8 guides nurses to measure the burden that a community carries due to social determinants of health and to improve the conditions of daily life in the community. Nurses can educate the public about health inequalities by participating in community organizations and groups. They can teach individuals and communities about healthy lifestyles and preventive care, including the importance of vaccination. Specifically, nurses can seek to alleviate COVID-19 vaccine hesitancy by providing access to credible information about authorized vaccines and how to get them. But most important, all nurses should engage in collaborative efforts with community stakeholders to influence public policy that promotes and protects the health of individuals, communities, and populations.
— Response by Elizabeth Swanson, DNP, MPH, APRN-BC,
member of the ANA Center for Ethics and
Human Rights Advisory Board.
References
Abrams EM, Szefler SJ. COVID-19 and the impact of social determinants of health. Lancet Respir Med. 2020;8(7):659-61. doi:10.1016/S2213-2600(20)30234-4
Registered Nurses Association of Ontario. Social determinants of health. rnao.ca/policy/projects/social-determinants-health
Robert Wood Johnson Foundation. Achieving health equity. rwjf.org/en/library/features/achieving-health-equity.html
Do you have a question for the Ethics Inbox? Submit at ethics@ana.org.