Patient and family perspective
- Individuals with strabismus have an increased risk of concurrent mental health diagnoses.
- Children and their families frequently are unaware of any possible connection between strabismus and mental health, but they welcome resources.
- Nurses have a pivotal role to play in helping patients and families navigate the stresses of strabismus care and mental health challenges.
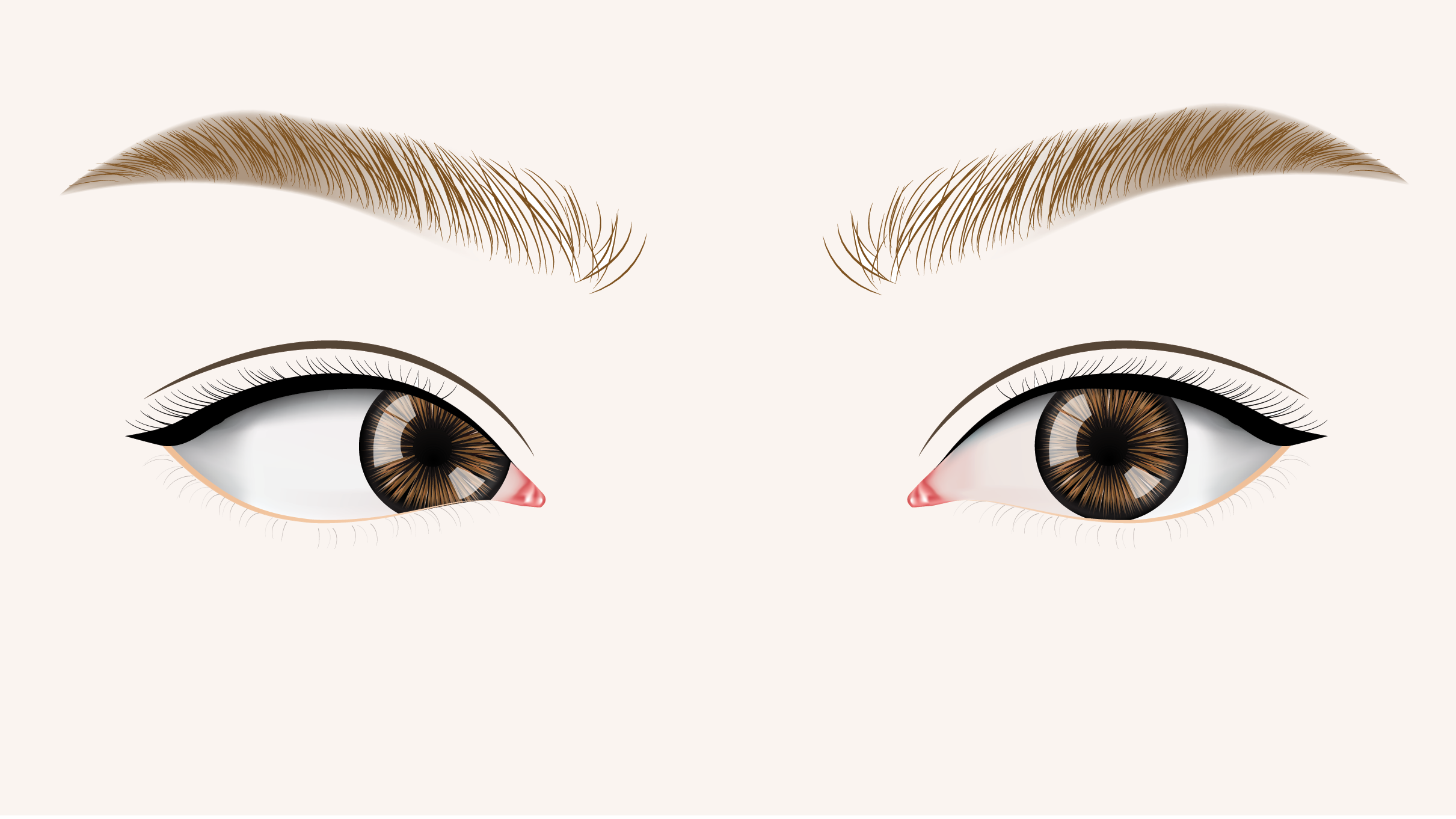
In a recent JAMA Ophthalmology article, Lee and colleagues’ retrospective chart review found that children with strabismus (a disorder in which the eyes do not line up in the same directions) have about a doubled risk of a concurrent diagnosis of anxiety disorder, bipolar disorder, or schizophrenia. A growing body of literature about this connection exists, but researchers have found few answers about the causative factors.
Strabismus affects 2% to 4% of the population. The eye can turn down (hypotropia), up (hypertropia), inward (esotropia), or away from the nose (exotropia). Esotropia is most common. Strabismus is considered normal when it occurs off-and-on in infants under 6 months. In pseudostrabismus, a wide nose-bridge gives the appearance of eye-turn.
Researchers have found connections between strabismus and developmental syndromes, autism spectrum disorder, and inattention symptoms. In addition, some genetic syndromes have an association with strabismus. A neurologic event or poisoning can cause sudden-onset strabismus; tumors, such as a retinoblastoma, rarely cause the condition.
I interviewed several patients and family members about strabismus and associated treatment anxiety, bullying and teasing, mental health effects, and resiliency. I received consent from all participants to be quoted.
Treatment anxiety
The most common and effective treatments for strabismus include surgery and covering or blurring vision in the unaffected eye with medicated eyedrops. These methods strengthen the muscles of the affected eye. Some professionals recommend eye exercises, but limited insurance coverage and evidence exist.
Many children find strabismus treatment upsetting. Eric remembers “hating” eye drops and has “horrible memories of having to be held down for them.” However, he now believes the strategy was “totally worth it.” Karen experienced discomfort and “terror” when removing adhesive patches from her unaffected eye. She would uncharacteristically “cry and cry,” and nothing seemed to help. She was grateful when, years later, her own daughter’s treatment for strabismus involved “much less sticky” patching that “wasn’t a huge deal for her.”
Eric’s outpatient laser eye surgery felt “scary” at the time, and Carol vividly recalls leaving her daughter alone in the hospital overnight at 13 months, “crying in a crib.” A health professional told Kim “you’ll cry blood” after surgery. Afraid to look at herself at first, Kim felt relief when she saw only “pink eyes.”
Bullying, teasing, exclusion
Some parents and patients reported no social difficulties during childhood. Kathryn, mother to a preschooler with strabismus related to the 17q12 deletion genetic syndrome, said her daughter received support from her classmates. Before her daughter’s surgery “people in grocery stores, strangers” invasively asked Carol about the plan for her daughter’s eye treatment. Carol’s concerns about teasing from her daughter’s peers, however, never materialized.
Eric faced verbal teasing, with some classmates calling him “four eyes.” Karen felt that her symptoms, including appearance of her gaze and difficulty reading and judging distances, affected her social development. Her reduced depth perception would lead her to “stand too close to other people” without realizing it.
Mental health effects
Growing up in New Hampshire, Eric had “never heard or been told about any sort of link between strabismus and mental health disorders by any doctors.” He started treatment for his eye condition at age 5 and developed obsessive compulsive disorder and generalized anxiety disorder about a year later. Karen experiences depression and anxiety, for which she takes medication and participates in talk therapy. Kathryn’s daughter, whose rare genetic condition is associated with mental health challenges, also experiences anxiety.
Kim felt acutely self-conscious, despite her parents’ efforts to normalize the cloth patch over her glasses lens. She had a fear of elevators, and after strabismus surgery at 8, her anxiety intensified. She developed stress around schoolwork and social situations and suffered panic attacks. Now a preschool teacher herself, Kim said, “When I think of who I am and what defined my childhood, my patch is definitely one of those things. I remember being so relieved when I could take it off and everyone could see my face.”
Resiliency
Many of the patients developed coping mechanisms and workarounds to help them participate in school and social activities. Carol’s daughter made the state tennis championships despite lacking coordinated vision and perfect depth perception. Karen credits her parallel parking skills to finding a strategy that works without depth perception. She also compensated for reading challenges, common with strabismus, by figuring out “how to read certain words based on their length.” She only recognized her innovation when watching her daughter learn to read without it. Eric feels “blessed” that his parents could afford surgery to correct his eye-turn.
Nursing implications
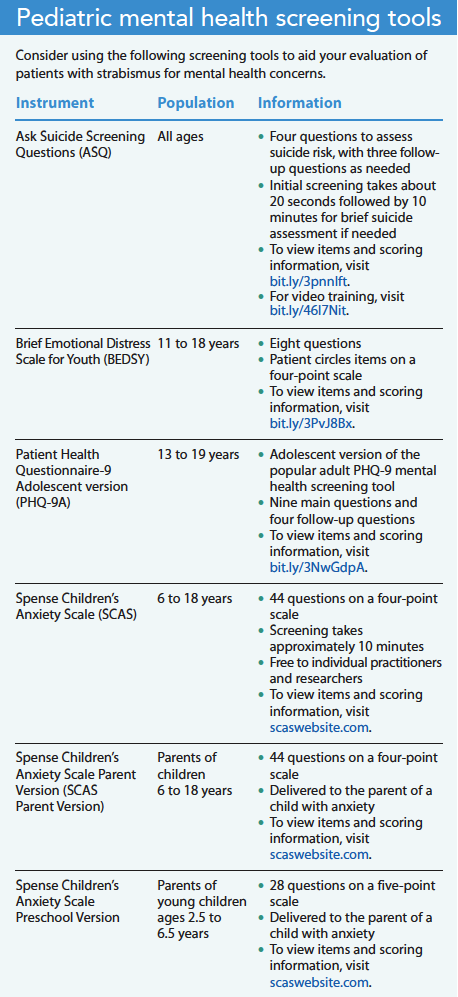
Nurses can help their patients with strabismus address mental health concerns with appropriate screening, referrals, and education. Begin by asking if they have any issues with coping in general, and specifically anxiety related to eye treatments. Knowing a few brief screening instruments for childhood mental health can help you identify problems early. Some free options include the Spense Children’s Anxiety Scale and preschool version, and the Patient Health Questionnaire-9 Adolescent version. The Ask Suicide Screening Questions is a common four-item option approved for all ages. (See Pediatric mental health screening tools.)
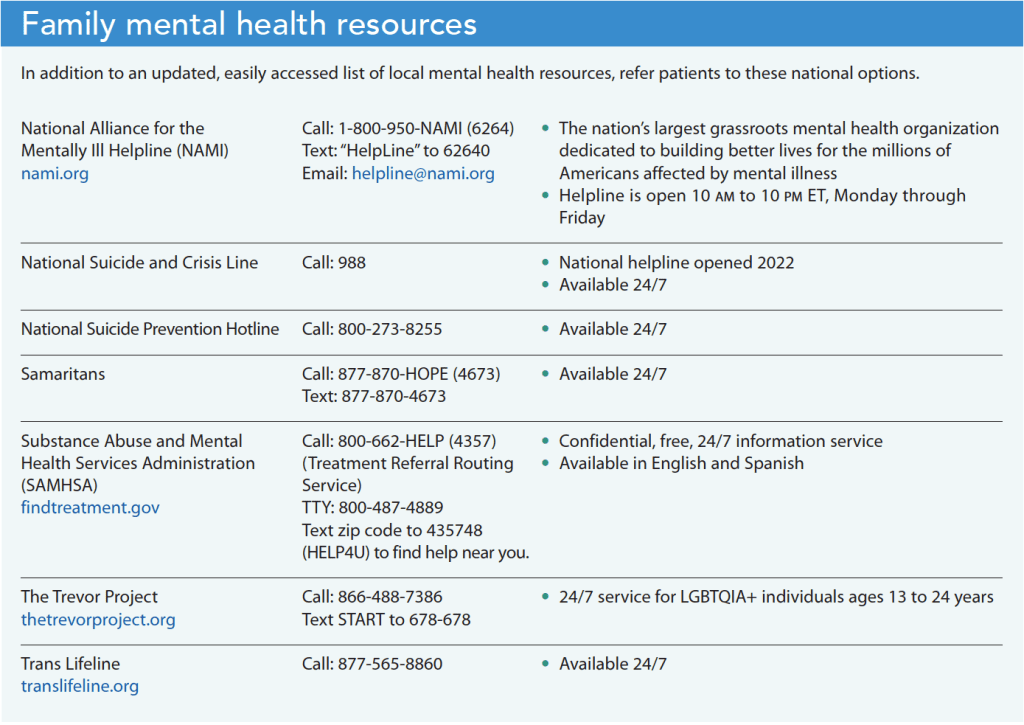
Refer families with mental health concerns to behavioral health for further evaluation. To save time, work with your organization to create and update an easily accessible list of local recommendations. (See Family mental health resources.)
Parents and children benefit from advice on the various strabismus treatment options. Rewards and distractions can make them more tolerable. Carol and Karen noted that watching TV or reading helped the time spent patching pass more quickly.
Surgical procedures create anxiety for children and families. Use a variety of multi-media educational methods, such as video, audio, and written materials scaled to the patient’s reading level, to anticipate and answer questions and reduce anxiety and misunderstandings.
Education and support
None of the patients or parents who shared their experiences knew about a link between strabismus and mental health conditions, but they were eager to know and understand more. All of them welcome screening, evaluation, and referrals to mental health, and they hope that sharing their stories will help others. Nurses can serve as a source of education and support and guide patients and families to the care they need.
Kathryn Kieran is an instructor at the MGH Institute of Health Professions School of Nursing in Boston, Massachusetts.
American Nurse Journal. 2023; 18(8). Doi: 10.51256/ANJ082324
References
American Optometric Association. Strabismus (crossed eyes). aoa.org/healthy-eyes/eye-and-vision-conditions/strabismus?sso=y
Jin Y, Jiang A, Jiang W, et al. Self-produced audio-visual animation introduction alleviates preoperative anxiety in pediatric strabismus surgery: A randomized controlled study. BMC Ophthal. 2021;21(1):163. doi:10.1186/s12886-021-01922-6
Lee YH, Repka MX, Borlik MF, et al. Association of strabismus with mood disorders, schizophrenia, and anxiety disorders among children. JAMA Ophthalmol. 2022; 140(4)373-81. doi:10.1001/jamaophthalmol.2022.0137
Mao D, Lin J, Chen L, Luo J, Yan J. Health-related quality of life and anxiety associated with childhood intermittent exotropia before and after surgical correction. BMC Ophthalmol. 2021;21(1):270. doi:10.1186/s12886-021-02027-w
Montecalvo B. To cut or not to cut? Weighing strabismus surgery referral. Review of Optometry. 2022;159(4):74-8. reviewofoptometry.com/article/to-cut-or-not-to-cut-weighing-strabismus-surgery-referral
MedlinePlus. 17q12 deletion syndrome. medlineplus.gov/genetics/condition/17q12-deletion-syndrome
MedlinePlus. Strabismus. medlineplus.gov/ency/article/001004.htm
National Institute of Mental Health. Ask Suicide-Screening Questions (ASQ) toolkit. nimh.nih.gov/research/research-conducted-at-nimh/asq-toolkit-materials
Patra KP, Kumar R. Screening for depression and suicide in children. StatPearls. December 12, 2022. ncbi.nlm.nih.gov/books/NBK576416
Prakalapakorn SG, Singh MK, Congdon N. Association between strabismus and children’s mental health. JAMA Ophthalmol. 2022;140(4):381-2. doi:10.1001/jamaophthalmol.2022.0149
Key words: strabismus, eye care, pediatric mental health




















2 Comments. Leave new
Great article. It would be wonderful to include information to address strategies for helping children to manage the discomfort of eye drops: Buzzy bee? Sweet treat? Music? Thanks
Hi Jennifer, I think distraction is a great technique and would agree with everything you suggested. I think the interventions would have to be individualized to the child, so creativity and responsiveness are important. Since eyesight will be blurred, TV and books are out; tactile, aroma-based, sweet treats, or other ways to soothe would be important. Distracting with alternate sensations like holding a cold pack in one hand and warm pack in another while administering might also help? Thanks for your comment and hope someone with more lived experience can also chime in.