Astute assessment prevents a poor outcome
- Three scores are used to assess a subarachnoid hemorrhage—Hunt and Hess, Fisher, and modified Fisher.
- Nursing care includes consistent assessment to monitor level of consciousness, urine output, and vital signs.
- Nimodipine, a calcium channel blocker, helps prevent vasospasm but can result in low blood pressure that harms the cerebral vasculature.
Karen Thompson*, a 55-year-old woman, arrives in the ED via ambulance. She reports the worst headache of her life and sensitivity to light. She has no significant medical history.
The stroke activation team completes the National Institute of Health stroke scale and orders a computed tomography (CT) scan. Ms. Thompson’s vital signs are BP 132/74 mmHg, HR 87 bpm, RR 20 breaths per minute, O2 saturation 97% on room air. She rates her headache pain as 10/10. Based on the assessments, Ms. Thompson receives an initial Hunt and Hess score of 2 (which indicates subarachnoid hemorrhage [SAH] severity based on a patient’s clinical condition), a Fisher score of 3 (which indicates 37% risk of vasospasm), and a modified Fisher score of 2 with intraventricular hemorrhage (which predicts the clinical risk of vasospasm and delayed cerebral ischemia).
Secondary postpartum hemorrhage: Risk factors, assessment, and intervention
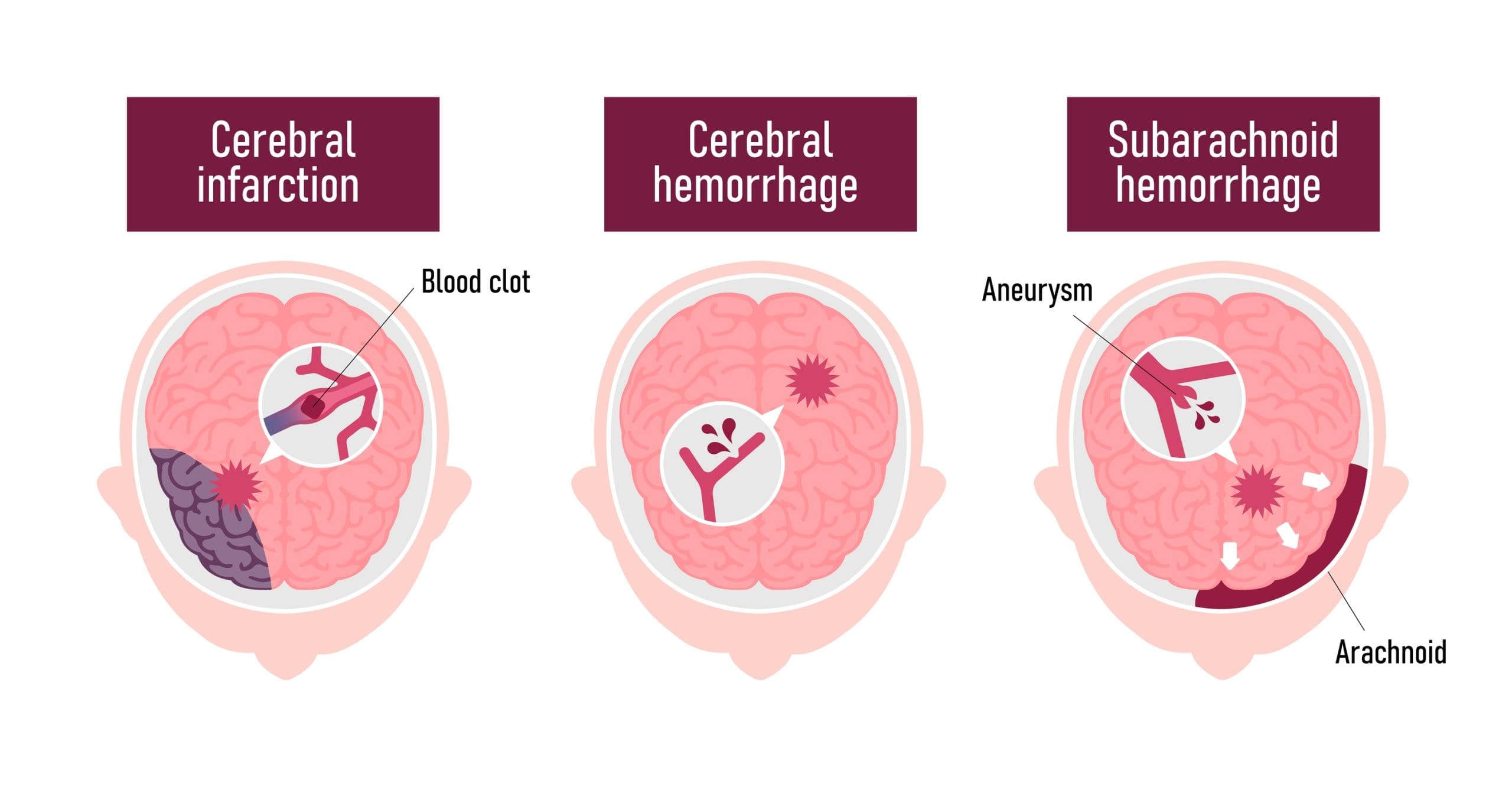
Complications after brain hemorrhage repair
The neuro ICU nurse, Martin, performs hourly neuro exams and administers nimodipine 30 mg by mouth every 2 hours to prevent vasospasm and levetiracetam for seizure prophylaxis. He also maintains strict blood pressure control of less than 160 mmHG.
On the scene
At an hourly exam, Martin notes increased urine in Ms. Thompson’s catheter bag and that she seems lethargic. Concerned about cerebral salt wasting, Martin contacts the provider on-call, states the change in the patient’s condition, and recommends stat labs and a head CT scan for further evaluation. The provider agrees and places orders for the scan, a basic metabolic panel to include serum sodium and serum osmolality, and urinalysis with electrolytes.
Education
Three types of scores are used to assess an SAH. The Hunt and Hess score, which ranges from 1 (asymptomatic or mild headache) to 5 (coma), measures SAH severity and potential prognosis. The Fisher scale predicts cerebral arterial vasospasm risk, and the modified Fisher scale includes intraventricular hemorrhage to determine the risk of cerebral artery vasospasm and delayed cerebral ischemia.
Nursing care includes consistent assessment to monitor level of consciousness, urine output, and vital signs. Spiking and dropping blood pressure may indicate cerebral edema, vasospasm, or rebleeding. Nimodipine helps prevent vasospasm, but this calcium channel blocker can result in low blood pressure and harm the cerebral vasculature. Systolic blood pressure parameters are key in preventing an extenuation of a cerebral bleed. To prevent temperature fluctuations, which can lead to delayed cerebral ischemia and are associated with increased morbidity and mortality, nurses should ensure the patient remains normothermic.
Results
The most significant results of the tests ordered by the provider reveal hyponatremia with a serum sodium of 127 mEq/L, urine sodium of 45 mEq/L, and urine osmolality of 110 mOsm/kg. Based on these results, the provider orders a bolus of normal saline, serum sodium every 6 hours, and fludrocortisone.
Outcomes
Ms. Thompson undergoes successful coiling to block blood flow into the aneurysm. She completes her nimodipine regimen and the cerebral salt wasting resolves. After 18 days, Ms. Thompson is discharged home. She receives education related to the coiling procedure, follow-up needs, and relevant lifestyle modifications and medication changes.
*Name is fictitious.
The authors work at the University of Florida Health – Jacksonville. Tara Mays and Adam Musto are rapid response clinical nurses. Alysia Adams is the division director of nursing education, professional practice, research, Magnet, and wound care.
American Nurse Journal. 2023; 18(8). Doi: 10.51256/ANJ082332
References
Claassen J, Bernardini GL, Kreiter K, et al. Effect of cisternal and ventricular blood on risk of delayed cerebral ischemia after subarachnoid hemorrhage: the Fisher scale revisited. Stroke. 2001;32(9):2012-20. doi:10.1161/hs0901.095677
Fisher CM, Kistler JP, Davis JM. Relation of cerebral vasospasm to subarachnoid hemorrhage visualized by computerized tomographic scanning. Neurosurg. 1980;6(1):1-9. doi:10.1227/00006123-198001000-00001
Hunt WE, Hess RM. Surgical risk as related to time of intervention in the repair of intracranial aneurysms. J Neurosurg. 1968;28(1):14-20. doi:10.3171/jns.1968.28.1.0014
Hoh BL, Ko NU, Amin-Hanjani S, et al. 2023 Guideline for the management of patients with aneurysmal subarachnoid hemorrhage: A guideline from the American Heart Association/American Stroke Association. Stroke. 2023;54(7):e314-70. doi: 10.1161/STR.0000000000000436
Hong L, Cadogan M. Hunt-Hess scale. Life in the FastLane. November 24, 2020. litfl.com/hunt-hess-scale
Nickson C. Subarachnoid haemorrhage grading system. Life in the FastLane. November 3, 2020. litfl.com/subarachnoid-haemorrhage-grading-systems
Key words: subarachnoid hemorrhage, stroke, cerebral salt wasting, stroke activation team



















1 Comment. Leave new
Good job ..you keep us updated.