Use this model to promote nurse retention.
Takeaways:
- The recent pandemic, and potential consequential post-traumatic stress disorder, might affect nurse retention significantly.
- Strategically planned job embeddedness principles will help retain nurses and create a healthy work environment.
During the COVID-19 pandemic, the nursing role has expanded to include emotional supporter, caregiver, and the last person a patient bonds with before they die. The extreme patient load many nurses are experiencing leaves them with no time to grieve or debrief. Instead, they “hold it together” and move on to the next patient. Many researchers (including Cai and colleagues, Li and colleagues, and Raudenská and colleagues) report staggering numbers of post-traumatic stress disorder among healthcare workers. How will the pandemic affect nurse retention in the long term?
As a nurse manager, you’re looking for ideas to enhance nurse retention, provide a healthy work environment, and maintain quality patient care. The job embeddedness model focuses on the reasons why nurses stay with an organization and guides administrators in reviewing every positive aspect of the workplace and strategizing to make what is good even better.
What is job embeddedness?
In 2001, two business management researchers, Mitchell and Lee, developed the job embeddedness model. Since then, many healthcare organizations have adopted it to successfully retain nurses by focusing on the positive organizational and community ties that keep nurses embedded. The tighter the web, the more embedded the nurse will be.
Organizational ties
The organizational dimension of the embeddedness model consists of three concepts: Fit-organization, links-organization, and perceived sacrifices-organization if a nurse decides to leave.
- Fit-organization refers to the compatibility between a nurse’s ethical morals and values, career goals, personality, and personal goals with those of the organization. When personal goals and ambitions align with those of the organization, fit-organization will improve retention.
- Links-organization describes a nurse’s connections and relationships with others, involvement in decision-making, committee service, and work team participation. The commitment and engagement of these activities will strengthen the links-organization concept.
- Sacrifices-organization indicates the perceived sacrifices a nurse makes when leaving an organization. These sacrifices can be obvious losses (such as salary, pension funds, sick leave, and paid time off), but they also include subtle psychological sacrifices (such as loss of seniority, office space, parking privileges, opportunities for advancement, job stability, and loss of further experience and knowledge that would help the nurse cope and succeed).
Community ties
The community dimension involves the same three concepts but applies them to the community in which the nurse lives.
- Fit-community includes compatibility between ethical morals and values with those of the community. A compatible culture and climate, as well as amenities, can strengthen the fit-community concept.
- Links-community involves such aspects as church activities, service on community committees, and children’s school involvement. Married nurses with school-age children, for example, will most likely sacrifice more than a nurse with no community links.
- Perceived sacrifices-community can include the prospects of selling a house, moving children out of the school they love, moving away from friends or family, or leaving a spiritual family behind.
Many healthcare organizations concentrate on these concepts to attract nurses, but they frequently overlook the fact that all ties must be in place and weaved into a strong enough web to keep nurses embedded. Impressive benefit packages—such as sign-on bonuses, retirement benefits, salaries, excellent healthcare insurance, and opportunities to enhance professional development—may not be enough to keep a nurse embedded, and they’ll leave the organization as soon as their contracts expire. Using the job embeddedness model as a guideline, administrators can explore other options to strengthen the fit and links concepts.
How to improve job embeddedness in nursing
The nursing environment is versatile, with different education levels, qualifications, and generations. Gibbs and Duke found that adapting to the differences among employees (rather than creating a one-size-fits-all benefit package) can help improve retention. For example, RNs place a high value on the links-community concept, so emphasizing community service, employee involvement in local schools and community-based organizations, and sponsoring sports teams are just a few ways to increase RNs’ job embeddedness.
In this same study, significant differences in the links-organization concept were demonstrated between generations. Suggested changes include facilitating peer recognition and providing opportunities for seasoned nurses to mentor novice nurses. Knowledge sharing among employees will improve customer service and patient care and also recognize individual contributions. Allow individual preferences by letting employees choose teams and projects to join.
In addition, provide career advancement opportunities for nurses who are improving their professional qualifications or educational level. Some nurses, as their educational levels increase, will begin to feel overqualified for their current role and may seek another position. However, if they’re embedded in the organization, they will look for internal opportunities. (See Increasing job embeddedness.)
Increasing job embeddedness
Not all of these examples of job embeddedness efforts by Fortune 100 Companies apply to nursing, but they may be worth considering.
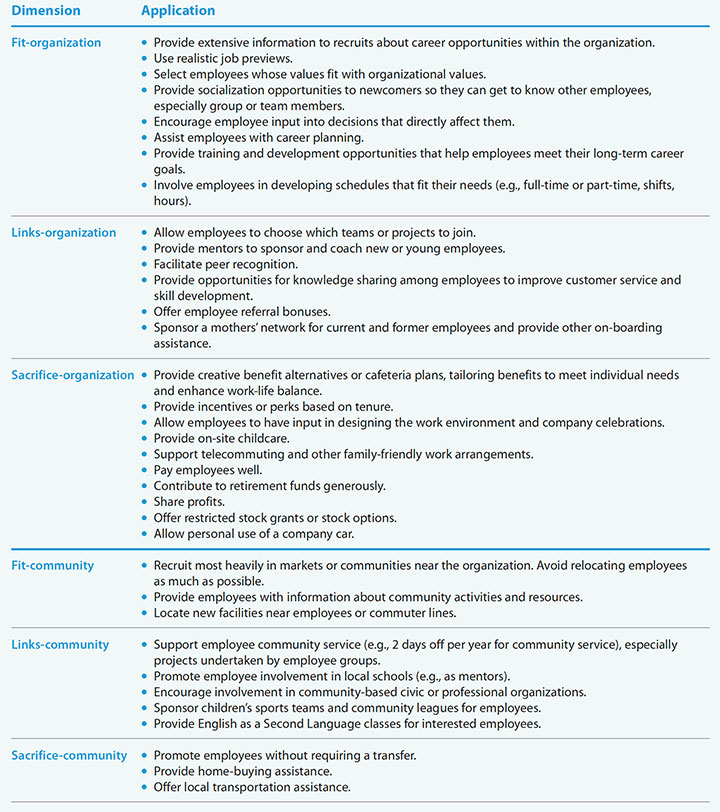

Using locus of control as a hiring strategy can strengthen organizational job embeddedness. For example, Ng and Feldman found that employees with a strong internal locus of control can better negotiate deals for unique contracts and develop strong social network links, thus improving the fit- and links-organization concepts. Leaving the organization will be more of a sacrifice for these employees than for those who don’t make those investments in their careers.
Examples of job embeddedness in healthcare
Stroth explains the advantages of applying job embeddedness strategies in rural areas and provides specific examples.
- A hospital in Arkansas, with a turnover rate of 127% among patient care intake specialists, adopted the job embeddedness model and focused their retention efforts on the fit concept. They reduced the turnover rate to 15%.
- A rural hospital in Illinois focused on the sacrifice-community concept and offered their employees down payment assistance to buy a house. The hospital incorporated stipulations, including that the employee must stay for at least 5 years and that the house should be no more than 10 miles from the hospital.
- Another organization allows employees to take 5 days off per year to attend their children’s school activities.
- One organization offers employees onsite oil changes and laundry services.
Supporting nurses
Nobody can predict the long-term consequences of the pandemic on the nursing profession. However, when organizations make efforts to improve job embeddedness now, they’re performing an act of care that will support the nursing workforce. (See Supporting nurses now.)


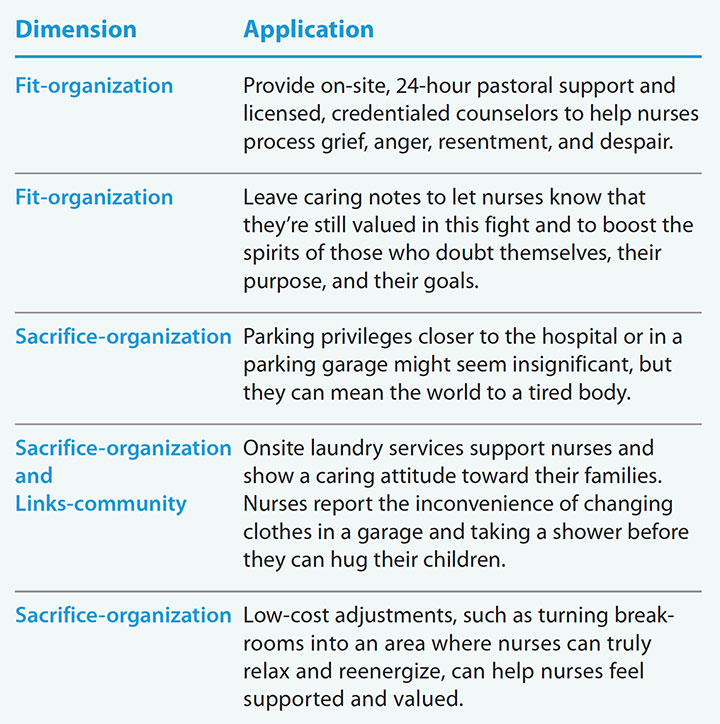
Supporting nurses now
Nurses who have worked on COVID-19 units and may be on the brink of burnout and post-traumatic stress disorder need support to move forward. Timely efforts to improve job embeddedness may help prevent a significant exodus from the profession.

Zelda Gibbs is an assistant professor of nursing at Tarleton State University in Fort Worth, Texas.
References
Cai Z, Cui Q, Liu Z, et al. Nurses endured high risks of psychological problems under the epidemic of COVID-19 in a longitudinal study in Wuhan China. J Psychiatr Res. 2020;131:132-7. doi:10.1016/j.jpsychires.2020.09.007
Gibbs Z, Duke G. Job embeddedness: The differences between registered nurses and healthcare assistants. West J Nurs Res. 2020:193945920963801. doi:10.1177/0193945920963801
Holtom BC, Mitchell TR, Lee TW. Increasing human and social capital by applying job embeddedness theory. Org Dyn. 2006;35(4):316-31. doi:10.1016/j.orgdyn.2006.08.007
Li X, Zhou Y, Xu X. Factors associated with the psychological well-being among front-line nurses exposed to COVID-2019 in China: A predictive study. J Nurs Manag. 2021;29(2):240-9. doi:10.1111/jonm.13146
Mitchell TR, Lee TW. The unfolding model of voluntary turnover and job embeddedness: Foundations for a comprehensive theory of attachment. Res Org Behav. 2001;23:189-246. doi:10.1016/S0191-3085(01)23006-8
Ng TWH, Feldman DC. Locus of control and organizational embeddedness. J Occup Organ Psychol. 2011;84(1):173-90. doi:10.1348/096317910X494197
Raudenská J, Steinerová V, Javůrková A, et al. Occupational burnout syndrome and post-traumatic stress among healthcare professionals during the novel coronavirus disease 2019 (COVID-19) pandemic. Best Pract Res Clin Anaesthesiol. 2020;34(3):553-60. doi:10.1016/j.bpa.2020.07.008
Stroth C. Job embeddedness as a nurse retention strategy for rural hospitals. J Nurs Adm. 2010;40(1):32-5. doi:10.1097/NNA.0b013e3181c47d30



















1 Comment.
There is no mention of adequate and appropriate staffing levels, the lack of which causes more stress and anxiety to nurses than any other factor. Other discouraging factors include lack of respect as an equal team member and unfair treatment by administration and physicians (who are treated as guests of the hospital.) Lack of control of work schedules (which is more pronounced when chronic inadequate and unsafe staffing levels exist) is also a great stress factor for hospital staff nurses. Some of the report (support for telecommuting) is irrelevant for most acute care staff hospital nurses.