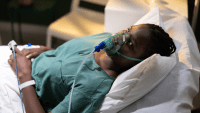
“I am a 59-year-old female recently diagnosed with Stage 2 COPD and chronic bronchitis. I smoked for 22 years. I have been hospitalized twice in the last seven months and have made several trips to the ER and urgent care. I am on and off antibiotics and steroids. I do daily breathing treatments and use Adair Diskus, Atrovent, and ProAir. I won’t leave home without the ProAIR.
I have a chronic cough that is sometimes dry when I’m off antibiotics but eventually the mucous build up returns. I used to work out three or four times a week and now I can barely walk a few feet without shortness of breath. I am not on oxygen, thank goodness, but I’ve been unable to work for the last three months. I feel like this disease is winning and I have no control. I guess I am looking for some hope because I don’t see the light at the end of the tunnel.”
This woman’s self-description of her health status was written on an Internet support blog for people with COPD. Her story encapsulates the course of this progressive and unstoppable disease for many people. But she is wrong in saying there is no light at the end of the tunnel.
What is COPD?
COPD is not curable. But there are medical and surgical treatments and self-help interventions that can significantly improve quality of life for the approximately 11 to 15 million Americans diagnosed with the disease, according to the COPD Foundation.
COPD is an umbrella term that encompasses emphysema, chronic bronchitis and, in some people, asthma. These conditions limit airflow into and out of the lungs. Airflow is limited because –
- the walls between many of the alveoli are destroyed;
- the walls of the bronchioles become thick and inflamed and produce more mucus, which can cause them to clog; and
- the walls of both the bronchioles and alveoli lose their elasticity.
All of the above factors lead to reduced oxygen exchange in the lungs.
Tobacco smoking or exposure to its smoke causes most cases of COPD. But it can also be caused by environmental air pollutants, infections and, in a small minority of people, the inherited alpha-1 antitrypsin deficiency.
Insidious lung disease is a worldwide problem
COPD is the third cause of death among Americans, many of whom do not even know what the initials COPD stand for never mind what it is. Ironically, Americans are much better educated about the first two killers: heart disease and cancer.
COPD is a global health problem as well. “It is a common, complex, and heterogeneous disorder that is responsible for substantial and growing morbidity, mortality, and healthcare expense worldwide,” according to an article in the May 2015 British Medical Journal The Lancet.
The World Health Organization’s goals of effective COPD management are to:
- Prevent disease progression
- Relieve symptoms
- Improve exercise tolerance
- Improve health status
- Prevent and treat complications
- Prevent and treat exacerbations
- Reduce mortality
COPD symptoms include coughing that produces large amounts of mucus, wheezing, shortness of breath, and chest tightness. Because the disease is insidious, most people are diagnosed in the later stages of the disease when the symptoms become more noticeable and start interfering with daily life. But some people may not have any symptoms, and COPD is detected coincidentally with another medical issue. Usually people are diagnosed in their late 40s, 50s, or older.
A definitive diagnosis of COPD is made through spirometry, which measures the volume and/or speed of air flow that can be inhaled and exhaled using a spirometer. The most common measurements used are: forced expiratory volume (FEV) and forced expiratory volume in one second (FEV1). This is the amount of air a patient can blow out within one second.
Hallmarks of COPD are the acute exacerbations of signs and symptoms that impair patients’ quality of life and decrease their health status, such as that of the COPD patient in the beginning of the article.
Patient involvement in care is essential
Some of the treatments and interventions that help patients cope with exacerbations and improve quality of life include medications; pulmonary rehabilitation, physical activity training, lifestyle changes, oxygen treatment and, in extreme cases, lung-reduction surgery.
Medications are administered using various bronchodilators, anticholinergics, steroids, and enzyme inhibitors. Inhalers are used to deliver medications such as –
- Short-acting bronchodilators such as Arcapta Neohaler and Servent Diskus
- Combination medications such as Advair Diskus, Symbicort, and Breo
- Anticholinergics such as Anoro, Combivent Respimat, Spiriva, and Tudorza
Physical activity training has the same benefits for people with COPD as for those without, even if they experience SOB. The right amount and type of exercise can reduce anxiety and insomnia and increase fitness and energy levels.
Oxygen Treatment is used when patients become hypoxic. It can be a long-term or short- term therapy to improve quality of life.
Lifestyle changes: The most important change is to stop smoking. Quitting smoking will slow the progression of COPD. Smoking will only make it worse.
Of course, there are other changes as well, such as staying active, avoiding air pollutants, such as pollen, and seeking emotional and social support.
There are many online resources now for patients that provide clear and useful information. But perhaps most important of all, they provide avenues to connect with other people who are also trying to live the best they can with COPD. A quick Google search results in numerous COPD related sites. They include:
- http://www.copdfoundation.org/
- http://www.thoracic.org/
- http://www.chestnet.org/Foundation/Patient-Education-Resources/COPD
- http://www.lung.org/lung-health-and-diseases/lung-disease-lookup/copd/
A message of hope
Hopefully, the woman at the start of this article took solace in a subsequent post that said, “If there is anything that I have learned from this site and its contributors, it is to do something and to feel good about doing it every day. As members of a site who are facing difficult physical, medical, and emotional challenges, I propose that if only for one minute, reflect on something that you did today that gave you a sense of accomplishment.”
Janet Boivin is a freelance writer and a staff nurse for a free clinic in Illinois.

















3 Comments.
I started on COPD/Asthma Herbal formula treatment from Akanni herbs centre , the treatment worked incredibly for my lungs condition. I used the herbal treatment for almost 5 months, it reversed my chronic obstructive pulmonary disease. My severe shortness of breath, dry cough, low energy, fatigue, chest tightness and others gradually disappeared. Visit Akanni herbs clinic official web page Akanniherbalcentre com This COPD treatment has improved the quality of my life greatly, i breath much better and It feels comfortable!
My husband is 54 and has had Parkinson’s for around 3-4 years. It is a debilitating disease that only gets worse and needs some serious funding to find out 1 because the cure is out there. What causes it and 2. some better treatment for it which multivitamincare org have the guaranteed cure for PD. He takes over 8 weeks treatment from Multivitamin care formula that finally cure him,as there is no-one available to help unless you have per week money to pay for a Nurse, but with this herbal system you can get rid of your Parkinson effectively ,he had tremors for several years and was gradually becoming worse before we found PD supplement from Multivitamincare that was able to get rid of my husband disease and alleviate all symptoms within the short period of his usage.,they have the best medication for PD.
My mother have been suffering from fibromyalgia disease for the last 3 years and had constant pain, especially in her neck,During the first year,she had faith in God that she will be healed someday by the Almighty. This disease started circulate all over my moms body and she have been taking treatment from her doctor, few weeks ago i came on search on the internet if i could get any information concerning the prevention of this disease, on my search i saw a testimony of someone who has been healed from (fibromyalgia) by this man DR Abumere and she also gave the email address of this man and advise we should contact him for any sickness that he would be of help, so i wrote to DR Abumere telling him about my mothers fibromyalgia disease he told me not to worry that my mom is gonna be okay with his herbal remedies!! actually i never believed it,, well after all the procedures and remedy given to me by this man i went to discuss it with my mom and explain everything to her on what she is about to take in,because Dr Abumere told me my mother must stop other medication just to make sure his own work properly,she agreed because this great doctor gave me assurance about his good work.
Weeks later after my mother start using this herbal medicine she started experiencing changes all over her as the DR assured me that she will cured,after some time i went to her doctor to confirmed if she has finally healed behold it was TRUE, So dear viewers my advise is if you have such sickness or any other at all you can email DR Abumere on: abumereherbalcentre @ gmail. com or visit his websit: www . abumereherbalcentre . simplesite . com
thank you doctor i will forever be grateful.