Alleviate barriers with collaboration.
Takeaways:
- An organizational infrastructure promoting a culture of inquiry is essential to advance nursing science with research and dissemination of findings.
- Minimizing barriers increases the comfort level of staff for the successful conduct of the nursing research process.
In the fourth component for Magnet® designation, the American Nurses Credentialing Center outlines the ethical and professional responsibility of organizations to positively impact patient care via current knowledge, innovations, and improvements. This component includes generating new evidence and contributing to the advancement of nursing science with research and outcome dissemination. Organizations that promote a culture of inquiry with an infrastructure that supports nursing research at the bedside and chairside help meet this responsibility.
A culture of inquiry encourages nurses to question practice, review existing literature, and integrate evidence-based outcomes that improve patient care. If not enough evidence exists to support change, nurses must conduct research. However, common barriers—lack of time, resources, knowledge, and support—may deter bedside nurses from taking on this work. The department of nursing research at Moffit Cancer Center helps alleviate these barriers for bedside nurses.
Two clinical nurse specialists (CNS)—one a nurse researcher and the other a blood and marrow transplant and cellular immunotherapy (BMT-CI) CNS—collaborate to alleviate barriers and lay the groundwork for successful implementation of research by bedside nurses.
Roles and responsibilities
The nurse researcher is an oncology CNS who transferred from the traditional CNS role. Within the department of nursing research, which was created in 2007, she assists with Magnet initiatives related to promoting a culture of inquiry by developing new evidence and advancing nursing science. Her main responsibilities center around establishing protocols and obtaining regulatory approval from the center’s internal scientific review committee and external institutional review board (IRB). She works closely with the biostatisticians for each study’s data analysis plan and disseminates updates to hospital leadership and nursing councils.
The CNS who supports BMT-CI works with staff nurses reviewing the literature for evidence-based practice related to their queries. If evidence is lacking, which frequently is the case within specialty populations, she encourages conducting or replicating a research study. Based on nurse interest, she discusses feasibility of the idea with the nurse researcher. The BMT-CI CNS focuses on staff education for the study, data collection, and data entry. Throughout the study, she mentors the principal investigator staff nurse and the research team.
Overcoming the time barrier
Staff nurses at the center receive protected time for reviewing the literature when searching for evidence related to patient care or generating an idea for a research study. The nurse researcher and BMT-CI CNS work collaboratively with the potential study team to develop a research proposal, which the Nursing Research & Evidence-Based Practice Council (formerly the Nursing Research & Innovation Council) then vets. The proposal, a one- to two-page summary, includes background, a purpose statement, research questions, study design, recruiting the strategies, and impact. (See Make a proposal.)


Before presenting the proposal to the council, the principal investigator’s supervisor signs off on the study. This ensures the principal investigator has up to 4 hours of protected time each pay period to work on study-related projects (Collaborative Institutional Training Initiative [CITI] training, informed consent, data collection), which helps alleviate time barriers to research. Other research team members may receive protected time, especially during the literature review and data collection, at the discretion of their supervisors.
Overcoming the resource barrier
The department of nursing research collaborates with biomedical librarians, biostatisticians, the organization’s scientific review committee, and the IRB. The nurse researcher and BMT-CI CNS can use these resources when working with staff nurses to write the research protocol before submitting it to the nursing research and innovation council. After approval and implementation of final changes, the nurse researcher submits the proposal to the scientific review committee and IRB. The nurse researcher and BMT-CI CNS also coordinate meetings with the research team to answer questions, discuss study protocols, and reinforce timelines and deadlines.
Biomedical librarians offer classes on database searching and provide one-on-one support. The biostatistician, who serves as a member of the study team, meets with team members after data analysis is completed to ensure they understand the results and to assist with manuscript preparation, particularly the data analysis and results sections.
Overcoming the knowledge and support barrier
Before data collection, the principal investigator completes the CITI-approved training as outlined in the center’s research policy. This provides a broad overview of how to conduct research and protect human subjects. The nurse researcher and CNS answer questions and offer support throughout the research process. For example, they help with writing protocols, creating spreadsheets, and entering data.
After completing the study, the nurse researcher and CNS assist staff nurses with internal and external dissemination. Within the organization, the study team presents their findings to the clinical unit, nurse executive council, coordinating practice council, and other shared governance councils and committees as appropriate. Externally, the team disseminates their research to professional nursing organizations and conferences.
Dissemination education and support include abstract writing and submission, poster or podium presentation preparation, and manuscript development and submission. Nurses also receive support with time off and funding to present their findings at external conferences.
Outcomes
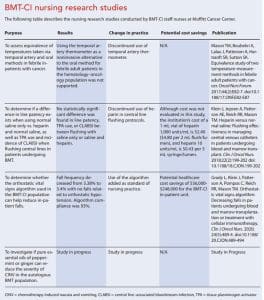
From 2014 to 2021, 12 BMT-CI nurses participated in four research studies as team members or principal investigators. Other unit nurses received education about study processes and assisted with study interventions. Three completed studies (the fourth is in progress) have resulted in abstract submissions and presentations at six conferences. All three studies have been published. With the support of both nursing and the organization’s executive leadership, study outcomes have resulted in practice changes and house-wide implementation. (See BMT-CI nursing research studies.)

Nurse-friendly research
By collaborating within their respective roles and using the resources provided by the department of nursing research, the Moffitt Cancer Center nurse researcher and BMT-CI CNS have minimized the barriers to research and increased staff comfort with the research process. Since the success of the initial study, the CNSs have built momentum by enriching a spirit of inquiry that continues, making research bedside-nurse friendly.
The authors work at Moffitt Cancer Center in Tampa, Florida. Tina M. Mason is a nurse scientist. Amy E. Patterson is a clinical nurse specialist.
References:
American Nurses Credentialling Center. Magnet model—Creating a Magnet culture.
Birkhoff SD, Nair JM, Monturo C, et al. Increasing nursing research capacity: The roles and contributions of nurse scientists within healthcare systems in the Greater Philadelphia region. Appl Nurs Res. 2020;55:151288. doi: 10.1016/j.apnr.2020.151288
DeGrazia M, Defazio RL, Conner JA, Hickey PA. Building and sustaining a culture of clinical inquiry in a pediatric quaternary hospital. J Nurs Adm. 2019;49(1):28-34. doi:10.1097/NNA.0000000000000704
Scala E, Price C, Day J. An integrative review of engaging clinical nurses in nursing research. J Nurs Scholarsh. 2016;48(4):423-30. doi: 10.1111/jnu.12223
Sy V. Igniting the fire of inquiry: Strategies to advance hospital nursing research. Nurs Manage. 2020;51(6):50-3. doi: 10.1097/01.NUMA.0000662708.03559.19
Wentland BA, Hinderer KA. A nursing research and evidence-based practice fellowship program in a Magnet®-designated pediatric medical center. Appl Nurs Res. 2020;55:151287. doi: 10.1016/j.apnr.2020.151287




















2 Comments. Leave new
Thank you for sharing your propsal template! I think it’s brilliant.
Thank you! It definitely helps the staff with the vetting process.