Nursing leaders—including managers, directors, and executives—are dedicated to advancing nursing excellence and inspiring and empowering teams. They must analyze nursing knowledge and practice environments, and strategize to ensure that safe, evidence-based nursing care is provided for positive patient outcomes. More than ever, the expertise and skills of the nurse leader in recognizing the value of creating and sustaining diverse, healthy work environments are essential to support nurse health and safety. Nurse leaders must not only role model, but also possess knowledge of healthy behaviors and practices to support wellness initiatives and healthy work environments for employees. They promote better health for patients and staff, but do they do the same for themselves? This report summarizes the current state of nurse leaders’ health behaviors.
On May 1, 2017, the ANA Enterprise launched the Healthy Nurse Healthy NationTM (HNHN) Grand Challenge focused on improving the health of the nation by improving the health of its nurses. The foundation of this national initiative is to make nurses’ health a national priority because their health, safety, and wellness have been shown to have a direct impact on patient outcomes. HNHN is dedicated to supporting and encouraging nurses to take action to improve both their personal and professional health within five domains: physical activity, rest, nutrition, quality of life, and safety. Previous data published from ANA’s 2013-2016 Health Risk Appraisal (HRA) showed room for improvement in nurses’ and nursing students’ health in all five domains. The fundamental principle to being a healthy nurse is prioritizing self to provide optimal patient care.
The HealthyNurse Leader results were obtained from anonymous HealthyNurse® Surveys completed from May 2017 to December 2018 through the HNHN Connect community. This sample of nurse leaders includes 2,047 RN or advanced practice RN respondents currently working in administration, leadership, and/or management positions. The demographic results of this nurse leader sample were primarily female (92%) and caucasian/white (82%) with an average age of 50 years. The mean height and weight were 5’4”, 177 pounds with a body mass index (BMI) of 30.4. Almost half (49%) of this sample were ANA members, and 31% worked for organizations that have received American Nurses Credentialing Center Magnet® recognition.
Work environment
The survey’s work environment questions focused on occupational health, safety, and wellness. Respondents identify workplace stress and excessive fatigue that impacts quality of life as the top two work environment risk factors for nurse leaders. They report working on average 41 to 60 hours per week, believe that their employer values their health and safety (81%), say that they’re treated with dignity and re-spect at work (84%), and feel recognized and thanked for their work (78%). In addition, most respondents say they frequently put the health, safety, and well-ness of patients before their own (61%).Nurse leader respondents report receiving adequate education and training on workplace bullying and violence prevention protocols and policies; 27% say they were victims of verbal or nonverbal aggression from a person in a higher level of authority and 34% were victims of verbal or nonverbal aggression from a peer.
Nutrition and physical activity
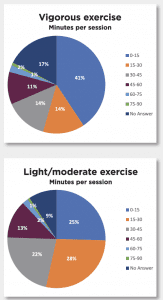

Nurse leaders’ responses on nutrition and physical activity habits yielded mixed results. In general, more than half report they have access to worksite wellness programs; however, fewer than half participate in the programs or have received self-care well-ness training (such as mindful-ness, resiliency, and stress reduction). Approximately 62.4% say that healthy food choices are available at work, but that they’re more expensive than less healthy options.
Nurse leader respondents engage in light or moderate aerobic work-outs an average of 2.5 days per week, vigorous aerobic workouts 1.6 days per week, and muscle-strengthening exercises 1.2 days per week spending less than 30 minutes per session. In comparison to others their age, over 60% of respondents describe their health as good, very good, and/or excel-lent. On average, respondents eat 2.9 servings of fruits and vegetables and 1.7 servings of whole grains daily. Sixty-seven percent eat food from a restaurant, fast food chain, cafeteria, or similar setting one to four times a week.
Quality of life and safety
Issues around nurse leaders’ quality of life and safety also were addressed in the survey. More than half of nurse leader respondents say they arrive early, stay late, and work through breaks to complete their work. Despite this and in addition to rating workplace stress as the number one risk factor, only 25% of respondents feel they have a higher workload than they’re comfortable with. They sleep on average 6 to 7 hours per night and missed an average of 3 days of work due to illness in the last year. Nurse leader respondents (35%) report that they “usually” get the emotional support they need; 10% “rarely” or “never” get need-ed emotional support. Within the last year, 75% of nurse leaders say they did not feel sad, down, or depressed for 2 weeks or more in a row; 25% say they did. In the past 30 days, a little over half did not experience pain or physical or mental health issues that prevented them from doing their usual activities.
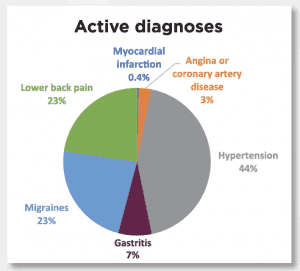

Healthcare providers most commonly identify hyper-tension (44%) as an active diagnosis for nurse leaders, followed by lower back pain and migraines (23% for each). Almost all respondents receive the seasonal flu vaccine and do not smoke. Additionally, most nurse leaders indicate they have not nodded off or fallen asleep, even for a brief moment, while driving, and that they “seldom” text and drive.
Healthy nurse leaders needed
These preliminary results from the HealthyNurse Survey show that nurse leaders struggle most with maintaining a healthy diet and BMI, reducing work-place stress, and creating an appropriate work/life balance. As the largest subset of healthcare workers, nurses are critical to America’s healthcare system. Nurse leaders are essential to organizational success because of their impact on patient outcomes at the point of care, their ability to drive organizational initiatives at the unit level, and their vital role in ensuring healthy work environments. In turn, healthy work environments provide the atmosphere for nurses and patients to thrive and succeed.
Taking the HealthyNurse Survey and participating in the HNHN Connect community is a positive first step to empower nurse leaders as well as other nurses. Identifying your current state of health and how it impacts all aspects of life, both personally and professionally, provides the ability to create a personalized definition of health and wellness and better understand what can be achieved. Once defined, nurse leaders can evaluate what’s working and uncover opportunities to support their own health and wellness. Of course, none of this information is beneficial without committing to a sustained action plan and prioritizing self-care. Self-care is not selfish nor is it self-indulgent. It is vital to being our best selves.
The well-being of nurse leaders is fundamental to the health of our nation. In 2020, the ANA Enterprise and organizations around the world are celebrating the “Year of the Nurse.” There is no better time than now to commit to prioritizing your own self-care and wellness. Let’s also designate this year as the “Year of You.”
— Stephanie Nolan is director of nursing perianesthesia services at New York-Presbyterian Hospital, Weill Cornell Medical Center. She is an ANA-New York member. Holly Carpenter is senior policy advisor in the Nursing Practice and Work Environment and Innovation departments at the American Nurses Association. Loressa Cole is chief executive officer of the ANA Enterprise. Joyce J. Fitzpatrick is vice chair of the American Nurses Foundation. She is the inaugural director of the Marian K. Shaughnessy Nurse Leadership Academy and the Elizabeth Brooks Ford Professor of Nursing at the Frances Payne Bolton School of Nursing, Case Western Reserve University in Cleveland, Ohio.














