Survivor care continues long after treatment ends.
Takeaways:
- Long-term effects of breast cancer treatment include fatigue, hot flashes and night sweats, sexual dysfunction, sleep disturbance, weight changes, and fear of recurrence.
- Nursing interventions contribute to quality cancer care in the extended phase of cancer survivorship.


After a breast cancer diagnosis, patients must navigate a host of difficult treatment decisions, debilitating physical and psychological symptoms, and treatment side effects. Even after completing treatment, many patients continue to struggle with significant physical and emotional stress, including anxiety, fear of recurrence, depression, and feelings of hopelessness and isolation. Before the most recent advances in cancer research, patients generally perceived quality cancer care as achieving remission after treatment. Patients now find themselves living with long-term treatment effects for which they may have received little education to manage. And, unfortunately, their primary care providers also may lack formal education of cancer treatment’s side effects.
Addressing long-term side effects
Opportunities for addressing comprehensive survivorship care exist in many cancer settings. For example, integration of survivorship care for breast cancer survivors should be implemented upon initial diagnosis with the start of adjuvant therapy. At the Greenville Health System Cancer Institute, Center for Integrative Oncology and Survivorship (CIOS), patients with breast cancer can attend an integrative oncology visit with a survivorship nurse practitioner (NP) and survivorship nurse navigator as soon as they’re diagnosed. In preparation for the integrative oncology visit, the nurse navigator reviews the patient’s health record to anticipate individual patient needs. During the visit, the NP assesses the patient for physical and psychosocial needs and provides referrals and resources to appropriate support services within CIOS and the community.
All nurses—whether they work in oncology settings or primary care—should have a basic understanding of the long-term effects of breast cancer treatment, including fatigue, hot flashes and night sweats, sexuality and intimacy difficulty, sleep disturbance, weight changes, and fear of recurrence.
Fatigue
Cancer-related fatigue (CRF) is the most common side effect of cancer treatment.
Overview: The National Comprehensive Cancer Network defines fatigue as a feeling of ongoing, draining exhaustion that limits the patient’s ability to participate in activities and interferes with quality of life. CRF may last for months or even years after completing cancer therapy.
Symptoms of CRF include a combination of subjective and objective conditions that the cancer survivor perceives as overwhelming. Some patients report a constant lack of energy and an inability to participate in normal activities of living. They frequently report feeling tired even after 8 hours of sleep. Many patients also correlate fatigue with cognitive deficits such as trouble concentrating and finding words. (See Fatigue assessment.)
 |
Management: According to the National Cancer Institute, exercise is the most effective intervention for CRF. Other benefits of exercise include reducing the chance of breast cancer recurrence, maintaining a healthy body weight, increasing mobility, building self-esteem, improving sleep hygiene, reducing treatment-related side effects, and achieving faster recovery from cancer treatments. (See Move it.)
Move it
|
Refer patients to an exercise program such as oncology rehabilitation after they complete cancer treatment. These programs introduce patients who are sedentary to the concept of exercise. And for those patients who were active before their diagnosis, rehabilitation programs can help them regain mobility, strength, and endurance that was lost during treatment.
Hot flashes and night sweats
Vasomotor symptoms (hot flashes or night sweats) are commonly reported by breast cancer survivors.
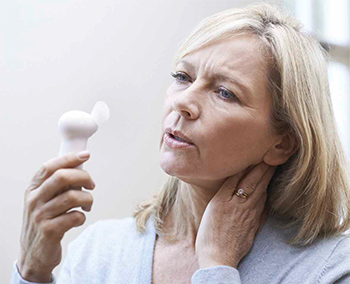
Overview: Hot flashes are defined as a temporary but sudden onset of body warmth accompanied by facial flushing with or without sweating. Hot flashes and night sweats (hot flashes experienced while sleeping) occur in both women and men. The onset of hot flashes varies among breast cancer survivors and may be reported as sudden or gradual. Hormone-blocking medications and nonhormonal pharmacologic cancer therapies used in breast cancer therapy contribute to these symptoms.
According to the National Cancer Institute, approximately two-thirds of women who are postmenopausal and have a history of breast cancer experience hot flashes that interfere with quality of life by affecting sleep, mood, and concentration. A thorough assessment of quality of life is necessary to determine the need for education and intervention. (See Assessment in a flash.)
Assessment in a flashHot flashes are a common side effect of breast cancer treatment. Use the Hot Flash Related Daily Interference Scale (http://bit.ly/2Q9Yi1Z) to assess the effects of hot flashes on patients’ quality of life.
|
Management: Educate patients about diet and behavioral triggers that may precipitate and contribute to the frequency and severity of hot flashes and night sweats. Explain that they should avoid alcohol and caffeine, hot or spicy food, hot baths or showers, and smoking. Healthy lifestyle changes include regular exercise, a balanced nutritious diet, and stress-reduction techniques such as yoga. As with any behavior change, patients may resist, so encourage slow, subtle, and attainable goals on their quest for a healthy lifestyle.
Sexuality and intimacy
The inability to engage in sexual activity because of lack of desire, inability to achieve orgasm, or pain with intercourse are collectively classified as symptoms of sexual dysfunction.
Overview: Breast cancer therapy can propel women into menopause, causing a distressing cascade of physical symptoms that result in sexual dysfunction. The psychological effects of a cancer diagnosis—anxiety and depression— and pre-existing stress and spousal conflict can worsen sexual dysfunction.
Management: Discussing sexuality can be difficult for some patients and requires your sensitivity. The PLISSIT model promotes discussion with open-ended questions, information, specific suggestions, and referrals. (See Discussing sexual health.)
Discussing sexual health
Sexual dysfunction that results from breast cancer treatment side effects can be addressed using the PLISSIT model to promote candid conversations between patients and clinicians. Permission—Create a comfortable environment by asking patients open-ended questions and giving them permission to talk about what they perceive as problems with their sexual health. Limited Information—After a sexual problem has been identified, provide the patient with specific information and examples about the nature of the sexual problem, including signs and symptoms and how best to approach treatment. Specific Suggestions—To give patients specific suggestions, you must thoroughly understand the dynamics and consequences of the identified sexual issues. When you’re equipped with this knowledge, you can play a significant role in helping the patient identify coping and management strategies. Intensive Therapy—Make referrals for additional physical and psychological support and guidance. Referrals for sexual dysfunction may include sexual health counselors, pelvic floor physical therapists, and self-help websites (such as will2love.com) that offer evidence-based strategies for managing many sexual health issues, such as relieving vaginal dryness, reducing pain during penetration, and addressing lack of sexual arousal and inability to climax. |
Sleep disturbance
Sleep disturbance is reported by 30% to 75% of patients newly diagnosed or recently treated for breast cancer. This is about two times higher than in the general population.
Overview: Sleep disorders are described as changes in one’s sleep pattern. Insomnia is common among breast cancer survivors and can manifest as difficulty falling asleep or staying asleep. Common causes of insomnia include anxiety and depression, which typically are provoked by diagnosis, cancer treatment modalities including steroidal medications, and hot flashes. Talk with the patient about past and present sleep patterns, especially difficulty falling asleep or staying asleep. Ask the patient how long it takes to fall asleep to help you understand the underlying causes of the insomnia. Many patients say that they find themselves lying awake for prolonged periods of time, and when questioned further, they admit to persistent thoughts of worry and that their minds are “constantly racing,” preventing relaxation.
Management: Eliminating sleep disturbances requires a solid sleep routine. Talk to patients about establishing consistent bedtimes and waking times, ensuring a cool dark environment, incorporating mindful breathing techniques and yoga, adding comfort measures such as warm baths before bed, and eliminating all electronic devices (cell phones, tablets, television) at least 2 hours before bedtime. Also instruct them to use the bedroom only for sleep and sexual activity.
Weight changes
Weight gain is a prevalent problem among patients treated for breast cancer.
Overview: Makari-Judson and colleagues report that weight gain of 2.5 to 11 lbs during breast cancer diagnosis and treatment is associated with loss of lean body mass and fat gain. This most commonly occurs in patients younger than 50 years old who require chemotherapy.
The incidence of weight gain during breast cancer therapy has increased throughout the years. Before the 1990s, weight gain was a less prevalent side effect of treatment because of few effective antiemetic agents. Anthracycline-based regimens, which are commonly used in breast cancer treatment, are highly emetogenic and have prompted the development of more effective antiemetic drugs. Adjunctive steroid medications are used to complement the effects of antiemetics; however, they contribute to increased appetite and weight gain.
Management: Women who gain more than 13 pounds during breast cancer diagnosis and treatment have a 1.5 times increased risk for breast cancer recurrence. To reduce chances of weight gain, begin prevention strategies at diagnosis.
After identifying risk factors for weight gain, implement behavior-modification techniques and goal setting. Provide referrals to a dietitian for education about the importance of a plant-based diet that includes at least five servings of fruits and vegetables each day. Phytochemicals in plant-based food groups protect human cells from oxidative damage that can lead to cancer. Also explain that engaging in moderate physical activity before treatment begins can help decrease fatigue levels by 40% to 50%.
After completing breast cancer treatment, patients may have difficulty implementing a daily exercise routine because of the profound fatigue and physical deconditioning that accompanies treatment and being sedentary. Many communities have programs dedicated to creating lifestyle and behavior change. For example, the Moving On oncology rehabilitation program at Greenville Health System provides a 3-month philanthropically supported exercise program for cancer survivors. It’s directly supervised by an oncology certified registered nurse and three oncology certified physical trainers. Another option is the YMCA, which partners with LIVESTRONG to offer free or low-cost 3-month exercise programs for cancer survivors. The program includes exercise navigation for patients who need one-on-one guidance and support.
Fear of recurrence
Many cancer survivors struggle with the fear of disease recurrence after treatment has ended.
Overview: Completing cancer treatment is a celebratory moment typically marked by a bell-ringing ceremony. However, many patients experience high levels of anxiety as they leave the acute phase of survivorship and enter an extended phase. They may fear no longer being followed by their oncology providers and nurses as often as they were during active treatment, and they miss the frequent social interaction with patient peers. In the extended phase of survivorship, patients often live each day worrying about every ache and pain and the possibility of cancer progression or spread. Although thoughts of cancer recurrence plague many patients at levels that affect their quality of life, a certain level of anxiety is necessary to promote adherence to recommended cancer surveillance and follow-up.
Management: Teach patients about strategies to identify and control triggers that escalate their fear and anxiety. Triggers may include scheduled follow-up examinations, a cancer diagnosis anniversary date, and annual cancer surveillance such as mammograms. Reassure patients that fear and anxiety are common, and encourage them to share their concerns with their healthcare team for referrals to support groups or individual counseling. Self-help strategies to relieve stress include mindfulness breathing techniques, yoga, and massage therapy.
Navigating survivorship
Effective navigation of breast cancer survivorship begins at diagnosis and lasts throughout the cancer continuum. Many providers lack knowledge of the debilitating late and long-term effects of cancer treatment, and nurses have an important role to play in educating their colleagues and patients. You can help close the gap in patient care by working with your oncology and non-oncology nursing peers to help guide the course of meaningful patient education, thereby improving patient outcomes.
Patricia Leighton is a survivorship nurse navigator at Greenville Health System Cancer Institute in Greenville, South Carolina.
Selected references
ACS guidelines for nutrition and physical activity. American Cancer Society. April 13, 2017. cancer.org/healthy/eat-healthy-get-active/acs-guidelines-nutrition-physical-activity-cancer-prevention/guidelines.html
Brief fatigue inventory. The University of Texas MD Anderson Cancer Center. mdanderson.org/research/departments-labs-institutes/departments-divisions/symptom-research/symptom-assessment-tools/brief-fatigue-inventory.html
Butow P, Sharpe L, Thewes B, Turner J, Gilchrist J, Beith J. Fear of cancer recurrence: A practical guide for clinicians. January 15, 2018. cancernetwork.com/oncologyjournal/fear-cancer-recurrence-practical-guide-clinicians.
Cancer stat facts: Female breast cancer. National Cancer Institute. seer.cancer.gov/statfacts/html/breast.html
Carpenter JS. Hot flash-related daily interference scale short form [poster]. 2017. sigma.nursingrepository.org/handle/10755/621500
Eldridge L. 9 ways to cope with the fear of cancer recurrence. February 5, 2018. verywell.com/coping-with-cancer-return-progression-2248862
Exercise for life. National Comprehensive Cancer Network. nccn.org/patients/resources/life_after_cancer/exercise.aspx
Exercising during cancer treatment. National Comprehensive Cancer Network. nccn.org/patients/resources/life_with_cancer/exercise.aspx
Fatigue (PDQ®)—Health professional version. National Cancer Institute. June 29, 2017. cancer.gov/about-cancer/treatment/side-effects/fatigue/fatigue-hp-pdq#link/_94_toc
Female sexual dysfunction: Symptoms and causes. Mayo Clinic. September 6, 2018. mayoclinic.org/diseases-conditions/femalesexual- dysfunction/symptoms-causes/syc-20372549
From cancer patient to cancer survivor: Lost in transition. The National Academies of Science Engineering Medicine. November 3, 2005. nationalacademies.org/hmd/Reports/2005/From-Cancer-Patient-to-Cancer-Survivor-Lost-in-Transition.aspx
Kwok A, Palermo C, Boltong A. Dietary experiences and support needs of women who gain weight following chemotherapy for breast cancer. Support Care Cancer. 2015; 23(6):1561-8.
LIVESTRONG at the YMCA. livestrong.org/what-we-do/program/livestrong-at-the-ymca
Makari-Judson G, Braun B, Jerry DJ, Mertens WC. Weight gain following breast cancer diagnosis: Implication and proposed mechanisms. World J Clin Oncol. 2014;5(3):272-82.
Palmisano B. PLISSIT model: Introducing sexual health in clinical care. Psychiatry Advisor. January 4, 2017. psychiatryadvisor.com/practice-management/improving-providereducation-regarding-sexual-health/article/629446
Patient and caregiver resources: Exercise. February 17, 2017. breastcancer.org/tips/exercise
Patient and caregiver resources: Fatigue. National Comprehensive Cancer Network. nccn.org/patients/resources/life_with_cancer/ managing_symptoms/fatigue.aspx
Patient and caregiver resources: Nutrition for cancer survivors. National Comprehensive Cancer Network. nccn.org/patients/resources/ life_after_cancer/nutrition.aspx
PDQ Supportive and Palliative Care Editorial Board. Hot flashes and night Sweats (PDQ®). March 14, 2018. ncbi.nlm.nih.gov/pubmed health/PMH0032590/
Phytochemicals. phytochemicals.info
Oncology rehabilitation. Greenville Health System ghs.org/healthcareservices/cancer/clinical-programs/moving-on/#14793223 60794-a4b93dc8-ff2d
Sleep disorders: Symptoms and causes. Mayo Clinic. September 14, 2016. mayoclinic.org/diseases-conditions/sleep-disorders/symptomscauses/syc-20354018
ant2-CE Survivorship-116






















2 Comments.
I’m an FNP and a breast cancer survivor. I struggle with all of these things daily. I feel like as a provider I should have known more about breast cancer and the side effects. I am two years out of treatment but still deal with the fatigue, sexual dysfunction, hot flashes, insomnia, lack of concentration, etc. and work daily to overcome.
I think that providing education to medical staff on these topics would be so helpful to women and bringing the questions up during visits, because many women are afraid to talk of their symptoms.
Thank You!!
I was diagnosed with breast cancer 6 months ago and began chemotherapy right away. I finished chemo 2.5 weeks ago and can absolutely relate to many of the treatment side effects. The information regarding the side effects and their management will be very helpful for me now and after my double mastectomy ( in 4 weeks). Thank you .