Follow these tips to keep your patients safe.
Takeaways
- Enteral nutrition (tube feeding) can be administered safely but is not without risks.
- Optimal nursing care can prevent many tube feeding related complications, including misconnections.
Enteral nutrition (EN), commonly called tube feeding, is defined by the American Society for Parenteral and Enteral Nutrition (ASPEN) as a system of providing nutrition directly into the GI tract via a tube, catheter, or stoma, bypassing the oral cavity. According to ASPEN, hundreds of thousands of patients in all age groups receive EN each year in U.S. hospitals, and many more in long-term care and home settings. It’s the preferred route for delivering nutrition to patients who can’t meet their nutritional needs with oral intake.
EN is a complex therapy with potential adverse events. Before recommending EN, a qualified nutrition clinician must evaluate indications and weigh individual patient risks and benefits. EN complications, which may be GI, infectious, mechanical, or metabolic, can be prevented with monitoring and evidence-based care protocols. (See EN complications.)
EN complications
Enteral nutrition (EN) complications can be classified as GI, infectious, mechanical, or metabolic. Here are a few examples in each category.
GI
- Abdominal discomfort
- Constipation
- Diarrhea
- Nausea
- Vomiting
Infectious
- Aspiration pneumonia
- Formula contamination
Mechanical
- Tube misplacement
- Tube obstruction
- Unintentional tube removal or dislodgement
Metabolic
- Electrolyte and mineral imbalances
- Fluid imbalances
- Glucose intolerance
- Vitamin deficiencies
This article focuses on five of the most commonly recommended strategies for reducing complications in short-term nasogastric (NG), nasoenteric (NE), and orogastric (OG) feeding tubes. (For the most part, discussion of NG feeding can be applied to OG and NE feeding.)
Use evidence-based methods to verify placement
Approximately 2% of NG tubes are misplaced during insertion, which, according to a review by Sparks, can result in serious complications, including pneumothorax, chemical pneumonitis, and death. Many organizations require a radiograph to verify NG tube placement, but concerns exist regarding accuracy and radiation exposure, especially in children. A review by Metheny and colleagues of 14 national guidelines found that most recommend radiography as the first-line verification measure in adults, followed by pH measurement, which is the most reliable bedside method for confirming NG tube placement.
Measurement of pH involves aspirating 1 to 2 mL of fluid from the NG tube and testing it for acidity. In many studies, a pH ≤5 or 5.5 is used to verify that the tube is in the stomach. Concerns about using this method in patients receiving acid-suppressing medication were mitigated when a retrospective review by Kemper and colleagues of over 1,000 enterally fed neonates (many of whom were receiving acid-suppressing medication) reported that 97% had a pH of ≤5 for initial and ongoing NG tube placement verification. However, adopting pH measurement for bedside NG tube placement verification has been slow.
A survey of 408 critical care nurses by Bourgault and colleagues reported that 76% still use auscultation, despite recommendations from their organizations to discontinue its use. Listening for a “whoosh” sound in the stomach to verify NG tube placement is unreliable because both the lungs and stomach are resonant organs. Nurses must stop using auscultation and start using pH measurement, which is reliable, evidence-based, and suitable for all patients.
Use new safer ENFit® connectors on all EN delivery devices
Enteral delivery systems consist of a feeding tube or device, an administration gravity or pump set, syringes, extension tubing, and other extra devices (such as a stopcock or drainage bag). Each time a connection between any of these devices is made, a risk of an enteral misconnection is possible. An enteral misconnection is defined as an inadvertent connection between an enteral feeding system and a non-enteral system such as an intravascular line, peritoneal dialysis catheter, tracheostomy tube cuff, or medical gas tubing. (See Continued misconnections.)
Continued misconnections
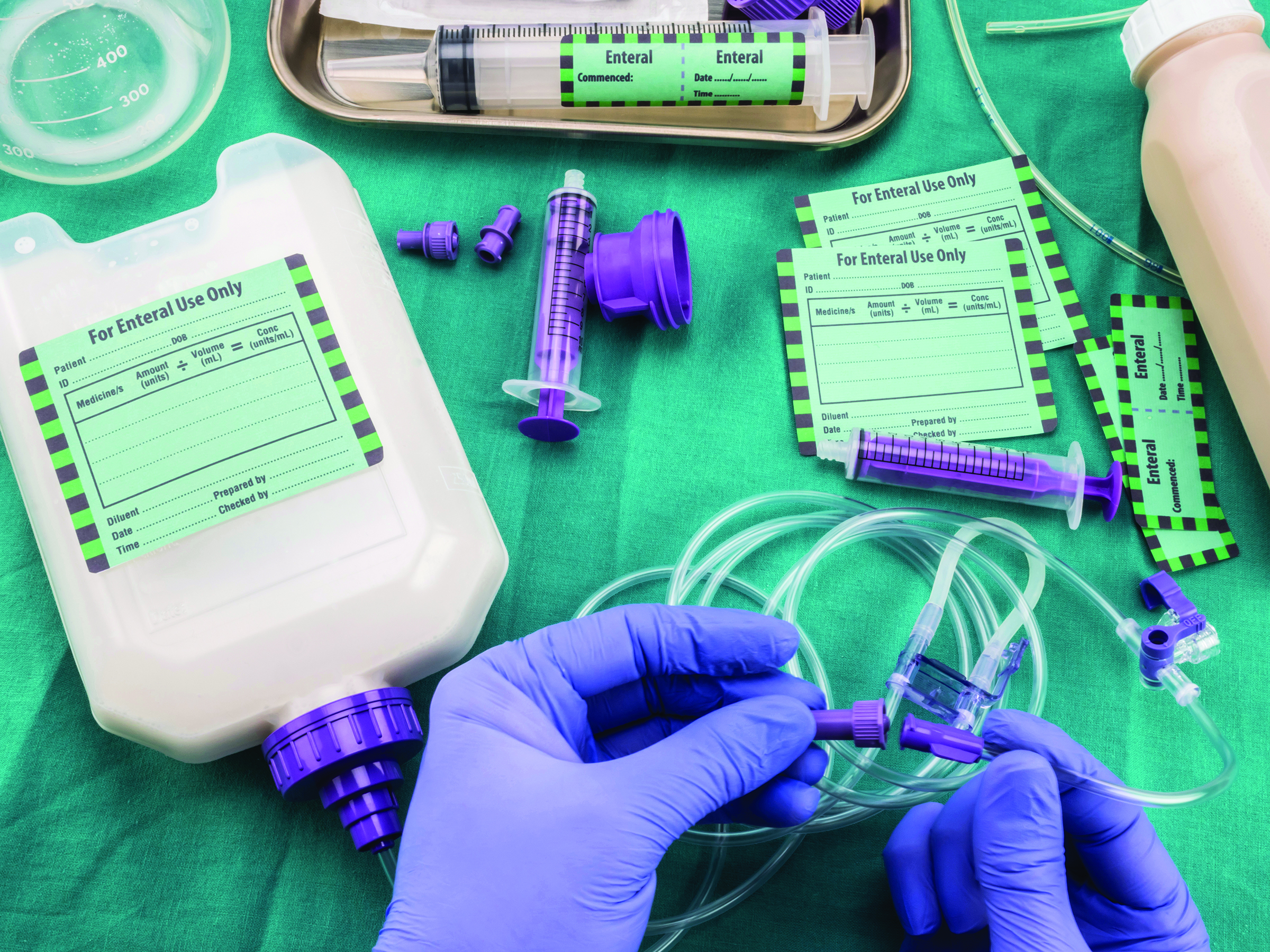

Despite a 2006 Joint Commission sentinel alert, enteral misconnections continue to be reported in the literature.
- Simmons and colleagues. In this review that spanned 1972 to 2010, the researchers found more than 116 reported cases of EN misconnection. Embolus or sepsis led to death in 18% of the patients. Similar to other voluntary adverse-event reporting systems, EN misconnections may be severely underreported.
- Guenter and colleagues. In 2008, these researchers classified EN misconnection errors by type. They reported 24 cases of EN misconnection with 33% leading to sentinel events (permanent injury, life-threatening situation, death). The misconnections were related to I.V. syringe pumps, ready-to-hang formula and I.V. tubing, enteral medications using I.V. syringes, and other solutions intended for the enteral route given via I.V.
- Pennsylvania Patient Safety Authority. In 2013, this organization reported 20 cases of inadvertent I.V. administration of oral medications between 2004 and 2012. All of the events reached the patient, and 20% (n = 4) resulted in patient harm, including one death. In many of these cases, oral drugs were administered using a parenteral syringe.
Because of adverse events, the International Standards Organization (ISO) 80369 standard for small-bore connectors was created to maximize patient safety by reducing the risk of medical tubing misconnections. The first clinical implementation was ISO 80369-3 for enteral feeding (ENFit), and the first connectors on the U.S. market were launched on EN administration sets in 2014. The primary challenge today is to help healthcare systems successfully convert to the new safer connectors. Successful transition requires participation by the entire healthcare team, including providers, nurses, pharmacists, dietitians, and supply chain specialists. In addition, patient education and standing equipment order revisions should be included in the transition plan.
The new connector design ensures incompatibility with other types of connectors, such as I.V. luer lock syringes, to prevent misconnections. However, because this reverse engineering makes it possible for EN formula or medications to accidentally spill into the male feeding tube connection, the ENFit connectors must be cleaned to remove debris. If the connector isn’t cleaned, you may not be able to disconnect the feeding tube from the enteral feeding set. A 2020 cleaning validation study by Lyman and colleagues demonstrated that cleaning with water and a brush (either a good-quality toothbrush or specially designed cleaning brush) successfully removed dried debris from the moat of an ENFit connector. Although this study didn’t look at frequency, clinical experts recommend cleaning at least daily and as needed when debris is visible. To prevent soiling the ENFit connector, draw up medications using a medication straw or adapter, which prevents the syringe tip from touching sticky liquid medications, and don’t prime the tubing to the very end of the feeding set.
Use aseptic technique when administering enteral formula
Reports in the literature by Beattie and Anderton, Bornemann and Zerr, and Fernandez-Crehuet Navajas and colleagues document patient harm caused from contamination of enteral formula at various points during preparation and administration. The most common factor associated with EN-related food-borne illness is touch contamination by nursing staff when manipulating the enteral feeding set during filling or when making connections. A 2011 study by Lyman looked at increasing hang time for prepared EN formulas (following manufacturer recommendations) from 8 hours (which is recommended for pediatric patients) to 12 hours. These investigators showed a low level of bacterial growth overall and no cases of patient illness. A 2017 study by Lyman and colleagues investigated three approaches to handling enteral feeding sets during bolus feedings: capping ready-to-hang formula every 3 hours, rinsing with sterile water, and placing the feeding set in a refrigerator between feedings. Although all of the techniques showed comparable and low bacterial growth, using ready-to-hang formula that was capped off between bolus feedings was the most cost-effective and time-efficient.
The Centers for Disease Control and Prevention reported that powdered enteral formulas that are reconstituted with water have been associated with sentinel events because the formulas can’t be sterilized. Therefore, any powdered, reconstituted EN formula has a limited 4-hour hang time.
ASPEN recommends practicing good hand hygiene and wearing clean gloves when accessing the feeding set, using purified water to flush it, handling the feeding set infrequently, and using ready-to-hang formula when possible.
Use established guidelines to properly administer medications
Most patients who require an NG tube for nutrition also will receive medications via the tube. These medications may adhere to the feeding tube, interact with the EN formula, or clog tubes. In addition, this administration route may decrease medication bioavailability. To prevent these complications, ASPEN suggests organizations establish policies for delivering medications via NG tube that include a list of medications that shouldn’t be crushed (such as sustained or extended-release) and are known to interact with enteral formulas, as well what to do if a tube is clogged. (See Tube occlusion risk factors.)
Tube occlusion risk factors

Risks for enteral nutrition tube occlusion when administering medications include
- delivering multiple medications at once without flushing between
- not flushing with water before and after administration
- using longer tubes
- using smaller diameter tubes.
A 2013 survey of 823 nurses by Guenter and Boullata assessed how frequently nurses followed national guidelines when administering medications via an enteral access device. Respondents indicated they frequently (11%) or occasionally (10%) add medications to enteral formula, but 78% reported never or rarely doing this; not adding medications is supported by ASPEN safe practice recommendations. In addition, ASPEN recommends flushing the access device with purified water between each medication rather than mixing medications, and diluting liquid medications to reduce viscosity and osmolality. Many liquid medications have an osmolality >1,000 mOsm/kg, which can lead to patient cramping and diarrhea.
Drug bioavailability is affected by properties specific to the medication and physiologic factors specific to the patient, such as delayed gastric emptying. Some medications may benefit from holding the EN for a short period before and after the drug administration, but this is not generally the case.
Newer enteral syringe and feeding set designs (which include use of the ENFit connector) embrace the concept of design incompatibility to prevent inadvertent delivery of enteral medications or formula via the wrong route. Consult with a pharmacist when you have questions about administering medication via an enteral access device.
Mitigate risks for pulmonary aspiration
Pulmonary aspiration can occur during an EN feeding when the formula in the stomach backs up into the lungs. This complication can cause pneumonia, sepsis, and even death. Proper patient positioning is critical to mitigating this risk. ASPEN recommends elevating the adult patient’s head of the bed at least 30 degrees while they’re receiving EN, unless an elevated position is medically contraindicated. In that case, consider the reverse Trendelenburg position.
Many nursing EN protocols include gastric residual volumes (GRVs) to reduce pulmonary aspiration risk, but ASPEN recommends not using GRV measurements as part of routine ICU monitoring of patients receiving EN. In settings where GRVs are used, avoid holding EN for GRVs less than 500 mL in the absence of other signs of intolerance. Parker and colleagues studied neonates who were randomly assigned GRV measurements before a feeding. They found that those in the group not having their GRV measured reached full enteral feeds faster, achieved better weight gains, and were discharged an average of 8 days earlier than those whose GRV was measured. This better outcome was largely attributed to not holding the feedings.
Safety is key
EN is a complex therapy associated with adverse events. Safety requires attention to detail and adherence to organization protocols and evidence-based guidelines and recommendations. Nurses can promote optimal clinical outcomes for patients receiving EN by following tube placement and verification best practices, using safe enteral devices, delivering enteral medications using appropriate measures, mitigating aspiration risk, and handling enteral formulas using aseptic technique. AN
Access references at myamericannurse.com/?p=77534.
Peggi Guenter is a nutrition support clinical nurse specialist and a special projects consultant to the American Society for Parenteral and Enteral Nutrition in Silver Spring, Maryland. Beth Lyman is a nutrition support nurse consultant in Kansas City, Missouri.
References
American Association of Critical Care Nurses. Prevention of aspiration in adults. Crit Care Nurse. 2016;36(1):e20-4. doi.org/10.4037/ccn2016831
Atalay YO, Aydin R, Ertugrul O, et al. Does bedside sonography effectively identify nasogastric tube placements in pediatric critical care patients? Nutr Clin Pract. 2016;31(6):805-9. doi:10.1177/0884533616639401
Beattie TK, Anderton A. Bacterial contamination of enteral feeding systems due to faulty handling procedures—A comparison of a new system with two established systems. J Hum Nutr Diet. 1998;11(4):313-21. doi:10.1046/j.1365-277X.1998.00112.x
Boullata JI. Enteral medication for the tube-fed patient: Making this route safe and effective. Nutr Clin Pract. 2020;36(1):111-32. doi:10.1002/ncp.10615
Boullata JI, Carrera AL, Harvey L, et al. ASPEN safe practices for enteral nutrition therapy. JPEN J Parenter Enteral Nutr. 2017;41(1):15-103. doi:10.1177/0148607116673053
Bourgault AM, Powers J, Aguirre L, Hines RB, Sebastian AT, Upvall MJ. National survey of feeding tube verification practices: An urgent call for auscultation deimplementation. Dimens Crit Care Nurs. 2020;39(6):329-38. doi:10.1097/DCC.0000000000000440
Fernandez-Crehuet Navajas M, Jurado Chacon D, Guillen Solvas JF, Galvez Vargas R. Bacterial contamination of enteral feeds as a possible risk of nosocomial infection. J Hosp Infect. 1992;21(2):111-20. doi:10.1016/0195-6701(92)90030-p
Guenter P, Hicks RW, Simmons D, et al. Enteral feeding misconnections: A consortium position statement. Jt Comm J Qual Patient Saf. 2008;34(5):285-92, 245. doi:10.1016/s1553-7250(08)34035-5
Guenter P, Lyman B. Safer enteral syringes. Patient Saf J. 2020;2(4):58-61. doi:10.33940/med/2020.12.4
International Organization for Standardization. ISO Small Bore Connectors Working Group. ANSI/AAMI/ISO 80369-1:2010. Small-bore connectors for liquids and gases in healthcare applications—Part 1: General requirements.Arlington, VA: Association for the Advancement of Medical Instrumentation; 2011.
International Organization for Standardizati.on ISO Small Bore Connectors Working Group. ANSI/AAMI/ISO 80369-3:2016. Small bore connectors for liquids and gases in healthcare applications—Part 3: Connectors for enteral nutrition. Arlington, VA: Association for the Advancement of Medical Instrumentation; 2016.
Irving SY, Lyman B, Northington L, Bartlett JA, Kemper C. Nasogastric tube placement and verification in children: Review of the current literature. Crit Care Nurse. 2014;34(3):67-78. doi:10.4037/ccn2014606
Irving SY, Rempel G, Lyman B, Sevilla WMA, Northington L, Guenter P. Pediatric nasogastric tube placement and verification: Best practice recommendations from the NOVEL Project. Nutr Clin Pract. 2018;33(6):921-7. doi:10.1002/ncp.10189
The Joint Commission: Sentinel Event Alert 53: Managing risk during transition to new ISO tubing connector standards. 2014. jointcommission.org/resources/patient-safety-topics/sentinel-event/sentinel-event-alert-newsletters/sentinel-event-alert-53-managing-risk-during-transition-to-new-iso-tubing-connector-standards
Kemper C, Haney B, Oschman A, et al. Acidity of enteral feeding tube aspirate in neonates: Do pH values meet the cutoff for pediatric gastric placement? Adv Neonatal Care. 2019;19(4):333-41. doi:10.1097/ANC.0000000000000591
Malone A, Carney LN, Carrera AL, Mays A. ASPEN Enteral Nutrition Handbook 2nd ed. Silver Spring, MD: American Society for Parenteral and Enteral Nutrition; 2019.
Metheny NA, Krieger MM, Healey F, Meert KL. A review of guidelines to distinguish between gastric and pulmonary placement of nasogastric tubes. Heart Lung. 2019;48(3):226-35. doi:10.1016/j.hrtlng.2019.01.003
National Health Service. Nasogastric tube misplacement: Continuing risk of death and severe harm. July 22, 2016. improvement.nhs.uk/documents/194/Patient_Safety_Alert_Stage_2_-_NG_tube_resource_set.pdf
Parker LA, Weaver M, Murgas Torrazza RJ, et al. Effect of gastric residual evaluation on enteral intake in extremely preterm infants: A randomized clinical trial. JAMA Pediatr. 2019;173(6):534-43. doi:10.1001/jamapediatrics.2019.0800
Read J, Guenter P. ASPEN Enteral Nutrition by the Numbers: EN Data Across the Healthcare Continuum. Silver Spring, MD: American Society for Parenteral and Enteral Nutrition; 2017.
Robinson D, Walker R, Adams SC, et al. American Society for Parenteral and Enteral Nutrition (ASPEN) Definition of Terms, Style, and Conventions Used in ASPEN Board of Directors–Approved Documents. May 2018 nutritioncare.org/uploadedFiles/Documents/Guidelines_and_Clinical_Resources/ASPEN%20Definition%20of%20Terms,%20Style,%20and%20Conventions%20Used%20in%20ASPEN%20Board%20of%20Directors%E2%80%93Approved%20Documents.pdf
Shah-Mohammadi A, Gaunt MJ. Oral medications inadvertently given via the intravenous route. Pennsylvania Patient Saf Advis. 2013;10(3):85-91.
Simmons D, Symes L, Guenter P, Graves K. Tubing misconnections: Normalization of deviance. Nutr Clin Pract. 2011;26(3):286-93. doi:10.1177/0884533611406134
Soghoian S, Hoffman RS, Nelson L. Unintentional I.V. injection of barium sulfate in a child. Am J Health Syst Pharm. 2010;67(9):734-6. doi:10.2146/ajhp080612
Sparks DA, Chase DM, Coughlin LM, Perry E. Pulmonary complications of 9931 narrow-bore nasoenteric tubes during blind placement: A critical review. JPEN J Parenter Enteral Nutr. 2011;35(5):625-9. doi:10.1177/0148607111413898