A new format and structure allows for timely updates and distribution.
- The 2017 updated Centers for Disease Control and Prevention Surgical Site Infection Guidelines was released in May.
- The new guideline format includes a new high-volume, high-burden procedure section.
- The new guideline format can be updated as soon as new evidence becomes available without rewriting the entire document.
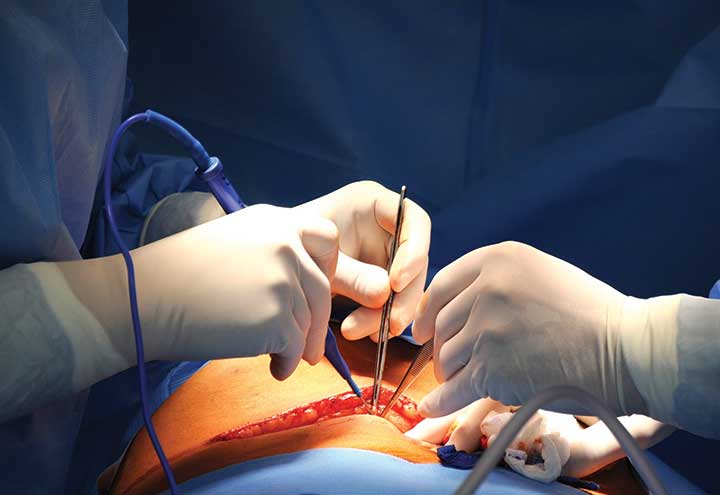
The prevention of surgical site infections (SSIs) continues to be a major goal for health care in both inpatient facilities and ambulatory surgical centers (ASCs). As nurses, surgeons, physician assistants, and healthcare technicians work together to care for their surgical patients, they rely on recommendations and guidelines to help them achieve positive outcomes with zero or low rates of SSIs.
A recent prevalence study found that SSIs are the most common healthcare-associated infections (HAIs), resulting in 31% of all HAIs in hospitalized patients. Those who develop an SSI are more likely to have an extended length of hospital stay and an increased risk of hospital readmission or death.
The Centers for Disease Control and Prevention (CDC) Guideline for the Prevention of Surgical Site Infection was last updated in 1999, when the terminology “surgical site infection” was first used. The new guideline was published in May 2017, and you can access it at www.jamanetwork.com.
New structure
The new guideline structure includes a core section with new high-volume, high-burden procedure sections. It provides recommendations applicable to a spectrum of procedures that are performed daily in hospital-based operating rooms and ASCs. The guideline also includes a section specific to prosthetic joint arthroplasties because of the number of these procedures performed in the United States (about 1.2 million per year) and their association with high costs and increasing SSIs.
The new evidence-based structure of the guideline allows timely, targeted updates to be implemented as new knowledge is acquired without rewriting the entire guideline.
Methodology
Beginning in 2010, the CDC and Healthcare Infection Control Practices Advisory Committee (HICPAC) implemented a new process for how the guideline is developed and issued. The core concept and framework uses an evidence-based methodology that includes:
- formulating key questions based on experts’ opinions
- performing targeted systematic reviews of the best current evidence
- using the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) method. (See Making the GRADE.)
Recommendations
Recommendations in this new guideline are categorized using a system that reflects the level of supporting evidence or regulation. (See Categorization recommendation scheme.) Following are selected recommendations from the 2017 guideline within both the core and prosthetic joint arthroplasty sections.
Parenteral antimicrobial prophylaxis
The 1999 Category IA recommendation for parenteral antimicrobial prophylaxis—Administer a prophylactic antimicrobial agent only when indicated, and select it based on its efficacy against the most common pathogens causing SSI for a specific operation and published recommendations—was changed to a Category IB recommendation—Administer preoperative antimicrobial agents only when indicated based on published clinical practice guidelines and timed such that a bactericidal concentration of the agent is established in the serum and tissues when the incision is made.
Making the Grade
The Grading of Recommendations Assessment, Development, and Evaluation (GRADE) method determines the strength of a recommendation using an assessment of the rigor of individual studies. The largest weight is placed on high-quality randomized prospective studies; however, observational studies also can be included. In cases of meta-analyses, the component studies are analyzed individually. Following the GRADE process, a list of key questions was developed from a review of the 1999 Centers for Disease Control and Prevention surgical site infection (SSI) guidelines. The key questions were reviewed by a panel of content experts and Healthcare Infection Control Practices Advisory Committee members.
Key questions were developed related to the core section covering parenteral antimicrobial prophylaxis, nonparenteral antimicrobial prophylaxis, glycemic control, normothermia, oxygenation, and antiseptic prophylaxis. For the prosthetic joint arthroplasty section, questions were developed about blood transfusion, systemic immunosuppressive therapy, immunosuppressive therapy—intraarticular corticosteroid injections, anticoagulation, orthopedic surgical space suit, antimicrobial prophylaxis duration with drain use, and biofilm. (See Core section questions and Prosthetic joint arthroplasty section questions.)
Literature review process
Targeted literature review searches were performed in MEDLINE, EMBASE, CINAHL, and the Cochrane Library databases from 1998, when the previous guideline searches ended, through June 2011 for the core section and December 2011 for the prosthetic joint arthroplasty section. Titles and abstracts were screened, and initial searches were designed to identify systematic reviews (SRs) and randomized controlled trials (RCTs).
SRs that included nonrandomized trials and observational studies were eligible for inclusion. Full-text articles were reviewed if they were relevant to one or more of the key questions, clinical practice guidelines, systematic reviews, or primary study designs meeting the inclusion criteria. When the key questions weren’t adequately addressed by the initial search, RCTs were included for the core and prosthetic joint arthroplasty sections and observational studies for the prosthetic joint arthroplasty section only.
After two independent reviewers screened the full-text articles and disagreements were resolved by discussion, a draft bibliography was shared with a panel of content experts and additional suggested references were reviewed using the same process.
Another 1999 Category IA recommendation—For high-risk cesarean section, administer the prophylactic antimicrobial agent immediately after the umbilical cord is clamped—was changed to a new Category IA recommendation—Administer the appropriate parenteral prophylactic antimicrobial agents before skin incision in all cesarean section procedures.
In addition, a new Category IA recommendation was included—In clean and clean-contaminated procedures, do not administer additional prophylactic antimicrobial agent doses after the surgical incision is closed in the operating room, even in the presence of a drain.
Nonparenteral antimicrobial prophylaxis
In the 1999 guideline, no recommendations existed for nonparenteral antimicrobial prophylaxis. The following recommendations were added in 2017:
- No recommendations/unresolved issue—intraoperative antimicrobial irrigation.
- No recommendations/unresolved issue—soaking prosthetic devices in antimicrobial solution before implantation for the prevention of SSI.
- Category IB—Do not apply antimicrobial agents (i.e., ointments, solutions, or powders) to the surgical incision for the prevention of SSI.
- Category II—Application of autologous platelet-rich plasma is not necessary for the prevention of SSI.
- Category II—Consider the use of triclosan-coated sutures for the prevention of SSI.
Glycemic controls
The 1999 Category IB recommendation for glycemic controls—Adequately control serum glucose levels—was changed to another Category IB recommendation—Adequately control serum blood glucose levels in all diabetic patients and particularly avoid hyperglycemia perioperatively. Also, an updated specific Category IA recommendation was added—Implement perioperative glycemic control and use blood glucose targets less than 200 mg/dL in patients without diabetes.
Normothermia
No normothermia recommendations existed in the 1999 guideline. The new guideline includes a Category IA recommendation—Maintain perioperative normothermia.
Oxygenation
Oxygenation wasn’t covered in the 1999 guideline. The new guideline includes this Category IA recommendation—For patients with normal pulmonary function undergoing general anesthesia with endotracheal intubation, administer increased fraction of inspired oxygen (FiO2) during surgery and after extubation in the immediate postoperative period.
Categorization recommendation scheme
Recommendations for the new guideline are based on the level of supporting evidence as outlined below. However, note that the 2017 guideline focuses on a few select areas; not all of the 1999 recommendations were reviewed. Many of the strong recommendations listed in the 1999 guideline are accepted practice for preventing surgical site infections (SSIs) and facilities should continue to follow them. Of the 30 recommendations in the core section of the 2017 guideline, six are Category IA, three are Category IB, none are Category IC, five are Category II, and 16 are classified as “no recommendations/unresolved issue.”
![]()
![]()
Category IA
A strong recommendation supported by high- to moderate-quality evidence, suggesting net clinical benefits or harms.
![]()
![]()
A strong recommendation supported by low-quality evidence, suggesting net clinical benefits or harms or an accepted practice (e.g., aseptic technique) supported by low- to very low-quality evidence.
![]()
![]()
Category IC
A strong recommendation required by state or federal regulation.
![]()
![]()
Category II
A weak recommendation supported by any quality evidence suggesting a trade-off between clinical benefits and harms.
![]()
![]()
No recommendations/unresolved issue
An issue with low- to very low-quality evidence and uncertain trade-offs between the benefits and harms or no published evidence on outcomes deemed critical to weighing the risks and benefits of a given intervention.
Source: jamanetwork.com
Antiseptic prophylaxis
Two Category IB recommendations were updated for antiseptic prophylaxis. Require patients to shower or bathe with an antiseptic agent on at least the night before the operative day was updated to a new Category IB recommendation—Advise patients to shower or bathe (full body) with soap (antimicrobial or nonantimicrobial) or an antiseptic agent on at least the night before the operative day. The 1999 recommendation—Use an appropriate antiseptic agent for skin preparation—was updated to a Category IA recommendation—Perform intraoperative skin preparation with an alcohol-based antiseptic agent unless contraindicated.
Two new Category II recommendations were added:
- The use of plastic adhesive drapes with or without antimicrobial properties is not necessary for the prevention of SSI.
- Consider intraoperative irrigation of deep or subcutaneous tissues with aqueous iodophor solution for the prevention of SSI. Intraperitoneal lavage with aqueous iodophor solution in contaminated or dirty abdominal procedures is not necessary.
Prosthetic joint arthroplasty
The new prosthetic joint arthroplasty section provides recommendations specific to primary and revision joint arthroplasty procedures, total knee arthroplasty, total hip arthroplasty, hip hemiarthroplasty, and primary shoulder, elbow, and ankle arthroplasty. The recommendations are presented under the following seven categories:
- Blood transfusion
- Systemic immunosuppressive therapy
- Intraarticular corticosteroid injections
- Anticoagulation
- Orthopedic surgical space suit
- Postoperative antimicrobial prophylaxis duration with drain use
- Biofilm
Eleven of the recommendations in this section were designated as “no recommendation/unresolved issue” and are associated with blood transfusion, systemic immunosuppressive therapy, intraarticular corticosteroid injections, anticoagulation, orthopedic surgical space suit, and biofilm.
A Category IA recommendation was made for systemic immunosuppressive therapy—For prosthetic joint arthroplasty patients receiving systemic corticosteroid or other immunosuppressive therapy, in clean and clean-contaminated procedures, do not administer additional antimicrobial prophylaxis doses after the surgical incision is closed in the operating room, even in the presence of a drain. Another Category IA recommendation was made for postoperative antimicrobial prophylaxis duration with drain use—In prosthetic joint arthroplasty in clean and clean-contaminated procedures, do not administer additional antimicrobial prophylaxis doses after the surgical incision is closed in the operating room, even in the presence of a drain.
A Category IB recommendation was made for blood transfusion—Do not withhold transfusion of necessary blood products from surgical patients as a means to prevent SSI.
Opportunities
SSIs continue to be a major concern in both inpatient and ASC settings. Using the best available evidence as the framework for the new guideline is a step in the right direction and a strength of this new process for issuing recommendations from HICPAC. The ability to quickly review and update the guideline as new information becomes available, while leaving the core intact, means new evidence can be swiftly disseminated and translated into practice.
However, the new guideline demonstrates several gaps in knowledge as is indicated by the number of “no recommendations/unresolved issue” designations. This represents an opportunity for nurses to develop and participate in well-designed randomized clinical trials to generate this evidence.
George Allen is director of infection prevention at NewYork-Presbyterian Brooklyn Methodist Hospital in Brooklyn, New York.
Core section questions
Parenteral antimicrobial prophylaxis (AMP)
• What are the most effective strategies for administering parenteral AMP to reduce the risk of SSI?
Nonparenteral AMP
• What are the most effective strategies for administering nonparenteral AMP at the surgical incision to reduce SSI?
Glycemic control
• How do perioperative blood glucose and hemoglobin A1C levels impact the risk of SSI, and what are the optimal perioperative target levels in diabetic and nondiabetic patients?
Normothermia
• How safe and effective is the maintenance of perioperative normothermia in reducing the risk of SSI?
• What are the most effective strategies for achieving and maintaining perioperative normothermia?
Oxygenation
• In patients with normal pulmonary function, how safe and effective is the perioperative use of increased fraction of inspired oxygen (FiO2) in reducing the risk of SSI?
• What is the optimal target FiO2 to reduce the risk of SSI; how and when should it be administered?
Antiseptic prophylaxis
• What are the most effective strategies for preparing the patient’s skin prior to surgery to reduce the risk of SSI?
• How safe and effective is antiseptic irrigation prior to closing the surgical incision?
• How safe and effective is repeat application of an antiseptic skin preparation agent to the surgical site immediately prior to closing the surgical incision?
Source: jamanetwork.com
Prosthetic joint arthroplasty section questions
Blood transfusion
• How do perioperative blood transfusions impact the risk of SSI in prosthetic joint arthroplasty patients?
Systemic immunosuppressive therapy
• How does systemic corticosteroid or other immunosuppressive therapy impact the risk of SSI in prosthetic joint arthroplasty patients?
• What are the most effective perioperative strategies for managing systemic corticosteroid or other immunosuppressive therapy to reduce the risk of SSI in prosthetic joint arthroplasty patients?
• What is the optimal duration of postoperative antimicrobial prophylaxis (AMP) to reduce the risk of SSI in prosthetic joint arthroplasty patients who are on systemic corticosteroid or other immunosuppressive therapy?
Intraarticular corticosteroid injections
• How do preoperative intraarticular corticosteroid injections impact the risk of SSI in prosthetic joint arthroplasty patients?
• What are the most effective strategies for managing the preoperative use of intraarticular corticosteroid injections to reduce the risk of SSI in prosthetic joint arthroplasty patients?
Anticoagulation
• What are the most effective strategies for managing perioperative venous thromboembolism prophylaxis to reduce the risk of SSI?
Orthopedic surgical space suit
• How safe and effective are orthopedic surgical space suits in reducing the risk of SSI in prosthetic joint arthroplasty patients, and which healthcare personnel should wear them?
Postoperative AMP duration with drain use
• What is the optimal duration of postoperative AMP to reduce the risk of SSI in prosthetic joint arthroplasty in the presence of a drain?
Biofilm
• What are the most effective strategies to reduce the risk of biofilm formation and SSI in prosthetic joint arthroplasty patients?
Source: jamanetwork.com
References
Anderson DJ, Podgorny K, Berrios-Torres SI, et al. Strategies to prevent surgical site infections in acute care hospitals: 2014 update. Infect Control Hosp Epidemiol. 2014;35(suppl 2):S66-88.
Berrios-Torres SI, Umscheid CA, Bratzler DW, et al. Centers for Disease Control and Prevention Guideline for the Prevention of Surgical Site Infection, 2017. JAMA Surg. 2017. [Epub ahead of print].
Centers for Disease Control and Prevention. Number and standard error of discharges from short-stay hospitals with and without procedures and percentage with procedures and standard error by selected characteristics: United States, 2010. Data from the CDC/NCHS National Hospital Discharge Survey, 2010. read more at cdc.gov
Fry DE. Fifty ways to cause surgical site infections. Surgl Infect. 2011;12(6):497-500.
Garner JS. CDC guideline for prevention of surgical wound infections, 1985. Supersedes guideline for prevention of surgical wound infections published in 1982. (Originally published in November 1985.) Revised. Infect Control. 1986;7(3):193-200.
GRADE Working Group. www.gradeworkinggroup.org
Hall MJ, DeFrances CJ, Williams SN, Golosinskiy A, Schwartzman A. National Hospital Discharge Survey: 2007 summary. Natl Health Stat Report. 2010;26(29):1-20, 24.
Kurtz S, Ong K, Lau E, Mowat F, Halpern M. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am. 2007;
89(4):780-5.
Kurtz S, Lau E, Watson H, Schmier JK, Parvizi J. Economic burden of periprosthetic joint infection in the United States. J Arthroplasty. 2012;27(suppl 8):61-5.
Magill SS, Edwards JR, Bamberg W, et al. Multistate point-prevalence survey of health care-associated infections. N Engl J Med. 2014;370(13):1198-208.
Magill SS, Hellinger W, Cohen J, et al. Prevalence of healthcare-associated infections in acute care hospitals in Jacksonville, Florida. Infect Control Hosp Epidemiol. 2012;33(3):283-91.
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR. Guideline for Prevention of Surgical Site Infection, 1999. Centers for Disease Control and Prevention (CDC) Hospital Infection Control Practices Advisory Committee. Am J Infect Control. 1999;27(2):97-132.
Shallwani H, Shakir HJ, Aldridge AM, Donovan MT, Levy EI, Gibbons KJ. Mandatory change from surgical skull caps to bouffant caps among operating room personnel does not reduce surgical site infections in class I surgical cases: A single-center experience with more than 15,000 patients. Neurosurgery. 2017. go to academic.oup.com
Simmons BP. Guideline for prevention of surgical wound infections. Am J Infect Control. 1983;11(4):133-43.
Umscheid CA, Agarwal RK, Brennan PJ; Healthcare Infection Control Practices Advisory Committee. Updating the guideline development methodology of the Healthcare Infection Control Practices Advisory Committee (HICPAC). Am J Infect Control. 2010;38(4):264-73.
U.S. Department of Health and Human Services. Overview: Health care–associated infections. read more at health.gov