With certification, nurses can help address access.
- Individuals with vision impairment, mobility issues, arthritis, and cognitive changes may have difficulty performing routine foot care.
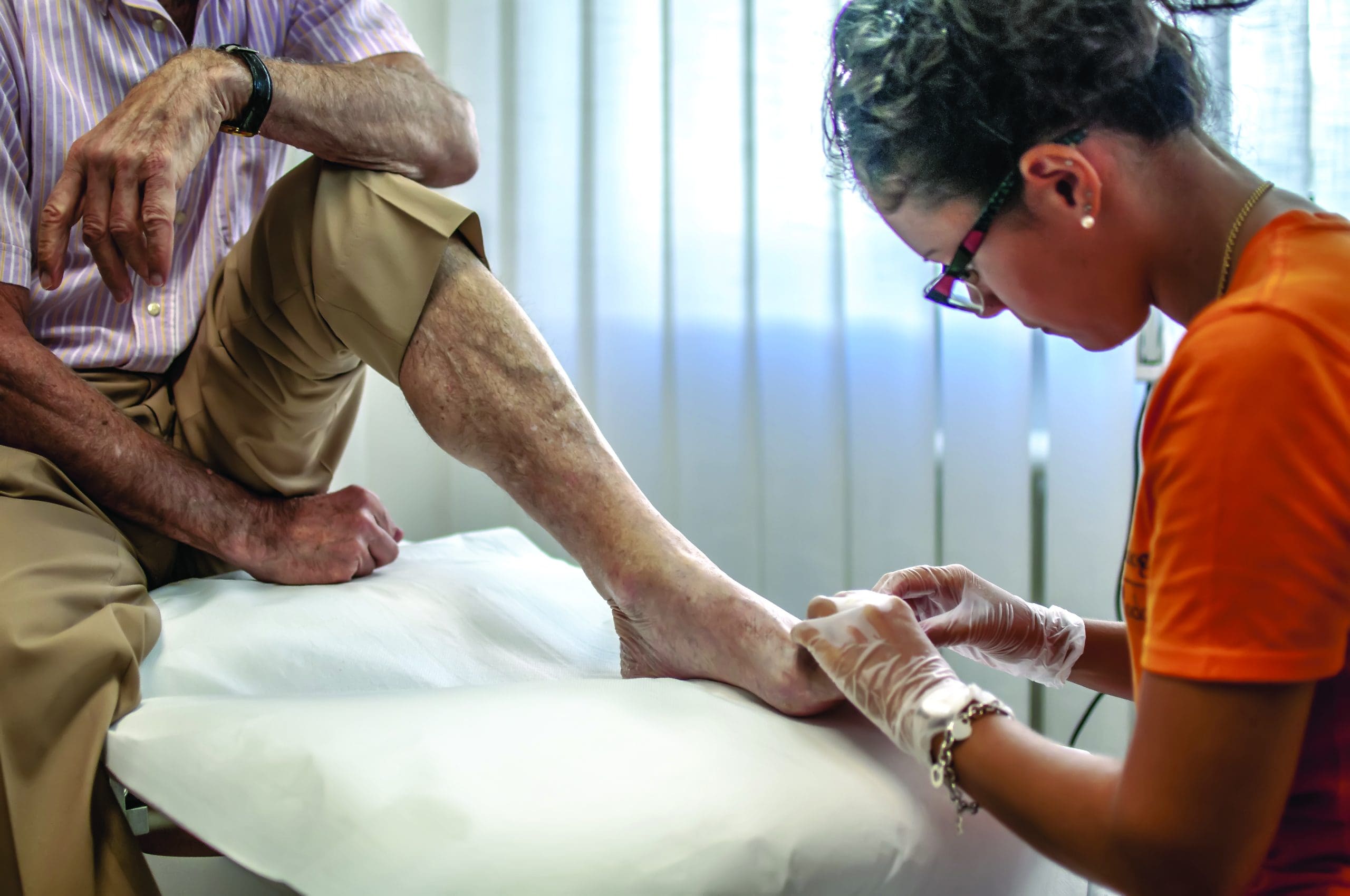
- Certified foot care nurses and foot care specialists play a critical role in providing assessments, patient education, and care.
- These specialists collaborate with other professionals (podiatrists, orthopedists, dermatologists, diabetes educators, and wound care experts) to ensure appropriate care.
Out of fear of contracting COVID-19 and overall travel challenges, many individuals missed healthcare provider appointments and neglected some routine care. This led to complications that might otherwise have been avoided. For example, those with vision impairment, mobility issues, arthritis, and cognitive changes may face difficulty performing foot and nail care. In addition, those with diabetes and other neuromuscular and sensory conditions face increased risk for feet complications. If they have no protective sensation in their feet, they may miss the warning signs of an injury and infection.
Before the pandemic, few knew about the role of the certified foot care nurse (CFCN®) or certified foot care specialist (CFCS®). However, these professionals play a critical role in providing assessments and patient education to prevent complications, especially for those with diabetes. They help identify issues and contribute to early intervention, including providing wound care, addressing vascular disease, and making referrals in response to social needs.
CFCN and CFCS role
CFCNs and CFCSs receive training to address patients’ lower extremities in various settings, including clinics, hospitals, long-term care and assisted living facilities, and in the community. They perform focused lower extremity assessments (paying attention to the moisture, temperature, color, and pulses of the feet), take comprehensive health histories, develop initial patient-centered plans of care, perform ongoing plan evaluations and modifications, and deliver preventive care. During assessments, they speak with clients to evaluate their socioemotional needs.
To collaborate effectively and make appropriate referrals, CFCNs and CFCSs must have knowledge of the roles and responsibilities of specialized healthcare providers (vascular specialists, podiatrists, orthopedists, dermatologists, pedorthists, orthotists, pain management specialists, diabetes educators, wound specialists, and dietitians). In addition, they teach patients about feet and nail care, proper use of footwear, and how to use assistive devices.
Working in collaboration with patients, CFCNs and CFCSs develop plans of care for home management. When patients can promptly identify and report issues, foot care professionals can make appropriate provider referrals, which lead to early diagnosis and intervention to reduce injury, amputation, and increased healthcare costs. (See Foot care certifications.)
Foot care certifications
Nurses and other healthcare professionals can take one of two paths to foot care certification: certified foot care nurse (CFCN®) or certified nurse care specialist (CFCS®).
CFCN
In 2005, the Wound, Ostomy and Continence Nursing Certification Board (WOCNCB®) created the CFCN to prepare nurses to assess, intervene, and teach patients how to manage common foot care issues. WOCNB certification, which requires a bachelor’s degree from any field, recognizes the nurses’ competency, knowledge, skills, and ability to provide high standards in foot care nursing while improving care quality and patient outcomes.
To learn more about becoming a CFCN, visit wocncb.org/certification/foot-care-certification.
CFCS
Dr. Julia Overstreet, DPM, founded the American Foot Care Nurses Association (AFCNA) to create a community of specialists to provide routine foot care and fill the gap in podiatric care (afcna.org). AFCNA offers the CFCS certification. Unlike the CFCN certification, which requires a bachelor’s degree, any healthcare professional—including RNs with less than 4 years of education, licensed practical nurses, and physical therapists—can become a CFCS. The AFCNA website states, “Podiatrists and other physicians are traditionally the first line providers of this care, but changes in the healthcare industry have led to access and reimbursement issues for many who need care.” This can necessitate that services such as routine foot care be provided by other qualified providers, including nurses.
To learn more about becoming a CFCS, visit afcna.org.
Both the WOCNCB and AFCNA provide the specific requirements for certification, which include classroom instruction and clinical hours that range from 24 to 40 hours. In addition, AFCNA has established a CFCS code of ethics.
Complication prevention
Several complications can result from lack of routine foot care, which are especially common among individuals with diabetes, who face increased risk of developing dry skin, odor, and ulcerations as a result of hyperglycemia, poor circulation, or ill-fitting shoes. Diabetes also can lead to arterial and vascular disease, structural foot changes (such as Charcot foot), and skin conditions (such as fungal and bacterial infections). Impaired skin increases the risk for infection and cellulitis, a common bacterial skin infection that causes redness, swelling, and pain. The risk of developing cellulitis is 40% higher with HgA1C levels above 7.5%.
CFCNs and CFCSs teach patients how to perform routine skin care, including proper moisturizing and daily skin checks. When caring for elderly clients, CFCNs and CFCSs should note and document any skin changes or conditions. For example, idiopathic guttate hypomelanosis, keratoses, mole changes, and skin color variations may indicate cancer. To avoid delayed referrals, CFCNs and CFCSs recognize that conditions appear different on individuals with darker skin tones.
During nail care, CFCNs and CFCSs can identify disease processes such as melanoma, poor circulation, vitamin deficiency, and ulceration. Elongated nails pose a fall risk that can result in injury, and discomfort or pain may deter patients from participating in activities. Nurses address these issues by providing education about foot hygiene and how to properly wear shoes. (See Foot care in action.)


Foot care in action
Certified foot care nurses (CFCNs) and certified foot care specialists (CFCSs) perform assessments, take health histories, perform routine foot care, and make referrals.
Case scenario 1
Robert Anderson*, a 93-year-old white man, receives home care for small-scabbed areas on his shin. He tells the CFCN, Robin, that the injuries occurred when he bumped into his walker. At a 6-week follow-up visit, Robin notes that the scabbed areas are still present. She explains to Mr. Anderson that the injuries should have healed by now and refers him to dermatology. The dermatologist makes a diagnosis of basal cell carcinoma and treats it with excision. Robin’s prompt assessment and early intervention recommendation helped Mr. Anderson resume his previous quality of life.
Case scenario 2
Susan Walker, who has dementia and receives home care, has thick pincered and fungal toenails. Ms. Walker’s daughter reports that her mother has a history of fungal nails and previously had received podiatry care. During his examination, David, the CFCS, notes that the skin of Ms. Walker’s left great toe appears red and raw; the patient reports pain when it’s touched. When David debrides the nail plate, he reveals a pin-sized wound in the nail bed. David talks with the family about Ms. Walker’s shoes, noting that she might need a wider box to accommodate her toes and reduce pressure on the nails. He refers Ms. Walker to her primary care provider for further evaluation; the provider prescribes antibiotics.
*Names are fictitious
Foot care reimbursement
The lack of reimbursement for routine foot care provided by an RN, as well as lack of recognition of the scope of practice of a nurse with additional education and certification, creates barriers for those who need routine foot care. According to the Centers for Medicare & Medicaid Services, some services usually considered routine may be covered if they’re an integral part of otherwise covered services, such as diagnosis and treatment of ulcers, wounds, or infection. Assessment, diagnosis, and treatment of systemic conditions—including metabolic, neurologic, or peripheral vascular disease and mycotic nails—fall into this category. When these services aren’t covered, patients must pay out-of-pocket.
Recognized need
One in four individuals with diabetes develops a foot ulcer, and up to a quarter of which don’t heal. As the economic burden of diabetes-
related foot disease increases, nurses and other healthcare professionals recognize CFCNs and CFCSs as integral to the interdisciplinary team. They provide assessments, interventions via patient education, and referrals to the medical community to ensure early diagnosis and treatment of medical conditions. The results include enhanced quality of life, increased independence, and cost savings. AN
Yvette Conyers is a clinical associate professor at the George Washington University School of Nursing in Washington, DC. Petula Griffith is the owner of The Foot Care RN and chief executive officer of Petula Griffith Inc., in White Plains, New York.
Key words:
foot care, diabetes, COVID-19, certified foot care nurse, certified foot care specialist, healthcare access
American Nurse Journal. 2022; 17(12). Doi: 10.51256/ANJ122221
References
Beuscher TL, Moe HL, Stolder ME, Peloquin L, Nesbitt B. Expanding a foot care education program for nurses: A quality improvement survey. J Wound Ostomy Continence Nurs. 2019;46(5):441-5. doi:10.1097/WON.0000000000000579
Boulton AJM, Armstrong DG, Kirsner RS, et al. Diagnosis and Management of Diabetic Foot Complications. Arlington, VA: American Diabetes Association; 2018.
Centers for Medicare & Medicaid Services. Medicare coverage database: Routine foot care. December 5, 2019. cms.gov/medicare-coverage-database/view/lcd.aspx?LCDId=37643
Fawaz M, Anshasi H, Samaha A. Nurses at the front line of COVID-19: Roles, responsibilities, risks, and rights. Am J Trop Med Hyg. 2020;103(4):1341-2. doi:10.4269/ajtmh.20-0650
Hart T, Milner R, Cifu A. Management of a diabetic foot. JAMA. 2017;318(14):1387-8. doi:10.1001/jama.2017.11700
Wound Ostomy and Continence Nursing. Foot care certification. wocncb.org/certification/foot-care-certification
Zacay G, Sikron FH, Heymann AS. Glycemic control and risk of cellulitis. Diabetes Care. 2021;44(2):367-72. doi:10.2337/dc19-1393