The single biggest change to nursing in a generation in the United Kingdom (UK) is the transition to a paperless National Health Service (NHS, the publicly funded healthcare system) by 2018. It offers an opportunity to radically improve the quality of care by using better information to make faster, safer clinical decisions. The challenge for nurses is to seize control of that change, using our expertise to shape the technology rather than letting the technology shape us.
The lesson from early NHS adopters of information technology (IT) is clear: Success hinges not on IT wizardry but on nurses’ willingness to lead the change they want to see. We have the chance to redefine what excellent care looks like. The test now is to make that a reality.
When challenging timelines are set, it’s all too easy to focus on the “when.” But for transformation to succeed, nurses first need to understand the “why.” That means putting information at the heart of clinical strategy. Too often, we make crucial decisions based on the pieces of information we have, not the complete picture we’d like to have. If we get it right, it’s in spite of the information, not because of it. That’s frustrating for us and dangerous for patients.
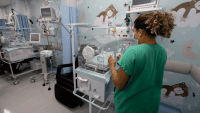
As early adopters of the information challenge, we’ve seen how things can be different. Where nurses have access to information at the bedside, they can make quicker decisions. Where they’re free from administrative burdens, they have more time for patient care. Where automated alerts prevent medication errors, patients are safer. Information underpins improved care.
A chance for nurses to influence the IT agenda
The drive to a paperless NHS in 2018 is an opportunity to influence the information agenda. It’s a chance to shape the underpinning technology, ensuring it provides the data we need to make the right decisions. The danger is that nurses may fail to grasp the scale of this opportunity. We all need to understand that this isn’t a back-office IT project with a start point and end point. It’s a clinical transformation project that will continually improve the quality of care. Technology is the means to enhance outcomes, not the end in itself.
The NHS isn’t facing this challenge from a standing start. Some trusts already are using improved information to improve patient outcomes. Experience from early adopters offers valuable lessons for those who will follow in their footsteps. (See First things first: Assess existing pro-cesses by clicking the PDf icon above.)
Visible clinical leadership
Clinical improvement requires visible clinical leadership. Clinicians must define medical objectives and communicate how these will be achieved. When the authors helped design the technology systems for our own hospitals, we provided a more holistic view of patient care, advising on the patient’s needs at each stage. That helped ensure the information flow aligned directly with the patient pathway. When our IT colleagues became distracted by project details, we brought the focus back to patients. What matters isn’t what’s technologically possible but what’s clinically essential.
The trend toward appointing chief medical or nursing information officers in the United States and chief clinical information officers in the UK is essential to strengthen clinical oversight of information projects. These officers help bridge the gap in understanding between the IT and clinical communities. The result is care transformed by data, which drives more proactive interventions and allows outcomes measurement. As we prepare for 2018, we need to see more nurses embrace the challenge of informatics leadership.
Clinical leadership fosters clinical credibility. Disrupting the status quo by asking nurses to change how they work is never easy. But it’s far more likely to succeed if led by someone the nursing community respects. To ensure that nursing is key in the transition requires someone who can speak the nurse’s language and engage nurses. Ideally, this person should be a nurse. Communication and leadership skills matter more than titles.
Helping nurses embrace change
Nurses need to be persuaded, not compelled. We need to acknowledge that change can be unsettling. That’s why engagement should be at the heart of the process, not an afterthought. Talk of code upgrades will cut
little ice on a busy unit. Instead, nurses need to understand how better information will streamline their work, promote more informed decisions, and release more time for them to provide care. Nurses will be more tolerant of bumps in the journey if they know why they’re on the journey and how it will benefit patients.
Visibility is crucial to persuading skeptics to embrace change. Even the best-planned change processes will encounter critics. It may be tempting to defer engaging difficult groups and instead focus initial energies on more persuadable colleagues. But difficult though it is, early engagement is far more effective. Where hostility festers, it grows stronger and risks spreading. Clinical leaders should take the time to understand nurses’ concerns, scheduling training early to help allay fears about what’s coming.
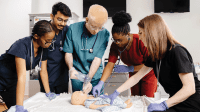
Establishing simulation units to demonstrate new technology is particularly effective in countering latent resistance to technology. Nurses who can visualize a change are less afraid of it. Clinical leaders should be a visible presence on units, answering questions and ensuring staff believe their opinions are heard.
Using information to transform the quality of care is a major change for the NHS, but it’s clinically essential. Putting information at the heart of care may not be easy, but if we fail to embrace the challenge, we’ll fail our patients—and that’s not an option. Instead, we have to seize the information agenda and offer the strong clinical leadership it needs. It will succeed only if nurses are clear about what they need and step up to the job of making it happen. That means assuming responsibility for informatics leadership rather than hoping someone else does. We know our jobs better than anyone, and we understand what our patients need. It falls to us to set new standards in the quality of care.
Gerry Bolger is nurse lead for Clinical Systems and Information and Communication Technology at Imperial HealthCare NHS Trust in London, England. Fergus Keegan is deputy director of nursing at the Kingston Hospital (UK) NHS Foundation Trust. Cathy Patterson is a nurse executive at Cerner Limited (UK).