Feeding tubes are used for various indications in patients with either acute or long-term needs. Critical care, acute care, long-term, and home care nurses provide nutrition and hydration via feeding tubes to patients with inadequate oral intake.
Enteral nutrition, which delivers nutrients directly to the GI tract, is linked to fewer complications than I.V. parenteral nutrition and is preferred in patients with functioning GI tracts. However, tube feedings can lead to mechanical, infectious, and metabolic complications. The most common mechanical complications—those affecting nutrient delivery to patients—are tube dislodgment with complete tube loss, tube displacement, and clogging. Less common mechanical complications include knotting and breakage of the enteral tube and buried bumper syndrome (BBS), associated with percutaneous endoscopic gastrostomy (PEG) tubes.
Understanding the various types of feeding tubes helps you manage them. (See Types of feeding tubes.) This article describes mechanical complications and offers tips for recognizing, preventing, and troubleshooting them in adult patients.
Enteral feeding: Indications, complications, and nursing care
Tube dislodgment
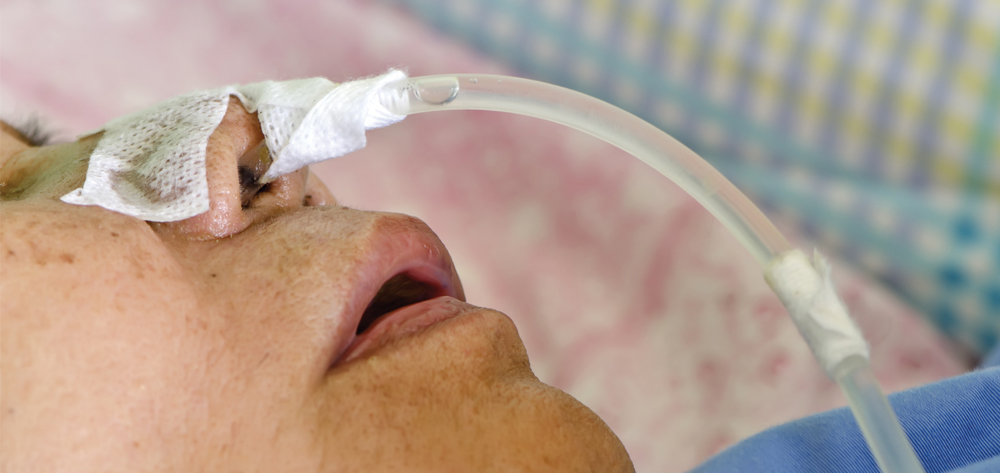
Any feeding tube can become dislodged. Patient factors linked to dislodgment include confusion or delirium, which can lead the patient to dislodge or remove the tube manually. Nasal or orally placed tubes are especially prone to patient removal because they may cause nares discomfort and a tube sensation in the pharynx.
Tube dislodgment also may occur when the patient is repositioned in bed, walking, mobilized to a chair, or transported for procedures. To prevent dislodgment from patient activity, secure a nasal or oral tube to the patient’s nares, cheek, or both near the tube’s exit point, without causing pressure on the nares or nasal septum. Secure a tube exiting the abdominal wall to the abdomen near the exit site without putting undue tension on it.
Also, you can secure the tube’s distal portion to the patient’s gown or other garment with sufficient slack on the tube to stop it from dislodging during movement. Apply a piece of tape to the tube and push a safety pin through the tape and clothing. Hold the tube and administration tubing with sufficient slack to prevent accidental dislodgment during movement. Alternatively, a bridle nasal feeding-tube retaining system may be useful for some patients. Bridles have been studied mainly in critical care and burn patients. When a nasal or oral feeding tube dislodges, tube replacement should be confirmed with radiography.
With long-term feeding, both gastrostomy and jejunostomy tubes may become dislodged; the latter dislodge at a higher rate. PEG tubes may dislodge inadvertently because they’re designed to be removed with external traction; most often, dislodgment is linked to internal balloon deflation or inadvertent removal of the external bumper or disc.
When complete tube dislodgment occurs, contact the physician or nurse practitioner (NP) immediately. Replacement through a mature GI tract (usually after 7 to 10 days of tube placement) may be done safely. But if doubt exists, endoscopic replacement may be required. If the GI tract isn’t mature, the stomach may fall away from the abdominal wall and lead to free perforation of the stomach with leakage of gastric contents into the abdominal cavity. For patients in home care or long-term care settings, the tube may need to be replaced in the emergency department. Tubes may be managed in an outpatient clinic setting as well, depending on GI tract maturity.
To prevent complications of inadvertent tube removal, the stomach wall commonly is placed in contact with the abdominal wall during insertion. Low-profile button-type devices can be used as the replacement tube to prevent patients from inadvertently pulling on the tube’s external portion, which can lead to a second accidental removal.
Tube displacement or migration
Patients may accidentally pull at an NG or nasointestinal tube, causing displacement rather than complete tube removal. As with dislodgment, patient activity and transport can cause tube displacement. So can coughing and gagging.
To detect displacement, monitor tube distance outside the patient. Many tubes have centimeter (cm) markings you can monitor and document. If no visible marking exists, use an indelible marker to mark the exit site at the nares or mouth. Also, you can use a tape measure to measure the length of the feeding tube extending from the nares or mouth. However, be aware that if the patient coughs or gags, the tube may become displaced and migrate into the esophagus, oropharynx, or larynx with no change in the external exit site. Suspect tube migration if the patient coughs or gags or if you obtain enteral formula during oral or tracheal suctioning.
Also, assess for tube coiling in the oral cavity. Radiography can detect coiling in the esophagus or upper airway. A coiled tube may need to be removed and replaced.
An NG tube may migrate into the intestine with food propulsion during digestion. Decreased residual volume and higher residual pH may indicate migration beyond the pylorus. If this occurs, notify the physician or NP, who will order an X-ray to confirm tube placement.
For a distally displaced tube, feeding volume and method may need to be altered. For example, if the patient was receiving bolus tube feedings into the stomach, continuous feeds are advised if the tube will remain in a post-pylorus position. Another option is to pull the tube back to a gastric location.
A gastrostomy tube may become displaced, sliding distally into the GI tract, where it obstructs the gastric outlet. Suspect gastric outlet obstruction if the patient complains of abdominal cramps and nausea and experiences vomiting. To prevent this complication, maintain the external bumper 0.5 to 2 cm from the skin to prevent the tube from being pulled into the stomach. Monitoring and documenting the external bolster setting can help prevent and detect potential gastric outlet obstruction from tube displacement. Dislodgment into the gastric outlet calls for a contrast study to determine tube location.
In some cases, gastrostomy tubes displace outward without being dislodged completely. This most often happens when the GI tract isn’t well formed, although it can occur at any time. Also, know that gastrostomy button tubes are prone to displacement, especially with the first standard gastrostomy tube replacement to a low-profile tube. If you suspect internal tube displacement, stop tube feedings and contact the physician or NP.
A patient with a displaced tube typically complains of abdominal pain that worsens during feeding as gastric contents leak into the peritoneal cavity; also, you may observe external leakage of gastric contents. In this case, peritonitis may occur. If the patient can’t communicate pain verbally, use a noncommunicative pain assessment scale. If you suspect displacement, discontinue tube feedings and notify the physician or NP immediately. A water-soluble contrast study or endoscopic procedure may be required to assess tube location.
Tube clogging
Clogging (occlusion) of a feeding tube interrupts nutrient and medication administration. Clogging incidence ranges from 10% to 35%. The most common cause is medication delivery.
Clogging can occur with any size tube but is more likely with smaller-bore tubes. Regular flushing with water can help prevent clogging not caused by medications. Flush the tube every 4 hours with 30 mL of water during continuous feeding, or before and after each intermittent bolus feeding. If you measure residual volume, follow with a flush of 30 mL.
Prevention
Preventing clogs caused by medications necessitates multiple interventions. If the patient can swallow medications and has a working GI tract, the oral feeding route is preferred. Some patients with enteral feeding tubes can swallow medications in liquid form; others can swallow medications with something other than water, such as thickened liquids. If you’re unsure of your patient’s aspiration risk, consult a speech therapist to determine the safest method of oral medication administration.
For patients unable to swallow medications, feeding tubes are preferred over parenteral administration, especially for long-term use. Collaborate with the physician or NP prescribing the medication, as well as the pharmacist, to ensure proper medication and dosage. Be aware that certain medication forms shouldn’t be given through a feeding tube.
Liquid medications are a good alternative, when available. However, they’re indicated for oral intake and aren’t reviewed by the Food and Drug Administration specifically for feeding-tube administration. Some liquid medications contribute to tube clogging when exposed to enteral nutrition formula. Liquid syrups, for instance, cause clumping and lead to tube clogging. Also, lansoprazole oral suspension granules, sucralfate suspension, and mineral oil are known to clog feeding tubes.
Many liquid medications contain sugars or sugar alcohols (such as sorbitol, used to enhance taste)—but these increase osmolality, which can cause osmotic diarrhea and tube clogging. Many liquid drug formulations also have high osmolality. This isn’t a concern when the drug is taken orally because it’s diluted with saliva, mucus, and gastric juices. But it can be a problem with medications given by feeding tube. High-osmolality drugs are tolerated more poorly with intestinal administration than gastric administration, where gastric juices provide more dilution. To help decrease diarrhea and the risk of tube clogging, dilute liquid medication with 20 to 30 mL of water before administering (unless contraindicated). Contact the pharmacist to determine optimal dilution volume for your patient and discuss specific feeding-tube location.
Keep in mind that drugs with a low pH (≤ 4) may be physically incompatible with tube-feeding formula and may lead to clumping with eventual tube clogging. For an overview of low-pH or high-osmolality medications of special concern for tube clogging when given by feeding tube, (See Low-pH or high-osmolality liquid medications.)
Drugs that shouldn’t be crushed
Crushing certain medications for feeding-tube administration isn’t recommended. Some medications are potentially carcinogenic, teratogenic, or cytotoxic. Crushing them could expose you to adverse health risks if the powder becomes aerosolized or contacts your skin.
Don’t crush enteric-coated pills, either. Doing so destroys the enteric coating and could irritate the gastric mucosa or reduce desired medication effects (from drug disintegration by gastric secretions). Also, be aware that enteric coatings can clog feeding tubes.
In addition, don’t crush sustained- or time-delayed release medications, and don’t give them by feeding tube. These formulations release medication over time to ensure a constant therapeutic dose. When crushed and given by feeding tube, the patient receives a high initial dose and, depending on drug action, may suffer such complications as respiratory depression or hypotension.
Delayed time-release medications are designated with various abbreviations. (See Abbreviations for delayed time-release medications.) Don’t give them by feeding tube; instead, request an alternative medication and dose.
Many medications have an alternative immediate-release form. If the delayed time-release capsule contains pellets, you can remove these from the capsule, if possible, and suspend them in water—but don’t crush them. However, be aware that pellets may increase the risk of tube clogging. For both enteric-coated and delayed time-release medications, discuss alternatives with the pharmacist and prescriber.
For medications that can be safely crushed and given by feeding tube, crush and dissolve each tablet separately; crush each one to a fine powder and mix with 15 to 30 mL of water. Hard gelatin capsules containing powdered drug can be opened and diluted with water.
During administration, flush the feeding tube with 30 mL of water before giving the first medication, between medications, and after the last medication. If you’re monitoring the patient’s water intake, be sure to document water flush volume with medication administration.
Finally, don’t mix medications with tube-feeding formula. Also, don’t give buccal or sublingual medications via feeding tube; instead, administer them by the ordered route.
Interventions
When a feeding tube becomes clogged, first withdraw any formula remaining in the tube. Then try to flush it with warm water and clamp for 5 minutes. Use a back-and-forth motion with the plunger of a 30- to 60-mL syringe as you instill water and try to aspirate. Repeat this several times.
If this maneuver doesn’t clear the tube, obtain an order for an alkalinized enzyme method using sodium bicarbonate and an uncoated pancreatic enzyme. In one method, a 324-mg sodium bicarbonate tablet is crushed to a fine powder and mixed with the contents of a crushed pancrelipase enzyme tablet (such as Viokase) with at least 5 mL of warm water. Flush the solution into the tube and clamp for 5 minutes; then flush with water until clear. You can try this several times. Check your organization’s policy for the specific alkalinized enzyme method to use, based on the sodium bicarbonate and pancrelipase enzyme your formulary stocks.
If you can’t clear the clog with the alkalinized enzyme, the tube may need to be replaced. Don’t use meat tenderizer or wires to clear a clogged tube. Special declogging devices are available,although research on their efficacy is limited. (See Overview of mechanical feeding-tube complications.)
Tube knotting and breakage
Feeding-tube knotting and breakage most often occur with small-bore, nasally placed tubes. A small-bore tube may become knotted when repositioned or removed; knotting prevents administration of feeding formula with a syringe. If the patient has a feeding pump, expect to detect high pressure or occlusion.
Tube breakage generally results from excessive pressure applied during flushing or instillation of bolus tube feedings or medications. Avoid excessive pressure by using a 30- to 60-mL syringe for formula, medication administration, and flushing.
If you suspect your patient’s tube is knotted or broken, contact the physician or NP. Generally, an endoscopic procedure is required to remove a knotted tube or a retained fragment from a broken tube.
Buried bumper syndrome
Buried bumper syndrome (BBS) occurs when the internal bumper (bolster) of a PEG tube migrates from the gastric lumen and lodges in the gastric mucosa or abdominal wall. Excessive traction on the internal bumper slowly pulls the bumper into the gastric wall, with eventual mucosal overgrowth. BBS occurs in approximately 1% to 8% of patients with PEG tubes; it’s rare with balloon-type gastrostomy tubes.
Signs and symptoms include feeding difficulties with the need for increased pressure during feedings, as well as inability to infuse the formula. Other findings include peristomal leakage, abdominal pain, and inability to move the tube. BBS most commonly occurs several months after PEG placement but has been reported as early as 21 days afterward.
Proper surgical technique and allowing a small distance between the external bumper and the patient’s skin can help prevent BBS. Generally, traction on the external bumper should be loosened 24 hours after placement. Consult the physician who placed the tube to verify when to loosen traction. Once the GI tract has formed (generally over 7 to 10 days), the catheter should move slightly. When the tract has formed and the stoma has healed completely, experts recommend daily tube movement of 1 to 2 cm in the stoma with 180-degree rotation.
To maintain appropriate tube tension, monitor and document the location of the external bumper setting. Over time, as the patient gains weight with enteral nutrition, the outer bumper may need to be loosened.
If you suspect BBS, stop feedings and notify the physician or NP. BBS can be detected endoscopically, by contrast injection, or by abdominal CT scan. If the gastric mucosa is enclosing the bumper completely, the tube must be removed.
New enteral connectors
New regulations to prevent accidental infusion of enteral nutrition into an I.V. line have led to development of new enteral connectors. Enteral nutrition administration sets, syringes, and feeding tubes are being updated with a unique patient access connector. If the end of a patient’s feeding tube has the new connector, a new compatible delivery system is needed.
New feeding bags have the new connector. However, a temporary adapter is needed to connect to the feeding tube until the ends of all feeding tubes have the new tube extension. Rollout of the new extension and syringes with the new connector will occur in 2016. A patient access transition set will help during the product change. Work with your facility’s supply providers during the transition to ensure you have the proper tube feeding administration supplies to provide nutrition and hydration.
Prevention is key
Preventing mechanical complications of feeding tubes helps ensure your patient receives proper nutrition and hydration intake. Important interventions include monitoring tube location frequently, securing the tube, flushing the tube regularly, and using proper medication administration technique.
Marilyn Schallom is a research scientist and critical care clinical nurse specialist at Barnes-Jewish Hospital in St. Louis, Missouri.
References
Ao P, Sebastianski M, Selvarajah V, et al. Comparison of complications rates, types, and average tube patency between jejunostomy tubes and percutaneous gastrostomy tubes in a regional home enteral nutrition support program. Nutr Clin Pract. 2015;30(3):393-7.
Bankhead R, Boullata J, Brantley S, et al; A.S.P.E.N. Board of Directors. Enteral nutrition practice recommendations. JPEN J Parenter Enteral Nutr. 2009;33(2)122-67.
Blumenstein I, Shastri YM, Stein J. Gastroenteric tube feeding: techniques, problems and solutions. World J Gastroenterol. 2014;20(26):8505-24.
Brugnolli A, Ambrosi E, Canzan F, et al; Naso-gastric Tube Group. Securing of naso-gastric tubes in adult patients: a review. Int J Nurs Studies. 2014;51(6):943-50.
Dibaise JK, Rentz L, Crowell MD, et al. Tract disruption and external displacement following gastrostomy tube exchange in adults. JPEN J Parenter Enteral Nutr. 2010;34(4):426-30.
Guenter P. New enteral connectors: raising awareness. Nutr Clin Pract. 2014;29(5):612-4.
Klang M, McLymont V, Ng N. Osmolality, pH, and compatibility of selected oral liquid medications with an enteral nutrition product. JPEN J Parenter Enteral Nutr. 2013;37(5):689-94.
National Patient Safety Agency. Rapid Response Report. Early detection of complications after gastrostomy. March 31, 2010.
Ojo O. Balloon gastrostomy tubes for long-term feeding in the community. Br J Nurs. 2011;20(1):34-8.
Rahnemai-Azar AA, Rahnemaiazar AA, Naghshizadian R, et al. Percutaneous endoscopic gastrostomy: indications, technique, complications and management. World J Gastroenterol. 2014;20(24):7739-51.
Rosenberger LH, Newhook T, Schirmer B, et al. Late accidental dislodgement of a percutaneous endoscopic gastrostomy tube: an underestimated burden on patients and the health care system. Surg Endosc. 2011;25(10):3307-11.
Stayner JL, Bhatnagar A, McGinn AN, et al. Feeding tube placement: errors and complications. Nutr Clin Pract. 2012;27(6):738-48.
Stepter CR. Maintaining placement of temporary enteral feeding tubes in adults: a critical appraisal of the evidence. Medsurg Nurs. 2012;21(2):61-8,102.
Toussaint E, Van Gossum A, Ballarin A, et al. Enteral access in adults. Clin Nutr. 2015;
34(3):350-8.
Williams NT. Medication administration through enteral feeding tubes. Am J Health System Pharm. 2008;65:2347-57.



















2 Comments.
Good Morning,
I work in an ICF for individuals with intellectual and developmental disabilities, many of whom are non-ambulatory but have use of their upper extremities. Would appreciate guidelines on how to place or curve long g-tubes under an individual’s shirt or blouse (not through out through the neck opening as other individuals may attempt to pull at them if they see the feeding port extending from the shirt). Attempting to avoid kinking of the tubing or extending the tube so that it may become taut and inadvertently pulled out . Also have individuals with behaviors who may attempt to pull the long g-tubes out. Understand abdominal binder is best, however on some individuals these cannot not used. Do you have illustrations of proper positioning of the tubing Also tips for direct care staff when turning and repositioning individuals as well as transferring individuals with g-tubes who are mostly small adults.
Hello,
I place dobhoff feeding tubes, and they often become pulled out 15-25 cm. We like then in the small bowel and usually place them at about 110 cm deep. The above research mentioned replacing a partially removed feeding tube. Does that mean that you re-insert the 10 -25 cm that was pulled out (with out the guide wire naturally) , following with a KUB. Or does that mean you remove the feeding tube completely and start with a new one.
thank you and I am greatly looking forward to your clairification