Insight study highlights critical perception gaps between leaders
and frontline nurses
A study exploring how healthcare organizations currently respond to todays challenges and how they could better use resources in the future revealed both congruence and striking differences in the perspectives of nurse leaders and frontline nurses. Most nurse leaders (72%) and frontline nurses (67%) in the Models of Care Insight Study agreed that their organizations current care delivery models need improvement. In contrast, considerably more nurse leaders (83%) than frontline nurses (60%) thought their organizations or departments have implemented or have considered changes to care delivery models since the pandemics start.
Nurse leaders and frontline nurses largely agreed that an unstable workforce is the primary reason their organization hasnt changed or considered changing care delivery models, but they diverged on other contributing factors. Nurse leaders were more likely to cite that current models are sufficient while frontline nurses named leadership resistance as the second most common reason for changes not being implemented.

The Models of Care Insight Study, supported by Healthcare Plus Solutions Group and conducted in early 2023 by Joslin Insight, involved in-depth interviews with some 50 healthcare leaders across the United States and an online survey of 3,387 nurses (healthcareplussg.com/models-of-care-insight-study/). The results reflect a 99% confidence level and 2.21% margin of error. Boston-Leary helped conceive and develop the study, and ANA promoted participation among its members and other stakeholders. The American Organization for Nursing Leadership also invited its members to participate.
The primacy of change management
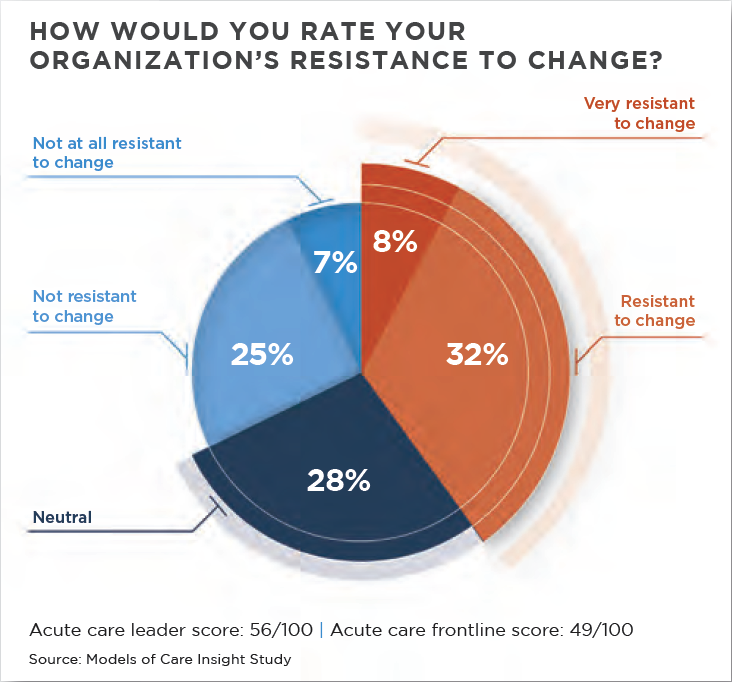
The study illustrates necessary but arduous change management efforts facing many healthcare institutions, according to Quint Studer, co-founder and partner of Healthcare Plus Solutions Group, a consultancy based in Pensacola, FL. Overall, 40% of respondents rated their organizations as very resistant or resistant to change, while 32% rated their organizations not resistant or not at all resistant to change. The 28% who were neutral on this question caught Studers eye. Theres a tendency to overestimate the readiness for change from the frontline staff, he said. We dont know that the people who said theyre neutral will embrace change. Nursing leaders have to take a step back and say, whats our communication plan to get the people who are neutral to understand where were going.
The study asked participants to rank care delivery roles that have or could have a positive impact on quality patient care delivery and RNs workloads. The top five such positions included certified nursing assistants, charge nurses, ancillary and auxiliary staff, float nurses, and patient care technicians. A similar question about programs that impact quality patient care and RN experience revealed the top five as healthy work environment, recruitment and retention, nurse mentoring, flexible scheduling, and professional development. The two new technologies incorporated in this ranking, remote patient monitoring and virtual nursing, ranked lowest among 15 options.
Exposing gaps
Across a series of questions about support for various roles and actions, the study assessed the perception gap between nurse leaders and frontline nurses from near perfect agreement to critical disagreement. The study found near perfect alignment on two issues; good, fair, and poor alignment each on one issue; and a critical gap on seven.
Consideration of LPNs in acute care settings was one of the areas with a critical gap assessment. Although 60% of leaders said their organizations had added or considered deploying LPNs in acute care, just 29% of frontline nurses thought their organizations had done so. A critical gap also existed regarding whether such a move would be welcomed60% of leaders thought staff nurses would support this care model, while a near equal percentage of frontline nurses (63%) said they would be opposed.
This dichotomy reinforces the communication chasm between nurse leaders and frontline staff, according to Hunter Joslin, CEO of Joslin Insight, a customer insights and strategy consultancy in Richmond, VA. This has less to do with whether LPN models would be effective and more to do with the conversations that leaders and frontline [nurses] are having, he said. I think that the conversations are coming to the frontline after the fact rather than before. And thats generally the problem, because its a top-down model.
Recognizing the challenges nurse leaders face in interacting consistently and meaningfully with frontline nurses, Joslin Insight created an app to enable leaders to connect with the frontline in real time and gather employee feedback 24 hours a day (joslininsight.com/realtime-listening/). Boston-Leary served as an advisor on its development.
(Dis)agreement on roles
Leaders and frontline nurses had near perfect alignment on whether staff nurses would back adding support nurses or a comparable role and whether they would favor adding nurse mentors and/or coaches. However, in both instances, a critical gap existed in understanding whether an organization had considered these approaches. Just 25% of frontline nurses thought their organizations had considered or added resource nurses, while 42% of nurse leaders indicated that they had tried or considered this approach. On the question of adding nurse mentors and/or coaches, 14% of frontline nurses thought this had been considered or implemented while 38% of nurse leaders said they had tried or considered this model.
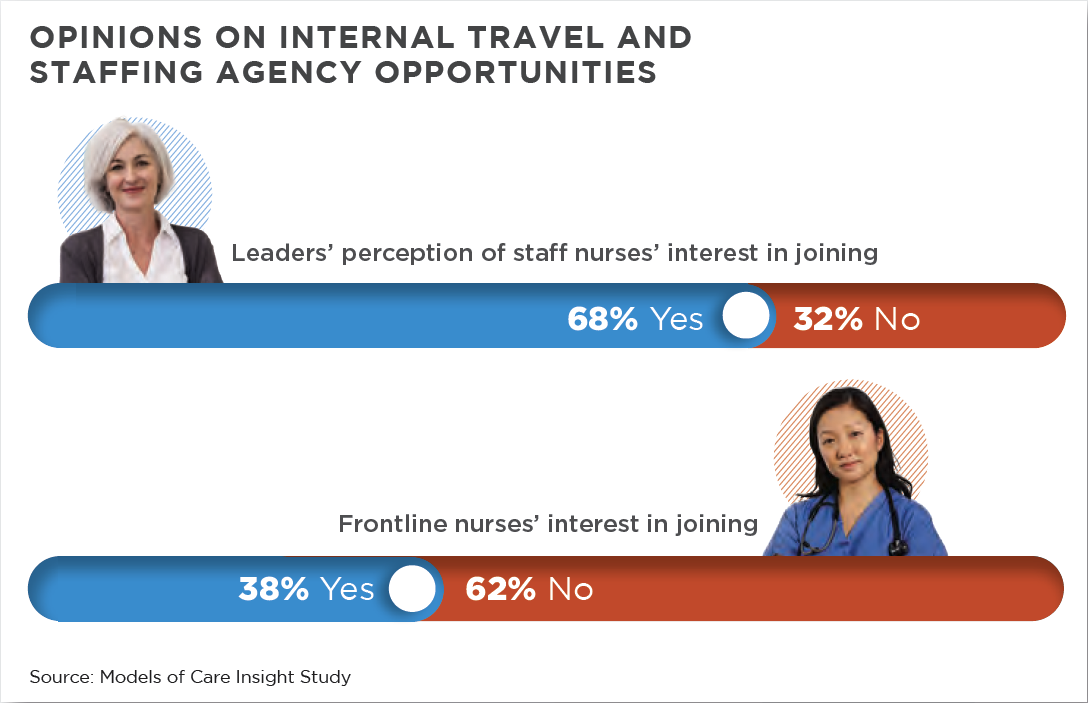
Most leaders and frontline nurses agreed that an internal travel or staffing agency had been tried or considered. However, there was a critical gap when it came to whether frontline nurses would be interested in joining such a program. More than half of nurse leaders (60%) thought frontline nurses would want to participate, whereas just 38% of frontline nurses said they would be interested.
Boston-Leary attributed this difference to social dynamics in the work setting that are hard to manage on the ground. One week Im working with you and were both peers and were making the same money. The next week I come in and were peers but Im making more than you and might have less experience than you, she observed. Fear of being othered by colleagues could turn nurses away from this option, she added.
Studer sees the results as a clarion call for nurse leaders to engage fully in skill development with a focus on change management. Weve really got to become experts in change management. This isnt just a little thing, he stressed.
Boston-Leary sees the study as leverage for nurse leaders to get funding for and enact new and revisited models of care. It helps make the strong case for nurse leaders to go to their CFOs and CEOs and get the resources that they need, she said. And it helps them create a list of roles that nurses say will help with what were facing now. Theyll be able to see where the gaps are, build a proforma, and get these roles funded.
Genna Rollins is a writer/editor at ANA.
American Nurse Journal. 2023; 18(6). Doi: 10.51256/ANJ062328