Many nurses find chest tube care intimidating—but it doesn’t have to be. Once you understand the basics, you can be confident when caring for patients who have chest tubes.
The practice of using a cannula to drain air or fluid from the pleural space dates back to antiquity. It’s one element in the trinity of life-saving medical procedures. (The others are endotracheal intubation and venous cannulation.) Hippocrates and Celsus recorded using hollow tubes to drain loculated empyemas. By the 1800s, catheters frequently were used to drain and irrigate empyematous cavities.
Chest Tube Care: It’s all about negativity
A brief review of pulmonary anatomy and physiology helps you understand where chest tubes are placed and how they work. Chest tubes aren’t placed in the lungs but in the pleural space—a potential rather than actual space between the parietal and visceral pleurae. The parietal (outer) pleura covers the chest wall and diaphragm. It contains a small amount (about 50 mL) of serous fluid that coats the opposing surfaces, allowing the visceral and parietal pleurae to glide over each other without friction while enabling the pleural surfaces to adhere to each other. Think of two glass plates with a thin coating of water; when you place the second piece of glass atop the first, the two plates slide smoothly. But when you try to separate them, they stick together.
How to recognize, prevent, and troubleshoot mechanical complications of enteral feeding tubes
The ability to adhere creates negative pressure within the pleural space, which becomes more negative as the visceral and parietal pleurae are pulled in opposite directions during inspiration. (Picture those two glass plates.) The negative intrapleural (and thus intrapulmonary) pressure generated causes air to flow from positive (atmospheric) pressure into the lungs. Expiration increases intrapleural and intrapulmonary pressures to the point where they exceed atmospheric pressure, creating an opposite pressure differential and causing air to flow out of the lungs into the surrounding atmosphere.
A breach in pleural integrity creates a separation between the parietal and visceral pleurae, allowing air or fluid to fill this potential space. (Using the glass-plate analogy, the two plates have become separated). The visceral pleura collapses inward along with the lungs, while the parietal pleura recoils outward along with the chest wall.
Indications for chest tubes
Chest tubes are used to treat conditions that disrupt the pleural space. The body can absorb small volumes of fluid or air over time. But larger volumes limit lung expansion, causing respiratory distress. In extreme cases, a tension pneumothorax may develop. This condition occurs when injured tissue forms a one-way valve or flap, enabling air to enter the pleural space and preventing it from escaping naturally. Seen mainly with thoracic trauma and line placement, this condition rapidly progresses to respiratory insufficiency, cardiovascular collapse, and ultimately death if unrecognized and untreated. It requires immediate live-saving treatment by inserting a needle to relieve pressure (needle thoracentesis), followed by chest-tube insertion. (See Conditions that disrupt the pleural space PDF page 2)
Chest tubes also may be used to prevent or mitigate postoperative complications. For example, after cardiac surgery or chest trauma, one or more chest tubes may be inserted in the mediastinum to drain blood and prevent cardiac tamponade. In addition, for proper chest tube care, chest tubes can be used to instill fluids into the pleural space, such as chemotherapy drugs or sclerosing agents to treat recurrent pleural effusions (a procedure called pleurodesis). Also, blood collected from chest tubes may be used for autotransfusion. (See Autotransfusion: Risks, benefits, and nursing care PDF, page 3)
Managing pleural-space disruptions
The overall goal of chest-tube therapy (chest tube care) is to promote lung reexpansion, restore adequate oxygenation and ventilation, and prevent complications. For treatment of pleural-space disruptions, chest-tube therapy should focus on three primary objectives:
- removing air and fluid as promptly as possible
- preventing drained air and fluid from returning to the pleural space
- restoring negative pressure within the pleural space to reexpand the lung.
Preparing for chest-tube insertion
Depending on the urgency of the situation, the nurse practitioner may insert a chest tube at the bedside, in the operating room, or in an interventional radiology suite. When-ever possible, informed consent should be obtained; caregivers should reinforce the benefits of the procedure (for instance, easier breathing with lung expansion).
The practitioner administers a local anesthetic, although use of a sedative/amnesic and analgesic agent or moderate sedation should be considered for patients without artificial airways. Provide supplemental oxygen and monitor the patient as you would during any invasive procedure. After chest-tube insertion, the patient may lose several hundred milliliters of blood or transudate, potentially leading to hypotension. So make sure emergency airway equipment and patent vascular access are available.
Equipment to gather for Chest tube care
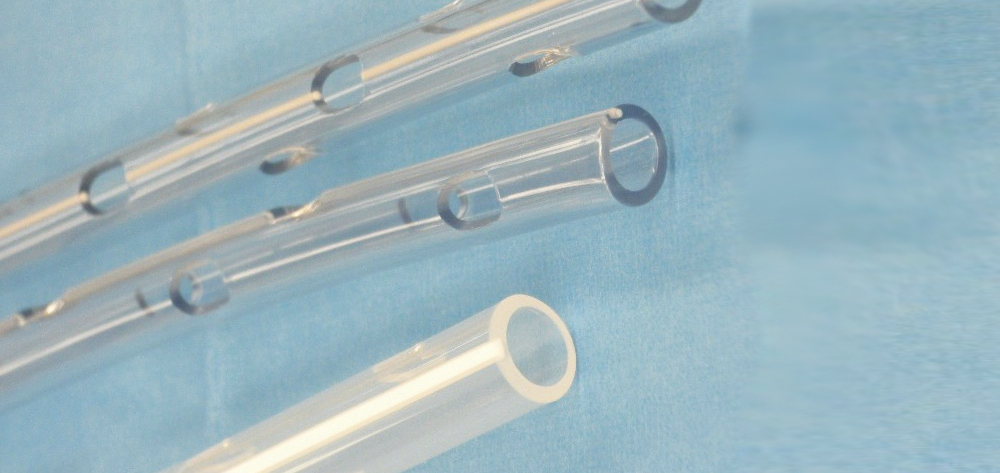
Obtain a thoracotomy tray and one or more chest tubes (sometimes called thoracic catheters)
of the appropriate size. Available in sizes ranging from infant to adult, chest tubes use the French sizing system—the larger the size, the larger the tube. Generally, larger tubes are used to drain blood and transudate, while smaller tubes are for air removal. Adults commonly require tube sizes between 24 and 40 French. Chest tubes also come in different configurations (curved or straight) and different materials (PVC or silicone) and are available with a heparin coating to reduce friction on insertion.
Set up the chest drainage unit (CDU) according to manufacturer’s instructions. (See Understanding chest drainage units PDF, page 3)
Patient positioning
Patient positioning depends on the insertion site, whether air or fluid will be drained, and the patient’s clinical status. Generally, the patient is positioned flat, with a small wedge or bolster (several folded towels or a blanket) placed under the shoulder blades to elevate the body and give the practitioner easier access. The arm on the procedural side must be kept out of the way; usually, it’s brought over the patient’s head and secured. Pendulous breasts or excessive adipose tissue may need to be secured out of the way as well.
The specific insertion site may vary with the condition being treated. Commonly, a chest tube is inserted at the midaxillary line between the fourth and fifth ribs on a line lateral to the nipple. (See A view of chest-tube insertion PDF, page 5)
Potential complications
Chest-tube insertion may cause bleeding, especially if a vessel is accidentally cut. Usually, bleeding is minor and resolves on its own, but bleeding into or around the lung may warrant surgical intervention. Proper Chest tube care is vital.
Infection risk increases with duration of tube placement. Regular dressing changes done according to facility policy can help identify and prevent site infections. Note changes in drainage amount and character, which may indicate increased bleeding or new-onset infection.
Subcutaneous emphysema may arise as pleural-space air leaks into subcutaneous tissue. When this happens, tissues of the neck, face, and chest swell and you may note crepitus on palpation. Notify the physician if you suspect subcutaneous emphysema; tube placement and suction level must be evaluated.
Nursing care: From patient to system
At least every 2 hours, document a comprehensive pulmonary assessment, including respiratory rate, work of breathing, breath sounds, and arterial oxyhemoglobin saturation measured by pulse oximetry (SpO2). Inspect the dressing and note any drainage. Assess the insertion site for subcutaneous emphysema and tube migration. Chest Tube Care basics: Keep all tubing free of kinks and occlusions; for instance, check for tubing beneath the patient or pinched between bed rails. Take steps to prevent fluid-filled dependent loops, which can impede drainage.
To promote drainage, keep the CDU below the level of the patient’s chest. Monitor water levels in the water-seal and suction-control chambers. Water in both chambers evaporates, so be sure to add water periodically to maintain the water-seal and suction levels.
Be aware that tidaling—fluctuations in the water-seal chamber with respiratory effort—is normal. The water level increases during spontaneous inspiration and decreases with expiration. However, with positive-pressure mechanical ventilation, tidaling fluctuations are the opposite: the water level decreases during inspiration and increases during expiration. If tidaling doesn’t occur, suspect the tubing is kinked or clamped, or a dependent tubing section has become filled with fluid. Also, don’t expect tidaling with complete lung expansion or with mediastinal tubes, because respirations don’t affect tubes outside the pleural space.
Intermittent bubbling, corresponding to respirations in the water-seal chamber, indicates an air leak from the pleural space; it should resolve as the lung reexpands. If bubbling in the water-seal chamber is continuous, suspect a leak in the system. To locate the leak’s source, such as a loose connection or from around the site, assess the system from the insertion site back to the CDU. When searching for the source of an air leak, use rubber-tipped or padded clamps to momentarily clamp the tubing at various points; bubbling stops when you clamp between the air leak and water seal. If you’ve clamped along the tube’s entire length and still can’t find the source, the CDU might be faulty; replacement should be considered.
Assess drainage: Chest Tube Care
Assess the color of drainage in the drainage tubing and collection chamber. Know that old drainage in the collection chamber may inaccurately reflect current drainage as shown in the tubing. At regular intervals (at least every 8 hours), document the amount of drainage and its characteristics on the clinical flow sheet. Report sudden fluctuations or changes in chest-tube output (especially a sudden increase from previous drainage) or changes in character (especially bright red blood or free-flowing red drainage, which could indicate hemorrhage). Frequent position changes, coughing, and deep breathing help reexpand the lung and promote fluid drainage.
Don’t milk, strip, or clamp the tube for Chest-tube care
Avoid aggressive chest-tube manipulation, including stripping or milking, because this can generate extreme negative pressures in the chest tube and does little to maintain chest-tube patency. If you see visible clots, squeeze hand-over-hand along the tubing and release the tubing between squeezes to help move the clots into the CDU.
As a rule, avoid clamping a chest tube. Clamping prevents the escape of air or fluid, increasing the risk of tension pneumothorax. You can clamp the tube momentarily to replace the CDU if you need to locate the source of an air leak, but never clamp it when transporting the patient or for an extended period, unless ordered by the physician (such as for a trial before chest-tube removal).
In the event of chest-tube disconnection with contamination, you may submerge the tube 1″ to 2″ (2 to 4 cm) below the surface of a 250-mL bottle of sterile water or saline solution until a new CDU is set up. This establishes a water seal, allows air to escape, and prevents air reentry.
Chest-tube removal
Indications for chest-tube removal include:
- improved respiratory status
- symmetrical rise and fall of the chest
- bilateral breath sounds
- decreased chest-tube drainage
- absence of bubbling in the water-seal chamber during expiration
- improved chest X-ray findings.
Chest Tube Care: Before starting chest-tube removal, inform the patient that the chest tube will be removed, and briefly describe the steps involved. Make sure the patient is premedicated to relieve pain and ease anxiety. Teach the patient how to do the Valsalva maneuver, which he or she must perform before tube removal to prevent air from reentering the pleural space.

Gather the supplies you’ll need, including sterile gloves, goggles, gown, mask, dressing supplies, sterile suture-removal kit, rubber-tipped hemostats, and wide occlusive tape. Place the patient in the semi-Fowler’s position and put a pad underneath the chest-tube site to catch any drainage.
After the dressing is removed and the sutures are cut, the practitioner clamps the chest tube with hemostats. Instruct the patient to perform the Valsalva maneuver as the practitioner quickly removes the tube at maximum inspiration. Immediately after tube removal, apply an occlusive dressing to the site and secure it with tape. Another chest X-ray should be taken several hours later to ensure that the lung is still fully inflated.
Nursing care after chest-tube removal includes:
- ongoing respiratory assessment
- vital-sign documentation
- monitoring the site for drainage
- assessing the patient’s comfort level.
De-stress over chest tubes
By understanding the indications for chest tubes and providing appropriate nursing care, from chest-tube insertion to removal and beyond, you’ll find chest-tube care less stressful while helping your patient breathe easier and recuperate without complications.
Selected references
American College of Surgeons. ATLS: Advanced Trauma Life Support Program for Doctors. 8th ed. Chicago, IL: American College of Surgeons; 2008.
Coughlin AM, Parchinsky C. Go with the flow of chest tube therapy. Nursing. 2006; 36(3):36-41.
Morton PG, Fontaine D, eds. Critical Care Nursing: A Holistic Approach. 9th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2008.
Parrillo JE, Dellinger RP, eds. Critical Care Medicine: Principles of Diagnosis and Management in the Adult. 3rd ed. St. Louis, MO: Mosby; 2008.
Protocol for autotransfusion: information from the Atrium 2450 self-filling ATS blood bag instruction insert. R Adams Cowley Shock Trauma Center, University of Maryland Medical Center. Last revised February 2008.
West JB. Respiratory Physiology: The Essentials. 8th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2008.
Both authors work at R Adams Cowley Shock Trauma Center, University of Maryland Medical Center in Baltimore. Mark Bauman is a senior clinical nurse II. Claudia Handley is a nurse manager in Select Trauma Critical Care. The authors and planners of this CNE activity have disclosed no relevant financial relationships with any commercial companies pertaining to this activity.



















8 Comments.
Never consider it a privilege to remove pacer wires or chest tubes. It’s simply transferring responsibility to a nurse. A giveaway is a “checklist” to follow before you do it.
Make the damned doctors do it. It’s not big deal and they can do it when they round. If a nurse is doing it, it’s in the name of time constraints and “getting a downgrade.” Screw your hospital. You do enough already.
So yes, I’ve seen a LOT of pericardial tears and chest tube errors in my life. Don’t do it. Ain’t worthi
Yes. Nurses in my Unit remove chest tubes and epicardial pacing wires. We do have a competency checklist that has to be completed – 4 CT removal under the supervision of a provider. Also, every time, we remove a CT, we document a complete checklist with all relevant details of the patient. This helps to review an episode should one need to. Must remove minimum 5 CT per month to maintain competency.
We also clamp & milk CT if ordered.
Never heard or seen a “curved chest tube”
WHAT IS MILKING
AND
HOW WE CAN DO IT??
Do Med/Surg nurses remove chest tubes in your facility, or just nurses in Critcal Care Areas? If Med/Surg nurses do-how do you maintain competency?
Hi, you mention in the article that there are curved chest tubes, though ive never seen one, any idea who makes them? Ive heard of one for effusions but im not sure its widely manufactured
Here is the author’s answer to sk’s question:
In my facility and in any other, there must be a physician’s order for clamping a chest tube. If not, the nurse is practicing out of scope of practice. As to who physically does it, that would be facility specific, although nurses here can and will do it, the physician or NP will usually do it as they assess the CT.
Do the nurses at your facility clamp the chest tube if there is an order? or must this be done by the physician?
I’m having a devil of a time just trying to login so that I can complete the test for my continuing education. What a hassle!