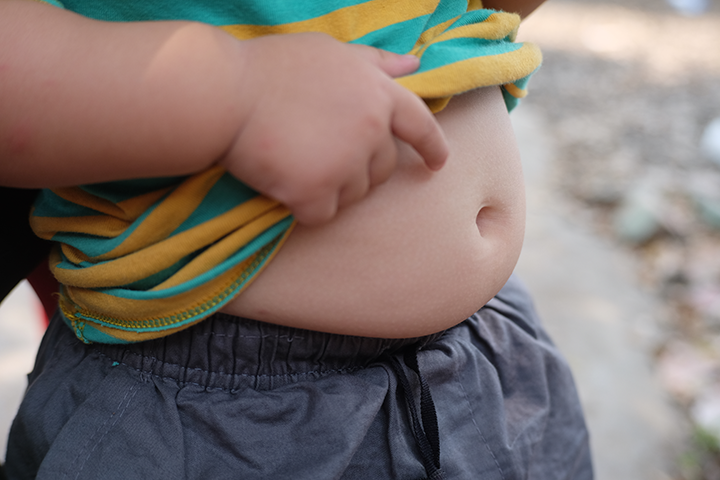
The number of overweight American children keeps growing at a rate that’s hard to swallow. And so does the number of American children at risk for becoming overweight. Unless we stop the spread of this problem now, the long-term debilitating effects on today’s children—and ultimately, on their children—will exhaust our healthcare resources. (See Big numbers get bigger and bigger by clicking on the PDF icon above.)
Obesity is linked to several serious conditions, including asthma, cancer, cardiac disorders, hyperlipidemia, and type 2 diabetes. In obese people, especially obese young adults, these conditions shorten the average lifespan by as much as 10 years. Obese children also face ostracism, social isolation, depression, and economic consequences.
No fast fix
Unfortunately, we have plenty of fattening fast food, but no fast fix for childhood obesity. We don’t have a vaccine to prevent it or a wonder drug to treat it. The only way to address the problem is one family at a time. That means teaching patients and their families about healthy lifestyle practices. Taking a family approach increases the chances that a child will make long-lasting changes to both diet and activity. Because parents control the home environment, they can make the right food choices and help increase physical activity by providing play and sports opportunities. And when parents participate in healthy behaviors with their children, success is more likely.
Because our scope of practice includes health promotion, assessment, screening, education, outcome evaluation, and referral to other professionals, nurses are uniquely positioned to help prevent and treat childhood obesity. We encounter children and families in their homes, schools, churches, parishes, clinics, and hospitals, and we have the professional skills and knowledge to attack childhood obesity on a grand scale. We can provide accurate, best-practice information and useful advice to children, families, and communities, whenever opportunities arise.
Guidelines plus practical tips
In 2007, the American Medical Association’s Expert Committee on the Assessment, Prevention, and Treatment of Child and Adolescent Overweight and Obesity issued comprehensive evidence-based guidelines for preventing and treating childhood obesity. The guidelines provide standards for physicians and nurse practitioners and recommend that nurses get involved. Knowing the guidelines will prepare you to help children and their families. (See Guidelines for addressing childhood obesity by clicking on the PDF icon above.)
The following sections on weight, diet, physical activity, family history, physical examinations, and laboratory tests cover the guidelines and provide additional practical information.
Weight
Height and weight should be measured at least annually between ages 2 and 20. The standard measure for assessing weight is the body mass index (BMI), which you can calculate. Divide the patient’s weight in kilograms by his or her height in meters squared: weight ÷ (height x height) = BMI. After obtaining a patient’s BMI, plot it on a BMI growth chart for boys or girls, as appropriate, to determine the percentile. You can find BMI for age and gender charts at www.cdc.gov/growthcharts. Ask overweight children how they feel about their weight and if they’re ready to make changes. (See What about skinfold measurements by clicking on the PDF icon above)
Diet
There’s no mystery about why children are overweight. They consume more calories than they burn through physical activity. Compared with normal-weight children, overweight children:
- eat larger portions
- consume calorie-dense foods at restaurants more often
- eat fast food more often
- consume more sugar-sweetened drinks
- snack more between meals
- eat breakfast less often
- drink less milk
- eat school lunches less often.
At each well-child visit, assess the patient’s dietary habits, using a 24-hour diet recall; a 3-, 5-, or 7-day food diary; or a food questionnaire. You can have parents and children write a 24-hour diet recall while they wait for their appointment.
Food diaries, the most reliable method, can help families and children identify unhealthy patterns that affect weight. Patients and parents must complete food diaries at home and bring them to their next appointment. When completing these forms, parents and children must include portion sizes.
Complete dietary assessments include the number of meals and snacks eaten during the day, the places meals are eaten, the number of times families eat together, the number of times a week patients eat at restaurants or fast-food places, the number of sweetened beverages (including fruit juices) consumed in a day, the food portion sizes, the number of times a week the patient eats breakfast, the types of foods eaten for breakfast, and the number of fruit and vegetable servings consumed in a day. You can gather this information by having the parent and patient fill out a questionnaire or by asking questions during an appointment.
Physical activity
At each well-child visit, assess the patient’s physical activity and sedentary behavior. Explore how confident the child is about participating in physical-activity programs and how willing he is to change his behavior. Assess other factors that can influence participation in physical activity, such as environmental conditions, social support, and barriers to activity. Find out the number of hours the child is physically active every day and the types of physical activities he engages in.
Also, determine how many hours a day the child watches television, plays video or computer games, and watches DVDs.
Questionnaires can help gather this information. Questions such as: “How do you get exercise (walk, jog, play recreational sports, play competitive team sports)?” and “How many minutes a day do you watch television, play computer or video games, or watch DVDs?” can elicit the answers you need. Compare the patient responses with these recommendations: 1 hour a day of at least moderate physical activity and less than 2 hours a day of sedentary activity.
Family history
Children of obese parents have a higher risk of being overweight or obese than children of normal-weight parents. Depending on the extent of parental obesity and the associated chronic conditions, the risk can be 3 to 13 times higher.
Screen overweight and obese children older than age 2 for a parental history of cardiovascular disease, hypertension, diabetes, and obesity. A parental history of these chronic diseases or early death from cardiovascular events, such as myocardial infarction and stroke, increases the risk that overweight children will develop the same problems at an earlier age. Your health history should elicit these risks factors, so children can be monitored appropriately.
Physical examination
As weight increases, so does the risk of complications in all body systems. To identify disorders and prevent devastating complications, perform a complete physical examination. Assess the skin, eyes, heart, lungs, abdomen, neurologic system, and musculoskeletal system. Measure the pulse and blood pressure.
Your assessment may reveal such findings as acanthosis nigricans—a darkening of the skin on the neck, in the axilla, and in the groin caused by hyperinsulinemia. This finding indicates insulin resistance, a risk factor for type 2 diabetes. In some states, school nurses screen children for this sign. The examination should also include an assessment of psychological functioning, self-efficacy, and willingness to change. Children with signs and symptoms of comorbid conditions need further evaluation.
Laboratory tests
Overweight and obese children should have fasting lipid, aspartate aminotransferase, and alanine aminotransferase levels measured. Obese children should also have blood urea nitrogen and creatinine levels measured.
According to the American Diabetes Association, children age 10 and older and pubertal children younger than age 10 with a BMI above the 85th percentile and two other risk factors should have a fasting plasma glucose test every 2 years. Risk factors include a history of type 2 diabetes in a first- or second-degree relative; American Indian, African American, Hispanic, Asian, or Pacific Islander ethnicity; and signs and symptoms of insulin resistance, such as acanthosis nigricans, hypertension, hyperlipidemia, and polycystic ovarian syndrome.
Early prevention and intervention
Identifying overweight and obese children provides an opportunity to treat the weight problem and to prevent or treat long-term complications. Unfortunately, many parents don’t think their children are overweight or obese, and they aren’t concerned about what they may call “baby fat.” But you can enlighten them about what the child’s weight really means and what sorts of health risks the child faces.
For normal-weight children, your primary goal is to teach them to maintain their weight. The Expert Committee recommends teaching children with a normal BMI about dietary intake, physical activity, and eating behaviors. Dietary counseling should encourage patients to limit sugar-sweetened beverages (including fruit juices) and calorie-dense foods, to eat the recommended amounts of fruits and vegetables every day, and to increase calcium, fiber, and macronutrient intake.
As appropriate, encourage mothers to breast-feed their children, even for a short period. Studies indicate that breast-feeding is associated with a lower risk of children becoming overweight. And the longer the duration of breast-feeding, the lower the risk. These benefits of breast-feeding may extend into the late teen years and even adulthood.
Recommend that all children increase physical activity to 1 hour a day and limit the time for television, computer and video games, and DVDs to 2 hours. Encourage healthy eating behaviors, including limiting portion size and eating meals with the family. Studies show that people who eat in front of the television tend to eat larger quantities of food and don’t stop when they are full. Family dining at home creates a healthy environment for eating as well as for socializing and developing language skills.
Parental behaviors strongly influence children’s eating and physical activity. Encourage parents to replace calorie-dense foods with healthy foods, such as fresh fruits and vegetables. Also, teach parents to encourage their children to stay active and avoid sedentary activities.
Stages of therapy
The treatment of overweight children involves a staged approach based on age, BMI, other medical conditions, parental weight status, and treatment progress. (See Weight-loss goals for children by clicking on the PDF icon above.)
Stage 1
Overweight children begin therapy at stage 1, which nurses can implement. Dietary changes include:
- eating five or more servings of fruits and vegetables daily
- eating breakfast every day
- consuming no sugar-sweetened beverages
- limiting eating at restaurants and fast-food places
- having families allow children to self-regulate meals.
Encourage children to engage in physical activity 1 hour a day and to limit sedentary activities to fewer than 2 hours a day.
The goal of stage 1 is weight maintenance; BMI will decrease as the patient’s age increases. If caloric intake is balanced with calories burned during physical activity, a child’s caloric requirements will be met, and weight will be maintained as height increases and children “grow into their weight.” When working with parents, stress the importance of weight maintenance for improving the child’s health. In stage 1, the child is evaluated every month. If weight status doesn’t improve in 3 to 6 months, the patient moves to stage 2.
Stage 2
In stage 2, which can be implemented by nurses who have special training in weight management, the dietary and physical activity changes are more structured. The goal of this stage is either weight management or gradual weight loss.
This stage has an individualized plan for meals and snacks that contain small amounts of calorie-dense foods. The patient engages in 1 hour of play, supervised by an adult. Sedentary activities are limited to less than 1 hour a day.
Nurses strongly encourage patients to keep logs of food intake, restaurant food consumption, physical activity, and sedentary activity, which the nurses review. If children don’t improve in 3 to 6 months, they move on to stage 3.
Stage 3
The goal is the same as for stage 2—weight maintenance or gradual weight loss. To help achieve this goal in stage 3, a multidisciplinary, obesity care team designs and implements an eating and activity plan. Nurses work with the children and their families to apply behavioral modification strategies and to develop specific goals for diet and physical activity.
Stage 4
The goal for this stage is significant weight loss. Children are referred to a pediatric tertiary weight-management center, which has multidisciplinary teams that include endocrinologists, pediatricians, psychiatrists, psychologists, dieticians, pharmacists, surgeons, nurses, and nurse practitioners. Aggressive treatments include meal replacement therapy, severe calorie restrictions, drug therapy, and surgery.Drugs including orlistat (Xenical), a lipase inhibitor, and sibutramine (Meridia), an appetite suppressant, as well as behavioral therapy can reduce weight and improve metabolic risk in obese adolescents. Surgery, such as gastroplasty, laparoscopic gastric banding, and gastric bypass, is reserved for children older than age 16 who have a BMI greater than 40 or obesity-related comorbidities and a BMI greater than 35.
Use your influence
As nurses, we have the opportunity to influence children and their families and thus help prevent and treat childhood obesity, one of the most serious health problems in America today. We can help spare children the physical and psychological complications of obesity and keep them from becoming unhealthy, obese adults who raise more unhealthy, obese children.
Selected references
American Diabetes Association. Standards of medical care in diabetes-2008. http://care.diabetesjournals.org/cgi/reprint/31/Supplement_1/S12. Accessed May 1, 2008.
American Medical Association. Expert committee recommendations on the assessment, prevention, and treatment of child and adolescent overweight and obesity. 2007. www.ama-assn.org/ama/pub/category/11759.html. Accessed May 1, 2008.
Davis MM, Gance-Cleveland B, Hassink S, Johnson R, Paradis G, Resnicow K. Recommendations for prevention of childhood obesity. Pediatrics. 2007;120(suppl 4):S229-S253.
Harbaugh BL, Jordan-Welch M, Bounds W, Blom L, Fisher W. Nurses and families rising to the challenge of overweight children. Nurse Pract. 2007;32(3):31-35.
Mullen MC, Shield J. Childhood and Adolescent Overweight: The Health Professional’s Guide to Identification, Treatment, and Prevention. Chicago, IL: American Dietetic Association; 2004.
Marti Jordan-Welch is an Assistant Professor, and Bonnie Lee Harbaugh is an Associate Professor at the University of Southern Mississippi School of Nursing in Hattiesburg. Marti Jordan-Welch holds stock in Pfizer. Bonnie Lee Harbaugh and the planners of this CNE activity have disclosed no relevant financial relationships with any commercial companies pertaining to this activity.