Follow this protocol and teach it to caregivers and patients.
- Nurses play an essential role in educating patients and caregivers about early recognition of hypoglycemia symptoms.
- Symptoms in children include sweating, tachycardia, tremor, palpitations, nervousness, hunger, pallor, confusion, lethargy, uncharacteristic behavior, irritability, seizures, and coma.
- Immediate treatment includes initiating the Rule of 15.
The parents of Susie Johnson*, a healthy 8-year-old child, bring her to the emergency department because she’s been experiencing abdominal pain, nausea, and vomiting. Susie recently was diagnosed with new-onset type 1 diabetes after a history of polydipsia, polyuria with bedwetting, and unexplained weight loss. Laboratory results reveal glucose 586 mg/dL, bicarbonate 18, and A1c 9.8%. Susie is admitted to the pediatric unit. You find her alert and sitting up in bed. Her vital signs are normal, and she says she’s hungry.
The provider’s orders include administering subcutaneous long-acting insulin nightly and rapid-acting insulin for carbohydrate coverage with meals and a correction factor to treat hyperglycemia. The orders also include maintenance I.V. fluids of normal saline with potassium chloride and insulin administration. At lunch, you administer 3 units of rapid-acting insulin to cover 40 grams of carbohydrate Susie ate.
Early recognition
About 2 hours later, Susie’s mother calls out to the nurses’ station. She’s concerned that Susie is acting strangely. Susie is awake but confused, her hands are shaking, and her skin is pale, cool, and clammy. You recognize these symptoms as acute hypoglycemia. You obtain a fingerstick glucose, which returns a result of 52 mg/dL.
As you reassure Susie and her mother, you ask a colleague to notify the physician on call. You take Susie’s vital signs, which are HR 120 beats per minute, RR 26 breaths per minute, and blood pressure 94/68 mmHg. Your neurologic assessment is unremarkable.
While waiting for the physician, you remember the Rule of 15 and provide Susie with 4 oz of orange juice. A repeat fingerstick glucose shows 68 mg/dL. Susie still appears confused and shaking. You provide her with another 4 oz of orange juice. On your next 15-minute reassessment, Susie’s glucose increases to 102 mg/dL. Susie remains quiet, but her hands are less shaky and her skin color is returning to baseline. You provide Susie with a snack of peanut butter crackers to help stabilize her glucose.
Education
Nurses are essential to educating patients and caregivers about early recognition of hypoglycemia symptoms, which include sweating, tachycardia, tremor, palpitations, nervousness, hunger, pallor, confusion, lethargy, uncharacteristic behavior, irritability, seizures, and coma.
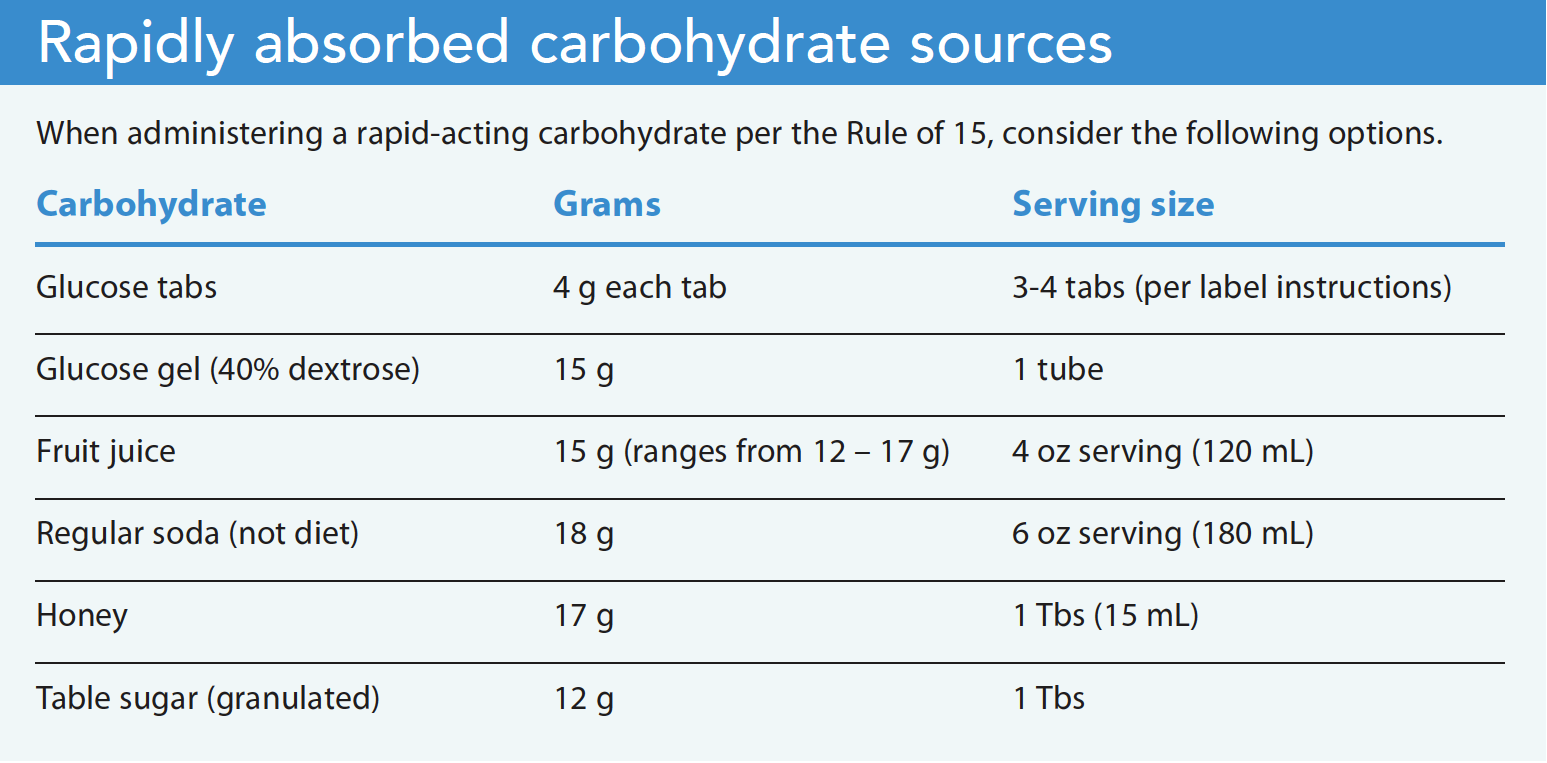
After obtaining a rapid bedside glucose level, standard hypoglycemia treatment begins when glucose values are <70 mg/dL (3.89 mmol/L) or when patients experience symptoms. Immediate treatment includes following the Rule of 15, which involves administering a 15 g rapid-acting carbohydrate.
After 15 minutes, the caregiver reevaluates the glucose level. Administering the rapid-acting carbohydrate continues until the glucose normalizes. When that happens, a snack or small meal can stabilize glucose. The Rule of 15 allows caregivers of children with diabetes to treat hypoglycemia without overcorrecting, which can result in hyperglycemia.
If the patient experiences extreme hypoglycemia with unconsciousness or inability to swallow, administer glucagon per instructions.
Outcome
Susie’s condition remains stable, and she’s discharged home after you provide her and her parents with instructions on the Rule of 15.
*Names are fictitious.
Vanessa Lee Hedge is an assistant professor at Radford University School of Nursing in Radford Virginia.
American Nurse Journal. 2023; 18(3). Doi: 10.51256/ANJ032340
Key words: hypoglycemia, type 1 diabetes, pediatric patients, Rule of 15
References
American Diabetes Association. Hypoglycemia (low blood glucose). diabetes.org/healthy-living/medication-treatments/blood-glucose-testing-and-control/hypoglycemia
UpToDate. Rapid overview for diagnosis and treatment of hypoglycemia in adolescents and children (other than neonates) in the emergency department. 2023. https://www.uptodate.com/contents/image?imageKey=PEDS%2F83485