Your quick action can help decrease morbidity and mortality, shorten hospital stays, and reduce costs.
Takeaways:
- Large total body surface area burns require immediate and aggressive assessment and management from well-trained nurses in a variety of settings.
- Patients’ responses to treatment need to be carefully and frequently monitored to prevent complication and improve survival.
In 2016, more than 200,000 people in the United States were hospitalized with injuries from smoke, fire, or flame exposure; more than 6,000 died. (See Facts and figures.) Burns damage skin and underlying tissue, disrupting the skin’s regulatory functions. Patients with acute burns require significant and costly interprofessional care that includes nurses, advanced practitioners, surgeons, pharmacists, physical and occupational therapists, and social workers.


The ABCDEs of emergency burn care
Excessive opioids lead to a close call for a burn patient
How to recognize and respond to hypovolemic shock
Proper initial management of a patient with serious burns can have significant impact on his or her long-term health outcomes. (See Skin and burns.)
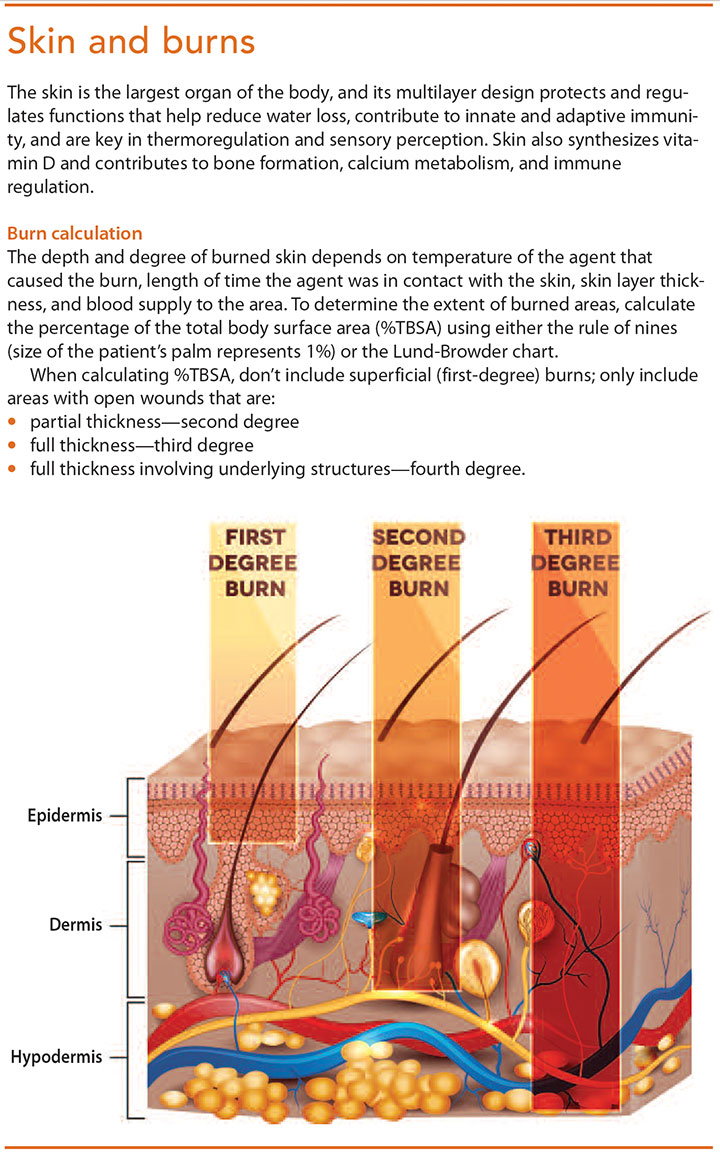

Primary assessment
Primary assessment of patients with acute burns starts with airway patency and cervical spine protection (in cases of a suspected spinal cord injury or if the patient is un-conscious and you have no other sources of information about the accident). Assess breathing, central and peripheral circulation, and cardiac status; stabilize any disability, deficit, or gross deformity; and remove clothing to assess the extent of burns and concurrent injuries.
Airway
Airway assessment includes visualizing the upper airway to look for obstructions, edema, or evidence of burn (soot; singed nasal hairs, eyebrows, facial hairs; raspy voice; cough). Place an oral pharyngeal device to protect an unconscious patient’s airway. If you see edema or evidence of burn in the upper airways, assess whether an endotracheal (ET) tube is needed to maintain the airway. There may be only a small window of opportunity to easily place an ET tube because edema from burn shock may obstruct the airway. If you suspect cervical spine injury, apply immobilization with a collar before doing anything that will flex or extend the neck.
Auscultate breath sounds and inspect and palpate the patient’s chest wall. Unless an ET tube is required, start high-flow oxygen at 15 L on a non-rebreather mask with concurrent partial pressure of carbon di- oxide monitoring on every patient with burns. Circumferential burns at the neck or torso may impair ventilation, and other conditions (such as pneumothorax) may cause respiratory distress. Help advanced practice providers perform procedures (bedside escharotomies to release constrictive eschar, needle decompression to relieve a tension pneu- mothorax, chest tube placement to drain fluid buildup) to improve the patient’s work of breathing.
Vital signs
Monitoring vital signs and the color of unburned skin can help you assess the patient’s circulatory and cardiac status. Carefully check pulses in any extremity with circumferential burns. These burns can act as tourniquets as burn-associated edema begins, leading to compartment syndrome. Heart rate (HR) in most adult burn patients will be elevated to 100 to 120 beats per minute (bpm) because of increased circulating catecholamines and hypermetabolism; HR higher than that may indicate hypovolemia from trauma, inadequate oxygenation, or uncontrolled pain and anxiety. Blood pressure and other vital signs in early stages of burn resuscitation should be the same as the patient’s baseline. Arrhythmias may be seen in electrical burn injuries, electrolyte imbalances, or underlying cardiac abnormalities. Begin interventions as ordered to avoid complications.
Neurologic assessment
In most cases, neurologic status won’t be altered in the early stages of burn injury. Determine if the patient is alert, responsive to verbal and pain stimuli, or unconscious. If the patient isn’t alert and oriented upon arrival, consider an associated injury, carbon monoxide poisoning, substance abuse, hypoxia, or preexisting medical conditions and intervene as appropriate. Use the Glasgow Coma Scale to trend the patient’s neurologic status throughout resuscitation.
Skin exposure
To prevent increased depth of injury, remove any causative burn agent from the skin and immediately flush the affected area with tepid water. However, use caution to pre- vent a rapid drop in body temperature and subsequent ventricular fibrillation or asystole. Don’t use ice to cool the area; it can further damage the skin or cause hypothermia. Remove all of the patient’s clothing, jewelry, shoes, diapers, and contact lenses to stop the burning process and prevent the items from becoming tourniquets when edema develops. To preserve core body temperature, cover the patient and the burn wounds with clean sheets or blankets, use warmed fluids, and maintain a warm environment.
Transport
If the patient needs more care or resources than currently available, prepare him or her for transport to the nearest burn center. Critically ill and multiple trauma patients, specialty population patients (such as children), and those who need additional technology may require transfer. The American Burn Association (ABA) has identified patients who are best served at a burn center.
Secondary assessment
The secondary assessment shouldn’t begin until the primary assessment is complete; resuscitative efforts are underway; and lines, tubes, and catheters are placed. (See Supporting the patient with burns.) This assessment includes a complete history, such as information about the burn injury, head-to-toe physical examination, accurate calculation of the percentage total body surface area (%TBSA) affected, fluid resuscitation requirements, and wound care.


History
If you can’t gather a history from the patient, interview family members, friends, or those who were at the scene. In addition to the patient’s medical history, record detailed information about the circumstances and mechanism of the injury. Additional questioning will be necessary if the patient was found in an enclosed space, has potential orthopedic injuries associated with the burns, or had clothing on fire. Data collected in these circumstances can significantly change your plan of care. For example, inhalation in closed spaces may involve toxins, which will prompt the provider to order additional tests. And burns to the face may significantly impact the airway. You’ll also want to gather addition- al information if an accelerant was used, an explosion was witnessed, the burn is related to a motor vehicle accident, or the reported circumstances are inconsistent with the burn pattern (suspected abuse).
Lab work and tests
A variety of laboratory tests will be needed within the first 24 hours of a patient’s admission (some during the initial resuscitative period and others after the patient is stab lized). Every patient will have complete blood count, electrolytes, blood urea nitrogen, creatinine, and glucose levels drawn. If the burn occurred in an enclosed space, arterial blood gas and carboxyhemo- globin levels will be needed because toxins in the air can cause carbon dioxide to displace oxygen in red blood cells; an arterial blood gas is also helpful if an inhalation injury is suspected.
Other tests include:
electrocardiogram—done at baseline before fluids are started because cardiac arrhythmias may occur during early stages of resuscitation for large burns
chest X-ray—to detect fluid accumulation, position of the ET tube (if intubation is required), or atelectasis caused by large-volume fluid resuscitation
serum lactate—helps detect acid-base imbalance and may help in predicting survival
cyanide level—done if unexplained lactic acidosis occurs; patients with smoke inhalation are at risk for cyanide toxicity
blood type and crossmatch—for patients with severe trauma in addition to burns who might need blood or blood products
urine myoglobin, serum creatine kinase—help detect injuries to kidneys or muscles and used to help diagnose rhabdomyolysis, which can occur with electrical or extensive third-degree burns. Tetanus immunization should be administered in any patient with burns deeper than superficial.
Wound care
Burns create a large open wound in which normal skin flora can begin to colonize. Left untreated, this can lead to severe cellulitis or sepsis. Wound care is essential to prevent infection and should be performed immediately after completing primary and secondary assessments and any life-or limb-threatening conditions are treated. After pre-medicating the patient with an analgesic agent to reduce pain, thoroughly wash the area with water and skin disinfectants or antibacterial soap. Clean away materials found on the wound and debride large ruptured blisters. Using a strip pattern, apply antibacterial ointment and nonadherent gauze to any open areas. Keep the gauze loose enough to allow for swelling and secure it with tape.
Additional interventions to prevent infection include:
- give daily baths with skin disinfectants
- perform wound care wearing isolation gown, mask, and surgical cap
- implement strict staff and visitor handwashing policies
- change lines every few days per institutional policy
- minimize performing interventions through nonintact skin.
If the patient develops a high fever, he or she may be pancultured and prescribed broad-spec- trum antibiotics until a specific organism is identified.
Fluid resuscitation
Most burn centers use a modified Parkland formula to calculate total fluid volume requirements, taking into account %TBSA and the patient’s body weight. (See Parkland formula.) This formula helps determine fluid needed from loss and shifts related to the injury, as well as insensible losses, and loss through nonintact skin.


After a total volume is calculated, half of that volume is given in the first 8 hours after the time of the injury, 25% in the second 8 hours, and the final 25% in the last 8 hours. If you don’t see the patient until 2 to 3 hours after he or she sustained the injury, you’ll have to catch up quickly. Use the patient’s urine output and physiologic response to determine if the volume is adequate for resuscitation. Consistently reassess for treatment effectiveness and make adjustments as necessary. Count fluids given via other methods (including I.V. medication diluents and nasogastric tube feeding) in the fluid calculation.
Fluid shifting that occurs with large %TBSA burns are a result of shock, which moves the circulating volume into the soft tissue and creates hypovolemia in the first 48 hours after the injury. Rapid and aggressive fluid resuscitation is needed to replace intravascular volume and maintain end-organ perfusion. The fluid in the damaged area will exit via the open wound, increasing the amount of fluid needed by the whole body to maintain homeostasis. Although crystalloids like lactated Ringers are the preferred volume-replacement therapy, some patients will require colloids, such as albumin, to retain as much fluid as possible inside the vessels.
During initial resuscitation (the first 24 hours), reassess the patient’s responsiveness to treatment hourly and follow protocols for adjusting fluid based on urine output. In the case of delayed resuscitation, assess the patient’s volume status every 24 hours, looking for fluid overload and other complications, such as rhabdomyolysis, rising lactate levels, acid-base imbalances, and compartment syndrome resulting from all the fluids given during resuscitation.
Pain and anxiety
Pain at the secondary assessment will vary based on injury depth and the amount of nerve involvement; a variety of nonpharmacologic interventions can reduce pain and allow you and other members of the healthcare team to provide treatments and therapies, such as dressing changes and physical and occupational therapy, that many burn patients can’t tolerate without medication. If no contraindications exist, the head of the bed should be elevated at least 30 degrees throughout resuscitation. In addition, elevate affected extremities above the level of the heart to de- crease edema and subsequent pain. Wounds, especially partial thickness and superficial burns, will be most painful when ex- posed to air, so perform dressing changes efficiently with only one exposed area at a time. Premedicating the patient (for example, with I.V. fentanyl or hydromorphone) and warming the room will improve the experience for both you and the patient. When possible, group painful interventions to be performed at the same time.
Psychosocial and the resulting responses to burn trauma vary. Be prepared to provide emotional sup- port throughout the resuscitation process. To help you engage in therapeutic communication and develop a rapport with the patient, talk him or her through interventions, refrain from making judgmental comments or giving unsolicited advice, and acknowledge rather than trivialize feelings of depression, guilt, fear, or anger. Advocate for psychiatric support by helping to connect the patient with survivor and family support groups; information is available at the ABA website.
Act quickly
When a patient presents with a deep burn or a burn covering a large %TBSA, quickly assess and intervene to prevent systemic and localized complications. Your interventions will be based on the type, extent, depth, and degree of the burn, as well as concurrent injuries. Early diagnosis and treatment lead to improved morbidity and mortality, shorter hospital stays, and decreased costs.
The authors work at the University of Cincinnati College of Nursing in Cincinnati, Ohio. Sarah Strauss is a nurse practitioner in the division of plastics, reconstructive, burn, and hand surgery. Gordon L. Gillespie is an associate professor.
References
American Burn Association (ABA). Advanced Burn Life Support Course: Provider Manual, 2017 Update. Chicago: ABA; 2017.
American Burn Association. Burn incidence and treatment in the United States: 2016. 2017.
Herndon DN. Total Burn Care. 5th ed. London, England: Elsevier; 2018.
Lai-Cheong JE, McGrath JA. Structure and function of skin, hair and nails. Medicine. 2017;45(6):347-351.



















1 Comment.
Excellent article. It was helpful since it was directed more toward nursing.