Report provides a road map for change.
Takeaways:
- A recent report from the National Academies of Sciences, Engineering, and Medicine estimates that between 35% and 54% of U.S. nurses and providers, across all clinical disciplines and care settings, have symptoms of burnout.
- The final report from the National Academies provides nurse leaders with a road map to prioritize workplace improvements and establish interventions to prevent and mitigate burnout and foster professional well-being.
Nurses and other clinicians are deeply committed to serving their patients with respect, fairness, and compassion. However, an accumulation of factors (including complex systems, emotional exhaustion, depersonalization, and loss of professional efficacy) creates a widening gap between what nurses believe they should be doing and what they’re able to accomplish. The result is system stress and clinician burnout. A recent report from the National Academies of Sciences, Engineering, and Medicine (the National Academies) estimates that between 35% and 54% of U.S. nurses and providers, across all clinical disciplines and care settings, have symptoms of burnout. Addressing these factors and providing physical, emotional, and institutional resources are critical to clinicians’ professional health. The National Academies’ report provides guidance that helps leaders with this process.
Examining the evidence
The National Academies convened an ad hoc 17-person committee, including nurses, physicians, pharmacists, and others, to examine scientific evidence about the causes of clinician burnout and its consequences, identify interventions that support clinician well-being, and propose a research agenda to improve the knowledge base. The committee reviewed more than 4,000 articles, synthesized findings, and drafted a report that underwent external peer-review before it was finalized. The final report, Taking Action Against Clinician Burnout: A Systems Approach to Supporting Professional Well-Being, provides leaders with a road map to prioritize workplace improvements and establish interventions to prevent and mitigate burnout and foster professional well-being.
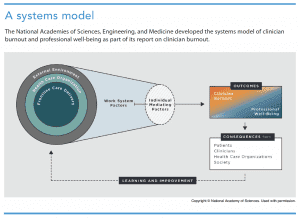
The committee focused on a systems approach that incorporates individuals, their activities, the technologies they use, and the environment in which they operate. The committee then developed a model that depicts work system factors (external environment, the healthcare organization, and care team interactions), recognizes that the individual is part of the work system, and considers individual mediating factors that influence the presence or absence of burnout and professional well-being. (See A systems model.)
Out-of-balance work system factors can contribute to burnout risk or positively impact professional well-being. The factors fall into two categories: job demands (workload, inadequate staffing, administrative burden, moral distress, inadequate technology usability) and job resources (meaning and purpose in work, organizational culture, job control, autonomy, professional relationships, and social support). Not all factors are easily modifiable, but some are responsive to interventions targeted at known work system factors (individual and organizational) that influence burnout and well-being.
The National Academies’ committee proposed six goals for improving clinician well-being.

Goal 1: Create positive work environments
Nursing has a proven track record for achieving positive hospital work environments. The American Nurses Credentialing Center Magnet Recognition Program® and many unit-level initiatives provide significant organizational impact. (See Expanding influence.) The American Association of Critical-Care Nurses has promulgated a well-established definition of a healthy work environment and created evidence-based standards that established the Beacon Award for Excellence. Other similar programs include the Emergency Nurses Association’s Lantern Award and the Academy of Medical-Surgical Nurses’ PRISM Award®. Expanding the impact of these standards offers opportunities to focus organizational attention and resources to benefit all clinicians.
The design of any intervention to prevent and reduce burnout and promote professional well-being must align with organizational values such as respect, justice, compassion, and diversity. What we know about large-scale change is that initiatives devoid of a grounding in core values are likely to fail. Start by examining how your organization’s values show up within its system, processes, and decisions related to clinician well-being. You may find that they have been applied only to patients, with less attention to living those values in the workplace. From this new perspective, work with other leaders in the organization to design solutions anchored in its values and to recognize patterns that may contribute to or undermine their success.
Goal 2: Create positive learning environments
The work environment can have an impact on new nurses’ resilience, sustainability in the workforce, and clinical performance during training. Nursing students, like other learners, thrive when they learn the skills they need to sustain themselves in their careers. Collaborate with other nurse leaders and educators to develop academic-practice partnerships that integrate clinical practice realities with meaningful contributions to patient care while students learn. Academic infrastructure investment that supports learner well-being also must prioritize faculty and staff well-being and intentionally dismantle factors that contribute to burnout. Evaluating the learner in team competencies that support a healthy culture is another addition both for education and nurse residencies. By doing these things, organizations can be one step closer to having psychologically safe cultures where help-seeking is the norm and not stigmatized because of fear of speaking up or asking questions.
In response to data about burnout and other indicators of clinician stress and distress, nurses have taken seriously their ethical mandate to be wise stewards of their own integrity and personal resources and to positively contribute to ethically sound and healthy work environments. The search for positive nursing cultures that prevent nurse turnover was the genesis of the classic study by McClure and colleagues, published in 1983, which identified the characteristics of organizations that lead to better nurse recruitment and retention through the professional practice environment. The findings led to the creation of the Magnet® program. Today, the American Nurses Credentialing Center Magnet Recognition Program® serves as a blueprint for positive work environments, and nurse leaders should consider the impact of nursing interventions on other clinicians and the overall healthcare work environment. Reports show positive outcomes for physician engagement when comparing hospitals that have received Magnet recognition to those that haven’t. In Magnet-recognized hospitals, most patient care systems are led by nurses, and the leadership nurses provide influences and impacts the entire organization.
Nurses can leverage their influence by working across disciplines to lead authentically, practice shared decision making, and create a culture of autonomy and dialogue that respects direct caregivers’ knowledge and capability. The result will be individual strategies aimed at fostering resilience and well-being coupled with systemic solutions that remove impediments.
Goal 3: Reduce administrative burden
Explore the rationale for adopting policies that add to nurses’ administrative burdens, and talk with staff about what matters to them most and what gets in the way of effective nursing practice. In addition, evaluate whether the organization has adopted a minimal dataset for nursing documentation that ensures nurses are required to document only what’s minimally required for safe patient care.
Goal 4: Enable technology solutions
Evaluate whether technology is optimized regularly. When organizations invest in systems that support patient safety, clinical nurses must evaluate workflows before implementation to ensure that they can be integrated into clinical practice. In addition, consider when technology might help alleviate stress by alerting nurses to critical patient changes or repeat testing. The functionality of technology must improve to reduce nursing cognitive burden by designing systems that complement nursing practice and aid in improving patient surveillance.
Goal 5: Provide support
Nurses pride themselves on being able to cope with whatever is put in front of them. However, all adaptive systems (and individuals) have limits. Work to transform asking for help from a sign of deficiency and incompetence to one of insight and wisdom. Cultures of blame and shame limit progress.
Nurse leaders can ask state boards of nursing whether they’ve adopted the most recent evidence about required licensure reporting of treatment for depression and emotional problems. Guidance instructs boards to inquire only about current impairment (not past treatment) to minimize nurses’ inhibition to seek and receive help.
Goal 6: Invest in clinician well-being research
Bring together researchers and nurse scientists to focus on measuring and improving clinician well-being. Many of the nursing studies included in the National Academies’ report are cross-sectional; longitudinal studies are needed to fully evaluate current programs. And a broader understanding of the impact of information technology on nurse well-being can inform future electronic health record system designs. Most of the nursing workforce is made up of millennials, so consider their unique experiences. What creates burnout and well-being in this population? Are our current measurement tools valid across all generations? What could be learned that we don’t already know?
Be bold
Improving clinician well-being requires bold vision and leadership. Nurses have a history of creating and maintaining positive work environments, and the National Academies’ report provides additional direction for expanding and influencing interprofessional improvement that focuses on patients, families, and clinicians. Burnout is complex and multilayered, but organizational systems that help nurse leaders facilitate teamwork, collaboration, autonomy, communication, professionalism, and adequate resources can revitalize a workplace. The result is meaningful, purposeful work that delivers value to patients.
Sharon Pappas is chief nurse executive at Emory Healthcare in Atlanta. Cynda Rushton is the Anne and George L. Bunting Professor of Clinical Ethics at the Berman Institute of Bioethics and School of Nursing Johns Hopkins University at Baltimore.
References
Aiken LH, Clarke SP, Sloane DM, Sochalski J, Silber JH. Hospital nurse staffing and patient mortality, nurse burnout, and job dissatisfaction. JAMA. 2001;288(16):1987-93.
American Nurses Association (ANA). Code of Ethics for Nurses with Interpretive Statements. 2nd ed. Silver Spring, MD: ANA; 2015. nursingworld.org/practice-policy/nursing-excellence/ethics/code-of-ethics-for-nurses/coe-view-only
American Medical Association. AMA Principles of Medical Ethics. ama-assn.org/sites/ama-assn.org/files/corp/media-browser/principles-of-medical-ethics.pdf
Dempsey C, Lee TH. How great nursing improves doctors’ performance. Harvard Business Review. May 22, 2019. hbr.org/2019/05/how-great-nursing-improves-doctors-performance
Halter MJ, Rolin DG, Adamaszek M, Ladenheim MC, Hutchens BF. State nursing licensure questions about mental illness and compliance with the Americans with Disabilities Act. J Psychosoc Nurs Ment Health Serv. 2019;57(8):17-22.
Institute for Healthcare Improvement. “What matters to you?” Conversation guide for improving joy in work. ihi.org/resources/Pages/Tools/Joy-in-Work-What-Matters-to-You-Conversation-Guide.aspx
Maslach C, Schaufeli WB, Leiter MP. Job burnout. Annu Rev Psychol. 2001;52:397-422.
McClure ML, Poulin MA, Sovie MD, Wandelt M; American Academy of Nursing, Task Force on Nursing Practice in Hospitals. Magnet Hospitals: Attraction and Retention of Professional Nurses. Kansas City, MO: American Nurses Association; 1983.
McHugh MD, Kutney-Lee A, Cimiotti JP, Sloane DM, Aiken LH. Nurses’ widespread job dissatisfaction, burnout, and frustration with health benefits signal problems for patient care. Health Aff. 2011;30(2):202-10.
Moss M, Good VS, Gozal D, Kleinpell R, Sessler CN. An official Critical Care Societies collaborative statement: Burnout syndrome in critical care healthcare professionals: A call for action. Crit Care Med. 2016;44(7):1414-21.
National Academy of Medicine, National Academies of Sciences, Engineering, and Medicine. Taking Action Against Clinician Burnout: A Systems Approach to Professional Well-Being. Washington, DC: The National Academies Press; 2019.
Rushton CH, Caldwell M, Kurtz M. Moral distress: A catalyst in building moral resilience. Am J Nurs. 2016;116(7):40-9.
World Health Organization. 2019. QD85:Burn-out an “occupational phenomenon”: International Classification of Diseases. who.int/mental_health/evidence/burn-out/en/




















1 Comment.
Greetings from a 40+ year nurse.
Nurses become nurses because they like to care for patients. In the world of nursing today ,care is on the back burner and nurses nurse their computers and have so many documentation requirements ,that can become the focus. the 12 hour shifts which seem convenient for both the hospital and nurses have had major impacts on patient care. Primary nursing as it was practiced in the past is non existent. With nurses only working 3 days a week to get to know their patients and be able to observe subtle changes that can lead to problems down the line are less likely. When nurses worked 8 hour shifts there was more time to develop relationships with your co workers and that lead to team building. Developing close personal relationships is one of the reasons nurses will continue to work on the same unit. You know who has your back. My daughter is one year out of school. She works on a tele floor and her assignment is 6 patients every day. She only has one nurse that has been on the floor longer than she has. She has no one to mentor her and help her grow as a professional. Sometimes she is the charge nurse and still carries a 6 patient assignment. Hospitals don’t seem to understand that nurses that are able to care for their patients in a safe environment with a reasonable nurse patient ratio ,stay at their jobs and the patients get better care.