A complete skin tear program benefits patients, staff, and organizations.
Takeaways:
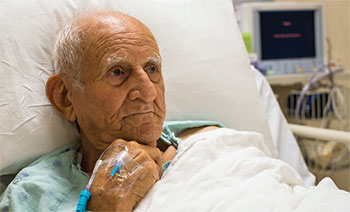
- Skin tears are a common and painful reality for the elderly.
- Skin tear risk assessment is key to prevention.
- Proper skin tear assessment and management promotes uncomplicated healing.

Wound care: Five evidence-based practices
A guide for adhesive removal: Principles, practice, and products
As you carefully peel away the dressing, you notice the gauze is stuck to the wound in several places, which causes bleeding. Mr. Brown cries out in pain. You use sterile saline to moisten the area and continue with removal. Once the dressing is off, you discover a large open wound with bruising and redness along the edges and a flap of skin bunched together at the proximal end. You know the wound would be in better condition if the flap had been repositioned over the wound bed when it was first assessed and dressed. Now, using saline to keep the area moist, you reposition the flap as much as possible. You plan to consult the wound care nurse to assess the flap for viability and possible debridement.
Skin tears in the elderly
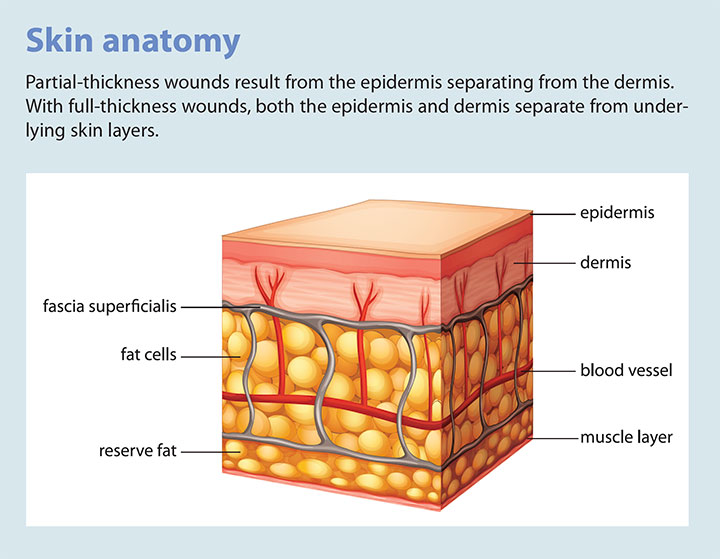
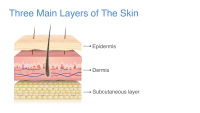
The International Skin Tear Advisory Panel (ISTAP) defines a skin tear as “a wound caused by shear, friction, and/or blunt force resulting in separation of skin layers.” ISTAP expands the definition by describing the difference between partial thickness (the epidermis and dermis are separated) and full-thickness wounds (the epidermis and dermis are separated from underlying skin structures). (See Skin anatomy.)

Skin tears are a frequent and painful reality for the elderly. A 1991 epidemiological study estimated that as many as 1.5 million skin tears occur in institutionalized residents in the United States every year. A 2013 study of the prevalence of skin tears in a Canadian LTC facility demonstrated a 22% prevalence. A study in Japan looked at elderly residents in a long-term medical facility. Over a 3-month period, 14 of 368 residents developed skin tears, a cumulative incidence rate of 3.8%.
Risk assessment and prevention
As part of Mr. Brown’s admission process, you perform a skin tear risk assessment. You note that he has several risk factors, including age, chronic disease, fragile skin, history of falls, history of previous skin tear, impaired mobility, and the need for an assistive device. You determine Mr. Brown is at high risk for skin tears, communicate this to the interprofessional treatment team, and implement a skin tear prevention plan.
The first step in preventing painful skin tears is risk assessment, using tools such as:
- Skin Integrity Risk Assessment Tool—This checklist includes 24 skin tear risk factors, divided into three categories. Based on the number of positive responses in each category, a risk reduction program is implemented. You can access an adapted version of this tool.
- ISTAP—The three categories included in this skin tear risk assessment tool include general health, mobility, and skin. This tool is available online.
Multiple intrinsic and extrinsic factors make older patients susceptible to skin tears, and, as with pressure injury and fall risk assessments, the goal of skin tear risk assessment is to identify factors that are amenable to prevention. (See Risk factors and the elderly.) For example, as we age (an intrinsic risk factor), several changes occur in the skinthinning of the dermal and epidermal layers and decreased sebum and sweat gland function—that increase skin tear risk. And the need for assistance with activities of daily living (an extrinsic risk factor) increases the chance of injury that may result in a skin tear. Many extrinsic risk factors can be reduced through modifications and other preventive measures.


Prevention
When developing a prevention plan based on your risk assessment, include all identified extrinsic risk factors, such as dependence on assistive devices and bathing habits. (See Skin tear prevention strategies.) For example, frequent bathing and using alkaline soap strips away natural lubricants and disrupts the acid mantle meant to protect the skin. To combat dry skin and prevent tears, decrease bathing frequency from daily to every other day, and use pH-neutral soaps. The incidence of skin tears in a Western Australian LTC facility was reduced by almost 50% when a twice-daily application of a pH-neutral moisturizer was implemented.
Include staff education as an integral part of your prevention program. Important components include information about skin anatomy, aging skin, skin tear risk factors, and safe patient handling.


Skin tear assessment
Three weeks after admission, a nursing assistant (NA) reports an injury to Mr. Brown’s left arm. The injury occurred when Mr. Brown lost his balance transferring with a walker from his bed to a chair. When the NA reached for his arm to help, Mr. Brown’s skin tore “like paper.” On assessment, you note minimal bleeding that you’re able to control with gentle pressure. You clean the wound and reposition the skin flap. You estimate that approximately 40% of the skin flap is missing and document it as a type 2 skin tear. You want to prevent infection, minimize trauma to the wound and surrounding skin, and optimize your time.
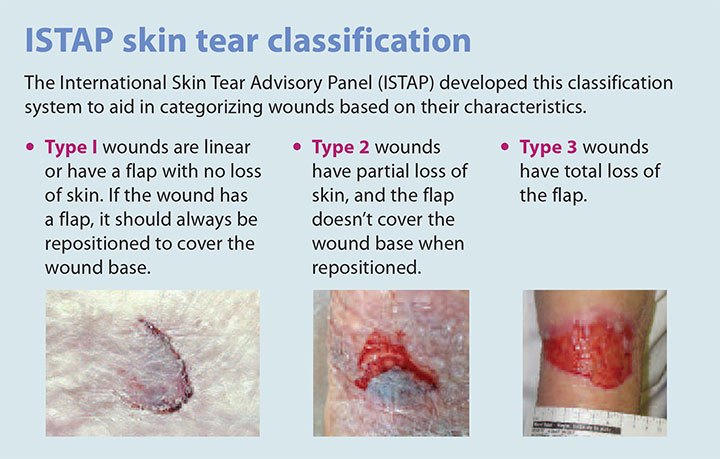
The most commonly used tool for skin tear classification is the ISTAP system (See ISTAP skin tear classification.) Using this system, you can categorize skin tears based on wound characteristics, including the presence and condition of the skin flap.

Skin tear management
As you assess Mr. Brown’s skin tear, you begin to formulate a management plan, following the same evidence-based principles used to treat pressure injuries but with a few additional best practices:
- Approximate skin flap back into place, if possible.
- Avoid using wound closure strips, hydrocolloids, and transparent films.
- Remove dressings in the same direction as the flap.
- On the outside of the dressing, illustrate the flap with an arrow indicating the direction of dressing removal.
You remove debris using normal saline (your other option is a nonionic wound cleanser) and then apply the dressing. Your dressing choice is based on the wound’s characteristics. (See Skin tear dressing options.)
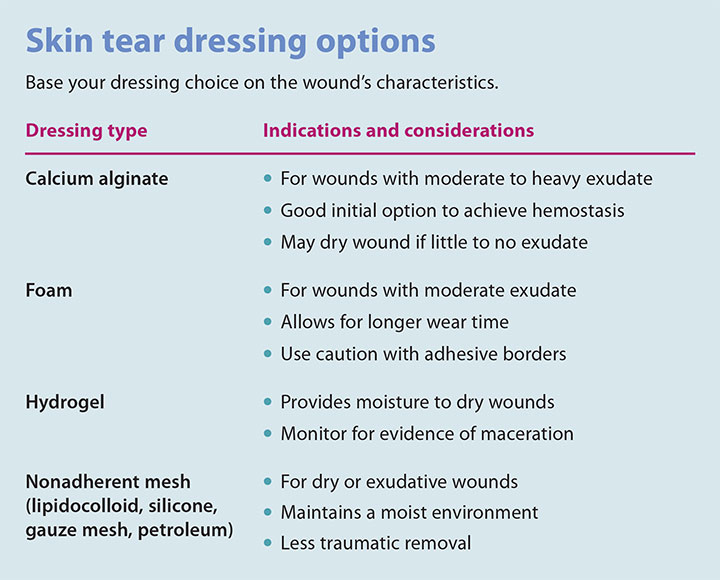

The goal of wound management is to maintain a moist environment, control exudate, and minimize pain. You also want to prevent infection, minimize trauma to the wound and surrounding skin, and optimize your time. The ISTAP tool kit includes a product selection guide to help you make the best dressing choice.
Additional best practices include reapproximating the skin flap and protecting it during subsequent dressing changes. (See Repositioning and protecting.)
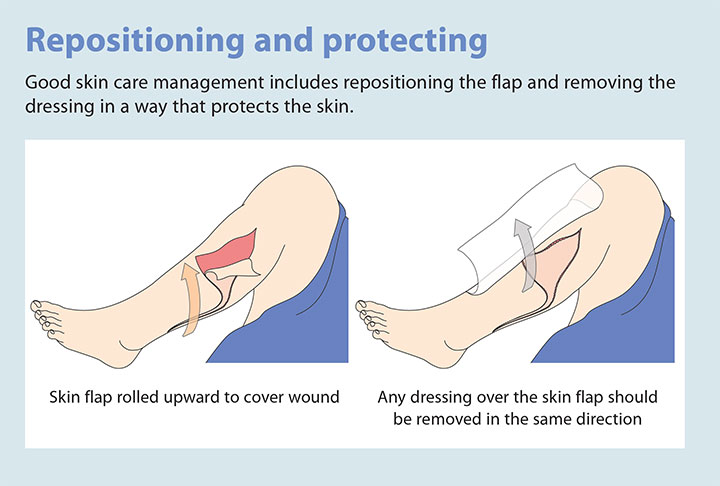

Best outcomes
Mr. Brown’s skin tear is dressed using a hydrophilic polyurethane foam pad. Dressing changes occur on days 3, 7, 11, and 14. On day 14, you note that the skin tear has healed without complications.
Mr. Brown’s experience is an excellent example of how a skin tear program that includes risk assessment, prevention, assessment and documentation tools, and management strategies can benefit everyone—residents avoid painful skin tears and nursing staff gain confidence in caring for skin tears and decrease their workload when skin tears are prevented. In addition, LTC facility costs decrease, and the public’s perception of quality care increases.
Joanne Laggan Davis is an adult nurse practitioner in geriatrics/extended care at Tuscaloosa Veteran Affairs Medical Center in Tuscaloosa, Alabama.
Selected references
Carville K, Leslie G, Osseiran-Moisson R, Newall N, Lewin G. The effectiveness of a twice-daily skin-moisturising regimen for reducing the incidence of skin tears. Int Wound J. 2014;11(4):446-53.
Koyano Y, Nakagami G, Iizaka S, et al. Exploring the prevalence of skin tears and skin properties related to skin tears in elderly patients at a long-term medical facility in Japan. Int Wound J. 2016;13(2):189-97.
LeBlanc K, Christensen D, Cook J, Culhane B, Gutierrez O. Prevalence of skin tears in a long-term care facility. J Wound Ostomy Continence Nurs.2013;40(6):580-4.
LeBlanc K, Baranoski S, Christensen D, et al. The art of dressing selection: A consensus statement on skin tears and best practice. Adv Skin Wound Care. 2016;29(1):32-46.
LeBlanc K, Baranoski S, Holloway S, Langemo D. Validation of a new classification system for skin tears. Adv Skin Wound Care. 2013;26(6):263-5.
LeBlanc K, Baranoski S; Skin Tear Consensus Panel Members. Skin tears: State of the science: Consensus statements for the prevention, prediction, assessment, and treatment of skin tears. Adv Skin Wound Care. 2011; 24(suppl 9):2-15.
LeBlanc K, Woo K, Christensen D. et al. Best practice recommendations for the prevention and management of skin tears. 2018.
Malone ML, Rozario N, Gavinski M, Goodwin J. The epidemiology of skin tears in the institutionalized elderly. J Am Geriatr Soc. 1991;39(6):591-5.
Focus 0n Wound Care












3 Comments.
I have a category 3 skin tear on my shin, will it leave a scar once healed and how long will it sting for too ?
I really liked it and got such many essential information from this. Thanks for such a fabulous blog.
Thanks for this blog, having such knowledge regrading skin treatment is very crucial.