Combining skill and knowledge ensures safe removal.
Takeaways:
- Improve your knowledge on how to remove medical tape or wound dressings
- Discover products and strategies to ease the tape removal experience for your patients


Who’s at risk for MARSI?
Wound care: Five evidence-based practices
Moisture-associated skin damage: The basics
| Patients with fragile or delicate skin are at risk for medical adhesive–removal skin injury (MARSI). These patients will have a weakened connection between skin layers that may be injured when pressure-sensitive adhesives are removed. Before beginning removal, consider these patient factors: • Newborns—The connection between the epidermis and dermis is weaker than in adults. • Older adults—As people age, the skin structure weakens and loosens, resulting in separation of the skin layers upon adhesive removal. • Medications—Some drugs, such as corticosteroids, can cause thinning of the skin, which increases a patient’s risk for MARSI and delayed healing. • Malnutrition and dehydration—Patients who are malnourished or dehydrated may have weakened skin integrity. |
Our understanding of PSAs and their removal can help prevent harm and patient anxiety. This article will look at the qualities of PSA adhesives and backings, explain the principles of removal, and discuss products that aid removal.
PSA adhesives and backing
The skin’s surface qualities—moisture, hair, oil, and shedding dead cells—make PSA adhesion challenging. PSAs are designed to overcome these challenges, while balancing successful adherence and easy removal. Both the adhesive side of the PSA as well as its backing material play a role in adherence and removal.
Adhesive
Acrylate, silicone, and hydrocolloid are three commonly used adhesives. They each work in different ways. (See Comparing adhesives.)
As acrylate adhesive warms, it fills in the skin’s rough surfaces. Many medical tapes and some dressings contain acrylate with varying levels of adhesion, making some easier to remove than others. Some strongly adhering acrylates place patients at risk for MARSI.
Silicone adhesives—found in wound dressings and tape—adhere to the rough surfaces of the skin at initial application. This low-energy connection separates easily from the skin. Because it easily detaches, silicone PSAs aren’t appropriate when adhesion is critical, such as when securing an endotracheal tube.
The adhesion of hydrocolloid products increases with time, creating the same level of risk for MARSI as a well-adhered acrylate. Detachment requires a combination of manipulating the PSA backing and dissolving the adhesive.
Comparing adhesives
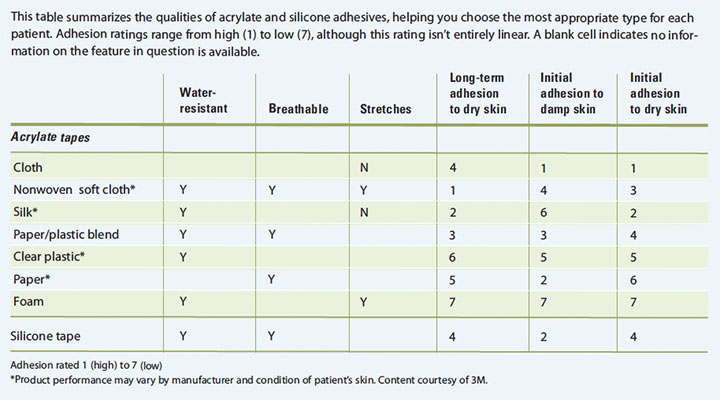

Backing
PSA backing materials also affect removal. To separate the PSA adhesive from the skin, we have to distort the backing by stretching or pulling. The challenge with stretching, however, is our ability to maintain directional control. In the presence of hair, a wound, or a catheter, we don’t want to cause discomfort, distortion, or dislodgment. Consequently, the removal procedure we select includes assessing both the adhesive and backing of the PSA as well as the presence of any object we don’t want to disturb.
Register today for American Nurse Journal’s free OnDemand webinar on Dermal Damage Control: Managing medical device-related skin injuries.
Principles of PSA removal
You have two options for PSA removal: low and slow or distortion. With low and slow, pull back the PSA at a low horizontal angle, away from the corner or edge, separating it from the skin. Distortion requires stretching the PSA backing to shear the adhesive from the skin. However, PSA removal is more than selecting one of two procedures; it requires understanding the core principle of supporting the skin while correctly detaching the product.
Skin is a soft and flexible organ that moves and bends in the direction we pull. Pulling off a PSA at a vertical angle creates the greatest force, but it may injure skin and distort a healing incision. Consequently, you must support the skin with your hands by anchoring the adhesive on the dressing (when stretching) or the newly exposed skin (when peeling back). A low angle of peel requires less force to separate adhesive from skin, which you accomplish with either procedure by keeping the PSA low and close to the surface. The goal is to avoid MARSI by minimizing the amount of force needed for detachment.
Adhesive-removal products
Silicone-based adhesive-removal products are the best option for aiding PSA removal. They evaporate, leave no residue on the skin, and are not noted for causing dry skin. If you don’t have access to silicone-based products, other options include water, alcohol, or emollients. Understanding the pros and cons of each will help you choose the right solution.
Water may be easily accessible, but it can weaken water-permeable PSA backings, separating them from the adhesive but not affecting its connection to the skin, leaving behind a sticky residue. Alcohol, on its own or combined with an antiseptic like chlorhexidine, can solubilize an adhesive, making it easier to detach. However, alcohol evaporation causes vasoconstriction and dries the skin. In contrast, emollients, such as mineral oil or lotions, facilitate separation of adhesive from the skin, causing no harm. Unfortunately, emollients may separate the adhesive from the backing and leave a sticky residue.
To ensure successful use of adhesive-removal products, follow product instructions. For example, an adhesive-removal product made with an odorless mineral spirit can effectively dissolve the adhesive for pain- and injury-free removal. However, if you don’t follow the product instructions to wash off any remaining product with soap and water, the patient’s skin may dry and crack.
Removal products aren’t appropriate in all cases. For example, they may be contraindicated in the presence of dermal glue or in close proximity to an incision.
| Case study: Low and slow prevents injury Joe Roberts, a 60-year-old man with type 2 diabetes, is ready for discharge from the hospital. His nurse, Alice, must first discontinue his peripheral intravenous (PIV) catheter. Mr. Roberts is eager to leave and asks Alice to hurry. Alice notes that the cannula is well secured with a transparent polyurethane dressing. Mr. Roberts’ skin is dry and loose. During shift handoff, Alice learned that Mr. Roberts has peripheral neuropathy. She understands that removal of the PIV will require knowledge and skill to prevent MARSI. As with removal of any PSA, the first edge is the most challenging. Alice chooses to use an adhesive-removal product. Because transparent polyurethane dressings are water-resistant, Alice applies the removal product liberally, gently detaching a corner of the dressing from the skin. When she has the edge of the dressing in her hand, she pulls it back low and slow. This technique gives Alice greater control and allows her to continue applying adhesive remover, while supporting Mr. Roberts’ skin. She removes the dressing from the edges toward the catheter, working with the direction of hair growth. When Mr. Roberts grows impatient with the slow progress, Alice takes the opportunity for patient education, explaining that her approach to removing the PSA will prevent a skin wound that may be slow to heal because of his diabetes. |
| Case study: Alleviating patient anxiety Nine-year-old Emily Gray arrives in the emergency department for evaluation of a head laceration. Before assessment can begin, David, the emergency department nurse, must remove a large plastic bandage from Emily’s forehead. Emily fearfully anticipates its removal.David recognizes that the acrylate adhesive foam-backed bandage, placed an hour ago, may not have adhered well to the skin. However, he realizes that sharing this logic may do nothing to alleviate Emily’s anxiety.To make sure removal of the bandage goes as smoothly as possible, David decides to use a removal aid. He chooses lotion because he doesn’t have access to products specifically designed for adhesive removal. With patience and slow removal, he eases the bandage off. David then cleanses the skin to remove any remaining lotion. This pain-free bandage removal may help Emily feel less anxious about similar situations in the future. |
Combine knowledge and skill
PSA removal is a combination of skill and knowledge. No single solution fits every patient or care environment, so understanding the qualities of various PSAs, the principles of removal, and the pros and cons of removal products helps ensure safe removal.
Ann-Marie Taroc is a staff nurse at Seattle Children’s Hospital in Seattle, Washington.
Selected references
Czech Z, Kowalczyk A, Swiderska J. Pressure-sensitive adhesives for medical applications. In Akyar I, ed. Wide Spectra of Quality Control. Rijeka, Croatia: InTech; 2011; 309-32.
Denyer J. Reducing pain during the removal of adhesive and adherent products. Br J Nurs. 2011;20(15):S28, S30-5.
Konya C, Sanada H, Sugama J, et al. Skin injuries caused by medical adhesive tape in older people and associated factors. J Clin Nurs. 2010;19(9-10):1236-42.
Matsumura H, Ahmatjan N, Ida Y, Imai R, Wanatabe K. A model for quantitative evaluation of skin damage at adhesive wound dressing removal. Int Wound J. 2013;10(3):291-4.
Matsumura H, Imai R, Ahmatjan N, et al. Removal of adhesive wound dressing and its effects on the stratum corneum of the skin: Comparison of eight different adhesive wound dressings. Int Wound J. 2014;11(1):50-4.
McLafferty E. (2012). The integumentary system: Anatomy, physiology and function of skin. Nurs Stand. 2012;27(3):35-42.
McNichol L, Lund C, Rosen T, Gray M. Medical adhesives and patient safety: State of the science: Consensus statements for the assessment, prevention, and treatment of adhesive-related skin injuries. J Wound Ostomy Continence Nurs. 2013;40(4):365-80.
Reevell G, Anders T, Morgan T. Improving patients’ experience of dressing removal in practice. J Community Nurs. 2016;30(5):44-9.
Salmanoğlu M, Önem Y. Diabetic foot: Even the most innocent may turn into a threat. Euro J Gen Med. 2014;11(2):117-8.
Taroc A. Staying out of sticky situations: How to choose the right tape for your patient. Wound Care Advisor. 2015;4(6):21-6.
van Schaik R, Rövekamp MH. Fact or myth? Pain reduction in solvent-assisted removal of adhesive tape. J Wound Care. 2011;20(8):380-3.



















9 Comments.
If only all health care workers would learn and/or apply this. Adhesion to skin is one thing. Hair is another. Most do not use adhesive removers. And a common procedure is to just pull hard and fast, “ripping” it off.
Thank you for such a detailed article. I need to remove my own shoulder surgery dressing and will try to soften it up with mineral spirits. Last year the dressing on my other shoulder required 2 nurses (4 hands) to remove and was very painful. (The oil method reminds me of how I take labels off perscription bottles – soak it in oil for awhile and it slides right off.)
thanks for the information
I used this adhesive removal bandages many times and believe me it is really easy to apply and remove. Thanks for this post.
Really appreciate your writing style. I loved it. You defined each and everything about Adhesive Tapes so clearly, in brief, thanks for this post.
Thanks for the tip to follow product instructions when handling adhesive-removal products. I am going to need some adhesive remover for a science project that my son is doing. Because handling this kind of material could cause the skin to dry and crack, as you mentioned, I will be sure to handle it properly to ensure a successful science project.
This is something amazing I’ve read today. even I’ve ordered wound care products from an online website named Wound care. even I’ve ordered wound care products from an online website named Wound care.
I read your blog. This quite informative and interesting. Thanks for this post.
A bandage should be easy to apply and do not cause too much pain removal. Therefore, I use Slimfast tubular bandages as it has both these qualities.