Follow evidence-based guidelines to target individual care needs.
- Using body mass index as an indicator for type 2 diabetes is now considered inaccurate, especially among Asians, who tend to develop the condition with normal BMIs.
- In 2019, compared to Whites, Blacks, and Hispanics, Asian Americans had the highest percentage of undiagnosed diabetes.
- The U.S. Department of Health and Human Services monitors the ABCs of prevention: A1C, blood pressure, cholesterol, and smoking.
When Claire Moy*, a 38-year-old Filipina, has her annual physical, she’s surprised when her primary care provider tells her that her hemoglobin A1C level is 7.2% and her fasting blood sugar is 177 mg/dL. Ms. Moy reports gaining 6 pounds in the last 8 months, but her body mass index (BMI) is 24 kg/m2. Her blood pressure (BP) is 153/90 mmHg.
Patient-centered medication selection for type 2 diabetes
The prescription for type 2 diabetes: Encouraging exercise engagement
Early, intensive therapy for type 2 diabetes can slow progression
Common nonmodifiable risk factors for diabetes include family history and ethnicity; modifiable risk factors include obesity, sedentary lifestyle, and diets high in fat and calories. Traditionally, a BMI greater than 30 kg/m2, an indicator of obesity, is considered a risk factor for type 2 diabetes. However, using the BMI as a primary indicator is now considered inaccurate, especially among Asians (including those with origins in East Asia, Southeast Asia, and South Asia), who tend to develop type 2 diabetes with normal BMIs. This may be because BMI fails to take into account fat and lean tissue proportions and distribution. In studies conducted throughout Asia and observations by U.S. clinicians, Asians with type 2 diabetes don’t meet the clinical criteria for the disease.
An understanding of the unique features of type 2 diabetes among Asian Americans can help nurses better care for patients by individualizing education and self-management recommendations.
Type 2 diabetes and Asian Americans
Asian Americans are the fastest growing ethnic minority group in the United States. Based on 2019 estimates, 18.9 million Asian Americans live in the United States. In 2019, according to the Department of Health and Human Services, compared to Whites, Blacks, and Hispanics, Asians had the highest percentage (4.6%) of undiagnosed diabetes. Although the annual rate of new cases of diabetes among U.S. adults has decreased overall, cases among Asian Americans have risen. According to the Centers for Disease Control and Prevention (CDC), between 2013 and 2018, the percentage of Asian adults with diabetes increased from 8.0% to 9.2%, with an age-adjusted percentage rate of 11.4% compared with 8% among non-Hispanic White adults.
Asians and Asian Americans are heterogeneous groups. Disaggregated data from the CDC show that, among non-Hispanic Asians, Asian Indians (12.6%) and Filipinos (10.4%) had the highest prevalence of diabetes, followed by Chinese (5.6%). Data from the 2003–2011 California Health Interview Survey showed that, compared to non-Hispanic Whites, age at diagnosis for Filipinos, Koreans, South Asians, and Vietnamese was 8.4 years, 4.2 years, 10.5 years, and 8.7 years earlier, respectively. Earlier age at diagnosis has been attributed to molecular predisposing factors, genetic nucleotide polymorphisms affecting fat mass and obesity, and lower levels of adiponectin (a protein that regulates glucose levels) among Asians, compared with Whites with similar BMIs.
BMI, an indirect measure of body fat based on height and weight of adults, is calculated using a person’s weight in kilograms divided by the square of their height in meters. High BMI has been correlated with higher all-cause mortality, primarily due to cardiovascular complications. Studies indicate that elevated BMI isn’t an accurate predictor of type 2 diabetes among Asians because they’re frequently diagnosed with the condition when they have a normal BMI (between 18.5 and 24.9). (See The role of visceral fat.)
Pathophysiology
The exact cause of diabetes remains unknown, but the main pathophysiologic features of type 2 diabetes is relative insulin deficiency caused by dysfunction of the pancreatic β-cell and insulin resistance in target organs. Obesity (BMI ≥30) and overweight (BMI between 25.0 and 29.9) are major risk factors for type 2 diabetes. Elevated BMI is associated with the release of inflammatory markers that lead to insulin resistance. Both type 1 and type 2 diabetes are polygenic inherited diseases, in which the condition results from the interaction of many genes and their variants, as opposed to a single gene expression. Individuals with type 2 diabetes frequently are overweight, obese, or average weight with visceral fat distribution.
Signs and symptoms
Asians with type 2 diabetes have the same pathognomonic signs (such as polyuria and polydipsia) as other races and ethnicities. These signs result from hyperglycemia, which causes osmotic diuresis and cellular dehydration. Polyphagia results from intracellular glucose deficiency. Other signs and symptoms of type 2 diabetes include fatigue, delayed wound healing, recurrent infections, numbing or tingling of the extremities, and blurry vision.
Screening and diagnosis
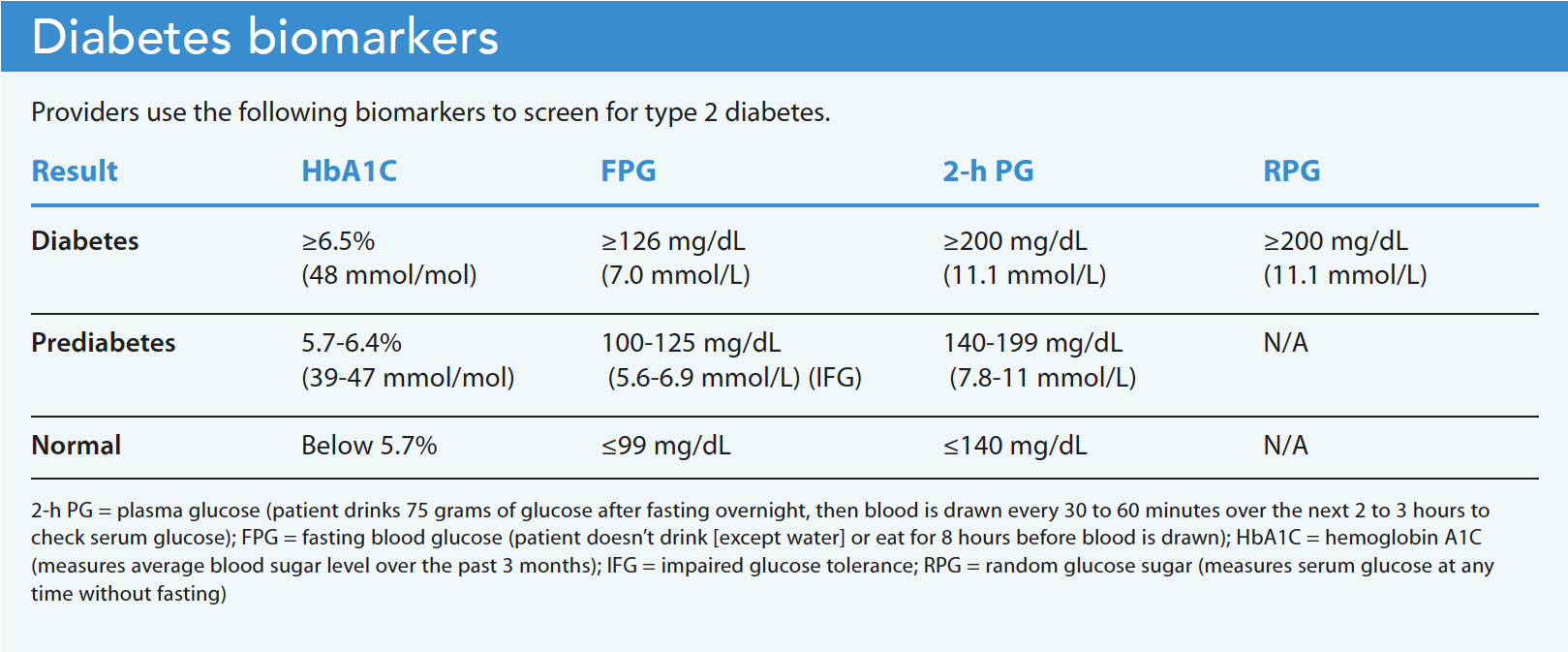
Individuals at risk for type 2 diabetes should receive routine screening to promote early diagnosis and avert the cascade of potentially catastrophic cardiovascular events. The U.S. Preventive Services Task Force recommends that asymptomatic adults between 35 and 70 years who are overweight or obese receive screening for prediabetes and type 2 diabetes. The American Diabetes Association (ADA) recommends type 2 diabetes screening for everyone starting at age 45, any adult with a BMI ≥25, and Asians of any age with a BMI ≥23. The ADA also recommends testing for prediabetes or type 2 diabetes in women who are overweight or with obesity who are planning to get pregnant. (See Diabetes biomarkers.)
On average, non-Hispanic Whites are diagnosed with type 2 diabetes at 55.7 years. Asian Americans tend to be diagnosed at younger ages. In a study by Becerra and Becerra, South Asians had the earliest age at diagnosis (44.9 years), followed by Vietnamese (46.7 years), Filipinos (47 years), Koreans (51.2 years), and Chinese (52.9 years).
Treatment
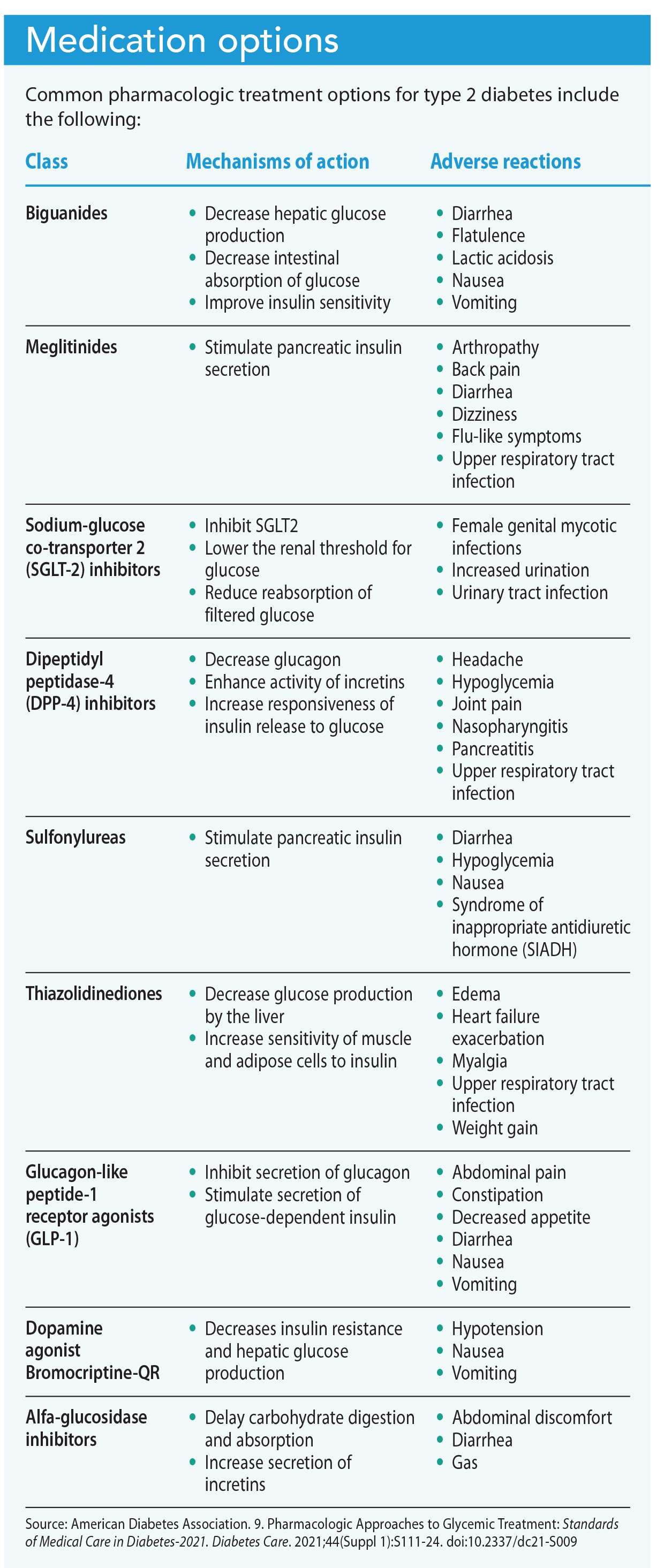
The latest ADA standards recommend metformin as the initial pharmacologic agent to treat type 2 diabetes. If the A1C goal of <7% for nonpregnant adults isn’t achieved after 3 months, metformin can be combined with other agents. (See Medication options.)
Patient education
Use the teach-back method when educating patients who’ve been diagnosed with type 2 diabetes. Linguistically appropriate teaching materials (sixth-grade or lower reading level) should be made available as well as medical interpreters when necessary. Emphasize blood sugar self-monitoring, complication surveillance, the importance of regular follow-up visits with providers, diet and exercise, foot care, medication interactions, and hypoglycemia management. Make the patient or caregiver aware of the manifestations of hypoglycemia (tremors, diaphoresis, tachycardia, headaches, and confusion) and know how to manage them.
ABCs of prevention
The U.S. Department of Health and Human Services monitors the ABCs of prevention (A1C, blood pressure, cholesterol, and smoking). Current data indicate that only 19.2% of Americans with diabetes are meeting the ABC goals. Every patient encounter should focus on risk assessment and helping patients achieve their treatment goals with lifestyle modifications related to exercise, diet and weight, and hypertension management.
Exercise
Most Asians appear slim and lean. Given the public health emphasis on the connection between being overweight and type 2 diabetes, many Asians with normal BMIs may not feel an urgency to exercise. However, for the average adult, the U.S. Department of Health and Human Services recommends 150 minutes of moderate or 75 minutes of vigorous aerobic activity per week. Examples of moderate activity include swimming or brisk walking; vigorous activity includes running or dancing. In addition, the department recommends strength training using weight machines or resistance bands at least twice per week.
The impression that Asians are better at exercising is influenced by the idealized image of Asians doing Tai Chi in public parks. However, this doesn’t match research data. A study by Yi and colleagues found that only 43% of Asians living in New York City and 56% of those living in Los Angeles meet the recommended exercise guidelines compared with 61% (New York City) and 64% (Los Angeles) of their non-Hispanic White counterparts.
Diet
Hypertension and uncontrolled diabetes are closely associated. The U.S. Department of Agriculture and the U.S. Department of Health and Human Services recommend sodium intake for adults of 2,300 mg/day. Compared with other racial and ethnic groups, Asians consume more sodium. A study by Firestone and colleagues evaluating dietary sources of sodium by ethnicity found that Asian Americans have a higher sodium density than adults of other racial or ethnic groups. The study also found that among the top 10 dietary sources of sodium in Asians, six are unique to Asian cuisine. They include rice, stir-fry and soy-based mixtures, fish, fried rice and lo/chow mein, and soy-based condiments. These findings highlight the importance of culturally congruent, targeted patient education and motivational interviewing. For example, nurses can ask, “How would you like things to be different after knowing your diagnosis?” “What have you tried before to make a change?” and “Help me understand your experience with diabetes.”
Nurses and other healthcare providers should note that acculturation to the dominant culture might expose Asian immigrants to dietary risks. For example, those living in Western countries may consume a high-calorie and high-fat diet associated with that country’s cuisine.
After Ms. Moy’s diagnosis with type 2 diabetes, her provider prescribes metformin 500 mg twice daily. Ms. Moy resumes her gym membership, checks her blood sugar once a day, reduces her salt intake, and monitors herself for signs of hypoglycemia and adverse drug effects. At her 3-month follow up, Ms. Moy’s HbA1C is 6.5%, her BP is 130/80 mmHg, and her BMI is 22.
Play your role
For years, the inclusion of race in diagnostic algorithms has generated controversy. Some health differences among minority populations are linked to socioeconomic factors and racism in medicine, rather than genetics. Nurses play an important role in reducing healthcare inequities.
Evidence regarding type 2 diabetes among Asian Americans requires a contextualized application of screening guidelines. The ADA recommends screening all Asian American adults with a BMI of ≥23. Nurses are key to implementing individualized, evidence-based, and culturally competent type 2 diabetes management.
Fidelindo Lim is a clinical associate professor at New York University Rory Meyers College of Nursing in New York, New York. Ivan Huang is a registered nurse at New York Presbyterian Columbia University Irving Medical Center in New York, New York.
American Nurse Journal. 2023; 18(3). Doi: 10.51256/ANJ032318
Key words: Type 2 diabetes, Asians, Asian Americans, body mass index, BMI, health disparities
References
Alba DL, Farooq JA, Lin MYC, Schafer AL, Shepherd J, Koliwad SK. Subcutaneous fat fibrosis links obesity to insulin resistance in Chinese Americans. J Clin Endocrinol Metab. 2018;103(9):3194-3204. doi:10.1210/jc.2017-02301
American Diabetes Association. 2. Classification and diagnosis of diabetes: Standards of Medical Care in Diabetes—2021 [published correction appears in Diabetes Care. 2021;44(9):2182]. Diabetes Care. 2021;44(Suppl 1):S15-33. doi:10.2337/dc21-S002
American Diabetes Association. 9. Pharmacologic approaches to glycemic treatment: Standards of Medical Care in Diabetes—2021. Diabetes Care. 2021;44(Suppl 1):S111-24. doi:10.2337/dc21-S009
American Diabetes Association. Hypoglycemia (low blood glucose). diabetes.org/healthy-living/medication-treatments/blood-glucose-testing-and-control/hypoglycemia
Becerra MB, Becerra BJ. Disparities in age at diabetes diagnosis among Asian Americans: Implications for early preventive measures. Prev Chronic Dis. 2015;12:E146. doi:10.5888/pcd12.150006
Centers for Disease Control and Prevention. (2021). Addressing Health Disparities in Diabetes. U.S. Department of Health and Human Services. https://www.cdc.gov/diabetes/disparities.html.
Centers for Disease Control and Prevention. Diabetes 2019 Report Card. cdc.gov/diabetes/pdfs/library/Diabetes-Report-Card-2019-508.pdf
Centers for Disease Control and Prevention. Diabetes and Asian American People. November 21, 2022. www.cdc.gov/diabetes/library/spotlights/diabetes-asian-americans.html
Centers for Disease Control and Prevention. National diabetes statistics report 2020: Estimates of diabetes and its burden in the United states. cdc.gov/diabetes/pdfs/data/statistics/national-diabetes-statistics-report.pdf
Centers for Disease Control and Prevention. Summary health statistics: National health interview survey, 2018. Table A-4a. ftp.cdc.gov/pub/Health_Statistics/NCHS/NHIS/SHS/2018_SHS_Table_A-4.pdf
Centers for Disease Control and Prevention. What is diabetes? July 7, 2022. cdc.gov/diabetes/basics/diabetes.html
Chatterjee S, Khunti K, Davies MJ. Type 2 diabetes [published correction appears in Lancet. 2017;389(10085):2192]. Lancet. 2017;389(10085):2239-51. doi:10.1016/S0140-6736(17)30058-2
Corona G, Pizzocaro A, Vena W, et al. Diabetes is most important cause for mortality in COVID-19 hospitalized patients: Systematic review and meta-analysis. Rev Endocr Metab Disord. 2021;22(2):275-96. doi:10.1007/s11154-021-09630-8
Davidson KW, Barry MJ, Mangione CM, et al. Screening for prediabetes and type 2 diabetes: US Preventive Services Task Force recommendation statement. JAMA. 2021;326(8):736-43. doi:10.1001/jama.2021.12531
Feingold KR. Oral and injectable (non-insulin) pharmacological agents for the treatment of type 2 diabetes. Endotext. 2022. ncbi.nlm.nih.gov/books/NBK279141
Firestone MJ, Beasley JM, Kwon SC, Ahn J, Trinh-Shevrin C, Yi SS. Asian American dietary sources of sodium and salt behaviors compared with other racial/ethnic groups, NHANES, 2011-2012. Ethn Dis. 2017;27(3):241-8. doi:10.18865/ed.27.3.241
Galicia-Garcia U, Benito-Vicente A, Jebari S, et al. Pathophysiology of type 2 diabetes mellitus. Int J Mol Sci. 2020;21(17):6275. doi:10.3390/ijms21176275
Hsu WC, Araneta MRG, Kanaya AM, Chiang JL, Fujimoto W. BMI cut points to identify at-risk Asian Americans for type 2 diabetes screening. Diabetes Care. 2015;38(1):150-8. doi:10.2337/dc14-2391
Skyler JS, Bakris GL, Bonifacio E, et al. Differentiation of diabetes by pathophysiology, natural history, and prognosis. Diabetes. 2017;66(2):241-55. doi:10.2337/db16-0806
U.S Department of Agriculture and U.S. Department of Health and Human Services. Dietary Guidelines for Americans, 2020-2025. 9th ed. 2020. dietaryguidelines.gov/sites/default/files/2020-12/Dietary_Guidelines_for_Americans_2020-2025.pdf
U.S Department of Health and Human Services. Physical Activity Guidelines for Americans. 2nd ed. 2018. health.gov/sites/default/files/2019-09/Physical_Activity_Guidelines_2nd_edition.pdf
U.S Department of Health and Human Services. Profile: Asian Americans. October 12, 2021. minorityhealth.hhs.gov/omh/browse.aspx?lvl=3&lvlid=63
Yi SS, Roberts C, Lightstone AS, Shih M, Trinh-Shevrin C. Disparities in meeting physical activity guidelines for Asian Americans in two metropolitan areas in the United States. Ann Epidemiol. 2015;25(9):656-60:e2. doi:10.1016/j.annepidem.2015.05.002