Progress is slow but steady as RNs head back to school to get their BSN.
By Janet Boivin, BSN, RN
Will 80% of RNs hold a bachelor of science in nursing (BSN) degree by the year 2020? Not likely, say nursing experts. But not to worry, they add. For the first time in the decades-old debate over whether a BSN should be required for practice, RNs are heading back to school in record numbers.
The match that lit this educational flame was the release of the Institute of Medicine’s 2010 Future of Nursing: Leading Change, Advancing Health report, which developed four key messages to help the nursing profession better meet the needs of a rapidly transforming healthcare system. One of those key messages was that “Nurses should achieve higher levels of education and training through an improved education system that promotes seamless academic progression.” This message encouraged the profession to work toward 80% of practicing RNs having a BSN or higher degree by the year 2020.
The recommendation was immediately embraced by nurse educators, nurse leaders, hospital administrators, and most important, nurses themselves. “My message would be that most nurses in this country are working very hard to meet this goal,” says Susan Hassmiller, PhD, RN, FAAN, the Robert Wood Johnson Foundation’s adviser for nursing and the director of the Future of Nursing™: Campaign for Action. “The profession now has more BSNs than associate degree nurses, so we have jumped that hurdle, and the numbers are going up and up in every state. But we are far from the 80/2020 goal.”


“The growth in RN-to-BSN graduates has more than doubled, from a bit below 23,000 to more than 56,000,” says Joanne Spetz, PhD, a health economist at the University of California San Francisco (UCSF). She’s also a professor at the Philip R. Lee Institute for Health Policy Studies and associate director for research at the Healthforce Center at UCSF.
It takes a team to grow a profession
Tina Gerardi, MS, RN, CAE, deputy director for Academic Progression in Nursing, agrees. She credits the increased numbers of associate degree nurses returning to school for a BSN degree to community college nursing faculties’ commitment to students achieving the BSN or higher degrees and the development of strong partnerships between community colleges, universities, and hospitals.
“The partnerships and collaboration fostered between associate degree programs and higher education has changed the culture about nursing education,” she says. “The IOM report also encouraged collaboration between education and employers. We need to continue to foster those programs with a strong partnership between these entities.”
Collaborators are breaking down roadblocks, such as financial, time, and distance constraints, that in the past deterred associate degree nurses from obtaining their BSN degree. Programs that allow direct entry into nursing programs for individuals with a non-nursing degree also have helped increase the number of RNs with a BSN degree.
Hybrid nursing programs use various tools—such as online courses and sharing of faculty between community colleges and 4-year nursing programs—to reduce costs and allow students to remain close to home so they can work and manage family responsibilities. “It uses the best of both worlds,” Gerardi says.
Healthcare employers should be credited for pouring money into opportunities for nurses to gain their BSN degree and faculty members for taking on larger class sizes to accommodate more students, Hassmiller says. Building this educational infrastructure in the last 7 years is, in some ways, more of an achievement than the increased number of RNs with a BSN degree, says Hassmiller.
“If I were to grade the infrastructure that has been built since 2010, I would give it an A minus,” she says. The progress toward 2020 has not caught up with the infrastructure, but this infrastructure will enable the profession to eventually reach the 80% goal.
Another motivator for nurses and the healthcare system is the mounting research-based evidence that patient outcomes are better when care is provided by RNs with a BSN degree, say the nursing experts. “That data resonates with nurses, whose concern for their patients comes first,” Spetz says.
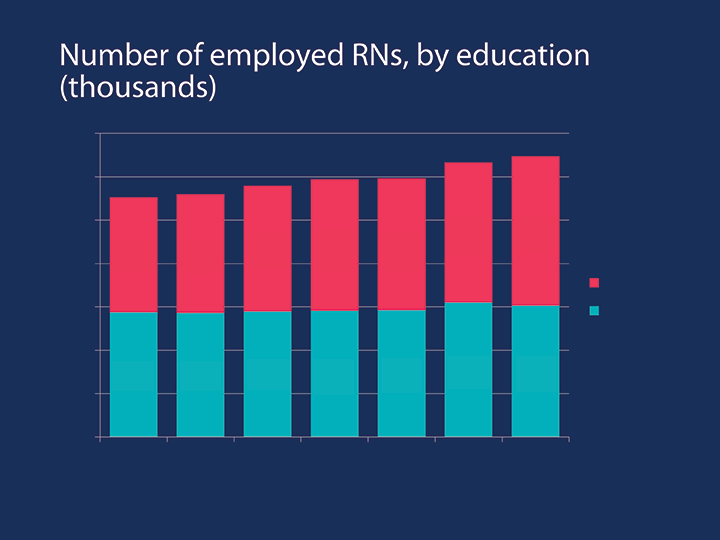
The number of employed nurses with a BSN or higher degree has increased since the Institute of Medicine’s 2010 Future of Nursing: Leading Change, Advancing Health report, as shown below.
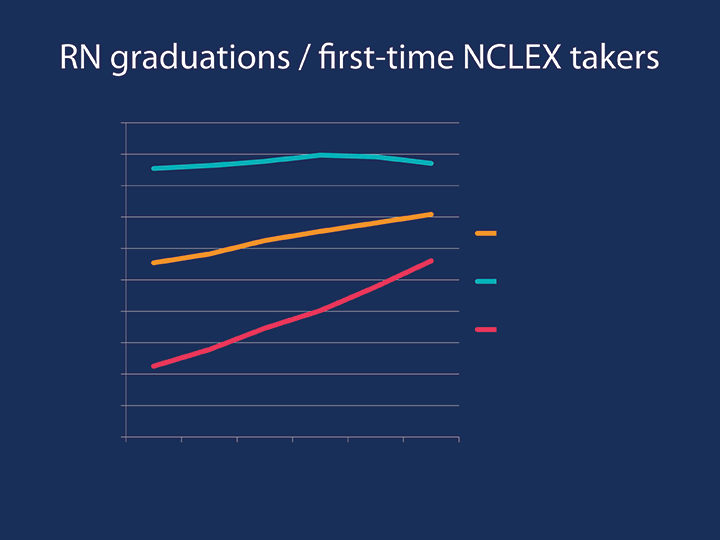
Steady growth has occurred since 2009 in the number of first-time test-takers with a BSN or higher entry degree, and the growth in RN-to-BSN graduates has more than doubled.
Source: Forecasting materials for RN workforce. http://rnworkforce.ucsf.edu/news/forecasting-materials-rn-workforce. Updated June 6, 2017. |
Statistics can be deceiving
An examination of the most recent statistics indicates that the increased percentage of associate degree-to-BSN nurses is slight. But the change is more significant given that 3 million nurses are licensed in this country, Spetz says. “The percentage change masks big numbers. The number of RNs who are not at the BSN or higher level has grown 78,000. But at the same time, the number with a BSN grew nearly 400,000.” (See Making progress.)
Each year since 2014, the number of new first-time NCLEX test-takers with associate and diploma degrees declined a small amount while the number of first-time test-takers with a BSN degree or higher has steadily grown. Remarkable changes in RN education have occurred when looking at new graduates and RN-to-BSN graduates since 2010, Spetz says.
While changes in education—both entry level and RN-to-BSN—have been impressive, she says, progress is still too slow and will continue to be slow for the following reasons:
• The inflow of new RN-to-BSN graduates into the workforce is a trickle into a very large bucket.
• Some incumbent RNs aren’t interested in going back to school.
• The profession continues to rely on associate degree programs to ensure an adequate number of RNs, especially in rural areas.
• Employers may give mixed messages; the preference for BSN degrees may fade as the labor market tightens.
Setting sights on 2025
Spetz says that while the 80% goal won’t be achieved by 2020, it may be possible by 2025. She suggests that the profession gather data on nursing workforce and education, using a forecasting model developed to project BSN plus share over 10 years, and testing scenarios that might speed progress.
An online tool that forecasts the share of RNs who will have a BSN or higher degree based on current numbers and strategies, along with tools to test varying scenarios to accelerate progress, is now available to nurse leaders. It can be accessed at www.rnworkforce.ucsf.edu/news/forecasting-materials-rn-workforce. The tool and website were developed by Spetz for the Robert Wood Johnson Foundation and Academic Progression in Nursing National Program Office.
Janet Boivin, BSN, RN, is a freelance writer.






















2 Comments.
Well how much longer do you want to work.. I am 68 and now going for my BSN. I have paid for conferences and certificates as well and btw , they do not take the place of the BSN. And dont be so complacent about “nurses taking the same test” In Texas since 2011 at least , there is a different test for BSNs and ADNs. A lot more is expected of the RN now than when we went to school. I just because you never borrowed or asked for a grant , good for you . A lot of us have no choice if we want to go to school but to get loan and grant. And there should be no judgement if one does.
AT age 62 Should I commit to $20,000 education? As a registered nurse I have self educated and paid for all of my continuing education attending the US Psychiatric Congress each year. Initiallt this conference was meant for psychiatrists so I went. Now I am unemployed, unable to get a job as it is almost 2020. I guess you are going to get rid of the NCLEX also. May I remind you that we all take the same test. And please don’t send the vultures after me the ones that want me to commit to $20,000. I never borrowed a penny or asked for a grant in my life.