To avoid injuring their patients and themselves, healthcare providers must get in the habit of using safe patient handling and mobility (SPHM) technology. In this supplement, national experts share their perspectives and best practices on topics ranging from dealing with bariatric patients, managing slings, and assessing a patient’s mobility to transforming the culture, building the business case for an SPHM, and developing a successful SPHM program.
Download a PDF of the entire supplement here.
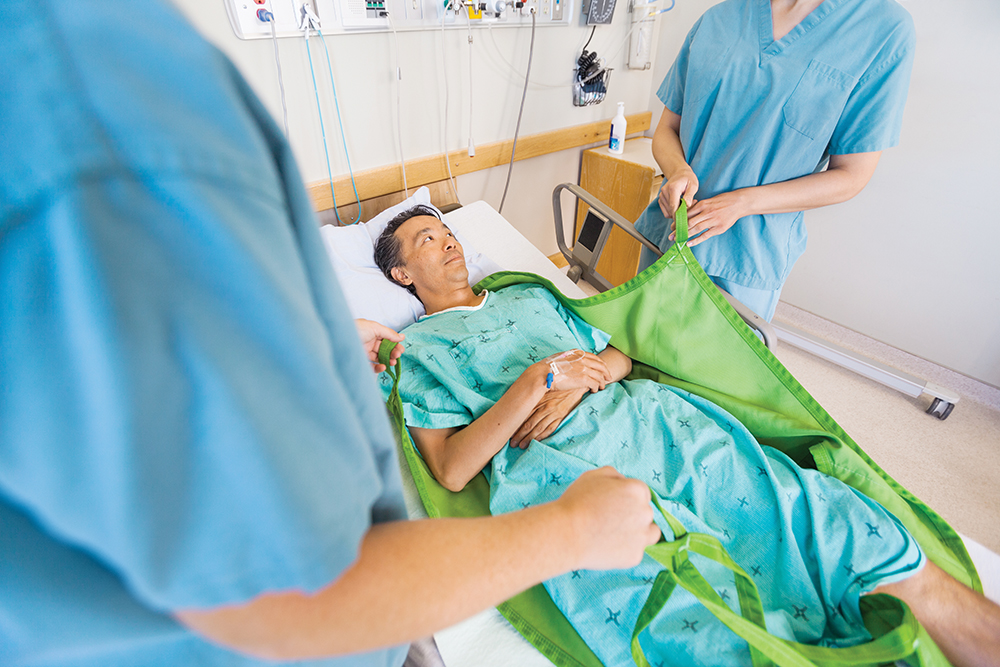
A patient mobility assessment determines your new patient needs a dependent sling. But when you finish your admission intake and reach the sling inventory storage site, you find no slings are available. Or perhaps you see a sling hanging on a hook and wonder if it’s clean or dirty.
If you’ve had an experience like this, you’re probably eager for your workplace to adopt a safe patient handling and mobility (SPHM) program that addresses slings, among other things. But before adopting such a program, a healthcare facility must perform a unit assessment to evaluate:
- medical conditions and mobility needs of its patient population
- maximum number of bariatric patients on the unit at a given time, and how often the unit reaches this number
- tasks performed on the unit
- unit staffing
- storage constraints.
Other parts of an SPHM program related to sling use include infection control and selection of the sling fabric.
Launderable vs. disposable
The SPHM committee, which oversees all aspects of the SPHM program, must decide if the facility should use launderable and reusable slings, disposable slings, or both types. Input from the laundry department is critical. Each type of sling has benefits and drawbacks. (See Comparing launderable and dis- posable slings.) If the committee chooses launderable slings,
the next decision is whether to launder them in-house or outsource laundering to a laundry company.
In-house laundering
Advantages of in-house laundering include:
- negligible number of missing or lost slings because all slings stay in the facility
- shorter turnaround time due to better control of the process
- reduced sling purchase cost due to reduced inventory
- better oversight for maintaining sling standards.
Disadvantages include:
- the need for a dedicated staff member to oversee and manage the process
- the need for space to house a washer, dryer, drying cabinet, folding surface, and storage carts
- a properly vented environment to avoid dampness and mold
- possible injuries to laundry staff due to the added workload. (See Case study: On-site laundry with centralized distribution.)
Outsourced laundering
Advantages of outsourced laundering include a reduced impact on laundry staff and transfer of responsibility for a smooth, successful process off-campus. Disadvantages are possible loss of slings, sling damage from industrial laundering methods, long turnaround time, and costs (determined by the pound or item).
Fabric maintenance
Whichever laundering process is chosen, fabric maintenance guidelines must be followed. Meeting infection-prevention standards is paramount. For example, a protocol for disposing of or treating soiled or infected slings must be established, along with protocols for single patient use of slings. Fabric integrity must be maintained to extend sling life; preserving sling quality for prolonged fabric reliability and sling longevity promotes patient safety and cost-effectiveness. If the facility has chosen to outsource its sling laundering, it must establish a good working relationship with the laundry company, with clear and regular communication.
Inventory purchase and stocking of supplies
A sling management process includes estimating the number and sizes of slings a unit uses, purchasing inventory, and stocking supplies in an organized, effective way. Several factors can affect inventory. For instance, as the SPHM program grows, the facility will need more slings and accessories, and purchasing may be slow to catch up. The laundry service, whether in-house or outsourced, also may be unable to keep up with demand. And despite seemingly reasonable initial expectations, turnaround time might become impractical as the SPHM program evolves. Also, the number or sizes of slings a unit uses may have been estimated improperly initially.
Healthcare facilities have two options for establishing and keeping a satisfactory sling inventory—periodic automatic replenishment (PAR) or centralized distribution.
PAR system
To maintain a PAR level, the facility must keep enough slings on hand so it doesn’t run out while waiting for resupply. Space constraints may limit the PAR level. PAR requires not just a storage area but also a dedicated staff member, along with unit staff, transport staff, and laundry staff for backup. What’s more, if specialized slings are stored on specific units, they’re not easily available on other units. On the other hand, using a PAR system means slings will be readily available on all shifts, which leads to better compliance with the SPHM program.
Centralized distribution
With this system, access to slings may not be available when needed, especially on evenings, nights, weekends, and holidays. A staff member must be put in charge of maintaining central storage for efficient distribution, and a process for obtaining slings must be established. For instance, is a runner needed? If so, who supplies the runner?
Nonetheless, a well-organized centralized distribution process can be highly effective if communication is clear and consistent. Also, lack of unit storage for slings isn’t a concern.
Sling tracking
Sling tracking promotes return of slings to the proper unit. Tracking can be handled in several ways:
- Slings can be labeled with an indelible marker, barcoded, or embroidered. A simple marking system can yield valuable benefits.
- Vendors may have sling tracking systems your facility can use.
Support for the SPHM program
A well-developed sling management system supports a facility’s SPHM program. The SPHM must elicit input from units that will use the system and from the laundry department or outsourced laundry company to ensure all parties’ needs are met. It must choose sling styles and fabric and put in place procedures for sling purchase, inventory maintenance, care, laundering, tracking, and replacement. Once these issues have been addressed, the facility is ready to embark on an SPHM program that can improve patient care and help prevent staff injuries.
Selected references
The Facility Guidelines Institute. 2010 Health Guidelines Revision Committee Specialty Subcommittee on Patient Movement. Patient handling and movement assessments: A white paper. April 2010. https://www.dli.mn.gov/wsc/PDF/FGI_PHAMAwhitepaper_042710.pdf. Accessed June 24, 2014.
Occupational Safety and Health Administration. Lift program policy and guide: Introduction to the lift program. https://www.osha.gov/CWSA-attachment/beverlyliftprogramguide.pdf. Accessed July 3, 2014.
Jan DuBose is director of Safe Patient Handling Programs and Services at Hill-Rom.